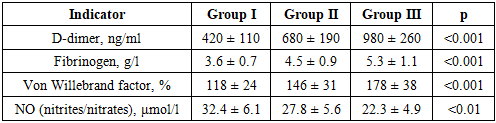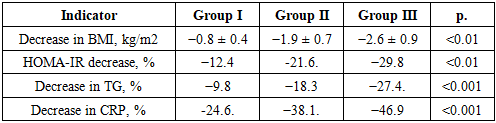-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(12): 4575-4577
doi:10.5923/j.ajmms.20251512.81
Received: Nov. 17, 2025; Accepted: Dec. 12, 2025; Published: Dec. 25, 2025

Influence of the Postovide Syndrome on Metabolic Parameters and the Risk of Cardiometabolic Complications in Obesity Patients
Khairullaeva G. S.
Bukhara State Medical Institute, Bukhara, Uzbekistan
Correspondence to: Khairullaeva G. S., Bukhara State Medical Institute, Bukhara, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The study showed that in patients with COVID-19, the severity of metabolic and inflammatory disorders directly depends on the degree of obesity. An increase in body mass index is accompanied by an increase in insulin resistance, hypertriglyceridemia, and systemic inflammation, which forms an unfavorable clinical and metabolic profile and contributes to the aggravation of the disease. The obtained results confirm the need for early diagnosis and comprehensive metabolic correction in COVID-19 patients with obesity.
Keywords: COVID-19, Obesity, Body mass index, Insulin resistance, HOMA-IR, Dyslipidemia, Triglycerides, Systemic inflammation, CRP, Post-COVID period
Cite this paper: Khairullaeva G. S., Influence of the Postovide Syndrome on Metabolic Parameters and the Risk of Cardiometabolic Complications in Obesity Patients, American Journal of Medicine and Medical Sciences, Vol. 15 No. 12, 2025, pp. 4575-4577. doi: 10.5923/j.ajmms.20251512.81.
1. Introduction
- Post-covid syndrome is considered one of the most significant consequences of a previous SARS-CoV-2 infection, accompanied by prolonged metabolic disorders and increased cardiometabolic risks [1-3]. A special risk group is formed by obese patients, in whom COVID-19 enhances initial metabolic disorders, including insulin resistance, dyslipidemia, and chronic subclinical inflammation [2,4,5]. Modern studies show that even 3-6 months after recovery, such patients maintain elevated levels of pro-inflammatory cytokines, lipid profile and endothelial function disorders, which contributes to accelerated formation of the atherogenic phenotype and increases the likelihood of cardiovascular complications [3,6,7,8]. Considering the widespread prevalence of obesity and the high risk of long-term consequences of COVID-19, studying metabolic changes in the post-COVID period has important clinical significance and allows for the optimization of preventive and therapeutic approaches.The purpose of the study is to assess the impact of post-COVID syndrome on lipid and carbohydrate metabolism, systemic inflammation indicators, and the formation of cardiometabolic risks in obese patients to justify optimal approaches to their early diagnosis and correction.
2. Materials and Methods of Research
- The study was conducted under multicenter observation and included 168 patients who had COVID-19 of varying severity and had signs of lipid metabolism disorders. The selection was carried out on the basis of the infectious diseases hospital and the consultative and diagnostic center. The age of the examined varied from 28 to 72 years (average age 49.6 ± 12.1 years); among them were 92 men (54.8%) and 76 women (45.2%). Inclusion criteria included laboratory-confirmed SARS-CoV-2 (PCR), presence of dyslipidemia or obesity (MI≥ 30 kg/m2), and consent to participate in the study.To analyze the characteristics of lipid metabolism, patients were divided into three groups. Group I (n=54) included patients with normal body weight and moderate dyslipidemia in COVID-19; Group II (n=62) - patients with obesity of I-II degree, who had COVID-19 in moderate form; Group III (n=52) consisted of patients with obesity of the III degree and pronounced lipid profile disorders who had a severe form of the disease. This distribution made it possible to assess the influence of the degree of obesity and the severity of metabolic disorders on the clinical course of COVID-19.
3. Research Results
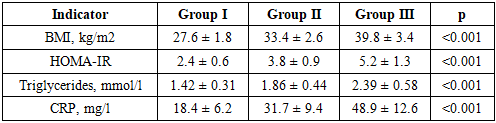
- During the acute phase of COVID-19, patients exhibited pronounced metabolic and inflammatory disorders, the degree of which increased proportionally to the increase in body weight (Table 1).
|
|
|
4. Conclusions
- The obtained data indicate that the initial state of metabolic and inflammatory status in COVID-19 patients is closely related to the degree of obesity. As the body mass index increases, there is a progressive increase in insulin resistance, hypertriglyceridemia, and systemic inflammation, which forms an unfavorable metabolic-inflammatory phenotype of the patient and contributes to a more severe course of the infection. The identified patterns emphasize the importance of early assessment of metabolic indicators and the need for timely correction of identified disorders in patients with obesity in the acute and post-COVID periods.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML