-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2026; 16(4): 2109-2111
doi:10.5923/j.ajmms.20261604.111
Received: Apr. 8, 2026; Accepted: Apr. 23, 2026; Published: Apr. 28, 2026

The Role of Prognostic Biomarkers for Neurological Complications in Hyperbilirubinemia in Newborns VEGF and BDNF as Prognostic Markers of Neurological Complications in Hyperbilirubinemia
Salikhova K. Sh., Bakhramova Sh. M.
Republican Specialized Scientific and Practical Medical Center of Pediatrics, Uzbekistan
Copyright © 2026 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

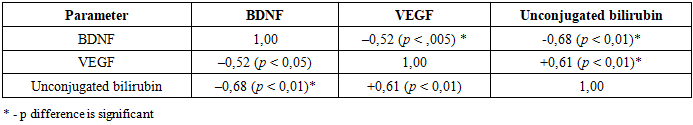
Objectives: Neonatal hyperbilirubinemia is a significant risk factor for bilirubin-induced damage to the central nervous system. Disruptions in neurovascular homeostasis, accompanied by an imbalance of angiogenic and neurotrophic factors, including vascular endothelial growth factor (VEGF) and brain-derived neurotrophic factor (BDNF), play an important role in the pathogenesis of this condition. The aim of the study was to assess the prognostic significance of serum VEGF and BDNF levels in the development of neurological complications in newborns with hyperbilirubinemia. Methods: A total of 135 newborns were included in this prospective study. VEGF and BDNF concentrations were determined using ELISA. A correlation analysis was performed to assess the relationship between these biomarkers and bilirubin levels as well as clinical neurological abnormalities. Results: It was found that elevated VEGF and decreasd BDNF were significantly associated with the severity of hyperbilirubinemia and adverse neurological outcomes. VEGF correlated positively with unconjugated bilirubin levels (r = 0.61; p < 0.01), whereas BDNF demonstrated a negative correlation (r = –0.68; p < 0.01). Conclusions: The data confirm that VEGF and BDNF are promising prognostic biomarkers for the risk of bilirubin-induced neurotoxicity.
Keywords: Hyperbilirubinemia, Newborn, Neurotoxicity, Bilirubin, Biomarkers
Cite this paper: Salikhova K. Sh., Bakhramova Sh. M., The Role of Prognostic Biomarkers for Neurological Complications in Hyperbilirubinemia in Newborns VEGF and BDNF as Prognostic Markers of Neurological Complications in Hyperbilirubinemia, American Journal of Medicine and Medical Sciences, Vol. 16 No. 4, 2026, pp. 2109-2111. doi: 10.5923/j.ajmms.20261604.111.
1. Introduction
- Hyperbilirubinemia is one of the most common conditions of the neonatal period and can lead to bilirubin-induced damage to the central nervous system [1,2]. Unconjugated bilirubin is capable of crossing the blood-brain barrier, causing neurotoxic effects accompanied by damage to neurons, glial cells, and disruption of synaptic connections [3,4].Current understanding points to a multifactorial pathogenesis involving oxidative stress, inflammation, mitochondrial dysfunction, and endothelial dysregulation [2,5]. Disruption of the neurovascular unit plays a particular role. Among the molecular mediators involved in the regulation of neurovascular homeostasis, vascular endothelial growth factor (VEGF) and brain-derived neurotrophic factor (BDNF) play key roles [6–9]. VEGF regulates angiogenesis, vascular permeability, and endothelial activation, facilitating adaptive responses to hypoxia and tissue damage [6,7]. However, its overexpression may contribute to disruption of the blood-brain barrier and exacerbation of neuroinflammatory processes [7]. BDNF, in turn, is one of the most important neurotrophins, regulating neuronal survival, differentiation, synaptic plasticity, and neurogenic processes [8,9]. Decreased BDNF levels are associated with increased vulnerability of neural tissue to toxic and ischemic effects [9,12]. An imbalance between angiogenic and neurotrophic factors may reflect the degree of disruption in compensatory mechanisms during hyperbilirubinemia and be associated with the risk of neurological complications. However, the prognostic significance of changes in VEGF and BDNF levels in hyperbilirubinemia remains insufficiently studied to date.Objective. To investigate the prognostic significance of vascular endothelial growth factor (VEGF) and brain-derived neurotrophic factor (BDNF) in the development of neurological complications in hyperbilirubinemia in newborns.
2. Materials and Methods
- A prospective observational study was conducted in the Department of Neonatal Pathology at the Republican Specialized Scientific and Practical Medical Center of Pediatrics. A total of 135 newborns were examined, including: the main group—115 full-term newborns with prolonged unconjugated hyperbilirubinemia aged 14 days to 1.5 months; and the control group—20 essentially healthy full-term newborns without jaundice. Inclusion criteria: Full-term newbornsUnconjugated hyperbilirubinemia >220 μmol/LExclusion criteriaIntrauterine infectionsCongenital anomaliesABO, Rh The mean level of unconjugated bilirubin in the main group by the end of the second week of life was 256.9 ± 21.7 μmol/L. Serum concentrations of VEGF and BDNF were determined by quantitative enzyme-linked immunosorbent assay (ELISA) using standard commercial kits in accordance with the manufacturer’s instructions. Student’s t-test was used for statistical analysis. Correlations were calculated using Pearson’s correlation coefficient. Prognostic value was assessed using ROC analysis with AUC calculation.
3. Results and Discussion
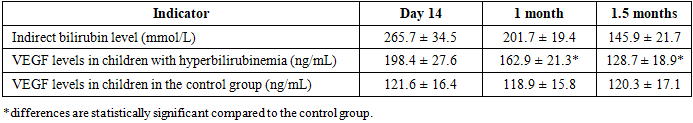
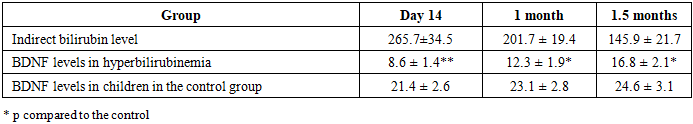
- The study found that newborns with prolonged unconjugated hyperbilirubinemia exhibited significant changes in neuromolecular markers. The levels of bilirubin and VEGF over the course of observation are presented in Table 1.
|
|
|
4. Conclusions
- Thus, the obtained data allow us to consider bilirubin-induced brain damage in newborns as a multilevel pathological process [2,5]. A comprehensive assessment of these biomarkers allows not only for the detection of early signs of subclinical central nervous system damage but also for the stratification of the risk of adverse neurological outcomes in newborns with severe hyperbilirubinemia. Thus, the obtained data allow us to consider bilirubin-induced brain damage in newborns as a multilevel pathological process, including: direct toxic damage to neurons, reactive activation of glial cells, disruption of the blood-brain barrier, and suppression of neurotrophic support and neuroplasticity.A comprehensive assessment of these biomarker data allows not only for the identification of early signs of subclinical central nervous system damage but also for the identification of risk factors for adverse neurological outcomes in newborns with severe hyperbilirubinemia [6–9].
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML