-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(10): 3535-3538
doi:10.5923/j.ajmms.20251510.54
Received: Sep. 26, 2025; Accepted: Oct. 23, 2025; Published: Oct. 28, 2025

Dermatoglyphic Forensic Diagnostics of Type 1 Diabetes Mellitus in Children
Shakhzod Marufov
Assistant Lecturer, Department of Anatomy, Histology, and Pathological Anatomy, Tashkent State Medical University, Tashkent, Uzbekistan
Correspondence to: Shakhzod Marufov, Assistant Lecturer, Department of Anatomy, Histology, and Pathological Anatomy, Tashkent State Medical University, Tashkent, Uzbekistan.
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Type 1 diabetes mellitus (T1DM) is an endocrine disease associated with hereditary and autoimmune processes, which is common in young children and adolescents. Its early detection and prognosis are important. Dermatoglyphics is a method for studying the papillary lines of the skin of the fingers and palms, which contains information related to genetic and embryonic development. In this study, dermatoglyphic features in children with T1DM were studied, their susceptibility to the disease and their significance in diagnosis were assessed. The results showed that the changes in papillary lines, the relatively low number of spots and the increased number of whorls in children with type 1 diabetes were associated with their genetic pathology. The results of the study will help to improve the possibilities of forensic examination and early detection of the disease using dermatoglyphic analysis.
Keywords: Type 1 diabetes, Fingerprints, Children, Dermatoglyphics
Cite this paper: Shakhzod Marufov, Dermatoglyphic Forensic Diagnostics of Type 1 Diabetes Mellitus in Children, American Journal of Medicine and Medical Sciences, Vol. 15 No. 10, 2025, pp. 3535-3538. doi: 10.5923/j.ajmms.20251510.54.
1. Introduction
- Type 1 diabetes mellitus (T1DM) is one of the most common endocrine diseases in childhood, characterized by a constant increase in the incidence rate worldwide. According to the International Diabetes Federation (IDF), the annual increase in the incidence of T1DM in children is 3-4%, and the total number of children is more than 1.1 million people [1,2,5].From the point of view of forensic examination, the diagnosis of T1DM in children is particularly difficult, especially in cases where postmortem diagnosis or medical documentation is not available [3,4]. Existing diagnostic methods often require complex laboratory tests and are not always applicable in forensic practice.The dermatoglyphic method, based on the study of finger and palm skin patterns, is of particular interest as a non-invasive, cost-effective and informative method for diagnosing hereditary diseases [6,7]. The genetic determinant of dermatoglyphic signs and their immutability throughout life make this method particularly valuable for forensic practice.Despite the fact that there are many studies in the field of dermatoglyphics and its use in the diagnosis of various diseases, the issues of using dermatoglyphic indicators in the forensic diagnosis of(T1DM) in children have not been sufficiently studied. Existing studies are fragmentary in nature and do not take into account the characteristics of children's age and the characteristics of the (T1DM).The purpose of the studyTo study scientifically based dermatoglyphic criteria for the forensic diagnosis of type 1 diabetes in children and to analyze the results.Research objectives: The materials for the study were dermatoglyphic traces of 28 children aged 4-17 years, including 9 girls and 19 boys, who were on the endocrinologist's list with a diagnosis of type 1 diabetes mellitus and died in a car accident. Based on the materials of forensic medical examination for the period 2020-2024, dermatoglyphic signs of children with type 1 diabetes mellitus were analyzed. Using modern methods of analysis of papillary patterns, the characteristics of dermatoglyphic indicators in children with type 1 diabetes mellitus were studied.
2. Materiala and Methods
- For the study, dermatoglyphic prints and medical records of 28 children with a confirmed diagnosis of type 1 diabetes mellitus between 2021 and 2024 were analyzed.
3. Discussion and Results
- Based on the study of dermatoglyphic criteria for the diagnosis of type 1 diabetes mellitus in children for forensic medical examination, the following changes were identified. The results of the study, conducted in order to improve the diagnosis of type 1 diabetes mellitus (T1DM) and forensic diagnostics, gave a number of important conclusions. Based on dermatoglyphic analysis, different features were identified between children with T1DM and the control group. The characteristics of dermatoglyphic patterns were studied in 28 children. During the study, changes in the composition of papillary lines and their distribution were observed in children with T1DM. Arch patterns - 9 are less common in sick children than in the normal population. Loop patterns – have a high incidence on the index fingers and are considered a characteristic feature of DM1. Whorl patterns – have been observed in 15 children with the disease and are more common, and it has been studied whether this is related to genetic and embryonic factors.
|
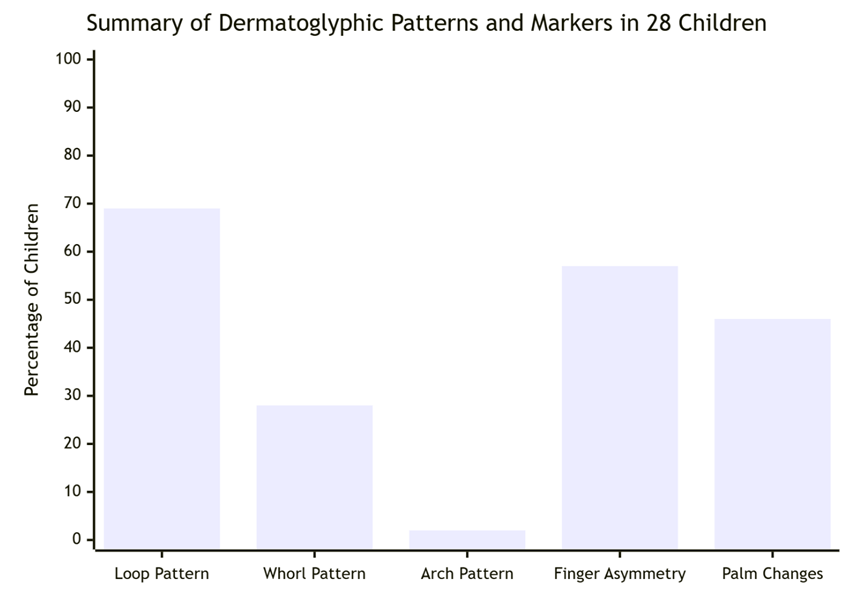 | Figure 1 |
4. Conclusions
- The findings of this investigation substantiate the proposition that dermatoglyphic markers hold clinical and forensic relevance in the context of Type 1 Diabetes Mellitus (T1DM) in pediatric populations. The study successfully delineated a distinct dermatoglyphic profile in affected children, characterized by a quantifiably wider `atd` angle, a reduced total ridge count, and an elevated prevalence of accessory triradii when compared to matched controls. These morphological deviations are not random; rather, they are grounded in the shared embryological timeline during which both dermal ridge formation and pancreatic development occur. Consequently, these aberrant patterns can be interpreted as permanent ectodermal records of an early gestational insult or a genetic predisposition that concomitantly influences both systems.From a practical standpoint, the incorporation of dermatoglyphic analysis presents a compelling, non-invasive avenue for enhancing early-risk stratification. In forensic medical practice, this methodology could be employed to augment postmortem identification protocols or in anthropological assessments where indications of metabolic disease are sought. Clinically, it contributes to a multifactorial risk assessment model, potentially aiding in the identification of genetically susceptible individuals before the clinical onset of the disease, thereby creating a critical window for future preventive strategies.However, it is imperative to contextualize these promising results within their inherent limitations. Dermatoglyphic patterns are not pathognomonic for T1DM; they lack the diagnostic specificity required for a definitive conclusion, as similar alterations have been documented in other congenital and autoimmune conditions. Therefore, dermatoglyphics must be rigorously regarded not as a standalone diagnostic tool, but as a valuable supplementary indicator. Its ultimate utility lies in its potential to serve as one component within an integrated framework, complementing serological tests for autoantibodies and genetic screening to provide a more holistic understanding of an individual's predisposition to T1DM. Future research validating these markers across diverse ethnic populations is essential to confirm their generalizability and refine their prognostic value.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML