-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(11): 4121-4123
doi:10.5923/j.ajmms.20251511.82
Received: Oct. 29, 2025; Accepted: Nov. 17, 2025; Published: Nov. 24, 2025

HSP-70 as a Biomarker of Stress Response in Experimental Pyeloureteral Junction Obstruction
Sottorov Bobur Bohodirovich1, Axmedov Kamoliddin Xakimovich2, Otamurodov Furqat Abdukarimovich3
1Assistant, the Department of Anatomy, Termez Branch of Tashkent State Medical University, Termez, Uzbekistan
2Associate Professor, Head of the Department of “Normal and Pathological Physiology,” Termez Branch of Tashkent State Medical University, Doctor of Medical Sciences, Termez, Uzbekistan
3Associate Professor, DSc, Director of the Termez Branch of Tashkent State Medical University, Termez, Uzbekistan
Correspondence to: Sottorov Bobur Bohodirovich, Assistant, the Department of Anatomy, Termez Branch of Tashkent State Medical University, Termez, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Background: Heat shock protein 70 (HSP70) is a critical mediator of the cellular stress response, promoting protein homeostasis and cell survival under injury. Its dynamic expression in obstructive nephropathy, such as pyeloureteral junction obstruction, is believed to reflect the tissue's adaptive capacity and the severity of damage, though its precise temporal role requires further elucidation. Objective: This study aimed to investigate the dynamic pathogenetic role of HSP70 as a biomarker of the stress response in an experimental model of pyeloureteral junction obstruction. Materials and Methods: An experimental study was conducted on 30 rats divided into three groups: intact control (n=10), sham-operated (n=10), and experimental (n=10) with unilateral ureteral obstruction (UUO) to induce hydronephrosis. Kidney tissue samples were collected on days 1, 7, and 14 post-operation. The expression level of HSP70 was quantified using Western blot analysis, with β-actin used as a loading control. Results: Western blot analysis revealed a significant early upregulation of HSP70 expression in the obstructed kidney on day 1, indicating an acute cellular stress response to the obstruction. By day 7, a marked decrease in HSP70 expression was observed in the pathological group, which persisted at a low level through day 14. This decline coincided with the progression of hydronephrosis. In contrast, the sham-operated group showed only a slight, non-specific increase in HSP70, while the control and contralateral healthy kidney groups exhibited stable, baseline expression levels. Conclusion: HSP70 serves as a dynamic biomarker of the cellular stress response in experimental pyeloureteral junction obstruction. The initial increase signifies an early protective mechanism, while the subsequent decrease reflects the exhaustion of compensatory reserves and the progression of inflammatory and degenerative changes. The specificity of this response to the pathological obstruction, rather than the surgical trauma itself, confirms the pathogenetic significance of HSP70 in obstructive nephropathy.
Keywords: HSP70, Heat shock proteins, Biomarker, Stress response, Pyeloureteral junction obstruction, Hydronephrosis, Unilateral ureteral obstruction, Obstructive nephropathy
Cite this paper: Sottorov Bobur Bohodirovich, Axmedov Kamoliddin Xakimovich, Otamurodov Furqat Abdukarimovich, HSP-70 as a Biomarker of Stress Response in Experimental Pyeloureteral Junction Obstruction, American Journal of Medicine and Medical Sciences, Vol. 15 No. 11, 2025, pp. 4121-4123. doi: 10.5923/j.ajmms.20251511.82.
Article Outline
1. Introduction
- Heat shock proteins, particularly HSP70, are important components of the cellular stress response and play a key role in maintaining protein homeostasis during tissue injury. Elevated levels of HSP70 help stabilize proteins, prevent their aggregation, and enhance cell survival [1,4]. In the setting of urinary tract obstruction, activation of the renal tissue stress response occurs within the first hours after the disturbance of urodynamics [7,9]. Early upregulation of HSP70 expression during hydronephrosis is considered an adaptive mechanism aimed at protecting cellular structures from ischemic and toxic damage. However, with prolonged obstruction, a decrease in HSP70 levels is observed, reflecting the exhaustion of compensatory reserves and the progression of inflammatory and degenerative changes. According to current data, HSP70 also modulates apoptotic and inflammatory signaling pathways, influencing the expression of pro-inflammatory cytokines and apoptotic caspases [8]. Thus, the assessment of HSP70 in obstructive nephropathy has important pathogenetic and prognostic significance, enabling the evaluation of tissue damage severity and the adaptive potential of the organism [8].
2. Purpose of the Research
- To investigate the dynamic pathogenetic role of HSP-70 in experimental pyeloureteral junction obstruction.
3. Materials and Methods
- The study was conducted in accordance with standard methodologies at a center accredited to perform testing under GLP standards [2,3]. A total of 30 rats weighing 180–240 g were included in the experiment and divided into three groups of 10 animals each: Group 1 — intact rats (n = 10); Group 2 — control (sham-operated, n = 10); Group 3 — experimental (n = 10). Before the experiment, all animals underwent at least one week of acclimatization. The control group did not receive any preventive treatment during this period.To induce hydronephrosis, the unilateral ureteral obstruction (UUO) method was used [5,6]. Surgery was performed under aseptic conditions and combined anesthesia. After a midline lumbar incision, the left kidney was exteriorized, the ureter was ligated and transected. Hemostasis was controlled, the kidney was returned to its anatomical position, and the wound was sutured in layers. In the sham-operation group, an identical procedure was performed without ureter ligation to exclude the effect of the surgical intervention itself. Postoperative care included clinical monitoring, free access to water, and standard chow [5]. On days 1, 5, and 14, blood samples (3–4 ml) were collected from the heart under ether anesthesia.In the same time points, kidney tissue samples were collected for Western blot analysis. Kidney tissue samples (20–100 mg) were homogenized in 5–10 volumes of lysis buffer containing protease and phosphatase inhibitors. Homogenates were incubated on ice for 30 min and centrifuged (12,000 rpm, 30 min, 4°C). Supernatants were collected, and protein concentration was determined using the Bradford assay. Proteins were denatured in 1× Laemmli buffer at 100°C for 10 minutes, cooled, centrifuged, and stored at −20°C.Gels were placed into the electrophoresis chamber and filled with 1× Running Buffer. Four microliters of molecular weight marker were loaded into the first well, and 10 µl of each sample into the following wells. Electrophoresis was performed at 60–80 V for 10 minutes (stacking gel), followed by 100 V for 1 hour (resolving gel).Polyvinylidene difluoride (PVDF) membranes were pre-activated in 100% methanol for 1 minute, then washed in cold 1× Transfer Buffer for 10 minutes. Filter papers were prepared similarly. The transfer sandwich was assembled in the following order: sponge – filter paper – gel – membrane – filter paper – sponge. Protein transfer was performed at 15 V for 1 hour and 10 minutes.Immediately after transfer, the membrane was incubated overnight at 4°C on a shaker in blocking buffer (5% BSA in TBST). The membrane was then incubated overnight at 4°C with primary antibodies diluted in the same buffer (5% BSA/TBST). After three 10-minute washes in 1× TBST, the membrane was incubated overnight at 4°C with diluted secondary antibodies, followed by another triple wash.For detection, an ECL reagent mixture (1:1 of reagent A and B) was used. The membrane was incubated with the reagent for 1–5 minutes. The signal was visualized using a chemiluminescent imaging system, and protein band intensities were quantified.
4. Results and Discussion
- To assess the cellular stress response in experimental hydronephrosis in rats, the expression of the heat shock protein HSP70 was evaluated using Western blot analysis. Hydronephrosis was induced by unilateral ureteral ligation, and kidney tissue was analyzed on days 1, 7, and 14 after surgery. The following groups were studied: control (no intervention), sham-operated (Sham), operated animals with an intact contralateral kidney (Op Healthy), and the pathological group (Op Pathol.) — animals with ureteral ligation and hydronephrosis development. β-actin was used for normalization of HSP70 levels; its expression remained stable across all groups, ensuring accurate sample comparison. The results are shown in Fig. 1.
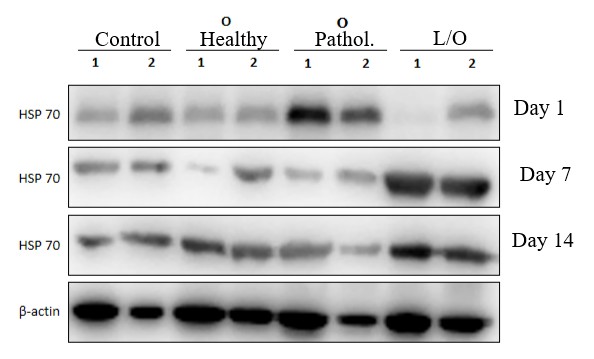 | Figure 1. Analysis of HSP70 heat shock protein expression by Western blot in experimental hydronephrosis in rats |
5. Conclusions
- The results of this study demonstrate that the heat shock protein HSP70 plays a significant pathogenetic role in the dynamics of the cellular response during experimental pyeloureteral junction obstruction in rats. The early increase in HSP70 expression (day 1) after ureteral ligation indicates a rapid activation of the renal tissue stress response to mechanical injury and impaired urodynamics. This reaction represents an early protective mechanism aimed at maintaining cellular protein homeostasis.At later time points (days 7 and 14), a decrease in HSP70 expression was observed in the pathological group, reflecting the exhaustion of cellular compensatory mechanisms under conditions of chronic injury, inflammation, and progressive hydronephrosis. In contrast, no significant changes were detected in the control and sham-operated groups, confirming the specificity of the stress response to the pathological process rather than to the surgical intervention itself.The stability of β-actin levels across all groups confirms the validity of the normalization method, while differences in the intensity of HSP70 bands on the Western blot reliably reflect the dynamics of the cellular stress response.1. HSP70 is an early marker of the cellular stress response in hydronephrosis. Its expression significantly increases as early as the first day after experimental pyeloureteral junction obstruction.2. The subsequent decrease in HSP70 expression reflects the exhaustion of the adaptive capacity of renal tissue, corresponding to the phase of progressive inflammatory and degenerative processes.3. A slight nonspecific increase in HSP70 in the sham-operated group indicates the organism’s response to surgical stress, unrelated to the development of the pathological process. This confirms the pathogenetic significance of HSP70 specifically in the context of impaired urodynamics.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML