-
Paper Information
- Next Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2026; 16(1): 200-203
doi:10.5923/j.ajmms.20261601.45
Received: Jan. 3, 2026; Accepted: Jan. 20, 2026; Published: Jan. 22, 2026

Optimal Choice of Autograft for Posterior Cross Light Reconstruction: Clinical Aspects and Innovative Solutions
Irismetov Murodjon Ergashovich1, Shamshimetov Dilshod Fayzakhmatovich2, Safarov Muhammad Maxmudovich3
1Professor, Doctor of Medical Sciences, Director of the Republican Specialized Scientific and Practical Medical Center of Traumatology and Orthopedics of the Ministry of Health of the Republic of Uzbekistan.
2PhD., Head of the Department of Sports Traumatology of the Republican Specialized Scientific and Practical Medical Center of Traumatology and Orthopedics of the Ministry of Health of the Republic of Uzbekistan.
3PhD Student, Department of Sports Traumatology of the Republican Specialized Scientific and Practical Medical Center of Traumatology and Orthopedics of the Ministry of Health of the Republic of Uzbekistan
Correspondence to: Irismetov Murodjon Ergashovich, Professor, Doctor of Medical Sciences, Director of the Republican Specialized Scientific and Practical Medical Center of Traumatology and Orthopedics of the Ministry of Health of the Republic of Uzbekistan..
| Email: |  |
Copyright © 2026 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Posterior cruciate ligament (PCL) injuries are significantly less common than anterior cruciate ligament injuries but are accompanied by pronounced sagittal instability of the knee joint and require surgical treatment. One of the key factors for successful reconstruction is choosing the optimal autograft and its preparation technique.
Keywords: Posterior cruciate ligament, Reconstruction, Autoplasty, Autograft, Semitendinosus tendon, Periosteum, Arthroscopy, Sports traumatology
Cite this paper: Irismetov Murodjon Ergashovich, Shamshimetov Dilshod Fayzakhmatovich, Safarov Muhammad Maxmudovich, Optimal Choice of Autograft for Posterior Cross Light Reconstruction: Clinical Aspects and Innovative Solutions, American Journal of Medicine and Medical Sciences, Vol. 16 No. 1, 2026, pp. 200-203. doi: 10.5923/j.ajmms.20261601.45.
Article Outline
1. Introduction
- Injuries to the posterior cruciate ligament (TCL) are significantly less common than ruptures to the anterior cruciate ligament, however, they represent a serious clinical problem. According to various authors, the proportion of TJ injuries ranges from 3 to 20% of all intra-articular knee joint injuries [1,2]. The main causes are traffic accidents, sports and domestic injuries [3].The clinical significance of TJ damage is determined by the development of sagittal instability, disruption of knee biomechanics, and a high risk of degenerative changes in the cartilage structures [4,5]. Despite the fact that conservative therapy can be used for partial ruptures, in most cases, surgical intervention is required to restore function [6].Choosing the optimal transplant remains one of the key issues in CBC reconstruction. Various autograft variants have been described in the literature: the tendons of the semipendillary and tender muscles, the quadriceps tendon, the proper patellar ligament, and the Achilles tendon [7,8]. Each of these options has certain advantages and disadvantages, making the choice problem relevant.In this regard, the development and implementation of new methods for preparing and using autotransplants aimed at increasing the strength of fixation, reducing complications, and improving functional outcomes [9] is of particular interest. In our work, the experience of applying the patent-protected autograft preparation method is presented, and its comparative assessment with traditional methods is given.The reconstruction of the posterior cruciate ligament (ACL) has undergone significant development. In the early stages, suture restoration and plasty methods using synthetic materials were used, however, such interventions were accompanied by a high risk of inadequacy and complications [10,11]. Subsequently, autoplasty using the patient's own tissues became the main direction. Traditionally, the tendons of the semipendillary and tender muscles, as well as the patella ligament [12], were used.Current trends are related to the search for transplants that provide the optimal combination of biomechanical strength and minimal donor trauma. Increasing attention is being paid to the quadriceps tendon, which demonstrates good results and comparable strength to classical variants [13,14]. Minimally invasive techniques ("all-inside") and the use of biological factors to accelerate transplant integration are also actively discussed [15,16].Thus, the evolution of views on reconstruction of the paranasal sinuses from simple sutures to anatomically oriented autoplasty emphasizes the importance of choosing the optimal transplant, which remains a pressing task of modern sports traumatology.
2. Objective
- To justify the rational use of the original method for preparing an autograft from the tendon of a semispinal muscle with a periosteal area during the reconstruction of the posterior cruciate ligament and to evaluate its clinical effectiveness.
3. Materials and Methods
- The work was carried out on the basis of the Republican Specialized Scientific and Practical Medical Center of Traumatology and Orthopedics (Tashkent, Uzbekistan) in 2023-2025. The study included patients with posterior cruciate ligament (TCL) injury who underwent arthroscopic reconstruction using the original autograft preparation method, protected by the patent of Uzbekistan (UZ FAP 2804, 2025).Surgical technique. The patient was laid on their back, and a tourniquet with a soft lining was applied to the upper third of the thigh. After standard antiseptic treatment of the limb and application of the ports, an arthroscopic revision of the knee joint was performed, the diagnosis of a knee joint rupture was confirmed, and the condition of the associated structures was assessed.Transplant collection. To prepare the transplant, a skin incision approximately 3 cm long was performed along the anterior medial surface of the lower leg, at 3.5-4 cm of the distal line of the knee joint, and at 2 cm of the medial tuberosity of the tibia when the knee joint was flexed at a 90° angle. The tendon of the semispinatus muscle was exposed, its distal end was grasped with a single-toothed hook, after which the tendon was separated from the muscular part using a striper. The free proximal end was brought out.The peculiarity of the proposed method is the resection of the distal end of the tendon of the semipendillary muscle together with a section of the periosteum with a length of 4-5 cm and a width of 1.5 cm, which allows for an increase in the strength and biological potential of the autograft due to the preservation of the bone-tendon component. As a result, a total length of 31-33 cm and a diameter of about 2.7 mm was formed.Preparation of a transplant. The free ends were sewn with a continuous multi-stitch seam about 2.8 cm long. The prepared transplant was folded in three layers from the outside inward, forming a bundle 10-11 cm long and 7.5-8 mm in diameter. To simplify the drainage through the bone channels, an additional multi-stitch suture was applied to one of the smaller sides.Formation of bone tunnels and fixation. Under arthroscopic control, tibial and femoral tunnels with a diameter of 8 mm were formed. The prepared autograft was passed through tunnels and fixed with absorbent interference screws (size 8-25 mm in the femur and 8-30 mm in the tibia). The tightness of the graft and the stability of the knee joint in the 90-100° bend position were monitored.Clinical materials. The method was used in 19 patients with PCI rupture. The study included patients aged 18-45, without pronounced degenerative changes in the knee joint, with isolated or predominantly isolated damage to the knee joint.To assess the effectiveness, the clinical scales of IKDC, Lysholm, and VAS were used before surgery and at 6, 12, and 18 months after intervention. Additionally, an MRI was performed to monitor the integration of the transplant into the bone channels.
4. Results
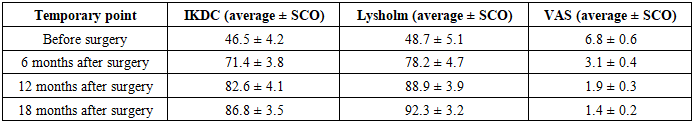
- The study included 19 patients with posterior cruciate ligament rupture, who underwent arthroscopic reconstruction using the proposed method of preparing an autograft from the tendon of the semispinal muscle with a periosteal area (patent UZ FAP 2804, 2025).The observation period ranged from 12 to 18 months. Good and satisfactory results were obtained in 18 (94.7%) patients. In 15 cases (78.9%), a good functional outcome was noted with the restoration of sagittal stability of the knee joint, in 3 patients (15.8%) - a satisfactory result. Only in one case (5.26%), instability arose, associated with the patient's disruption of the orthopedic regimen in the postoperative period.According to MRI data, in 15 patients, almost complete adaptation of the autograft in the femoral and tibial bone canals was observed 1 year after surgery.Functional indicators demonstrated significant improvement on the IKDC, Lysholm, and VAS scales.
|
5. Discussion
- Reconstruction of the posterior cruciate ligament remains one of the most complex tasks in sports traumatology. The main discussions are related to the selection of the optimal transplant and the methodology for its preparation. The most common variants remain the tendons of the semipendillary and tender muscles, the proper patellar ligament (BPTB), and the quadriceps tendon (QT). Each of them has its advantages and disadvantages.Using tendons of the semipendillary and tender muscles provides a sufficient length of the transplant, however, it is associated with the risk of damage to several musculoskeletal structures, which increases donor morbidity and prolongs the rehabilitation period [12]. The use of the patellar ligament (BPTB) is considered the "gold standard" for the anterior cruciate ligament, however, during the reconstruction of the patellar ligament, it is accompanied by high trauma, pain syndrome, and the risk of patellar fracture [13]. The quadriceps transplant (QT) demonstrates good biomechanical indicators, but requires a longer incision and is also accompanied by a disruption of the extensor apparatus [14].The proposed method for preparing an autograft from the tendon of the semispinal muscle, including a section of the periosteum, has several advantages. Firstly, the transplant is taken through a short (3 cm) incision, which reduces the trauma of the intervention. Secondly, using only one tendon reduces the risk of atrophy and functional disorders of the inner thigh muscle group. Thirdly, the inclusion of a periosteal fragment allows for the formation of a transplant with a sufficient length (31-33 cm) and diameter (7.5-8 mm after three-layer folding), which ensures its strength and biological integration into the bone channels.Comparison of the obtained results with literature data shows that the proposed method is not inferior to traditional methods in terms of functional outcomes and stability, while surpassing them in terms of trauma parameters and rehabilitation duration. Thus, good and satisfactory results were noted in 94.7% of patients, which is comparable or even higher than in studies using BPTB or QT-transplants [15,16].It should be especially emphasized that the frequency of complications when using the new method was only 5.26%, and the only case was related to the patient's violation of the orthopedic regimen, and not to the technical features of the operation. This indicates the high reliability of the proposed technology.Thus, the new method of BCC autoplasty allows for reducing the trauma of the intervention, simplifying the surgical technique, and ensuring reliable clinical and functional results.
6. Conclusions
- The conducted research confirmed that reconstruction of the posterior cruciate ligament using an autograft formed according to the original method from the tendon of the semispinal muscle with an area of the periosteum is an effective and minimally invasive method for restoring knee joint stability.The peculiarity of the proposed technology is the possibility of obtaining a transplant of sufficient length and diameter from a single tendon without the need to extract additional tissues. The inclusion of the periosteal fragment increases the strength of the transplant and promotes its biological integration into the bone channels.Clinical application of the method in 19 patients showed high effectiveness: more than 90% of patients achieved good and satisfactory functional outcomes, complications were noted only in isolated cases. The obtained data are comparable or superior to the results described when using traditional grafts, while the new method is characterized by less trauma and shorter rehabilitation periods.Thus, the presented methodology can be recommended for widespread use in the practice of sports traumatology and orthopedics as a promising option for posterior cruciate ligament autoplasty.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML