-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2026; 16(2): 440-443
doi:10.5923/j.ajmms.20261602.12
Received: Jan. 7, 2026; Accepted: Feb. 1, 2026; Published: Feb. 3, 2026

State of Immune Status in Patients with Chronic Purulent Otitis Media
Narzullayev Nuriddin Umarovich
Bukhara State Medical Institute named after Abu Ali Ibn Sino, Bukhara, Uzbekistan
Correspondence to: Narzullayev Nuriddin Umarovich, Bukhara State Medical Institute named after Abu Ali Ibn Sino, Bukhara, Uzbekistan.
| Email: |  |
Copyright © 2026 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

We studied 25 patients aged from 28 to 45 years with CHSO who were undergoing inpatient treatment in the ENT department of the Bukhara Regional Multidisciplinary Medical Center. Men made up 56.6%, women - 43.4%. Unilateral otitis was observed in 57.8%, bilateral - in 42.2%. In addition to signs of inflammation, general anxiety, poor sleep, refusal to eat, and headaches were noted. In addition to the traditional examination (general blood test, urine test, bacteriological and biochemical studies), all patients underwent an ENT examination, and, if indicated, paracentesis (26.5%) and mastoid radiography (9.6%). In the main group there were 25 patients with CHSO patients, and in the control group there were 14 practically healthy patients of the same age who did not have a history of otitis media. All 25 patients were registered at the Bukhara regional clinic. Patients received antibacterial, anti-inflammatory and local therapy in a hospital setting.
Keywords: Chronic suppurative otitis media, Patients, Immunity
Cite this paper: Narzullayev Nuriddin Umarovich, State of Immune Status in Patients with Chronic Purulent Otitis Media, American Journal of Medicine and Medical Sciences, Vol. 16 No. 2, 2026, pp. 440-443. doi: 10.5923/j.ajmms.20261602.12.
Article Outline
1. Introduction
- The problem of chronic inflammation of the middle ear is one of the urgent problems of clinical otorhinolaryngology. Chronic otitis media accompanied by accumulation of purulent masses in the tympanic cavity are characterized by a long course, contribute to the deterioration of the quality of life and create conditions for the development of otogenic intracranial complications. It is known that the pathogenesis of chronic purulent otitis media is based on changes in various parts of immunity, especially in the state of the local immune system [3]. At the same time, it is proved that long-term inflammatory processes on the mucosa of the tympanic cavity lead to secondary immunodeficiency states and inhibition of local defense mechanisms [4,7], and a vicious circle of disease development is created, which the patient's organism cannot overcome. Along with this, traditional methods of treatment of chronic purulent otitis media, including surgical intervention, antibiotics and hormones, contribute to the aggravation of immunodeficiency state and, among other things, disrupt the natural course of local defense mechanisms [1,9].Cytokines play an important role in the development of an adequate local immune response to the introduction of infection, triggering a cascade of reactions aimed at detection, destruction and removal of the damaging agent. The production of proinflammatory cytokines (TNF, IL-1, IL-8) serves as the first link in the activation of nonspecific resistance and then specific immune response [5,8]. One of the main proinflammatory mediators that control all stages of the inflammatory response is IL-1. In addition, IL-1 has a stimulatory effect on the growth and metabolism of connective tissue and regulates regeneration in the focus of inflammation [2,10].The aim of the study was to investigate the parameters of the immune system in patients with chronic purulent otitis media.
2. Material and Methods of Research
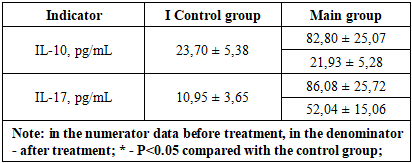
- We studied 25 patients aged from 28 to 45 years with chronic purulent otitis media (CHPOM), who were on inpatient treatment in the ENT department of Bukhara regional multidisciplinary treatment center. Men made 56,6%, women - 43,4%. Unilateral otitis media was observed in 57.8%, bilateral - in 42.2%. In addition to signs of inflammation, general restlessness, poor sleep, refusal to eat, headaches were noted. In addition to traditional examination (general blood, urine, bacteriologic and biochemical tests), all patients underwent ENT examination, paracentesis (26.5%), mastoid process radiography (9.6%).In the main group there were 25 patients with chronic purulent otitis media (CHPOM) patients, and in the control group there were 14 practically healthy patients of similar age who had no history of otitis media. All 25 patients were registered in Bukhara regional polyclinic. The patients received antibacterial, anti-inflammatory and local therapy in hospital. Immunologic researches were carried out together with the Research Institute of Immunology of the Academy of Sciences of the Republic of Uzbekistan. (Tashkent). The study included patients with chronic purulent otitis media (CHPOM), whose patients gave informed consent to participate in this study (the work was performed in accordance with the Declaration of Helsinki and approved by the ethical committee of the Bukhara State Medical Institute).Lymphocyte phenotyping was performed by indirect immunofluorescence method using monoclonal antibodies to CD-receptors produced by "Sorbent Ltd" of the Institute of Immunology of the Ministry of Health and Social Development of the Russian Federation and "Medbioservice". T-lymphocytes (total population - CD3); T-helpers (Tx subpopulation - CD4); T-suppressors (Tc subpopulation - CD8); B-lymphocytes (CD19 subpopulation) were determined. The immunoregulatory index (IRI) - CD4/CD8 ratio was calculated.The concentration of serum immunoglobulins (Ig) A, M and G was determined by radial immunodiffusion.The level of cytokines (IL-10, IL-17) in peripheral blood serum was studied by enzyme-linked immunosorbent assay using Vector-Best test systems. Immune status parameters were studied twice: before treatment and 1 month after treatment.The obtained data were subjected to statistical processing using the computer program Microsoft Excel 2003 on LG-Pentium IV computer. Reliability of differences when comparing mean values was determined by Student's t test. Data are presented as M ± m. Differences were considered reliable at p<0.05.
3. Research Results and Their Discussion
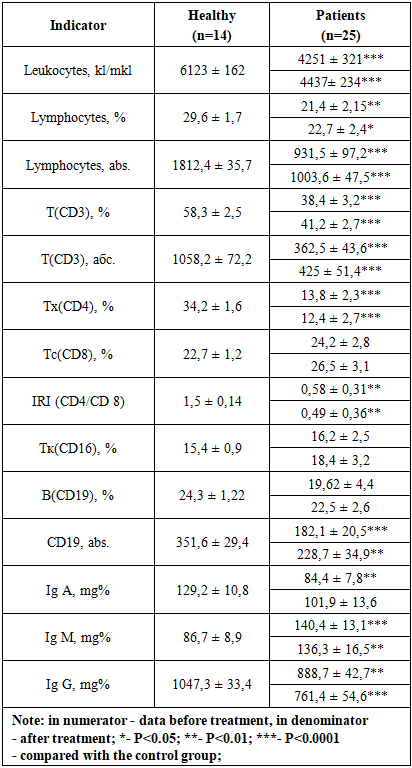
- Retrospective analysis of the study of immune status in patients with CHSSO showed that in the period before the pre-treatment they had significant disorders on the part of their immune system (Table 1).A 0.7-fold decrease in the absolute number of leukocytes and relative content of lymphocytes, a two-fold decrease in the absolute value of lymphocytes were observed in patients with CHPOM. Such decrease was reflected in statistically reliable decrease from 2 to 3 times of absolute values of total pool of T(CD3)- and B(CD19)-lyphocytes (Table 1).In patients with chronic purulent otitis media (CHPOM) patients we revealed deep suppression of T-cell immunity in their relative expression, namely 0.6-fold decrease of T-cells with phenotype (CD3), even more noticeable suppression of helper T-cells - Tx (CD4) - up to 13.8 ± 2.3% (in the control group 34.2 ± 1.6; P<0.0001), while the content of T-cell subpopulation - T(CD8)-cytotoxic lymphocytes exceeded the background values of the control group to a moderate extent (P>0.05). In this regard, in this group there is an inversion of immunoregulatory index (IRI) - CD4/CD 8 ratio - which leads to serious changes in the immune system combined with CGSS. Thus, we found an imbalance of T-cells subpopulations with a decrease of their helper part - Tx (CD4) and increase of suppressor part - Tc (CD8) (Table 1). The decrease of IRI registered by us in patients with chronic purulent otitis media (CHPOM) testifies to functional insufficiency of cells with Tx(CD8) phenotype, and it is a sign of deep immunodeficiency developed in patients. In patients with chronic purulent otitis media (CHPOM) we revealed a small activation of T-killer subpopulation - Tk (CD16), which is probably also pathogenic in this pathology. With regard to the B-cell component of the immune system, we can say that there was a moderate decrease, which was not statistically confirmed (P>0.05). The decrease of B (CD19) lymphocytes was reflected in the spectrum of serum immunoglobulin (SI) content of two classes - IgA and IgG, and the amount of IgM, on the contrary, increased (Table 1).The data obtained by us testify to deep disturbances in the function of the immune system in patients with chronic purulent otitis media (CHPOM), which reflected the spectrum of cellular and humoral immunity factors. These disorders, apparently, can be considered as quite possible fact, playing an important role in the pathogenesis of this mixt-pathology in patients. A decrease in the relative amount of Tx (CD4) is an aggravating factor and an unfavorable prognostic criterion.The conducted treatment did not lead to noticeable changes in the parameters of the immune system in patients with CGSO. We observed a tendency in moderate increase of separate links of cellular immunity and humoral immunity, but restoration of the main parameters of immune status (Table 1). Besides, in patients the tension of humoral component of immunity system was preserved at p>0,05. In patients with chronic purulent otitis media (CHPOM) we found a weak increase in T(CD3) and B(CD19) in their relative and absolute values, as well as a moderate increase in the production of Tc(CD16), Tc(CD8), Ig A concentration (Table 1).
|
|
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML