-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(12): 4565-4568
doi:10.5923/j.ajmms.20251512.78
Received: Nov. 28, 2025; Accepted: Dec. 21, 2025; Published: Dec. 25, 2025

Clinical and Immunological Characteristics of Chronic Allergic Conjunctivitis in Children and Evaluation of the Effectiveness of Treatment on Quality of Life
Badritdinova Matluba Najmitdinovna, Tukhtayeva Matlab Ashurovna
Bukhara State Medical Institute, Bukhara, Uzbekistan
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The research presents an assessment of the effectiveness of complex treatment of chronic allergic conjunctivitis in children, taking into account immunological parameters and quality of life. The study included the determination of IgE, IL-6 and IL-10 levels before and after therapy, as well as an analysis of the dynamics of the psychoemotional state according to the adapted scale of the Pediatric Quality of Life Inventory (PedsQL). Prior to treatment, patients showed marked immune shifts in the form of increased IgE, IL-6 and IL-10, accompanied by a decrease in the overall quality of life index to 58.4 ± 3.2 points. After the treatment, a significant decrease in IgE, IL-6 and IL-10 was revealed, which reflected a decrease in the activity of the Th2-dependent inflammatory process, and the PedsQL index increased to 83.7 ± 2.9 points (p < 0.05). The data obtained indicate the high effectiveness of complex therapy aimed not only at immunological stabilization, but also at significantly improving the quality of life of children with chronic allergic conjunctivitis.
Keywords: Chronic allergic conjunctivitis, Immunoglobulins, Interleukins, Treatment, Quality of life
Cite this paper: Badritdinova Matluba Najmitdinovna, Tukhtayeva Matlab Ashurovna, Clinical and Immunological Characteristics of Chronic Allergic Conjunctivitis in Children and Evaluation of the Effectiveness of Treatment on Quality of Life, American Journal of Medicine and Medical Sciences, Vol. 15 No. 12, 2025, pp. 4565-4568. doi: 10.5923/j.ajmms.20251512.78.
1. Introduction
- Allergic conjunctivitis (AK) is one of the most common manifestations of allergic diseases in children and occupies one of the leading places among chronic inflammatory eye diseases. In recent years, there has been a steady trend towards an increase in the frequency of this pathology, which is associated with a deterioration in the environmental situation, an increase in population sensitization, and a change in the immune status of children [2,5,8].According to the literature, up to 40% of children with allergic diseases have clinical manifestations from the eyes, and in the structure of all allergic lesions of the eye surface, the share of AK reaches 60-70%.The immunopathogenesis of allergic conjunctivitis is caused by dysregulation of T-helper reactions (Th2-type) and activation of immunoglobulin E (IgE) production, which leads to дегрануляцииmast cell degranulation, release of inflammatory mediators (histamine, IL-4, IL-5, IL-13) and damage to the conjunctival epithelium. Clinically, this is manifested by itching, hyperemia, edema and lacrimation, which significantly reduce the quality of life of the child [1,3,4,10].Modern therapeutic approaches for AK are aimed not only at relieving symptoms, but also at modulating the immune response, restoring the barrier function of the mucous membrane, and preventing relapses. However, the effectiveness of treatment is often evaluated only by clinical criteria, while the effect of therapy on the patient's quality of life remains insufficiently studied [6,7,11,12].In this regard, it is of interest to conduct a comprehensive clinical and immunological assessment of the condition of children with various forms of allergic conjunctivitis, as well as to analyze the effectiveness of treatment in terms of improving the quality of life [9].Purpose of the study. To evaluate the clinical and immunological features of allergic conjunctivitis in children and determine the effectiveness of the treatment, taking into account its impact on the quality of life of patients.
2. Materials and Methods of Research
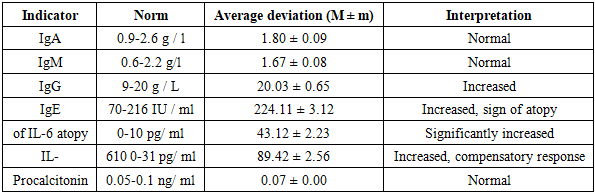
- To solve these tasks, a comprehensive examination of 150 children suffering from various forms of allergic conjunctivitis is being conducted in 2023-2025.* Bukhara branch of the Republican Scientific and Specialized Center of Allergology,* Republican Specialized Scientific and Practical Medical Center of Eye Microsurgery.All patients were divided into four groups:1. The first main group consists of children suffering from chronic forms of allergic conjunctivitis (the duration of the disease is more than 2 years).2. The second main group consists of children with newly diagnosed allergic conjunctivitis.3. Comparison group — children with allergic conjunctivitis combined with other eye diseases (blepharitis, keratoconjunctivitis, etc.).4. The control group consisted of practically healthy children of the same age without signs of allergic diseases (n=30).Modern ophthalmological, laboratory, immunological (determination of the level of IgA, IgG, IgM, IgE, IL-1B, IL-4, IL-6, IL-10, procalcitonin, complement C3, lactoferrin in the blood), instrumental (visiometry, biomicroscopy, ophthalmoscopy) and statistical methods of research were used in the study. The quality of life assessment was carried out using the adapted Pediatric Quality of Life Inventory (PedsQL) scale and analysis of the dynamics of indicators before and after treatment.
3. Results
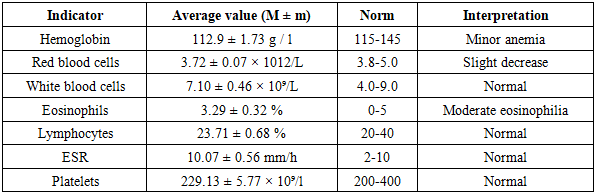
- The average age of the examined children was 10.8 ± 0.45years.Of the 45 patients included in the study, 48.9% were aged 6-10 years, 40.0% were aged 11-14 years, and only 11.1% were older than 15 years.Thus, allergic conjunctivitis was more often diagnosed in school-age children, which is consistent with the data of the world literature indicating the greatest sensitization of the body in this age period.The average duration of the disease from the onset of symptoms to a doctor's appointment was 6.8 ± 0.24 days.All patients (100%) complained of itching and redness of the eyes, while 82.2% noted swelling of the eyelids and conjunctiva.These data reflect a typical picture of allergic inflammation of the ocular surface associated with the activation of inflammatory mediators (histamine, interleukins, prostaglandins).The majority of those surveyed had previously received treatment for allergic diseases.The most frequent cases in the anamnesis were:* allergic dermatitis - in 22 patients (48.9%),* allergic conjunctivitis (recurrent course) - in 11 patients (24.4%),* allergic rhinitis — in 15 patients (33.3%),* bronchial asthma — in 12 patients (26.7%),Quincke's and Lyell's syndromes were less common (4-6%).The data obtained indicate a close relationship between allergic conjunctivitis and other atopic manifestations, confirming the systemic nature of the allergic process.Of those surveyed, 57.8% were treated repeatedly, 11.1% — for 3 years, and 13.3% - for more than 4 years.This reflects the chronic course of the disease and the need to improve therapeutic approaches.
|
|
|
4. Conclusions
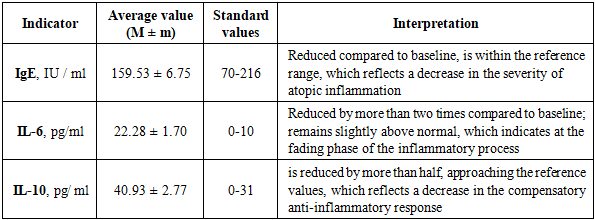
- After treatment, there is a pronounced positive dynamics of immunological parameters, characterized by a decrease in the level of both pro-inflammatoryand anti-inflammatory cytokines with normalization of IgE. These changes confirm the effectiveness of the therapy and reflect the stabilization of the immune status in children with chronic allergic conjunctivitis.The dynamics of the results on the PedsQL scale closely correlated with immunological changes: a decrease in the levels of IgE, IL-6 and IL-10 was accompanied by an increase in subjective well-being and a decrease in the clinical manifestations of the disease. This confirms that therapy not only normalizes the immune status, but also significantly improves the quality of life of patients, reducing psychoemotional stress and improving social adaptation.Thus, complex treatment of chronic allergic conjunctivitis provides not only biochemical and immunological stabilization, but also leads to a significant increase in the quality of life on the PedsQLscale, which is an important integral criterion for the effectiveness of the therapy.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML