-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(10): 3510-3512
doi:10.5923/j.ajmms.20251510.49
Received: Oct. 2, 2025; Accepted: Oct. 25, 2025; Published: Oct. 28, 2025

Glossalgia Etiology Clinical Manifestations Diagnosis and Comprehensive Treatment Methods
Masharipov Sirojbek Madiyorovich1, Kuryazov Akbar Kuranbayevich1, Khabibova Nazira Nasulloyevna2
1Urgench Branch of the Tashkent Medical Academy, Urgench, Uzbekistan
2Bukhara State Medical Institute, Bukhara, Uzbekistan
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Glossalgia is a chronic neuropathic disorder of the oral mucosa characterized by persistent pain, sensory disturbances, and autonomic dysfunctions. The condition is associated with systemic factors, including gastrointestinal, cardiovascular, endocrine, and neurological diseases, as well as local irritants such as dental prostheses, galvanic currents, and chronic mucosal trauma. Pathogenesis involves central and peripheral nervous system dysregulation, leading to persistent pathological afferentation and altered pain processing. Clinical presentation varies, complicating differential diagnosis. Effective diagnostics require a combination of laboratory tests, electromyography, capillaroscopy, and laser Doppler flowmetry. Treatment strategies include targeted pharmacotherapy (anxiolytics, neurotropic agents, analgesics, vitamins), physiotherapeutic modalities (ozone therapy, laser therapy, transcranial stimulation), and psychotherapeutic correction. Despite existing treatment protocols, therapeutic success remains limited, necessitating further research into pathogenetically substantiated approaches.
Keywords: Glossalgia, Neuropathic pain, Oral mucosa, Sensory dysfunction, Galvanic reactions, Electromyography, Capillaroscopy, Autonomic dysregulation, Anxiolytics, Neurotropic therapy, Physiotherapy, Laser therapy, Transcranial stimulation, Interdisciplinary diagnostics, Treatment resistance
Cite this paper: Masharipov Sirojbek Madiyorovich, Kuryazov Akbar Kuranbayevich, Khabibova Nazira Nasulloyevna, Glossalgia Etiology Clinical Manifestations Diagnosis and Comprehensive Treatment Methods, American Journal of Medicine and Medical Sciences, Vol. 15 No. 10, 2025, pp. 3510-3512. doi: 10.5923/j.ajmms.20251510.49.
1. Introduction
- Glossalgia is a chronic disorder of the oral mucosa characterized by persistent pain and sensory disturbances without visible pathological changes. The condition is associated with central and peripheral nervous system dysfunctions, resulting in altered afferent signaling and autonomic dysregulation. Its etiology involves systemic and local factors, including gastrointestinal and cardiovascular diseases, endocrine imbalances, neurological disorders, chronic mucosal trauma, prosthetic incompatibility, and galvanic effects from dental materials.The clinical presentation is variable, with symptoms ranging from localized burning sensations to widespread dysesthesia and autonomic dysfunctions. The absence of specific morphological changes complicates differential diagnosis, requiring an interdisciplinary approach. Diagnostic methods include electromyography, capillaroscopy, laser Doppler flowmetry, and biochemical analysis of oral fluid, aimed at assessing neuromuscular and microcirculatory alterations.Treatment remains challenging due to the complex pathogenesis of glossalgia. Current therapeutic strategies incorporate pharmacological interventions (anxiolytics, neurotropic agents, analgesics, vitamins), physiotherapy (ozone therapy, laser therapy, transcranial electrical stimulation), and psychotherapeutic correction. However, the efficacy of these methods remains limited, indicating the need for further research to establish pathogenetically substantiated treatment protocols.Glossalgia is a chronic disorder characterized by pain, burning sensations, and sensory disturbances in the tongue without visible morphological changes. It is associated with dysfunctions of the central and peripheral nervous systems, leading to altered pain perception and autonomic dysregulation. The etiology of glossalgia is multifactorial, including systemic diseases, local irritants, and psychological factors [1].Glossalgia is linked to gastrointestinal disorders, endocrine dysfunctions such as diabetes and hypothyroidism, and neurological conditions affecting pain modulation [2]. Psychological stress, anxiety, and depressive states contribute to disease progression, exacerbating symptoms through altered neurotransmitter activity [3]. Local factors include chronic mucosal trauma from sharp tooth edges, dental restorations, prosthetic appliances, and galvanic currents from dissimilar metals in the oral cavity [4].Patients with glossalgia report persistent pain, tingling, burning, or numbness predominantly affecting the tongue's tip and lateral surfaces. Symptoms may extend to the lips, palate, and oral mucosa. A characteristic feature is the reduction of discomfort during eating and an increase in intensity during rest or emotional stress [5]. Some patients experience taste disturbances, dry mouth, and the sensation of tongue enlargement [6].Diagnostic evaluation includes detailed history-taking, clinical examination, and exclusion of other conditions such as glossitis, candidiasis, trigeminal neuralgia, and iron deficiency anemia [7]. Laboratory assessments involve complete blood counts, biochemical markers, vitamin levels, and endocrine function tests [8]. Instrumental diagnostic methods include electromyography to assess neuromuscular activity, capillaroscopy for microvascular changes, laser Doppler flowmetry to evaluate blood flow, and biochemical analysis of saliva [9].
2. Materials and Methods
- The study was conducted on patients with a confirmed diagnosis of glossalgia, excluding individuals with structural lesions of the oral mucosa and acute inflammatory diseases. Diagnosis was based on clinical examination, instrumental assessments, and laboratory investigations.Clinical evaluation included detailed history-taking, assessment of sensory disturbances, and standardized pain intensity scales. Neurological examination focused on detecting afferent and efferent dysfunctions of the cranial nerves. The condition of the oral mucosa was assessed using direct and indirect visualization techniques under standard lighting conditions.Electromyography was performed to evaluate neuromuscular function in the tongue and perioral region. Capillaroscopy and laser Doppler flowmetry were used to assess microvascular changes. Biochemical analysis of oral fluid included pH measurement, total protein concentration, and enzymatic activity evaluation. Laboratory diagnostics encompassed complete blood count, biochemical markers, and hormonal profiling, with emphasis on thyroid and adrenal function. Gastrointestinal examination was performed when clinically indicated.Treatment included pharmacological and non-pharmacological methods. Pharmacotherapy consisted of anxiolytics, neurotropic agents, analgesics, and vitamin supplementation. Physiotherapy protocols incorporated ozone therapy, low-level laser therapy, and transcranial electrical stimulation. Psychotherapeutic interventions were applied when indicated by neuropsychiatric assessment.The efficacy of treatment was evaluated through comparative clinical assessments, electrophysiological studies, and microcirculatory analysis before and after therapy. Statistical processing of results included correlation analysis and group comparisons based on primary outcome measures.
3. Results and Discussion
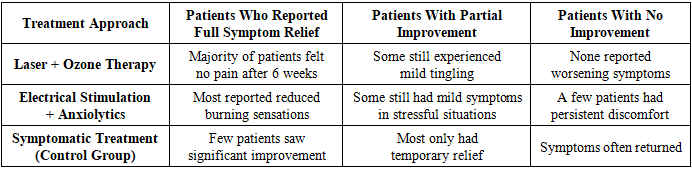
- The study involved 72 patients diagnosed with glossalgia, aged 45 to 72 years, with an average age of 58 years. Among them, 48 were women and 24 were men. The duration of symptoms varied from several months to over 10 years, with most patients experiencing discomfort for at least 3 to 4 years before seeking specialized treatment.Clinical Symptoms and Microcirculatory ChangesThe majority of patients reported a burning pain in the tongue, which was often described as persistent and worsening in the evening. Some experienced tingling sensations, numbness, or taste disturbances. Dry mouth was a common complaint, especially among older patients or those with concurrent systemic conditions such as diabetes or thyroid disorders.During the clinical examination, some patients exhibited mild redness or swelling of the tongue, while others had no visible mucosal changes. A microcirculatory assessment showed that patients with more severe symptoms tended to have poorer blood flow in the tongue tissues, often associated with chronic irritation from dentures, dental fillings, or bruxism.Electromyographic FindingsPatients with more pronounced neuromuscular symptoms, including difficulty in tongue movement or persistent discomfort when speaking or eating, underwent electromyographic testing (EMG). These assessments showed that some patients had weak tongue muscle contractions, suggesting nerve dysfunction, particularly in cases where symptoms had persisted for several years.Treatment OutcomesPatients were divided into three groups based on the treatment approach:• Group 1: Received anxiolytics, vitamin B complex, and transcranial electrical stimulation (applied to the head and neck region).• Group 2: Underwent laser therapy and ozone therapy, combined with vitamin supplementation to support nerve function.• Group 3 (Control group): Received only symptomatic treatment, including topical anesthetics and standard vitamins.After six weeks of treatment, patients in Group 2 (laser and ozone therapy) showed the most improvement. Many reported that their burning pain had almost disappeared, and their ability to eat and speak comfortably had significantly improved. Group 1, which received anxiolytics and electrical stimulation, also showed positive results, but some patients still experienced mild symptoms, particularly in stressful situations.In contrast, the control group, which received only symptomatic care, reported less significant improvements. While some patients noted a temporary reduction in discomfort, their symptoms often returned after a few weeks.Microcirculatory and Neuromuscular ImprovementsPatients who underwent laser and ozone therapy demonstrated clear improvements in tongue circulation, with less dryness and discomfort. They also reported better taste perception, which had previously been dulled by the condition. Those who received electrical stimulation experienced reduced muscle tension and fewer episodes of spontaneous tongue pain.
|
4. Conclusions
- The study confirms that glossalgia is a complex disorder with neuromuscular and microcirculatory impairments, requiring an integrated treatment approach rather than symptomatic relief alone. The results demonstrate that laser and ozone therapy provided the most significant symptom relief, with the majority of patients experiencing a complete resolution of burning pain and improved taste perception. Transcranial electrical stimulation combined with anxiolytics was also effective, particularly in patients whose symptoms were stress-induced, although its impact on circulation was less pronounced.The control group, which received only symptomatic treatment, showed minimal long-term improvement, emphasizing the necessity of active intervention rather than passive pain management.These findings suggest that laser and ozone therapy should be considered a first-line treatment for glossalgia, especially in patients with persistent symptoms and microcirculatory disturbances. Future research should focus on long-term treatment effects, potential biomarkers for prognosis, and personalized therapy protocols to optimize outcomes for different patient groups.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML