-
Paper Information
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2026; 16(4): 2196-2198
doi:10.5923/j.ajmms.20261604.132
Received: Apr. 3, 2026; Accepted: Apr. 26, 2026; Published: Apr. 29, 2026

Optimization of Radiological Diagnostic Methods in the Treatment of Chronic Apical Periodontitis Using Bioactive Glass Osteotropic Paste
Juraeva Nigora Iminjonovna1, Avzal Akbarov Nigmatullaevich2
1Andijan State Medical Institute, Andijan, Uzbekistan
2Tashkent Medical University, Tashkent, Uzbekistan
Correspondence to: Juraeva Nigora Iminjonovna, Andijan State Medical Institute, Andijan, Uzbekistan.
| Email: |  |
Copyright © 2026 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

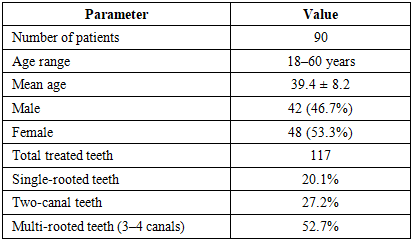
Chronic apical periodontitis is one of the most common inflammatory diseases of periapical tissues caused by infection of the root canal system. The aim of this study was to optimize radiological diagnostic methods for the conservative treatment of chronic apical periodontitis using a paste based on bioactive glass. The study included 90 patients aged 18–60 years with destructive forms of apical periodontitis. A total of 117 teeth were treated. Radiological evaluation was performed using digital radiography and cone-beam computed tomography with assessment according to the PESS scale before treatment and after 1, 3, 6 and 12 months. The results demonstrated a significant decrease in PESS scores in patients treated with bioactive glass, particularly when combined with platelet-rich plasma. After 12 months, the reduction of PESS reached 89.6%, accompanied by radiological signs of bone regeneration.
Keywords: Chronic apical periodontitis, Radiological diagnostics, Bioactive glass, Endodontic treatment, PESS scale
Cite this paper: Juraeva Nigora Iminjonovna, Avzal Akbarov Nigmatullaevich, Optimization of Radiological Diagnostic Methods in the Treatment of Chronic Apical Periodontitis Using Bioactive Glass Osteotropic Paste, American Journal of Medicine and Medical Sciences, Vol. 16 No. 4, 2026, pp. 2196-2198. doi: 10.5923/j.ajmms.20261604.132.
Article Outline
1. Introduction
- Chronic apical periodontitis is one of the most prevalent inflammatory diseases affecting periapical tissues and remains a major cause of tooth loss worldwide. The condition typically develops as a consequence of microbial infection of the root canal system, leading to progressive destruction of periapical bone structures and inflammatory changes in the surrounding tissues. Early detection and accurate evaluation of these pathological processes are essential for effective treatment planning and prognosis assessment in endodontic practice.Radiological examination remains the cornerstone of diagnostic evaluation in patients with suspected apical periodontitis. Conventional intraoral radiography is widely used due to its accessibility and relatively low radiation dose. However, the two-dimensional nature of radiographic images limits diagnostic accuracy, particularly in cases where anatomical structures overlap or lesions are confined within cancellous bone. As a result, early stages of bone destruction may remain undetected using conventional radiographic methods.In recent years, cone-beam computed tomography (CBCT) has significantly improved the diagnostic capabilities of dental imaging by providing three-dimensional visualization of dental and maxillofacial structures. CBCT imaging allows more precise identification of periapical lesions and assessment of the extent of bone destruction compared with traditional radiography. Several studies have demonstrated that CBCT can detect a higher number of periapical lesions that are not visible on periapical radiographs, thereby improving diagnostic sensitivity and treatment planning [2].In addition to improved visualization, modern research increasingly focuses on the quantitative assessment of bone tissue changes using radiographic densitometry and standardized radiological indices. One of the most promising tools is the Periapical and Endodontic Status Scale (PESS), which integrates evaluation of periapical bone lesions and the technical quality of endodontic treatment. The PESS system allows objective monitoring of treatment outcomes and has demonstrated prognostic value for predicting the success of endodontic therapy [9]. At the same time, regenerative approaches in endodontics have gained increasing attention. Bioactive materials capable of stimulating osteogenesis and promoting tissue regeneration are being actively investigated as adjuncts to conventional endodontic therapy. Bioactive glass materials demonstrate osteoconductive and osteostimulating properties, facilitating bone regeneration in areas of periapical destruction. The addition of biological stimulators such as platelet-rich plasma (PRP) further enhances tissue healing due to the presence of growth factors involved in bone regeneration.Despite significant progress in endodontic technology and imaging methods, the optimization of diagnostic protocols and evaluation criteria remains an important research objective. Combining modern imaging techniques with standardized radiological indices may significantly improve the accuracy of diagnosis and the evaluation of treatment outcomes [6].Therefore, further clinical studies aimed at optimizing radiological diagnostic methods and assessing the effectiveness of regenerative materials in endodontic therapy are of considerable scientific and clinical interest.
2. Aim of the Study
- To optimize radiological diagnostic methods for evaluating the effectiveness of conservative treatment of chronic apical periodontitis using osteotropic paste based on bioactive glass.
3. Materials and Methods
- The study included 90 patients aged 18–60 years diagnosed with destructive forms of chronic apical periodontitis. Among them, 42 (46.7%) were men and 48 (53.3%) were women. A total of 117 teeth were treated during the study period.Patients were divided into two main groups according to the treatment method.In Group I, endodontic treatment included transapical placement of an osteotropic filling material based on bioactive glass into the periapical lesion area. The group was further divided into two subgroups:Subgroup Ia – bioactive glass mixed with sterile sodium chloride solution (0.9%)Subgroup Ib – bioactive glass combined with platelet-rich plasma (PRP)In Group II, delayed endodontic treatment was performed using calcium hydroxide and iodoform paste (Metapex).Radiological evaluation was performed using digital periapical radiography, orthopantomography and cone-beam computed tomography. The effectiveness of treatment was assessed using the PESS (Periapical and Endodontic Status Scale) before treatment and after 1, 3, 6 and 12 months.
|
|
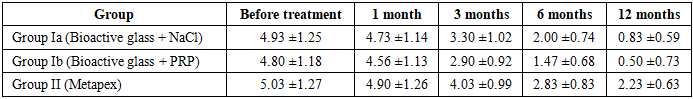
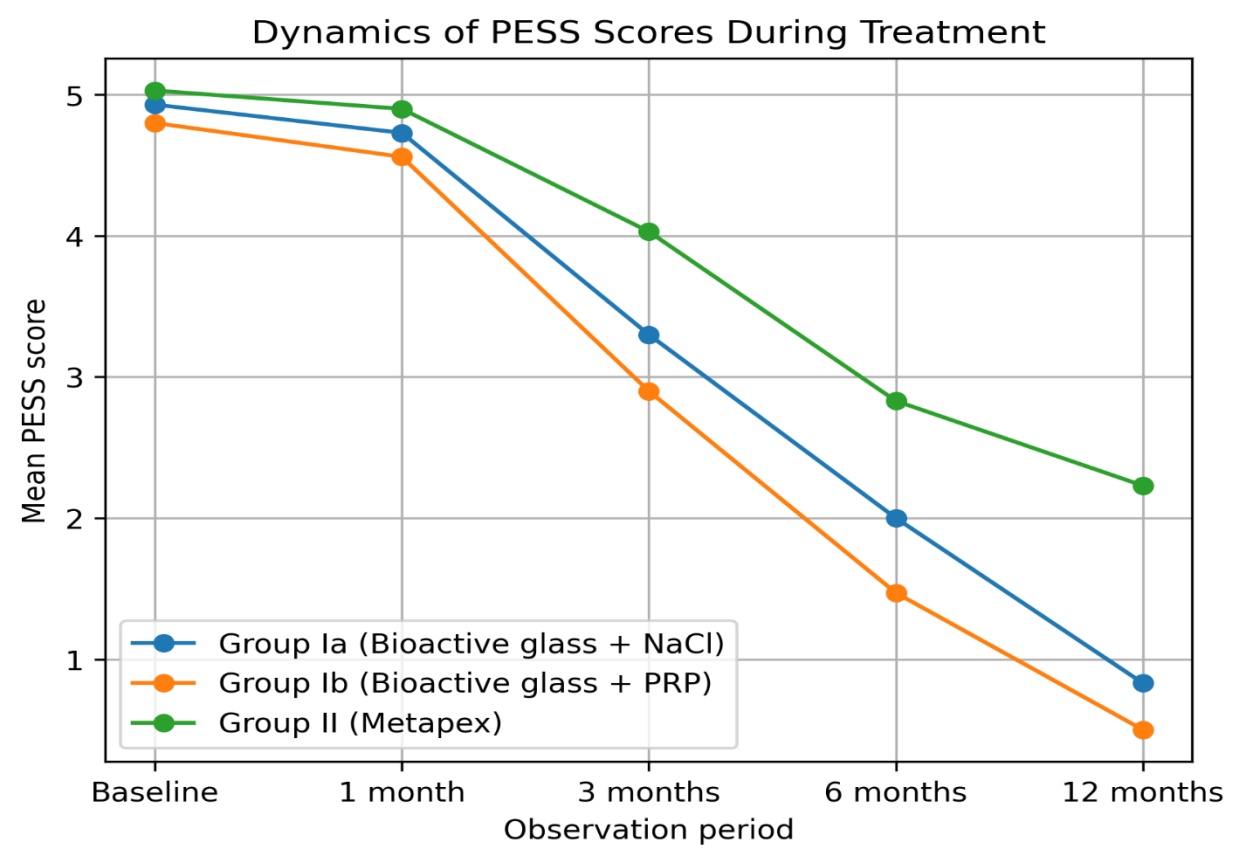 | Figure 1. Dynamics of mean PESS scores during treatment |
4. Results
- Before treatment, high PESS scores were observed in all study groups, indicating severe periapical pathology and unsatisfactory endodontic status.The greatest improvement was observed in subgroup Ib, where bioactive glass was combined with platelet-rich plasma. After 12 months, the total PESS score decreased from 4.8 to 0.5, indicating almost complete healing of the periapical lesion.Subgroup Ia also demonstrated significant improvement, although the dynamics of healing were slightly slower.The comparison group treated with Metapex showed a slower reduction in PESS scores and persistent radiological signs of inflammation in several cases.
5. Discussion
- The obtained results demonstrate that osteotropic therapy using bioactive glass significantly enhances bone regeneration in periapical tissues. The addition of platelet-rich plasma further stimulates osteogenesis and accelerates healing processes.The findings are consistent with previous studies reporting improved outcomes when regenerative materials are used in endodontic treatment of destructive periapical lesions.
6. Conclusions
- The use of bioactive glass osteotropic paste, particularly in combination with platelet-rich plasma, significantly improves the effectiveness of conservative treatment of chronic apical periodontitis.Radiological evaluation using modern imaging methods combined with the PESS scale allows objective assessment of treatment outcomes and provides reliable monitoring of bone regeneration in periapical tissues.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML