-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(11): 3956-3957
doi:10.5923/j.ajmms.20251511.46
Received: Oct. 11, 2025; Accepted: Nov. 6, 2025; Published: Nov. 14, 2025

Integrative Diagnosis of Uterine-Factor Infertility: Possibilities of Hysteroscopy and Immunogenetic Markers
Khikmatova N. I., Khalilova M. U.
Bukhara State Medical Institute named after Abu Ali ibn Sina, Bukhara, Uzbekistan
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The article examines the clinical significance of hysteroscopy and immunogenetic markers in the diagnosis of uterine-factor infertility in women. Hysteroscopy is shown to be a highly effective method for detecting anatomical alterations of the endometrium and uterine cavity. Immunogenetic analysis enables the assessment of the endometrial functional state and its implantation potential. The study results demonstrate that an integrative approach combining hysteroscopy and immunogenetic marker analysis significantly increases diagnostic accuracy (sensitivity 92%, specificity 89%). This approach allows for personalized treatment planning for uterine-factor infertility and contributes to improved fertility outcomes.
Keywords: Uterine-factor infertility, Hysteroscopy, Immunogenetic markers, Integrative diagnosis, Endometrium
Cite this paper: Khikmatova N. I., Khalilova M. U., Integrative Diagnosis of Uterine-Factor Infertility: Possibilities of Hysteroscopy and Immunogenetic Markers, American Journal of Medicine and Medical Sciences, Vol. 15 No. 11, 2025, pp. 3956-3957. doi: 10.5923/j.ajmms.20251511.46.
1. Introduction
- Infertility remains one of the most prevalent issues in women’s reproductive health, with uterine-factor infertility holding special clinical significance. This type of infertility accounts for approximately 10–15% of all infertility cases and represents one of the leading causes of reproductive disorders in women [1,2,3,4,5]. Traditional diagnostic methods are often limited to imaging and laboratory tests, which may not identify subclinical endometrial pathologies.Hysteroscopy enables direct visualization of the uterine cavity and detection of anatomical and morphological changes in the endometrium, such as polyps, synechiae, and developmental anomalies [6,7,8]. Immunogenetic markers, including HLA typing, cytokine profiles, and adhesion molecules, reflect the functional state of the endometrium and its implantation capability. Integration of these methods can enhance diagnostic accuracy and support individualized treatment approaches [9,10,11,12,13,14,15].Objective. To evaluate the diagnostic value of hysteroscopy and immunogenetic markers in identifying uterine-factor infertility in women. The study presents an analysis of modern endoscopic diagnostic methods and key immunogenetic factors affecting fertility. The obtained results show that an integrative approach increases diagnostic precision and optimizes infertility treatment strategies.
2. Materials and Methods
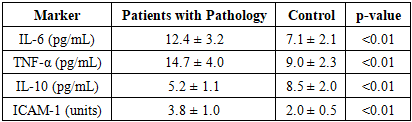
- The study included 120 women of reproductive age (25–40 years) with infertility lasting more than 12 months.Methods of investigation:1. Hysteroscopy with photodocumentation and endometrial biopsy.2. Immunogenetic analysis:o HLA typing;o Determination of cytokine levels (IL-6, TNF-α, IL-10);o Assessment of adhesion molecule expression (LFA-1, ICAM-1).3. Statistical analysis: Data were processed using SPSS 26.0 with a significance threshold of p < 0.05.
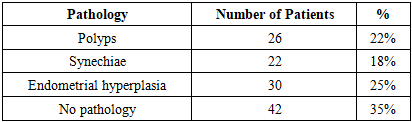
3. Results
|
|
4. Discussion
- The results demonstrate that combining hysteroscopy and immunogenetic marker assessment as an integrative diagnostic approach provides high efficacy in diagnosing uterine-factor infertility. Hysteroscopy allows the identification of anatomical abnormalities such as polyps and synechiae, improving diagnostic precision, while immunogenetic markers help assess the implantation potential of the endometrium and overall reproductive function.Achieved sensitivity (92%) and specificity (89%) confirm that the integrative method surpasses traditional diagnostic techniques. This is crucial for developing individualized treatment strategies, increasing therapy effectiveness, and improving fertility outcomes. The findings are consistent with modern international studies (Sutaria R. et al., 2020; El-Shabrawy Ali A. et al., 2021), confirming the diagnostic and prognostic value of combining hysteroscopy with immunogenetic marker analysis. Such an integrative approach could serve as a foundation for improving standard diagnostic and management algorithms for patients with uterine-factor infertility.
5. Conclusions
- 1. Hysteroscopy is an effective method for detecting anatomical causes of uterine-factor infertility.2. Immunogenetic markers reflect the functional status of the endometrium and can predict implantation success.3. Integrative diagnostics enhance the accuracy of uterine-factor infertility detection and allow optimization of treatment strategies.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML