Narzullaev Nuriddin Umarovich, Safarov Samadjon Sodiqovich
Bukhara State Medical Institute named after Abu Ali Ibn Sino, Bukhara, Uzbekistan
Correspondence to: Narzullaev Nuriddin Umarovich, Bukhara State Medical Institute named after Abu Ali Ibn Sino, Bukhara, Uzbekistan.
| Email: |  |
Copyright © 2026 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Abstract
Clinical, neurological and diagnostic studies were conducted on the basis of the Department of Neurology of the RNCMPF. We examined 33 patients with a confirmed diagnosis of type 1 diabetes from 28 to 38 years old, the average age was 24.79±2.88 years, who were in a state of compensation or subcompensation of carbohydrate metabolism. Of these, there were 12 men (36.36%), 21 women (63.63%), the average duration of the disease was 24.96=3.49 years. The main group was divided into two subgroups according to the duration of the disease. Patients with DM duration of less than 3 years were included in the I-th group 15 (47%), patients with experience of more than 3 years 18 (32%) in the II-th subgroup. The control group included 23 healthy people of comparable age, on average 12.42±2.69, of whom 10 (43.47%) men and 13 (56.52%) women with undisturbed carbohydrate metabolism and without chronic and acute diseases.
Keywords:
Neurocognitive disorders, Diabetes mellitus, Carbohydrate metabolism and without chronic and acute diseases
Cite this paper: Narzullaev Nuriddin Umarovich, Safarov Samadjon Sodiqovich, Diabetes Mellitus and Cognitive Impairment, American Journal of Medicine and Medical Sciences, Vol. 16 No. 3, 2026, pp. 955-958. doi: 10.5923/j.ajmms.20261603.23.
1. Introduction
Diabetes mellitus is considered one of the most urgent health problems, as it appears to be the cause of many complications of various organs and systems. The central nervous system is no exception, which, according to many authors, is affected already at the initial stages of the disease. On the part of the brain, diabetes has complications in the form of cognitive impairment 20-70% more than in healthy people, and the risk of developing dementia is 5% higher. According to the International Diabetes Federation, by 2045, the number of patients with diabetes in the world will increase to 628.6 million people, while in most countries there is a documented increase in the incidence of type 1 diabetes in patients [4,6,8,11,14]. It is known that type 1 is usually detected, that is, during the most rapid development of the central nervous system, and naturally, during this period, the young brain is more susceptible to frequent fluctuations in glycemia. The manifestation of type 1 diabetes in preschool and school age may contribute to the early onset of cognitive impairment, such as decreased memory and attention. In the scientific work of Duarte J.M.N. (2015) it was demonstrated that diabetes invariably contributes to the development of cognitive changes, which at a young age can manifest (and in most cases manifest) moderately, and with increasing age of patients, duration of diabetes, as well as with insufficient glycemic control, tend to increase [1,2,9,12,15].The issue of diagnosing subclinical forms of central nervous system damage, in order to carry out early and adequate correction in order to prevent the manifestation of its severe manifestations, is very relevant. The most significant brain disorders in type 1 diabetes in children include subclinical memory and attention disorders, which require appropriate neuropsychological testing. Neuropsychological research provides an opportunity to obtain additional diagnostic criteria for assessing the severity and nature of cognitive dysfunction, as well as to determine the effectiveness of various therapeutic and rehabilitation measures carried out by patients [3,5,7,10,13].The aim of the study was to study the cognitive characteristics of the brain in patients with type 1 diabetes mellitus.
2. Materials and Methods of Research
Clinical, neurological and diagnostic studies were conducted on the basis of the Department of Neurology of the RNCMPF. We examined 33 patients with a confirmed diagnosis of type 1 diabetes from 28 to 38 years old, the average age was 24.79±2.88 years, who were in a state of compensation or subcompensation of carbohydrate metabolism. Of these, there were 12 men (36.36%), 21 women (63.63%), the average duration of the disease was 24.96=3.49 years. The main group was divided into two subgroups according to the duration of the disease. Patients with DM duration of less than 3 years were included in the I-th group 15 (47%), patients with experience of more than 3 years 18 (32%) in the II-th subgroup. The control group included 23 healthy people of comparable age, on average 12.42±2.69, of whom 10 (43.47%) men and 13 (56.52%) women with undisturbed carbohydrate metabolism and without chronic and acute diseases (Fig. 1).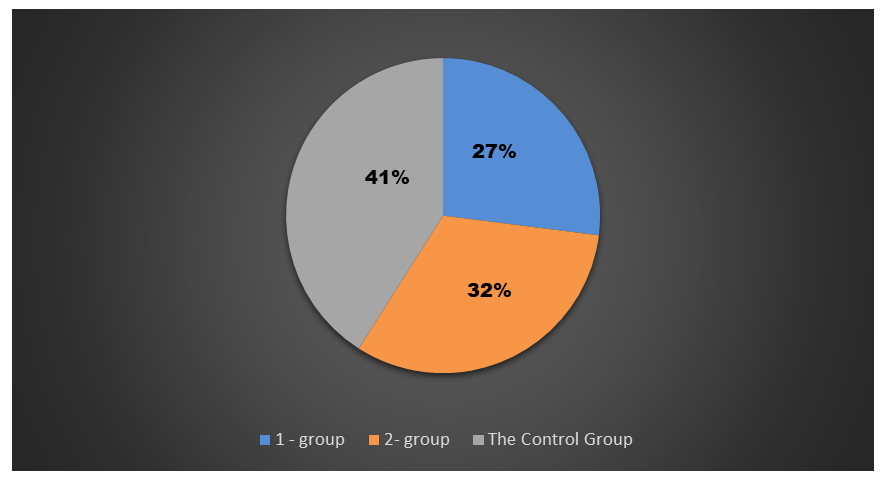 | Figure 1. Distribution of patients by groups |
The criteria for inclusion of patients in the study were as follows: Ø the presence of clinically manifest diabetes mellitus; Ø conducting regular insulin therapy with genetically engineered human insulin preparations or insulin analogues; Ø the possibility of regular self - monitoring of glycemic levels; awareness of the patient and his parents within the framework of the educational program "Schools of diabetes mellitus"; Ø the state of optimal (H1C < 9.0%) glycemic control of diabetes mellitus at the time of the study (according to ISPAD Consensus Guidelines, 2000);The criteria for excluding patients were as follows: Ø the presence of decompensation of carbohydrate metabolism at the time of the study; Ø the presence of severe organic neurological, mental or somatic diseases at the time of the study; Ø the lack of the possibility of regular self - monitoring of glycemic levels; origin from an antisocial environment. Clinical, neurological and neuropsychological examinations were conducted, anamnestic data on the severity of diabetes, the number of comas, and the course of the perinatal period were clarified. Psychological testing was standardized by place and time. The study of memory was carried out using the "10 words" technique with the determination of indicators of the volume of short-term arbitrary auditory-speech memory in accordance with age norms in points, the presence of repetitions and additional words during playback, and an assessment of the memorization curve. The study of the sphere of attention was evaluated using the Bourdon proof-reading test. In order to objectify affective disorders, the following psychometric tests were used. The Spielberger Test (1972) provides an opportunity to assess personal (LT) and reactive (RT) anxiety. To diagnose the presence of vegetative dystonia syndrome (SVD), the following were used: "Questionnaire for detecting signs of vegetative disorders", consisting of 11 items, filled in by the patient (if the total number of points is equal to or more than 15, the presence of SVD was assumed); "A study scheme for detecting signs of vegetative disorders", consisting of 13 points, filled in by a doctor (the total score obtained should not exceed 25 in healthy individuals).
3. The Results of the Study and Their Discussion
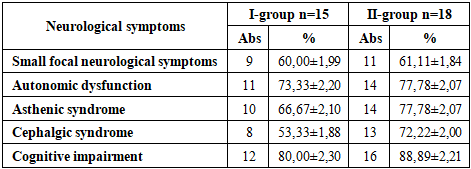
During the neurological examination of patients suffering from type 1 diabetes mellitus, various clinical syndromes of cerebral disorders were identified in patients of both groups (Table 1). The most common of which was the syndrome of cognitive dysfunction. Moderate cognitive impairment was diagnosed in the presence of complaints from patients about reduced intelligence, memory loss, unstable attention and was noted in group I in 80.00%, in group II in 88.89% of cases. The study of ANS showed dysregulation of vegetative processes in patients with both a predominance of the sympathetic and parasympathetic nervous systems. Vegetative dysfunction was observed in 73.33% of children in group I and 77.78% in group II, which manifested themselves most often in several anatomical and physiological systems and were accompanied by active somatic complaints. The asthenic symptom complex observed in patients of both groups – 66.67% and 77.78%, respectively, manifested itself in the form of increased fatigue and exhaustion, mood lability, sleep disorders. The development of this syndrome is associated with the depletion of the functional capabilities of the nervous system due to auto-intoxication, impaired blood supply to the brain and metabolism in brain tissue.Table 1. Frequency of neurological syndromes in patients with DM-1
 |
| |
|
Another very common neurological disorder is cephalic syndrome, which was detected in 53.33% of the examined patients with diabetes duration less than 3 years and 72.22% of patients with diabetes experience of more than 3 years. In most patients of both groups, the structure of the cephalgic syndrome was dominated by headaches corresponding to tension headaches: dull, aching, squeezing (squeezing like a "vise" or "helmet"), more often bilateral, sometimes with a predominance in the frontal-parietal and frontal-temporal regions, sometimes radiating into the temples from both sides, the face, shoulders, which is explained by the tension of the pericranial and cervical muscles, which are intensified by psycho-emotional stress, as a rule, in the afternoon. Less often, mainly in older patients, headaches of a pulsating nature were detected: unilateral, localized in the frontal-temporal-orbital region, paroxysmal, intense accompanied by nausea, hypersensitivity to light and sound stimuli. The formation of cephalgic syndrome is caused by the disintegration of non-specific brain systems under the influence of provoking factors: stress, dishormonal disorders, as well as fluctuations in the level of glycemia. Small-focal neurological symptoms were observed in group I – 60.00% and in group II - 61.11%. The most common manifestations were in the form of fine-grained nystagmus, hyperkinesis of the tip of the tongue, diffuse decrease in muscle tone, revived reflexes, tremor of the fingers of the upper extremities and hypesthesia of the distal parts of the lower extremities. After conducting clinical trials, all patients and children from the control group underwent neuropsychological testing to study in more detail the state of memory, attention and thinking functions. Pathological and low values of attention accuracy according to 2 indicators - the volume and stability of attention in patients with DM were determined in group I in 46.67% of patients, in group II in 66.67%, memory impairment according to 7 criteria: short–term memory - the volume of reproduction of auditory-speech memory after three times repetition, the volume of delayed reproduction, the volume of short-term visual verbal memory, the volume of delayed visual verbal memory, immediate memory, operative memory, and the success of spatial memory were noted in group I in 60% of patients, in II- in the group of 77.78% of patients, there was also a decrease in 5 indicators of thinking: the level of generalization, the ability to identify specific signs, conceptual thinking, task completion time and the number of associations. In total, the average values were 66.67% in the I-group and 72.22% in the II-group. Patients of both groups were unable to achieve a 100% result when performing neuropsychological testing. The presence of cognitive deficits according to the average total values in this case has a mild and moderate degree of severity (Fig. 2).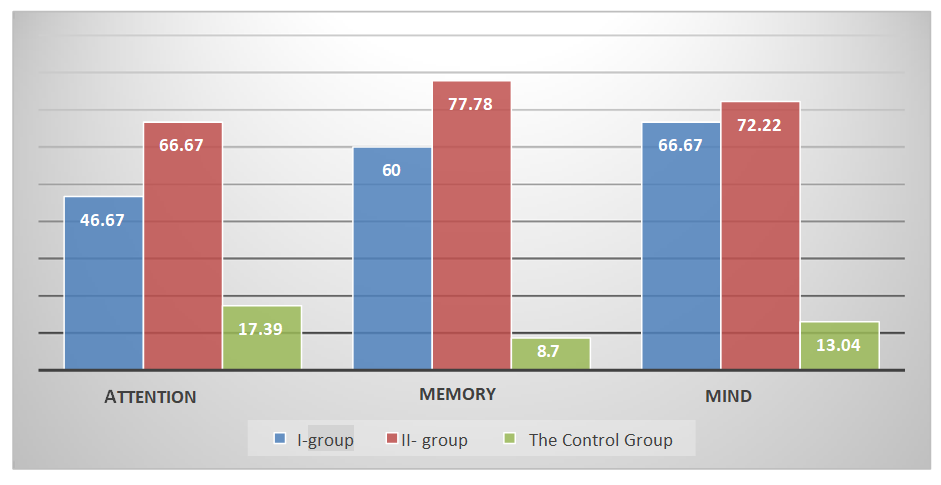 | Figure 2. Indicators of cognitive status |
The study of emotional stability using the Spielberger Khanin test revealed increased indicators of personal anxiety were determined in all examined children, regardless of age, gender and duration of diabetes. A fairly high level of personal anxiety in children and adolescents with diabetes mellitus indicates their constitutional sensitivity to stress and a tendency to experience negative emotions associated with various difficulties much more acutely than their healthy peers. This can cause a more labile course of DM and, consequently, a much more pronounced lesion of the non-specific regulation systems of the brain, which are part of the limbic system and are the anatomical substrate of emotions. In addition, prolonged overstrain of the processes of nervous activity with continuous irritation of the structures of the limbic-reticular complex (LRC) leads to increased activity of the hippocampus with a weakening of control from the anterior regions of the cerebral cortex.Thus, despite the presence of optimal and suboptimal metabolic control of the disease, all examined patients with DM, according to clinical neurological and neuropsychological examination, had clinical manifestations of cerebral disorders: small-focal neurological symptoms, autonomic dysfunction, cephalgic and asthenic syndromes. Also, in children with type 1 diabetes, a high incidence of cognitive disorders was revealed, which are the main cerebral disorders in diabetes, while with an increase in the duration of the disease, which tend to increase.
4. Conclusions
Cognitive dysfunctions against the background of concomitant anxiety and depressive disorders negatively affect good and long-term glycemic control, in addition, they have a significant impact on social activity, work capacity and quality of life of patients. In solving this problem, a promising direction is to study the pathogenesis of cognitive impairment from the standpoint of determining the role of neurospecific proteins and proton magnetic resonance spectroscopy indicators, as well as the features of interaction between them in the formation of brain damage in diabetes mellitus in children and adolescents. The results obtained will provide an opportunity to deepen existing understanding of the processes that form the basis of central nervous system damage in DM, and to substantiate new approaches to the diagnosis, prevention and correction of cerebral disorders.
References
| [1] | Dedov I.I., Shestakova M.V. Algorithms of specialized medical care for patients with diabetes mellitus. 7th issue. // Diabetes mellitus. 2015. No. 1. - pp. 1-112. |
| [2] | Mikhailova E.A. Clinical and pathogenetic features of the formation of psychopathological disorders in children with severe diabetes mellitus: dis. ... Doctor of Medical Sciences: cipher spec. 14.01.06. Kharkiv, 2016. –p. 250. |
| [3] | Puzikova O.Z. Clinical and pathogenetic aspects of the formation of cerebral disorders in type 1 diabetes mellitus in children and adolescents: dis. ... Doctor of Medical Sciences: cipher spec. 14.01.08. Rostov-on-Don, 2019. –p. 299. |
| [4] | Sidorova N.S. Diagnosis and therapy of early stages of diabetic encephalopathy: abstract. ... candidate of Medical Sciences: cipher spec. 14.01.11 / St. Petersburg State Medical University named after Academician I.P. Pavlov. St. Petersburg, 2004. – p. 20. |
| [5] | Arbelaez A.M. Glycemic extremes in youth with T1DM: the structural and functional integrity of the developing brain / A.M. Arbelaez, K. Semenkovich, T. Hershey // Pediatric Diabetes. – 2013. – Vol. 14. – P. 541–553. |
| [6] | Duarte J.M.N. Metabolic Alterations Associated to Brain Dysfunction in Diabetes / J.M.N. Duarte // Agingand Disease. – 2015. – Vol. 6, № 5. – P. 304–321. |
| [7] | Gohel M.G. Evaluation of glycemic control in patients with type 2 diabetes mellitus with and without microvascular complications International. Journal of Pharma and Bio Sciences. 2013; 4. (4): - p. 794–802. |
| [8] | Jash K., Gondaliya P., Kirave P., Kulkarni B., Sunkaria A., Kalia K. Cognitive dysfunction: A growing link between diabetes and Alzheimer’s disease. Drug. Dev. Res. 2019; 81: - Pp. 144-64. |
| [9] | Naguib J.M., Kulinska E., Lomax C.L. Neuro-cognitive performance in children with type 1 diabetes – a meta-analysis // J. Pediatr. Psychol. 2009. Vol. 34(3). P. 271-282. |
| [10] | Northam E.A., Rankins D., Lin A. Central nervous system function in youth with type 1 diabetes after 12 years after onset // Diabetes Care. 2009. Vol. 32(3). -P. 445-450. |
| [11] | Haeusler K.G., Schmidt W.U., Fohring F., Meisel C., Helms T., Jungehulsing G.J., Nolte C.H., Schmolke K., Wegner B., Meisel A., Dirnagl U., Villringer A., Volk H.D. Cellular immunodepression preceding infectious compli- cations after acute ischemic stroke in humans // Cere- brovasc. Dis. 2008. Vol. 25, № 1-2. - Р. 50–58. |
| [12] | Hug A., Dalpke A., Wieczorek N., Giese T., Lorenz A., Auffarth G., Liesz A., Veltkamp R. Infarct volume is a major determiner of post-stroke immune cell function and susceptibility to infection. // Stroke. 2009. Vol. 40, №10. - P. 3226–3232. |
| [13] | Narzullaev N.U., Raxmatov A.A. Immunological aspects of diagnosis and treatment of sick children with chronic purulent medium otititis on the background of chronic hepatitis в // Journal for New Zealand Herpetology. vol. 2023. - P. 1590-1594. |
| [14] | Narzullaev N.U., Kurbanov M.K. Clinical and immunological features of the course of acute otitis media in children with type 1 diabetes mellitus // Journal of Advenced Zoology. vol. 44. 2023. - P. 282-286. |
| [15] | Narzullaev N.U. Prevalence analysis incidence of upper respiratory COVID-19 infekted patientis // International journal of Health systems and medical sciences. vol. 2 / jul. 2023. - P. 70-72. |




 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML