-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(11): 3832-3834
doi:10.5923/j.ajmms.20251511.16
Received: Oct. 9, 2025; Accepted: Oct. 28, 2025; Published: Nov. 6, 2025

Morphofunctional Features of Testes in 5- and 7-Month-Old White Outbred Rats in Experimental Rheumatoid Arthritis
Temurshokh U. Khabibullayev, Dildora K. Rozikova
Assistant, Bukhara State Medical Institute, Bukhara, Uzbekistan
Correspondence to: Temurshokh U. Khabibullayev, Assistant, Bukhara State Medical Institute, Bukhara, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Rheumatoid arthritis (RA) is a highly prevalent (affecting approximately 1% of the global population) chronic autoimmune systemic disease with an unfavorable prognosis. It is characterized by damage to the synovial membrane of joints, its hyperplasia, and a rapid increase in synovial tissue volume, accompanied by progressive destruction of cartilage and bone tissue. Experimental models, induced in both conventional and genetically modified animals, are widely used to study RA, achieving varying degrees of similarity to the human disease and serving as a valuable tool for investigating potential treatments. Currently, the study of rheumatoid arthritis holds broad medical significance, as it contributes to understanding the fundamental mechanisms of disease development and improving pharmacotherapy for other common human diseases (atherosclerosis, type II diabetes, osteoporosis, etc.), which are pathogenetically linked to chronic inflammation, underscoring the importance of comprehensive research into this condition [1]. This disease has significant social importance due to its widespread prevalence. Rheumatoid arthritis accounts for approximately 10% of all rheumatic diseases, with an annual incidence rate of new cases around 0.02%. According to WHO data, the prevalence of rheumatoid arthritis in the population ranges from 0.6 to 1.3%, reaching 3-5% among close relatives [2,3]. Currently, there is a lack of detailed information and a limited number of scientific studies addressing the state of the male reproductive system, including the testes, in the context of rheumatoid arthritis. This data gap highlights the high relevance and significance of this topic for further research and understanding the impact of rheumatoid arthritis on the body.
Keywords: Rheumatoid arthritis, Synovial membrane of joints, Male reproductive system, Chronic inflammation, Chronic autoimmune systemic disease
Cite this paper: Temurshokh U. Khabibullayev, Dildora K. Rozikova, Morphofunctional Features of Testes in 5- and 7-Month-Old White Outbred Rats in Experimental Rheumatoid Arthritis, American Journal of Medicine and Medical Sciences, Vol. 15 No. 11, 2025, pp. 3832-3834. doi: 10.5923/j.ajmms.20251511.16.
Article Outline
1. Introduction
- The male reproductive system is formed by such organs as the paired gland – the testis, the spermatic ducts, the prostate gland, the seminal vesicles, and the penis. The testes are oval in shape and represent paired organs. Each testis is externally surrounded by several layers (membranes), two of which – the serous and the tunica albuginea – are considered its proper membranes.The serous membrane consists of mesothelial cells and covers the main part of the testis. It merges with the fibrous, that is, the tunica albuginea; the boundary between them is indistinct. The tunica albuginea is rich in elastic fibers and consists of dense connective tissue. In its deeper layers, the tunica albuginea contains many blood vessels; therefore, it is also called the vascular tunic (tunica vasculosa).The tunica albuginea thickens on the medial side of the testis, forming the mediastinum testis, within which are located capillaries and the rete testis. From the mediastinum, connective tissue septa (septula testis) extend radially toward the vascular tunic, dividing the testis into lobules (lobuli testis). The broad bases of the lobules face outward, while their apices open toward the mediastinum of the testis.
2. Purpose of the Research
- The aim is to conduct a study aimed at the comparative examination of the morphometric characteristics of the testes in experimental animals subjected to rheumatoid arthritis modeling. In addition, this study includes a thorough and detailed analysis of the structural changes occurring in the testes as a result of the impact of this disease.
3. Materials and Methods
- For the modeling of rheumatoid arthritis, complete Freund’s adjuvant (0.1 ml subcutaneously at the base of the tail) is used in 120 randomized male white rats aged 5 to 7 months, maintained under stationary conditions in the vivarium of Bukhara State Medical Institute. All animal experiments are carried out in compliance with the international principles of the European Convention for the Protection of Vertebrate Animals used for Experimental and Other Scientific Purposes, as well as in accordance with the “Regulations on the Use of Experimental Animals.”All laboratory animals will be divided into three groups:1. Group 1 – Intact animals (healthy rats).2. Group 2 – Animals with experimentally induced rheumatoid arthritis that did not receive treatment.3. Group 3 – Animals with experimentally induced rheumatoid arthritis that received NSAIDs (meloxicam 1 mg/kg orally, once daily, for 14 days).
4. Results and Discussion
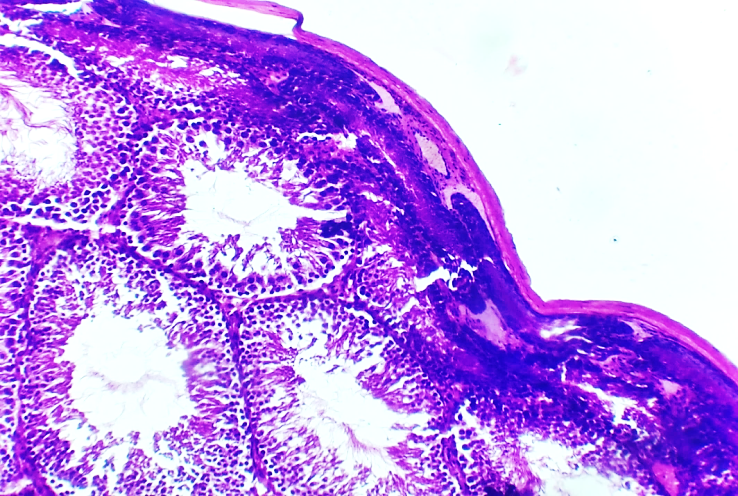
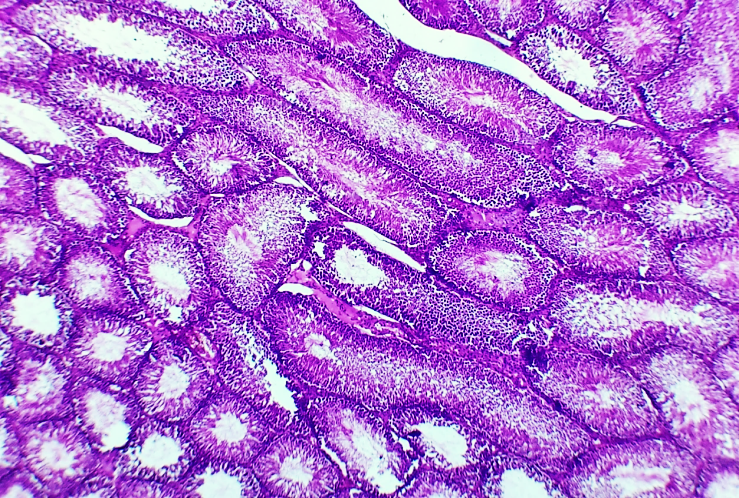
- In the study of testicular tissue changes in 5 and 7 month-old white outbred rats of the experimental group, in which rheumatoid arthritis was induced under experimental conditions, pronounced morphological alterations were revealed. These changes were specific in terms of both macroscopic and microscopic manifestations compared to the control group.In the mechanism of rheumatoid arthritis development, a hypothetical factor is the damage to the covering membranes, which triggers an immune reaction and the appearance of aggregated immunoglobulins that rapidly proliferate. In this process, immunoglobulin M is detected in the blood plasma, while immunoglobulin G is found both in synovial fluid and in blood plasma. This altered immunoglobulin G is considered both an antigen and an antibody. Thus, immunoglobulin G functions as an autoantibody, which, by binding to complement, forms immune complexes.Vascular injury by immune complexes ensues. The process begins with specific damage to the endothelium, leading to the development of acute vasculitis. At the same time, neutrophils and macrophages are activated, and in order to phagocytose the resulting immune complexes, they release lysosomal enzymes—neutral proteases and collagenases. These enzymes actively damage the vascular wall and surrounding connective tissue.As a result, acute vasculitis develops, accompanied by edema and hyperemia in the surrounding tissues. With the prolonged course of this process, vascular stasis and plasmorrhagia appear, ischemia develops in the tissue, and subsequently necrotic changes occur. Due to stasis, small thrombi are formed in the vessels, which leads to a reduction in the functional capacity and viability of tissues and organs.When comparing the results obtained from this group with those of the control group, macroscopic examination revealed relatively reduced testicular size, comparative opacity, thickening, and slight wrinkling of the tunica albuginea covering the testes. In addition, hyperemia and dilation of blood vessels were observed.Microscopically, coarsening and irregular thickening of the tunica albuginea of the testis is observed, caused by the disordered dense arrangement of connective tissue collagen fibers composing it, which surrounds the testis externally. Edema is detected in the interstitial tissue. The edema in the interstitial tissue developed as a result of vascular congestion, particularly in the venous system, and increased vascular permeability, leading to the leakage of the liquid component of blood (plasma) into the interstitial tissue.As a consequence of endothelial damage, adhesion of erythrocytes and other blood elements within the vessel is noted, i.e., agglutination occurs, which represents a false stasis. True stasis is confirmed in many vessels, indicating slowed blood flow due to adhesion. Along the walls of the seminiferous tubules, a small number of thin, sparsely distributed connective tissue collagen fibers were observed, and in some regions of the interstitial tissue, slight edema of the interstitial tissue was present (Figure 1).
4. Conclusions
- When comparing the morphological, morphometric, and organometric characteristics of macroscopic and microscopic specific changes in the testicular tissue of outbred white rats aged 5 and 7 months with experimental rheumatoid arthritis across age groups, similar morphological alterations were observed in the tunica albuginea, intertubular septa, and tubules. It was demonstrated that their morphometric parameters decreased 1.43-fold compared to healthy tissue.Morphometric and histochemical analyses proved that morphological changes in the testicular tissue during experimental rheumatoid arthritis begin in the blood vessels in the form of vasculitis; the process rapidly extends to the vascular-rich tunica albuginea and gradually progresses toward the center through the intertubular septa. A more pronounced reduction and atrophy of the subalbugineal tubules was detected compared to the central regions.The histochemical aspects of testicular tissue in experimental rheumatoid arthritis are characterized by a sharp increase in the number of fibers staining red in the testicular stroma, including the tunica albuginea, vascular walls, and intertubular septa. Atrophy of Sertoli cells and spermatogenic cells in the tubule lumen, resulting from hypoxia, was observed, indicating the development of early infertility.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML