-
Paper Information
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
International Journal of Stomatological Research
p-ISSN: 2326-1129 e-ISSN: 2326-1153
2013; 2(1): 5-10
doi:10.5923/j.ijsr.20130201.02
Incorporation of Casein Phosphopeptide-Amorphous Calcium Phosphate into Glass-Ionomer Cement for Orthodontic Band Cementation – An in vitro Study
Tejas. R. Pol1, C. R. Naik2, Ravi Gupta2, Anuradha Pol3, Sanket Sanghvi2
1Department of Orthodontics, YMT Dental College & Hospital Mumbai India
2Department of Orthodontics, Dr.D.Y. Patil Dental College & Hospital, Pune India
3Department of Conservative and Endodontics, MGM dental college and hospital, Mumbai India
Correspondence to: Tejas. R. Pol, Department of Orthodontics, YMT Dental College & Hospital Mumbai India.
| Email: |  |
Copyright © 2012 Scientific & Academic Publishing. All Rights Reserved.
Aim:To determine the effect of incorporating Casein Phosphopeptide-amorphous calcium phosphate (CPP-ACP) into self-cured glass-ionomer cement (GIC) and to compare the shear-peel band strength.Materials and method:1) Ion Measurements and CPP Detection: Discs of 6 mm diam x 2 mm thick was prepared for following groups: Group I - GIC & Group II - GIC +1.56% w/w CPP-ACP. The discs incubated at 37°C in 2mL of deionized water (pH 6.9) and 2mL of 50mM sodium lactate buffer at pH 5.0. The release of calcium, inorganic phosphate, and fluoride ions was measured in each solution.2) Shear-Peel band strength: 60 Non carious human molars collected, stored in distilled water after decontamination in 0.5% chloramine. Extracted molars divided into 2 groups each group containing 30 molars. Group I – bands were cemented with GIC & Group II - bands were cemented with GIC +1.56% w/w CPP-ACP. With the use of an Instron universal testing machine, a shear-peel load was applied to each cemented band. SEM analysis was done with each group.Results: Incorporation of 1.56% w/w CPP-ACP into the GIC resulted in an increase in shear peel band strength. Fluoride, Calcium & Phosphate ions release was significantly higher in Group II as compare to Group I. Conclusion: Incorporation of 1.56% w/w CPP-ACP into the GIC significantly increased shear-peel band strength and significantly enhanced the release of fluoride, calcium and phosphate ions at neutral and acidic pH. Thus incorporation of CPP-ACP phosphate can prevent demineralization and promotes remineralization of enamel subsurface lesions.
Keywords: Shear Peel Band Strength, CPP-ACP , GIC, Orthodontic Material
Cite this paper: Tejas. R. Pol, C. R. Naik, Ravi Gupta, Anuradha Pol, Sanket Sanghvi, Incorporation of Casein Phosphopeptide-Amorphous Calcium Phosphate into Glass-Ionomer Cement for Orthodontic Band Cementation – An in vitro Study, International Journal of Stomatological Research, Vol. 2 No. 1, 2013, pp. 5-10. doi: 10.5923/j.ijsr.20130201.02.
Article Outline
1. Introduction
- Fixed orthodontic appliances, by hampering effective oral hygiene, can result in increased oral plaque accumulation and increase the risk of white-spot lesion formulation[1]. The reported prevalence of white-spot lesions during orthodontic treatment has ranged from 2 to 96% of affected individuals[1-4].Orthodontic bands around the crowns of molars and second bicuspids still play an important role in providing stable attachment for an arch wire and the use of additional appliances such as headgear or palatal arch and thus, their retention around the crowns is vital in the successful application of orthodontic forces leading to successful treatment. A common problem experienced by many orthodontists and patients is the development of enamel demineralization and even caries following the use of brackets and bands bonded and cemented to teeth[5-7]. Orthodontic bands are believed to facilitate more enamel demineralization than bracketed teeth[3].Dental caries is initiated via the demineralization of tooth hard tissue by organic acids produced from fermentable carbohydrate by dental plaque cariogenic bacteria. Fluoride ions, in the presence of calcium and phosphate ions, can help replace the lost mineral of early caries lesions by remineralization.However, unfavorable properties found in many of luting cements, such as high solubility in oral fluids and low bond strengths, may contribute to demineralization beneath the bands. However, GIC are ion-releasing materials and the incorporation into and slow release of fluoride ions from the cement provides a significant anticariogenic property[8].Casein phosphopeptide-amorphous calcium phosphate nanocomplexes (CPP-ACP) have been shown to prevent enamel demineralization and promote remineralization of enamel subsurface lesions in animal and human in situ caries models[9-11]. The anticariogenic potential of CPP-ACP has been attributed to the ability of the CPP to localize amorphous calcium phosphate at the tooth surface, thereby helping to maintain a state of supersaturation with respect to tooth mineral[11].Extensively researched, CPP-ACP has proven to bind readily to pellicle, plaque, soft tissue and even hydroxyapatite when applied within the oral cavity. This helps to maintain a state of supersaturation of calcium and phosphate at the tooth surface, which depresses demineralization and enhances remineralization. Thus a product of combination of these two materials can show a synergistic effect.The Aims of this study were.1. To determine the effect of incorporating CPP-ACP into self-cured GIC on shear peel band strength.2. To evaluate Fluoride, Calcium and Phosphate ions release.3. To evaluate surface characteristic of both groups under scanning electron microscope.
2. Materials & Method
- Ion Measurements and CPP Detection:Discs of 6 mm diam x 2 mm thick were prepared for following groups.Group I --GICGroup II--GIC +1.56% w/w CPP-ACPThe GIC disc was prepared with self-curing glass-ionomer luting cement (Gold label, GC, Tokyo, Japan). The disc containing GIC+ CPP-ACP was prepared from the same GIC , with 1.56% w/w (Percent by weight) CPP-ACP (Tooth Mousse plus/MI paste, GC Corporation, Tokyo, Japan) incorporated. The CPP-ACP and GIC powder were manually mixed, and the powder: liquid ratio 2: 1 as recommended by manufacturer.The mixed cement was carried into the mold, condensed, and allowed to set at 37°C and 100% humidity for 1 hr in humidor. During setting, the bottom and top of the filled molds was covered by glass slab. The discs was removed from the molds, placed in individual sealed plastic tubes, and incubated at 37°C in both 2mL of deionized water (pH 6.9) and 2mL of 50mM sodium lactate buffer at pH 5.0. The solutions was changed every 24 hrs for 3 days, and the release of Fluoride, Calcium and Phosphate ions was measured in each solution.A calcium concentration was determined by atomic absorption spectrophotometry[8] (lab India), fluoride and inorganic phosphate was determined by Ion chromatogram [11] (Dionex India ltd.).By measuring the Fluoride, Calcium and Phosphate ions in parts per million (ppm) in a known volume of deionized water and sodium lactate buffer, it was possible to calculate the total amount of ions released from the specimens. After each reading was taken, the total ions released in micrograms was calculated by multiplying the parts per million (1 ppm = 1 µg/mL) by the deionized water sample volume or sodium lactate buffer. The total fluoride, calcium and phosphate were then divided by the area of the sample disk to obtain the ion release in micrograms per square centimeter.Shear-Peel band strength:The force required for debanding was used as a measure of shear-peel band retention. 60 Non carious human third molars collected, stored in distilled water after decontamination in 0.5% chloramine. The teeth were randomly divided into two groups of 30 teeth. In preparation for measuring bond strength, 60 teeth were notched in the apical third with a diamond bur, and then mounted below the cementoenamel junction in block of self cure acrylic, with the long axis of each tooth vertical. The teeth were then cleaned with pumice slurry, rinsed in distilled water and dried thoroughly in a stream of air. As bands do not exist for third molars, first permanent molar bands (3M Unitek) were used with attachments fitted i.e. tubes welded on buccal and lingual surface of bands were seated around the teeth including adaptation of the margins. Bands were selected and placed by the same operator to eliminate any operator bias in band positioning and fitting. 1.56% w/w of CPP-ACP was incorporated to GIC which was manually mixed, and the powder: liquid ratio for GIC used was 2: 1 as recommended by manufacturer. Groups were as followsGroup I - bands were cemented with GIC Group II - bands were cemented with GIC+ 1.56% w/w CPP-ACP Once the bands had been positioned accurately on the tooth surface and pressed firmly into place, excess cement was removed with dry cotton rolls. All specimens were then transferred to a humidor set at 37° C for 24 hours before measuring shear peel band strength.Band removal: - Each mounted tooth was fixed to the customized holding device to the lower load cell of the Universal testing machine. 0.8mm Stainless steel wire was passed from the attachment both on the buccal and lingual side of the band and held by holding device (Fig 1). This configuration allowed all forces to be directed parallel to the long axis of the tooth during debanding. With the use of a Universal testing machine[Star Testing System, India. (Model no .STS 248)] , a shear-peel load was applied to each cemented band. The shear load was applied at a crosshead speed of 5mm/min and the load cell used was 500N. Testing proceeded for each specimen until the band was removed from the tooth. The maximum force recorded during debonding was chosen from the stress– strain curve[12] for each specimen. The force required to deband was registered in Newtons and converted into Megapascals as a ratio of Newton to surface area of the band (MPa=N/mm2).SEM analysis was done for both groups[FEI- quanta 200 (SEM under low vacuum)].
3. Stastical Analysis
- The mean retentive strengths for the cements tested were compared using t- test. In addition, we calculated Weibull modulus. This form of analysis might be more meaningful for evaluating bond strength data because it takes into account the bond strength values at the extremes of the distribution[13, 14]. Weibull modulus has been used previously to assess fracture processes in chemically activated and light-activated composites[15] and in the evaluation of bonding agents[14] and band cements[13], for orthodontic use. By generating a Weibull modulus for each band cement, numerical evaluation of its reliability is feasible. A low value of Weibull modulus indicates a wide scatter of bond strength values, whereas a high value of Weibull modulus indicates close grouping of bond strength values and better dependability of the cement[14].
4. Results
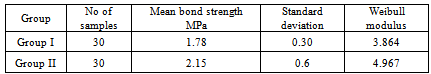
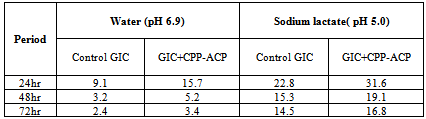
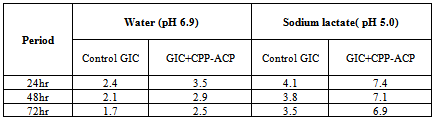
- Incorporation of 1.56% w/w CPP-ACP into the GIC resulted in an increase in shear peel strength. Unpaired t test was applied, p < 0.001; which means that there is statistically highly significant difference between the Group - I and Group – II, it has observed that Group – II (2.15 MPa) has more shear band strength than Group - I (1.78 MPa) (Table 1) and higher weibull modulus was found in Group II (Table 1).Ion and CPP ReleaseThe pattern of fluoride release in water was similar between both groups, with the highest release occurring during the first 24 hrs and a slower but continued release during the next two 24-hour periods. Fluoride release was significantly higher in the pH 5.0 sodium lactate buffer than in water for both materials. Significantly higher fluoride release was found with the Group II, when compared with the Group I at both pH values (Table 2).Similarly Calcium ion release was detected for both groups at both pH. The release was low relative to fluoride but continuous during the three 24-hour periods (Table 3). At both pH values, inorganic phosphate ion release was significantly higher from the Group II than from the Group I during the first 24-hour period. The release of inorganic phosphate was significantly higher in sodium lactate buffer at pH 5.0 than in water for both Groups (Table 4).
|
|
|
|
5. Discussion
- Orthodontic treatment is almost always an elective procedure to improve the patient’s dentofacial appearance. Patients may develop areas of decalcification adjacent to orthodontic brackets and bands such lesions could be considered iatrogenic. The effects of decalcification may be white spots on the enamel, or even cavitations. They appear as unsightly lesions on previously healthy teeth at the end of orthodontic treatment. They can require further treatment after orthodontic treatment to mask or remove them.In this study, 30 third molars were used per group for shear peel band strength testing. This sample size has been recommended as optimal for studies of this nature[14], and specimen storage before use complied with guidelines in the orthodontic literature[14]. A major reason for the use of Glass ionomer cement in a variety of clinical applications is their capacity to bond chemically to different surfaces[16].In the study reported here the shear peel band strength for Group II was more as compare to the Group I. Strength obtain for Group I was very much similar to the results obtain in other studies by Millett et al where mean values for GIC on natural teeth ranged from 1.27 to 1.65Mpa.[17-20]. The intent of this experiment was to examine orthodontic luting cements such as GIC and combination of GIC+CCP-ACP for improved handling characteristics and potential fluoride, calcium and phosphate release. Comparisons with previous studies were difficult because different material were used.The role of CPP-ACP in decreasing the incidence of dental caries in the community is anticipated to be additive to the beneficial effects of topical fluoride[21]. The CPP molecules contain a cluster of phosphoseryl residues which markedly increase the apparent solubility of calcium phosphate by stabilizing amorphous calcium phosphate[22] under neutral and alkaline conditions. CPP-ACP nanocomplexes have been shown to prevent enamel demineralization and promote remineralization when used in a mouthwash or sugarfree gum so the combination of GIC & CPP-ACP enhances protection of the adjacent enamel to acid demineralization promote enamel subsurface lesion remineralization. CPP-ACP nanocomplexes subsequently act to buffer free calcium and phosphate ions in the plaque fluid, in order to maintain a state of supersaturation of ACP with respect to enamel mineral, thereby limiting enamel demineralization and enhancing remineralization[9-10, 22-24].With respect to the release of ions from the GICs, Ion chromatograph was used to monitor fluoride release in this study. This has the advantage of being accurate at very low concentrations and gives a direct measurement of the effective free fluoride ion concentration which may not be possible using other methods[25] it was shown that the fluoride release in sodium lactate buffer (pH 5.0) was significantly higher than that in water (pH 6.9). The pattern of fluoride release for glass ionomer indicates a high initial release rate followed by a slow rate of release over time. This finding has been previously reported for normal GIC[8, 20, 26]. Fluoride release was significantly higher from Group II than from the Group I at both pH values. It is possible that the CPP-ACP promoted the release of fluoride ions from the GIC by forming CPP-ACP nanocomplexes, which were released from the cement matrix[27].Significantly more inorganic phosphate was also released from Group II at both pH values (5.0 & 6.9) than from the Group I, consistent with the addition of the stabilized amorphous calcium phosphate. Calcium is an ion not easily leachable from GIC once the cement has set[28], due to its rapid binding, in an insoluble form, to the polyacrylic acid matrix[29]. Elution of calcium, when it does occur, has been attributed to acid erosion of the cement matrix[8, 28].It has not been clearly established whether the mode of failure for a particular material is associated with its bond strength or elastic modulus. It is known that the pores in a solid body act as stress-concentration points where fracture can initiate[30] and it has been speculated that this explains the frequency of cohesive failure within a GIC[31]. (Fig 2 & Fig 3) illustrates SEM analyses of the fractured surfaces of the different GICs which suggest a greater porosity of the. Group I relative to the Group II. More cracks were seen in Group I & greater porosity in the Group I could be the probable reason for less bond strength. This lends support to the findings of the Weibull modulus for both of these cements.The CPP-ACP in the GIC may have also directly increased shear peel band strength by the incorporation of the CPP-ACP nanoparticles into the crosslinked matrix of the GIC. Further research in an in-vivo setup would be required before extrapolating these results to the intraoral environment.
 | Figure 1. Universal testing machine experiment setup |
 | Figure 2. SEM image of Group I |
 | Figure 3. SEM image of Group II |
6. Conclusions
- Incorporation of 1.56% w/w CPP-ACP into a GIC was shown to increase shear peel band strength and enhance the release of fluoride, calcium and phosphate ions. The results of this study suggest that the 1.56%-CPP-ACP-containing GIC is superior luting cement for orthodontic band cement with an improved anticariogenic potential.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML