Ismailova Mekhriban Olimbaevna
PhD., Urgench Branch of Tashkent Medical Academy, Urgench, Uzbekistan
Correspondence to: Ismailova Mekhriban Olimbaevna, PhD., Urgench Branch of Tashkent Medical Academy, Urgench, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Abstract
In this study, pathomorphological changes in the cerebrospinal fluid system in traumatic brain injury were studied. Thus, in subarachnoid hemorrhage, all three links of the cerebrospinal fluid bed are involved in the pathological process, and the degree of their damage in each specific case is determined by the localization of hemorrhage, the number of hemorrhages, the volume of subarachnoid and ventricular hemorrhage. This allows for a deeper understanding of the dynamics of cerebrospinal fluid, the features of the development of cerebral edema and other complications. The results of the study will contribute to a better understanding of the pathogenesis of pathologies of the blood-cerebrospinal fluid circulation system in traumatic brain injury. In addition, new treatments and preventive measures can be developed based on the data obtained.
Keywords:
Traumatic brain injury, Choroid plexus, Ventricular system, Cerebrospinal fluid circulation, Ependymal, Pathomorphological changes, Forensic medical examination
Cite this paper: Ismailova Mekhriban Olimbaevna, Examination Methods of the Pathology of the Liquid Circulation System as a Result of Brain Injury, American Journal of Medicine and Medical Sciences, Vol. 15 No. 10, 2025, pp. 3676-3680. doi: 10.5923/j.ajmms.20251510.84.
1. Introduction
Traumatic brain injury (TBI) is one of the pathologies of great importance not only in clinical practice, but also in forensic examination [1,7]. Organic damage to brain tissue, dynamic changes in the brain parenchyma and cerebrospinal fluid system as a result of injury are considered the main link in thanatogenesis.According to researchers Ruziev Sh.I. et al. (2020), Bahriev I.I. et al. (2023), various aspects of this problem have been studied, in particular, the gradual course of thanatogenic processes as a result of TBI, as well as the development of criteria for identifying morphofunctional changes and expert assessment.Various forensic studies have also analyzed thanatogenic processes and causes of death under different traumatic and non-traumatic conditions [4].Currently, the thanatogenic significance of changes in the cerebrospinal fluid system as a result of TBI has not been sufficiently studied in existing scientific research. Burkhanitdinov F. (2017) analyzed the mechanism of injury and clinical pathomorphology in cases of traumatic brain injury, but did not provide sufficient considerations on the dynamics of CSF [2,3].The main objective of the study is to analyze the morphological changes in the pathology of the CSF circulation system as a result of traumatic brain injury.
2. Materials and Methods
The material for this study was 15 cases of acute traumatic brain injury treated and died at the Specialized Neurosurgery Center under the Ministry of Health of the Republic of Uzbekistan during 2019–2024. In each case, medical documents, instrumental examination results, forensic medical examination conclusions, and brain preparations of the victims were analyzed.
3. Result and Discussion
It is known that the combined consideration of the ventricles, blood vessels, meninges (and the spaces between them) as a single functional, three-link CSF [1,5] circulation system allows us to deeply analyze from a new perspective the complex pathogenetic mechanisms of a number of diseases that arise within this system after a traumatic brain injury (leptomeningitis, chorioependymitis, pachymeningitis, hydrocephalus, arachnoid cysts, subarachnoid and ventricular hemorrhages, etc.).Despite the diversity of pathomorphological manifestations of these diseases, they are united not only by localization, but also by the fact that the pathological process to a certain extent covers all three links of the CSF circulation system - of course, to varying degrees and in sequence.The important point here is that in each case, damage to the structures of the cerebrospinal fluid circulatory system is of primary importance relative to damage to brain tissue (excluding the direct effects of the injury). The cause-and-effect relationships are determined in each case by the pathogenetic characteristics of the disease, the location of the pathological process, the degree of its manifestation, and other factors.Evaluating the general pathogenesis of diseases of the CSF circulation system due to BMJ, it should be noted that when one joint of this system is damaged, the rest of the joints are also damaged. However, each disease has its own characteristics, which are manifested in the dominance of a certain link of the system:• In case of leptomeningitis, arachnoid cysts, subarachnoid hemorrhages, the joint of liquid circulation (in the subarachnoid space) is mainly damaged.• In ventricular hemorrhages (as a complication of subarachnoid hemorrhage) - the joint of liquid circulation in the ventricles is damaged.• In hydrocephalus, first of all, the CSF leak joint is damaged (Fig. 1).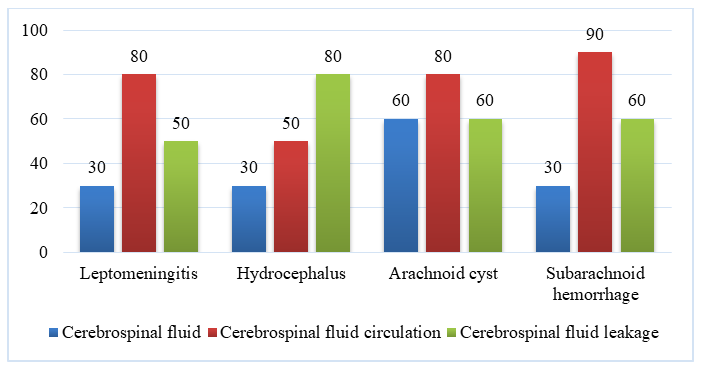 | Figure 1. Scheme of diseases of the cerebrospinal fluid circulation system as a result of CSF, taking into account the predominant involvement of one or another part of the system in the pathological process |
One of the most important aspects is to emphasize the interrelationship of diseases of the cerebrospinal fluid circulation system. For example, the consequences of acute leptomeningitis often turn into subchronic or chronic leptomeningitis, which is accompanied by fibrosis of the leptomeninges. This condition, in turn, can cause the development of occlusive or areosorptive hydrocephalus.Subarachnoid hemorrhage often leads to the development of aseptic leptomeningitis. Purulent (purulent) meningitis can be complicated by pachymeningitis. Each of these diseases, in turn, causes secondary brain lesions.Therefore, a comprehensive study of the structures in all joints of the cerebrospinal fluid circulation system under pathological conditions allows to understand the variety of clinical and morphological changes of this system manifested in diseases after brain injuries and to deeply evaluate the pathogenetic mechanisms.1. Subarachnoid hemorrhage (SAH)Subarachnoid hemorrhage is a condition considered as a special form among acute disorders of cerebral blood circulation, which can occur under various pathologies. In this case, we evaluated the changes in the structure of the morphological substrates of the paracerebral barriers - in particular, in SAQ caused by the rupture of an aneurysm of the cerebral arteries, and in the conditions of experimental infusion of autogenous blood into the cerebrospinal fluid.The analysis of pathomorphological data was carried out in a manner consistent with the fact that it was carried out taking into account pathophysiological indicators such as changes in CSF pressure, impaired CSF microcirculation, and narrowing of the arteries and arterioles.The changes in SAC resulting from aneurysm rupture and experimentally after the introduction of autogenous blood into the CSF have a three-stage periodic course:1. Blood flow into the subarachnoid space (SAS) and its distribution along the system of CSF occlusion channels and subarachnoid spaces;2. Blood coagulation and the formation of blood clots in the CSF;3. Lysis (dissolution) of blood clots (Fig. 2).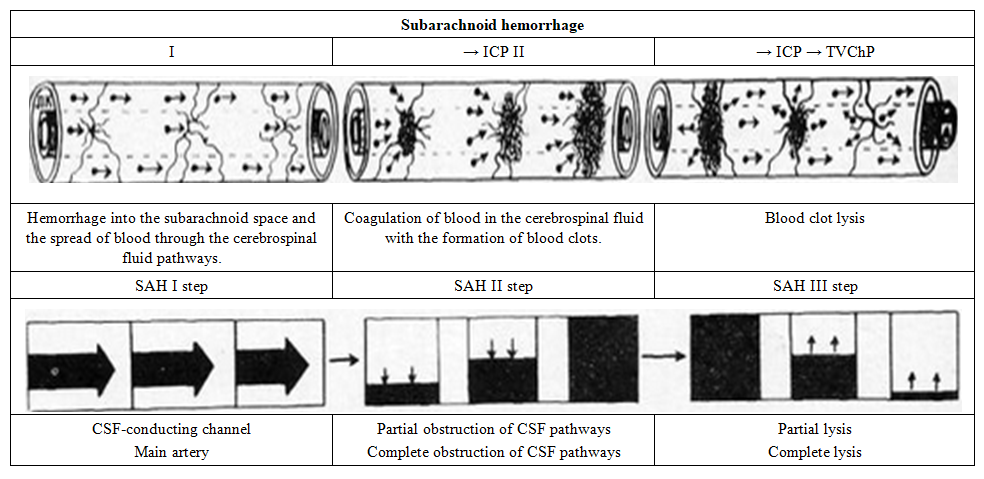 | Figure 2. Scheme of the course of subarachnoid haemorrhage |
Spasm of the cerebral arteries, that is, the condition that develops as a result of blood entering the cerebrospinal fluid, in turn occurs in two stages -1. short-term spasm,2. long-term spasm.If the process ends positively, that is, the function of the arteries is not completely lost as a result of the two previous stages, the previous diameter of the cerebral arteries is gradually restored. This condition should be considered as the third stage of arterial spasm.All the pathologies and pathomorphological changes that will be considered below are individual manifestations of SAC and develop in an interconnected manner (Figure 3).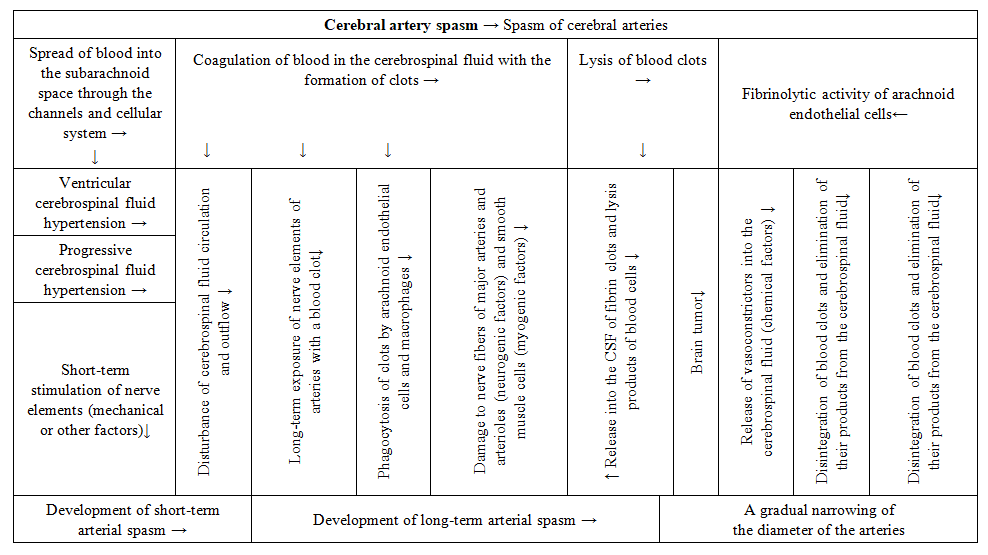 | Figure 3. Scheme of the pathogenetic mechanisms of SCI |
1. Blood flow into the subarachnoid space and its distribution along the CSF-carrying channels and the subarachnoid cell system (SAC stage 1)Autogenous blood entering the subarachnoid space (SAS) spreads along with the CSF flow through the CSF-carrying channels and reaches the excretory channels located at the peak of inflammation. At the same time, blood enters the subarachnoid cell space through the holes in the channel walls.The appearance of a large amount of blood in the SAS leads, first of all, to an increase in the volume of CSF due to blood components, and as a result, to the development of acute CSF hypertension.Clots are formed, and in the period preceding the disruption of the CSF circulation in the CSF channels, an increase in CSF pressure helps to enhance the outflow of CSF through the pulmonary-hematological barrier.During the development of SCD, in the first minutes, hours and days, intensive excretion of erythrocytes and other blood components along with CSF outside the CSF area is observed, which contributes to partial sanitation (sanitation) of the CSF.Erythrocytes pass with the CSF flow into the area of the spinal cord, into the area of the excretory ducts, and through the intercellular spaces and, changing their shape, reach the “subdural space” (SDS). From here, erythrocytes, together with the subdural fluid, enter the dura mater, where they are detected around the blood vessels in the internal capillary network.During the spread of blood along the system of cerebrospinal fluid channels, hemolytic shock in the bloodstream around the arteries located inside the channels and stabilized by columns exerts a strong mechanical effect on the nerve elements and receptors located on the surface of the arterial adventitia and columns, as well as paravasal nerve nodes in the external neural plexus of the cerebral arteries. This leads to the development of short-term arterial spasm.2. Blood clotting in the cerebrospinal fluid and the formation of blood clots (stage 2 of SCI).It turns out that the formation of blood clots in the subarachnoid space leads to partial or complete obstruction of the cerebrospinal fluid channels. This obstruction causes a violation of the microcirculation of the cerebrospinal fluid in the channels - in one or more channels, even in only one hemisphere or in both. Such microcirculation disorders lead to a gradual increase in CSF hypertension.In addition, the outflow of CSF from the SAC through the PBB (pulmonary-hematological barrier) is also impaired, which is associated with impaired CSF microcirculation in the excretory ducts. As a result, the removal of blood components from the subarachnoid space slows down, which, among other factors, contributes to the development of prolonged arterial spasm.The localization of the resulting blood clots is observed mainly between the paravasal structures in the system of CSF-excreting ducts and the paravasal nerve bundles connected to the large arteries of the brain.The density of the clots depends on the ratio of the amount of CSF and subarachnoid blood. A very important point is that during the process of blood clotting, some platelets disintegrate, releasing serotonin, which has a pronounced vasoconstrictor effect. The appearance of even 0.05 ml of serotonin in the cerebrospinal fluid can lead to a sudden spasm of all arterial branches.The hardening of blood clots in the area of paravasal nerve fibers and cords of the large arteries of the brain leads to long-term irritation of “nerve elements (receptors and paravasal nerve fibers)” by the clot. This, in turn, provokes the development of long-lasting arterial spasm.Since the movement of cerebrospinal fluid in the subarachnoid space (SAS) is much slower than in the system of cerebrospinal fluid-carrying channels, during SCA, the formed elements of the blood also stagnate and harden in these areas.Within 2–3 days after SCA, the components of the blood clot are phagocytosed by arachnoid endothelial cells and macrophages lining the subarachnoid space. This process serves to sanitize, that is, purify, the cerebrospinal fluid and, among other factors, normalize the composition of the cerebrospinal fluid.3. Lysis of blood clots (stage 3 of SAQ)Blood clots formed in the subarachnoid space (SAB) are lysed by fibrinolytic activity, which is carried out by the arachnoidendothelial cells lining the SAB. At the next stage, fibrin clots and formed blood elements (erythrocytes, leukocytes, platelets) are released into the cerebrospinal fluid due to fibrinolysis [3,5].Apparently, spasmogenic substances (i.e., products of fibrinolysis) that appear as a result of the breakdown of blood clots in the cerebrospinal fluid cause the development of long-lasting spasm of the arteries.At the submicroscopic level, clearly expressed changes in the ultrastructure of the barrier system between the cerebrospinal fluid and the border tissues, i.e., the ultrastructure of the cerebrospinal fluid-tissue barrier, have been identified in the case of SAQ. As a result of these changes, blood clot fragments penetrate:• into the deep layers of the paravasal nerve fibers,• into the walls of large arteries and arterioles,• and directly into the brain tissue.This leads to:• damage to axons,• smooth muscle cells, and• the development of brain edema.The basis of these changes is the high reactivity of the arachnoid endothelial cells lining the subarachnoid space. When they enter the subarachnoid space, they not only have the ability to phagocytize foreign substances, but also exhibit macrophage properties.
4. Conclusions
This study has demonstrated that traumatic brain injury leads to complex pathomorphological changes in the cerebrospinal fluid (CSF) circulation system, involving all three functional links — ventricles, blood vessels, and meninges. The research highlights that the dynamics of CSF circulation, the processes of blood clot formation and lysis, as well as the development of arterial spasm, are central mechanisms in the pathogenesis of complications such as hydrocephalus, leptomeningitis, and cerebral edema.The findings expand current knowledge on the thanatogenic significance of CSF circulation disorders and emphasize the role of arachnoid endothelial cells and macrophages in the clearance of clots and restoration of CSF flow. The results obtained contribute to a deeper understanding of the mechanisms underlying brain injury complications and may serve as a basis for improving diagnostic criteria, developing therapeutic strategies, and refining forensic medical evaluation of traumatic brain injury cases [1,6,7].
References
| [1] | Bakhriev, I.I., Eshmuratov, B.A., Raimberdiev, S.A., Shamatov, I.Ya., & Yakubov, B.T. (2023). Pathomorphologic features of craniocerebral trauma. Journal of Universal Science Research, 1(3), 136–144. https://universalpublishings.com/index.php/jusr/article/view/3437. |
| [2] | Burkhanitdinov, F., & Iskanderov. (2016). Ekspertnaya otsenka poverjdeniy golovnogo mozga pri smertelnyx ChMT. Novyy den v meditsine, 4(15–16), 258–261. |
| [3] | Burkhanitdinov, F., Abdikarimov, B., & Djuraeva, D. (2017). Pathogenesis of subarachnoid hemorrhage in expert practice. In Proceedings of the scientific-expert conference “Puti sovershenstvovaniya sudebnoy ekspertizy. Zarubezhnyi opyt” (p. 35). |
| [4] | Giyasov, Z.A., Makhsumkhanov, K.A., Bakhriev, I.I., & Islamov, Sh.E. (2022). Retrospective forensic-medical analysis of the dynamics of mortality rates in suicide patients. Sudebnaya medicina, 8(4), 37–46. |
| [5] | Dukarev, V.V. (2020). Immunological disorders in brain trauma and prognostic informatics. [Abstract of PhD thesis]. Moscow. 22 p. |
| [6] | Zikrillaev, T.Kh. (2023). Pathomorphology of ustanovleniya davnosti cherepno-mozgovoi travmy. International Bulletin of Medical Sciences and Clinical Research, 3(9), 83–87. https://doi.org/10.5281/zenodo.8395124. |
| [7] | Ruziev, Sh.I., Bakhriev, I.I., & Nazirov, S.N. (2020). The role of constitutional-morphological type of human in the analysis of pathology and its meaning in forensic medicine. Pediatrics, 1, 167–173. |




 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML