-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
Clinical Medicine and Diagnostics
p-ISSN: 2163-1433 e-ISSN: 2163-1441
2011; 1(1): 8-16
doi: 10.5923/j.cmd.20110101.02
Antibiotics Overuse in Children with Upper Respiratory Tract Infections in Saudi Arabia: Risk Factors and Potential Interventions
Arwa Alumran 1, 2, 3, Cameron Hurst 1, 2, Xiang-Yu Hou 1, 2
1School of Public Health, Queensland University of Technology, Brisbane, 4059, Australia
2Institute of Health and Biomedical Innovation, Queensland University of Technology, Brisbane, 4059, Australia
3Health Information and Management Department, College of Applied Medical Sciences, University of Dammam, Saudi Arabia
Correspondence to: Arwa Alumran , School of Public Health, Queensland University of Technology, Brisbane, 4059, Australia.
| Email: |  |
Copyright © 2012 Scientific & Academic Publishing. All Rights Reserved.
Background: Antibiotics misuse is currently one of the major public health issues worldwide. This misuse can lead to the development of bacterial resistance, increasing the burden of chronic diseases, rising costs of health services, and the development of side effects. Several factors may influence this pattern of overuse. Objectives:This article will review the pertinent factors contributing to the overuse of antibiotics worldwide, and to assess the intervention strategies to limit this overuse. Methods: studies about antibiotics use in children were reviewed from several electronic databases, such as MEDLINE and Pubmed. Results: Factors contributing to the overuse of antibiotics could include psychosocial factors, such as behaviors and attitudes (e.g. self-medication, over-the-counter medication, or patients/parents pressure), and demographic factors, such as socio-economic status and education level. Several intervention strategies were reported to be effective in reducing the overuse of antibiotics, such as health education, doctor-patient communication, and policies change. Multifaceted interventions were found to be the most effective in reducing the antibiotics overuse.
Keywords: Antibiotics, Misuse, Overuse, Intervention Strategies, Children, Upper Respiratory Tract Infections, Saudi Arabia
Cite this paper: Arwa Alumran , Cameron Hurst , Xiang-Yu Hou , "Antibiotics Overuse in Children with Upper Respiratory Tract Infections in Saudi Arabia: Risk Factors and Potential Interventions", Clinical Medicine and Diagnostics, Vol. 1 No. 1, 2011, pp. 8-16. doi: 10.5923/j.cmd.20110101.02.
Article Outline
1. Introduction
- Despite the effectiveness of antibiotics in the treatment of numerous bacterial infections, it is often used inappropriately. This misuse of antibiotics is currently one of the major public health issues worldwide (Fahey, Stocks, & Thomas, 1998; Flora, Scott, Jason, & Jonathan, 2008; Grigoryan, et al., 2007; Le, Ottosson, Nguyen, Kim, & Allebeck, 2011; Tenover, 2006). Although antibiotics are targeted to kill or inhibit the growth of bacteria and have no effect on viral agents (JETACAR, 1999), it is often inappropriately used to treat viral infections, such as most of Upper Respiratory Tract Infections (URTIs). Problems associated with the overuse of antibiotics include development of antibacterial resistance, increasing the burden of chronic diseases, raising costs of health services, and the development of side effects (e.g. adverse gastrointestinal effects). Antibiotic misuse was found to be significantly frequent in children, especially when presenting with viral upper respiratory tract infections (URTIs) (Cebotarenco & Bush, 2007). El-Gilany(2000) studied the trends in antibiotic use/misuse for adult patients attending primary health care center and found that of all prescriptions for URTIs, approximately 87 percent contained antibiotics.Several contributing factors are evidently associated with the overuse of antibiotics both at the patient’s (or parents of children) level and doctor’s level, namely: cultural factors, behavioral characteristics, socio-economic status, and level of education (Braun & Fowles, 2000; Kozyrskyj, et al., 2004; Teng, Leong, Aljunid, & Cheah, 2004). Furthermore, doctors usually relate their pattern of over prescribing to patients’/parents’ pressure (Peche're, 2001). Also, lack of health education is one of the major contributing factors in the overuse of antibiotics (Cebotarenco & Bush, 2007). Self medication is a very important behavioural aspect that contributes to the misuse of antibiotics (Bi, Tong, & Partonc, 2000; Sarahroodi, Arzi, Sawalha, & Ashtarinezhad, 2010). This article is a review of the literature regarding the global overuse/misuse of antibiotics in children with upper respiratory tract infections. Factors influencing this behavior and interventions targeted to limit this phenomenon are also discussed in this review.
2. Materials and Methods
- Studies about antibiotics misuse were reviewed from several electronic databases, such as MEDLINE and Pubmed. A total of 72 worldwide articles were reviewed, countries included in this review are: Australia, the United States of America, Canada, the United Kingdom, some European countries, some Middle East countries (Saudi Arabia, Jordan, Kuwait, and Iran), some South American countries, some African countries, and some Asian countries.
3. Literature Review
3.1. Antibiotics Misuse
- Antibiotics are chemical agents capable of either killing or inhibiting the growth of bacteria (JETACAR, 1999). Antibiotics have a major role in the treatment of bacterial infections, which have led to significant reduction in child morbidity and mortality rates worldwide (Teng, et al., 2004). However, since the introduction of antibiotics in 1941 (Waksman, 1947), antibiotics consumption has significantly increased around the world (Cebotarenco & Bush, 2007). Several researchers have studied this increasing consumption of antibiotics through the years and an increasing trend of inappropriate consumption has been demonstrated in a range of countries (Ahmed & Al-Saadi, 2005; Al-Faris & Al-Taweel, 1999; Irshaid, Al-Homrany, Hamdi, Adjepon-Yamoah, & Mahfouz, 2004; JETACAR, 1999; Mainous, Hueston, Davis, & Pearson, 2003; Simasek & Blandino, 2007; Simoes, et al., 2006).Huang et al. (2007) believed that a considerable amount of antibiotics prescribed to children is inappropriate. This significant finding of the escalating antibiotic misuse especially in children is therefore considered one of the most important global public health issues. Ali & Ahmed (1995), found that antibiotics were the drugs most commonly prescribed by the primary care physicians for all age groups representing 40-63% of the total drug prescriptions in the Asir region, in southern Saudi Arabia. Similarly, Ahmed & Al-Saadi (2005) studied the prescribing patterns of 200 doctors in Saudi Arabia and found that the most frequent drug categories prescribed for all age groups were antibiotics. Thus, information from these resources emphasizes the need for continuing medical education on the physicians’ rational prescribing behavior.
3.1.1. Upper Respiratory Tract Infections (URTIs)
- Literature reports (Palmer & Bauchner, 1997; West, 2002) have shown that upper respiratory tract infections (URTIs) are the most common infectious diseases worldwide, including common cold, influenza, rhinorria, and bronchitis. URTIs were responsible for almost one-quarter of all encounters in a general practice evaluated in a Malaysian study (Teng, et al., 2004). Bhasin, Budden, Ketkar, & Pawar(2002) reported that URTIs are responsible for a large percentage of consultations in general practices, mostly in the case of neonates, infants and children. A study in the United Kingdom have been conducted to evaluate the prevalence of URTIs specifically in children, showed that the average number of common cold episodes occurring in each child annually is 3-8 times and some children (10-15%) have at least 12 episodes of common cold per year (West, 2002). It is argued that this increasing number of URTIs episodes in children is associated with attendance at day-care centers or nurseries (McCutcheon & Fitzgerald, 2001; Palmer & Bauchner, 1997; West, 2002). The public’s knowledge in regard to URTIs in Saudi Arabia needs to be further investigated to measure its association with antibiotics overuse.
3.1.2. Inappropriate Antibiotic Use to Treat Viral URTIs
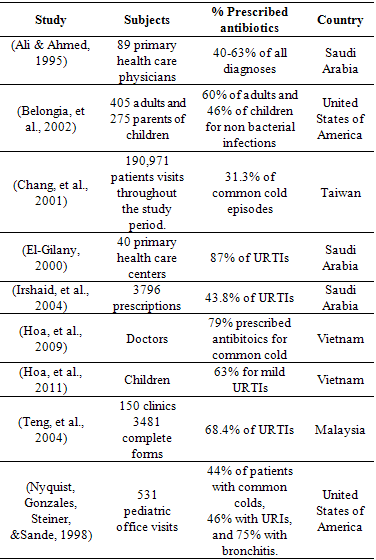
- Although antibiotics therapy is considered appropriate for treating acute bacterial infections such as acute otitis media, rhino-sinusitis, and bacterial pharyngitis; it is proven to be inappropriate for treating bronchitis or viral URTIs (Hoa, et al., 2009; Skull, Ford-Jones, Kulin, Einarson, & Wang, 2000). Proper decision-making regarding the appropriate use of antibiotics is challenging and experience is needed to promote decision-making skills. Three criteria were documented by Bennet & Geme (1999) to promote decision-making process regarding antibiotics prescriptions: (1) antibiotics are not indicated at all (e.g. common cold and bronchitis), (2) using clinical criteria to justify the need for antibiotics (e.g. otitis media and sinusitis), or (3) diagnostic testing confirming the need for antibiotics (e.g. pharyngitis). Appropriate judgment can lead to an overall decrease in antibiotics use and ultimately in reducing antibiotics resistance (Bennet & Geme, 1999). Physicians’ decision-making skills in Saudi Arabia need to be investigated to find its association with the over prescription of antibiotics.URTIs are usually viral in nature and using antibiotics to treat them is considered inappropriate, except for cases where bacterial infections are obvious. URTIs are usually self-limiting and resolve in the same amount of time regardless of antibiotic consumption(Wutzke, et al., 2007). A meta-analysis by Al-Faris & Al Taweel(1999) and several systematic reviews(Arroll & Kenealy, 2005; Fahey, et al., 1998) concluded that there is no evidence to support the use of antibiotic treatment for acute bronchitis. Despite the proven ineffectiveness of antibiotics in the treatment of viral URTIs, research around the world shows a high prevalence of antibiotics used to treat URTIs (Table.1). In a study conducted in Malaysia by Teng et al. (2004), antibiotics were prescribed more frequently in patients with URTIs (68.4%) than those without URTIs. Similarly, The Saudi literature revealed that the most frequent diagnosis in all age groups for which antibacterial drugs were prescribed was URTI (43.8%) (Irshaid, et al., 2004). Also, El-Gilany (2000) found consistent results when they assessed the pattern of drug prescriptions in all age groups attending primary health care centers in Saudi Arabia; one-third of the prescriptions analyzed in their study were for URTIs and 87% of those were prescribed antibiotics. Concurrent results were found in Taiwan where antibiotics were prescribed in 31.3% of patients with common cold (Chang, Shiu, & Chen, 2001). Belongia et al. (2002) revealed that, of those with non bacterial infections, 60% of the adults and 46% of the children were prescribed antibiotics. Also, in a recent study in Vietnam Hoa, et al. (2011) found that 62% of the study children were given antibiotics and 63% of antibiotic courses were used for mild ARIs.These worldwide figures highlight the importance of exploring the factors affecting the excessive use of antibiotics to treat viral URTIs.
|
3.2. Problems Associated with Unnecessary Exposure to Antibiotics
- The excessive use of antibiotics exposes the community to several public health issues, some of which are:
3.2.1. Antimicrobial Resistance
- Although antibiotics have a significant role in the reduction of morbidity and mortality rates worldwide, their increasing inappropriate consumption leads to the development of bacterial resistant strains. Such resistance to antibiotics is likely to lead to reduction in the effectiveness of many antibiotics (Sorkhou, et al., 2002). Moreover, antimicrobial resistance places both populations and individuals at risk (JETACAR, 1999; Mainous, et al., 2003; Simasek & Blandino, 2007). Green (2006) asserts that antibiotics are becoming inadvisable with the emergence of antibacterial resistance. One of the main reasons that encourage the development of antibiotic resistance is the inappropriate use of antibiotics to treat viral URTIs (Teng, et al., 2004). Individuals’ risk from unnecessary consumption of antibiotics, especially to treat URTIs, should be emphasized. Numerous studies confirmed that high proportions of young children get URTIs from childcare attendance, and most of these children receive antibiotics to treat their URTIs; thus indirectly leading to the development of bacterial resistance in the community (Arnold & Straus, 2005; Nyquist, et al., 1998). Skull et al. (2000) and Kozyrskyj et al.(2004) concur that child-care center attendance is an indirect risk factor for developing bacterial resistance. Promoting the judicious use of antibiotics by parents could protect children from bacterial resistance.
3.2.2. Cost
- The cost of health services will be significantly elevated ifthe problem of antibiotic misuse persists(Al-Faris & Al-Taweel, 1999; Foster & Sabella, 2011; JETACAR, 1999; Sarahroodi, et al., 2010).For example, according to West (2002), $2 billion are spent each year in USA on over-the-counter preparations to treat cold symptoms, mainly in children. Moreover, Mainous & Hueston (1998) examined the use of antibiotics to treat URTIs in outpatient setups in USA, and found that 23% of the total cost was for the unnecessary use of antibiotics. Pestotnik, Classen, Evans, & Burke(1996) assert that antimicrobial agents are one of the costliest drug categories in hospital expenditures, accounting for approximately 20% to 50% of the total spending on drugs in USA.These studies are supportive of Mainous & Hueston(1998), who believed that it is important to reduce the use of inappropriate treatments for low-cost, high-volume conditions, such as antibiotics for URTIs, since it has significant implications for the cost of health care.The financial burden of the emergence of bacterial resistant strains is significant. Studies have confirmed that the emergence of bacterial resistance strains leads to significant economic loss, since the cost of length-of-stay and treatment of patients with bacterial resistance infections are significantly increasing(Emanuele, 2010; Mora, et al., 2002). According to Mora, et al. (2002), Almost 100 million dollars are estimated to be spent annually in USA to treat patients with resistant bacterial infections. Minimizing the overuse of antibiotics will lead to reduction in bacterial resistance pattern; which will consequently deflate the excessive cost spent for treatment.
|
3.2.3. Side effects
- Several side effects may occur from over consumption or inappropriate consumption of antibiotics. A risk of adverse gastrointestinal effects may be caused by antibiotics over use (Irshaid, et al., 2004; Simasek & Blandino, 2007). According to Schroeder & Fahey (2002), drowsiness, diarrhea and hyperactivity are also significant side effects related to antibiotic use in children. These adverse effects are more significant in children (Simasek & Blandino, 2007). Moreover, Mora et al. (2002) suggest that adverse events may occur when people use multiple drugs, which may be associated with the increase in resistant bacterial infections. Goolsby(2001) believes that it is important to increase patients’/parents’ awareness regarding antibiotics potential to inflict unnecessary side effects, such as, gastrointestinal effects, allergies, the development of antibiotic-resistant strains, and other infections. Al-Faris & Al Taweel(1999) suggest that doctors also need to be aware of the lack of evidence of effectiveness of antibiotics in the treatment of URTIs, as well as the obvious cost and side effects of many prescriptions for self-limiting conditions. Problems associated with the unjustified use of antibiotics, emphasize the need to educate the community (doctors and parents) about the consequences of the overuse of antibiotics, especially for the treatment of URTIs in children. Therefore, information about patterns of antibiotics utilization and factors influencing this pattern are necessary to be collected in order to develop a constructive approach to minimize this important public health issue.
3.3. Factors Influencing the Overuse of Antibiotics
- The problem of antibiotic misuse may be influenced by several contributing factors, such as cultural, cognitive (e.g. parents pressure), educational, and socio-economic factors integrated at the level of patients or parents, physicians and pharmaceutical industries (Table.2).
3.3.1. Parents’ Pressure
- Parental expectation (Real or perceived) is a major factor that influences physicians’ prescribing behavior. Studies have revealed that most parents expect physicians to prescribe antibiotics for their children even when presenting with viral infections such as most URTIs (Huang, et al., 2007). A survey conducted in Hong Kong showed that almost one third of the respondents (adult patients and guardians) presented at the family practice center particularly to obtain antibiotics (Chan, 1996). In addition, about half of pediatricians in USA report frequent parental pressure to prescribe non-indicated antibiotics (Huang, et al., 2007). In Canada nearly half of the physicians believe that they would reduce their antibiotic prescribing if parents pressure for prescriptions was reduced (Paluck, et al., 2001). Parental perceptions regarding antibiotics prescription have a huge impact on physicians’ decision-making.Several researchers believe that although physicians might feel uncomfortable in prescribing antimicrobial to children with URTIs, they may resort to irrational prescription in order to foster good relationship with patients’ guardians (Barden, Dowell, Schwartz, & Lackey, 1998; Butler, et al., 2001; Mangione-Smith, McGlynn, Elliott, Krogstad, & Brook, 1999).Sorkhou et al.(2002) conducted a study in Kuwait (a country similar to Saudi Arabia geographically and culturally) to evaluate the factors influencing the antibiotic misuse, and found that many physicians feel obliged to prescribe antibiotics to their patients assuming the patients’ or guardians’ desire for such medication. However, this irrational prescribing behavior may encourage parents’ false idea of antibiotics to treat URTIs and its side effects.The problem of antibiotic over prescribing may also be associated with parents’ expectations regarding antibiotics or physicians’ perception about parents’ expectation. Britten & Ukoumunne(1997) concluded from their study in London, UK that patients’ expectations for prescriptions exceeded doctors’ perceptions of these expectations. On the other hand, Macfarlane, Holmes, & Britten (1997) believed that physicians’ generally overestimate patients’ expectations. Therefore, it is important to identify the source of the overuse of antibiotics to treat URTIs, whether it is physicians’ prescribing behavior, parents’ expectations, or an interaction between parents’ expectations and physicians prescribing behavior. Thus, suggesting an intervention strategy that would be beneficial in reducing this inappropriate use of antibiotics.
3.3.2. Lack of Health Education
- Health education is an important factor contributing to the escalating problem of antibiotic over prescription. Cebotarenco & Bush(2007) revealed that patients’ or parents’ lack of knowledge in antibiotics therapy (i.e. to treat bacterial infections) and the harmful effect caused by inappropriate use (i.e. to treat viral infections) is a contributing factor to the trend of antibiotic misuse. For example, the majority of the parents of patients attending family practice centers in Hong Kong had a false notion that URTIs affecting their children would not resolve on its own and antibiotics are necessary to treat the symptoms (Chan, 1996). Cebotarenco & Bush(2007) believed that parents’ misconceptions about appropriate indication for antibiotics use leads to an increase in their children’s consumption of antibiotics often without physicians’ knowledge. Moreover, almost all physicians (93.5%) in a study conducted in Canada believed that educating parents about antibiotics and their implications would reduce expectations for antibiotics (Paluck, et al., 2001). Patients’ lack of health education needs to be emphasized in order to minimize the irrational use of antibiotics.Health education could take place in physician’s offices, schools, and universities. However, evidence shows that health education is minimal in many pediatric clinics, which may be due to the lack of time. Several researchers considered the lack of time to negotiate a different management plan as an important issue that needs to be addressed in order to improve antibiotics prescription practices (Davey, Pagliari, & Hayes, 2002). Huang et al.(2007) revealed that mothers often felt that physicians do not clarify why an antibiotic is not needed. Evidence shows that in a Saudi health care centre, 75% of consultations ended with a prescription, while health education took place in only 7.6% of the consultations (Al-Faris & Al-Taweel, 1999). These international figures emphasize the importance of health education programs at the community level in order to have a healthier population.The physician-patient relationship needs to be investigated in the population in order to improve the practice. Several physician–patient interaction models have been suggested to improve proper antibiotic prescribing decisions (Butler, et al., 2001). Barden et al. (1998) reported that parents believed that physicians’ cooperation in regards to listening to the patients concern, answering their questions, and explaining the reasons for treatment, will lead to their satisfaction even where antibiotics are not prescribed. Development of educational programs for physicians combined with community education is necessary to minimize the antibiotic misuse and the burden of bacterial resistance.
3.3.3. Socio-economic Status
- Socio-economic status needs to be considered as an important factor contributing to the rising issue of antibiotic misuse. Kozyrskyj et al. (2004) believed that inappropriate consumption of antibiotics is related to low socio-economic status, which might be associated to low education levels. Similarly, Matuz et al. (2005) suggest that poor socio-economic status is associated with antibiotic consumption in Hungary.On the other hand, it was argued that parents with high socio-economic status are more likely to request antibiotics, because of the parents believe that antibiotics treat URTIs faster, thus reducing the time taken off work (Braun & Fowles, 2000; Vanden Eng, et al., 2003). Braun & Fowles(2000) argued that full-time employed parents are more likely to request antibiotics. Results from the Vanden Eng et al. (2003) study shows that patients with higher socioeconomic status are more likely to consume antibiotics, which may be due to their better access to health care services. Although many researchers considered patients’ socioeconomic status as an important factor in the use of antibiotics (Braun & Fowles, 2000; Kozyrskyj, et al., 2004; Maria Matuz, et al., 2005; Vanden Eng, et al., 2003), there is a lack of worldwide information regarding the association between socioeconomic status and antibiotic use, therefore, it is important to study this association, as a contribution to the knowledge gaps.
3.3.4. Self-medication
- Self-medication was identified by Kunin et al.(1987) as self-administering inadequate doses of non-prescription medicines prior to doctors’ diagnosis. High rate of self-medication, especially antibiotic self-medication, may cause several problems to the child: it slows down children development, increases drug resistance, creates an unbalanced bacteria distribution, and leads to other side effects (Bi, Tongb, & Partonc, 2000). Moreover, studies have been conducted to measure the extent of parental self-medication to their children. In Turkey, Akici, Kalaca, Ugurlu, & Oktay(2004), found that almost 60% of parents had self-medicated their children before visiting the doctor. Likewise, Bi et al. (2000) found that almost 59% of children in China had parental self-medication. Furthermore, URTIs were the most common reasons for self-medication in Europe (Grigoryan, et al., 2007). It is necessary to consider the problem of self-medication when exploring factors influencing antibiotics misuse.Self-medication is more common in developing countries due to factors such as ready availability of antibiotics without prescription, the unrestricted access to antibiotics,lack of regulation over drugs, and physicians and pharmacists prescribing and dispensing antibiotics without regard to the cause of infection(Bawazir, 1992 ; Bi, Tong, et al., 2000; Cebotarenco & Bush, 2007; Grigoryan, et al., 2007; Le, et al., 2011). Bi et al. (2000) also studied factors associated with parental self-medication in China and found that well-educated mothers are more likely to self-medicate their child, parental self-medication usually increases with the age of the child, and severity of disease was related to parental self-medication (i.e. when the diseases were not serious self-medication and antibiotics misuse are more likely to occur). Grigoryan et al.(2007) reported that past experience with prescribed use of antibiotics triggers people to use self-medication. These factors may vary according to geographical locations, social behaviors, patients’ educational status, and cultural factors. Self-medication is an important issue in Saudi Arabia (Bawazir, 1992 ) and several adjacent countries such as Iran (Sarahroodi, et al., 2010), Jordan (Al-Azzam, et al., 2007; Al-Bakri, et al., 2005) and Sudan (Awad, et al., 2005). However, self-medication is a significantly growing public health issue in developed countries as well as developing countries (Bi, Tongb, et al., 2000). For example, a survey in USA showed that 54% of children had parental self-medication (Kogan, et al., 1994). Factors influencing this behavior (self-medication) in Saudi Arabia need to be measured in order to minimize to the overuse of antibiotics in children with URTIs and therefore reducing antibacterial resistance in the community.
3.4. Interventions to Prevent Overuse of Antibiotics
- Carefully planned and well-designed methodological intervention can result in behavior change for achieving the expected outcome. Several intervention protocols have been implemented around the world to reduce the overuse of antibiotics. It is important to investigate these worldwide intervention strategies and find the best protocol to be used in countries like Saudi Arabia according to the contributing factors to this overuse of antibiotics.
3.4.1 Health Education
- Evidence shows that careful health professional education in addition to patient awareness would be effective in reducing excessive use of antibiotics (Green, 2006; Panagakou, et al., 2011; Teng, et al., 2004). Public educational interventions may include: simple messages delivered by public relation campaigns, clinic-based education and community-wide educational materials (e.g. printed leaflets)(Belongia & Schwartz, 1998). All of these methods could be effective in delivering information about the use of antibiotics to the general population. There is a need for educational programs for physicians; Croft et al. (2007) suggested that physicians should receive evidence-based recommendations for diagnosis and treatment from professional societies, as well as feedback about their antibiotic use to facilitate behavior change. Although some methods were proven to be effective, some of the interventions targeting physicians were evidently ineffective. Arnold & Straus(2005) compared different intervention strategies around the world to find the most effective interventions in reducing the overuse of antibiotics: physicians’ printed educational materials, audits, and feedback were found to be ineffective, but educational meetings appeared to be more effective. Several studies have also found that multi-faceted interventions, directed at both patients’/guardians’ level and doctors’ level, are more successful in reducing the inappropriate use of antibiotics than a single intervention (Belongia, et al., 2002); Combining health care provider, patient, and public education after addressing local barriers to change(Arnold & Straus, 2005; Belongia & Schwartz, 1998; Gonzales, Barrett, Crane, & Steiner, 1998). Rising public and health care providers’ awareness regarding antibiotics is evidently effective in reducing antibiotic misuse. However, delivering such education may differ according to the setting where the intervention strategy is targeted.
3.4.2. Doctor-patient Communication
- Shared decision making has been shown to be an effective tool that can help in reducing overuse of antibiotics, where the physician provides clear information about the disease and treatment, and the patients provide their experience of the symptom and their beliefs, and knowledge about the treatment (Akici, et al., 2004; Butler, et al., 2001). This way both the patients’ guardians and the physician facilitate the decision-making process. Furthermore,Britten & Ukoumunne(1997) suggest that physicians may ask the patients or their guardians directly if they were hoping for an antibiotic, leading to the discussion of the reasons for such expectations. Moreover, Belongia & Schwartz(1998) believe that physicians should be convinced that patients’ satisfaction is based on communication more than prescription. Patient-physician communication is clearly important. Thus, interventions targeted at improving this communication may lead to a decrease in antibiotics overuse.
3.4.3. Changing Policies
- Some studies advocate developing organizational policies or review of existing ones, to support judicious use of antibiotics (Belongia & Schwartz, 1998; Radyowijati & Haak, 2003). While others, believe that a computerized antibiotic-management program can improve the overall quality of patient care(Evans, et al., 1998). The latter was confirmed by a seven year intervention study by Pestotnik et al. (1996), which found that using computer-based decision-making programs with specific guidelines brought about a remarkable reduction in antibiotic misuse and its associated cost. Furthermore, implementing a policy for delaying antibiotic prescription for 48 hours is another method that was suggested by Spurling, Del Mar, Dooley, & Foxlee(2006), this may give self-limiting conditions time to heal without using medications. Evidently this method is likely to be effective in reducing antibiotic use, however, it may as well reduce patient satisfaction. Although policy change is an effective method in reducing antibiotic overuse, targeted policies need to be reviewed before suggesting the intervention strategy in order to ascertain the aspects that need to be improved.
4. Conclusions
- Antibiotics misuse/overuse is an important public health issue that affects the community and the individual. Using antibiotics to treat children from upper respiratory tract infections is evidently inappropriate unless the infection was proven to be bacterial. This misuse of antibiotics, especially in children, will increase the risk of developing bacterial resistance which emphasis on the need to discover the contributing factors to this overuse of antibiotics. Factors influencing the misuse/overuse of antibiotics in the literature include (1) psychosocial factors, such as: behaviors, beliefs, and attitudes (e.g., self-medication & over-the-counter medication), (2) parents pressure, often documented by doctors, (3) demographic characteristics (e.g., socio-economic status, education levels) and (4) and lack of health education. Discovering the factors affecting the misuse/overuse of antibiotics in Saudi Arabia, whether they are patients’/ parents’-related or doctors’-related could assist in the development and implementation of a well-designed methodological intervention protocol that can lead to a decrease in antibiotics use. Interventions that could lead to the reduction in antibiotics overuse may include: (1) health education campaigns, professional education as well as public awareness campaigns are evidently effective in the reduction of the unnecessary use of antibiotics in children with upper respiratory tract infections. (2) Doctor-patients interactions, where the patient/parent gets involved in the decision making process with the doctor. And/or (3) policy change, such as: implementing a new policy for delaying antibiotics prescription for 48 hours which will give the self-limiting conditions to time to heal without the use of medications. Choosing the best intervention protocol relays on discovering the most influencing factor(s) associated with this overuse.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-Text HTML
Full-Text HTML