-
Paper Information
- Next Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2026; 16(2): 712-715
doi:10.5923/j.ajmms.20261602.67
Received: Nov. 22, 2025; Accepted: Dec. 16, 2025; Published: Feb. 26, 2026

Evaluating Educational and Behavioral Shifts Under Modular Credit System in Medical University Setting
Zafar Zayirovich Aminov
Samarkand State Medical University, Uzbekistan
Correspondence to: Zafar Zayirovich Aminov, Samarkand State Medical University, Uzbekistan.
Copyright © 2026 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The introduction of the Modular Credit System (MCS) in Uzbekistan's higher education system represents a pivotal reform aimed at aligning with international standards, particularly the Bologna Process. Its relevance is heightened in medical education due to the intensive curricula and high demands on clinical competence. Objective. To assess the academic, behavioral, and digital engagement outcomes of students following the implementation of the MCS at Samarkand State Medical University. Materials and Methods. A retrospective comparative study was conducted on two cohorts of undergraduate students (n=160 each) from the 2018/2019 (pre-MCS) and 2022/2023 (post-MCS) academic years. Academic data were extracted from institutional records, including GPA, academic debts, attendance rates, digital resource usage, and module exam attempts. Results. Implementation of MCS resulted in significant improvements in academic performance: mean GPA increased from 3.58 to 3.89 (p<0.001); students with GPA ≥4.0 rose from 34.4% to 54.4% (p<0.001); academic debts decreased from 16.3% to 8.8% (p=0.036). Attendance rates and digital resource engagement also improved markedly. First-attempt success in module exams increased from 61.3% to 78.8% (p<0.001), while the number of repeated attempts declined. Conclusion. The MCS significantly enhanced student performance, engagement, and digital integration, supporting its adoption as an effective educational reform in medical training.
Keywords: Modular Credit System, Medical education, Academic performance, Digital learning, Curriculum reform
Cite this paper: Zafar Zayirovich Aminov, Evaluating Educational and Behavioral Shifts Under Modular Credit System in Medical University Setting, American Journal of Medicine and Medical Sciences, Vol. 16 No. 2, 2026, pp. 712-715. doi: 10.5923/j.ajmms.20261602.67.
1. Introduction
- The implementation of the Modular Credit System (MCS) in the higher education system of Uzbekistan has become part of a large-scale transformation of the educational landscape initiated by the state to enhance academic mobility, transparency, and the international competitiveness of graduates [1]. A key driver of these reforms was the Republic of Uzbekistan’s accession to the Bologna Process and its active movement toward integration into the global higher education space [2,3].The formal foundation for the transition to the MCS was laid by resolutions of the Cabinet of Ministers of the Republic of Uzbekistan and orders issued by the Ministry of Higher Education, Science and Innovation—most notably, Cabinet Resolution No. 607 of October 24, 2020, “On Measures for the Implementation of the Credit-Module System in Higher Education Institutions,” and Order No. 87 of January 26, 2021, which regulates credit calculation standards and their distribution across academic disciplines [4].The MCS is based on the calculation of academic workload in credits (learning units), where one credit equals 30 academic hours. Unlike the traditional model, in which evaluation occurs primarily at the end of the semester, the modular credit system implies phased, module-based assessment throughout the learning process. This approach ensures greater flexibility in students’ educational trajectories, fostering autonomy and a higher level of responsibility for their own learning [1,5,6].The transition to the MCS has gained particular importance in medical education, where the length of study, the intensity of the curriculum, and the critical responsibility of developing clinical competence require a carefully structured approach [7,8,9]. At Samarkand State Medical University (SSMU), one of the country’s leading medical institutions, the phased implementation of the MCS began in 2020, starting with first-year students. By 2023, nearly all undergraduate and postgraduate programs had transitioned to the modular credit format.A significant context for the MCS introduction in medical universities was the urgent need to modernize approaches to clinical reasoning development, as the traditional lecture-seminar format demonstrated limited capacity [10,11]. Thus, reforming the educational model through MCS has become both a technical and substantive transformation—a platform for implementing active, digital, and simulation-based learning methods.Research Objective. To assess the impact of implementing the modular credit system (MCS) on the academic performance of students at Samarkand State Medical University.
2. Materials and Methods
- A retrospective comparative analysis was conducted, involving two student cohorts: the 2018/2019 academic year (prior to the implementation of the MCS) and the 2022/2023 academic year (following its full-scale implementation). Each cohort included 160 students, matched by gender, age, faculty affiliation, and academic program.Data were collected from the official university database, which included individual academic performance records, attendance statistics, the number of academic debts, the number of attempts to pass module assessments, and the frequency of use of electronic learning platforms (such as Moodle, Zoom, etc.).Indicators and Variables. The primary quantitative variables included: the average annual grade point average (GPA); the percentage of students achieving a GPA of 4.0 or higher; the proportion of students with academic debts; the attendance rate for in-person classes (%); the share of students using digital learning resources; and the number of module attempts (first, second, or more).Statistical Analysis. To assess the normality of data distribution, the Shapiro–Wilk test was applied. For normally distributed data, comparisons were made using the independent samples Student's t-test. In cases of non-normal distribution, the non-parametric Mann–Whitney U test was used. Categorical variables were analyzed using the chi-square (χ²) test. Statistical significance was set at p<0.05. All calculations were performed using SPSS Statistics software, version 25.0 (IBM Corp., USA).
3. Results
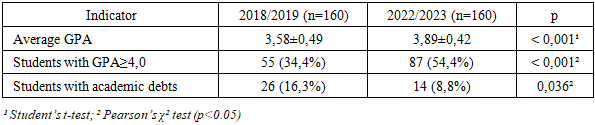
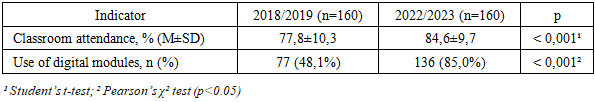
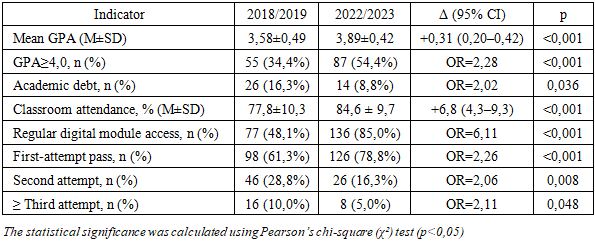
- The implementation of the Modular Credit System (MCS) at Samarkand State Medical University was accompanied by fundamental changes in the organization of the educational process, the assessment system, the role of instructors, and the level of student engagement. To objectively evaluate the impact of the MCS, a comparative analysis of the educational process before (2018–2020) and after (2021–2023) the transition was conducted across several key indicators.Before the implementation of the MCS, the curriculum followed a traditional linear model: subjects were studied throughout the semester with final control in the form of exams and pass/fail tests. The transition to the MCS introduced a modular structure, integrating lectures, practicals, independent work, and knowledge assessment within compact, logically complete units.The MCS established a cumulative point-rating system, where each stage of learning is accompanied by formative assessment. Final grades are based on ongoing participation, interim tests, project work, mini-OSCEs, and final checkpoints. This has improved transparency and manageability of the process.Instructors transitioned from being knowledge transmitters to facilitators and mentors, supporting students throughout each module. Active methods are now widely used, including case-based learning, simulations, problem-based learning elements, digital assignments, and reflective journals.To objectively evaluate the MCS’s impact on academic outcomes, two comparable cohorts of 160 students each (2018/2019 and 2022/2023) were analyzed across multiple performance indicators. There was a statistically significant increase in average GPA (from 3,58 to 3,89; p<0,001), along with a higher proportion of students achieving GPA≥4.0 (from 34,4% to 54,4%). Academic debts decreased from 16,3% to 8,8% (p=0,036), confirming a positive shift in academic success. Attendance—an indicator of student engagement—also improved significantly. Average in-person attendance rose from 77,8% to 84,6% (p<0,001), attributed to both improved scheduling and enhanced motivation through continuous assessment. (tab. 1).
|
|
|
|
4. Discussion
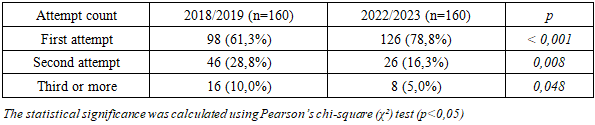
- The findings of this study provide substantial evidence supporting the effectiveness of the Modular Credit System (MCS) in improving academic performance, engagement, and digital integration in medical education. The observed increase in GPA and the proportion of students achieving high academic performance (≥4.0) indicates that the MCS fosters a more consistent and outcome-oriented learning process. These results are consistent with prior research that highlights the benefits of modular, competency-based, and student-centered education models in enhancing academic outcomes and learner autonomy [4,5].The significant reduction in academic debts and repeated module attempts suggests improved learning retention and reduced cognitive overload, likely due to the structured, iterative nature of modular assessments. Continuous formative evaluation may have provided students with more timely feedback, reinforcing active learning strategies [9,11]. Moreover, the substantial rise in digital platform usage—from 48.1% to 85.0%—underscores the system’s compatibility with modern e-learning tools and its role in cultivating self-regulated learning behaviors [7].Equally important is the pedagogical transformation observed within the MCS framework. The shift in instructor roles—from content delivery to mentorship and facilitation—has created space for more interactive, reflective, and case-based approaches, aligning with contemporary global standards for clinical training [2,3]. These transformations are especially relevant for medical education, where clinical competence demands early exposure to real-world problem-solving and interdisciplinary thinking [10].However, the implementation of MCS also necessitates ongoing faculty development, technological infrastructure, and curricular adjustments to maintain quality and avoid superficial modularization. Longitudinal studies are needed to assess the long-term impact of MCS on clinical performance, residency outcomes, and professional identity formation.
5. Conclusions
- The introduction of the Modular Credit System at Samarkand State Medical University led to statistically significant improvements in student academic performance, engagement, and digital learning behavior. The system contributes to the formation of sustainable educational discipline, promotes digital integration, and supports competency-based learning, thereby validating its effectiveness as a modern reform in medical education.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML