-
Paper Information
- Next Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(10): 3506-3509
doi:10.5923/j.ajmms.20251510.48
Received: Oct. 3, 2025; Accepted: Oct. 22, 2025; Published: Oct. 28, 2025

Clinical and Stomatoscopic Changes in the Oral Cavity Organs in Leukemia
Akhmedov S. P.1, Yunuskhodjaeva M. K.2
1Samarkand State Medical University, Samarkand, Uzbekistan
2Tashkent State Medical University, Tashkent, Uzbekistan
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The article examines clinical and stomatoscopic changes in the oral cavity organs among different groups of patients. The main focus is on assessing the condition of the mucous membrane, dental tissues, gums, and tongue using visual and instrumental research methods. The study results revealed a correlation between clinical manifestations of dental diseases and the quality of oral hygiene practices, as well as identified specific features characteristic of particular age and occupational groups. The obtained data substantiate the need for individualized preventive programs aimed at maintaining optimal oral health and reducing the risk of developing dental pathologies.
Keywords: Oral cavity organs, Clinical and stomatoscopic examination, Oral hygiene, Dental plaque, Gingival changes, Prevention of dental diseases
Cite this paper: Akhmedov S. P., Yunuskhodjaeva M. K., Clinical and Stomatoscopic Changes in the Oral Cavity Organs in Leukemia, American Journal of Medicine and Medical Sciences, Vol. 15 No. 10, 2025, pp. 3506-3509. doi: 10.5923/j.ajmms.20251510.48.
1. Introduction
- The organs of the oral cavity play a key role in ensuring the normal functioning of the human body's masticatory, digestive, and speech systems, as well as perform important protective functions. Maintaining their health is directly linked to oral hygiene and the prevention of dental diseases. Despite significant advancements in dental science, the issues of comprehensive assessment of clinical, dental, and hygienic changes in various categories of patients remain relevant and require a systematic approach [1,6].Numerous studies show that dental health largely depends on the condition of the mucous membrane, gums, dentition, and tongue, as well as on the regularity and quality of hygiene practices [2,4,5]. In CIS countries, special attention is paid to identifying age-related and occupational characteristics of changes in the oral cavity organs, which allows for the development of targeted preventive programs [3].Thus, the study of clinical and stomatoscopic changes in oral organs, taking into account age, professional, and social factors, is an important area of modern dental science. This allows not only for the early detection of pathological signs but also for the development of effective programs for the prevention and improvement of oral health in various categories of patients.
2. Materials and Methods of Research
- The study is based on the examination of 151 patients with acute and chronic forms of leukemia, comprising 62 women and 89 men aged 20 to 70 years.The patients were hospitalized at the Research Institute of Hematology and Blood Transfusion of the Ministry of Health of the Republic of Uzbekistan. The diagnosis was made by a hematologist based on a comprehensive clinical and hematological examination of the patient, including mandatory cytological and cytochemical analysis of the bone marrow.During the period from September 2020 to October 2024, 151 individuals were examined. Three clinical groups were formed for observation. The clinical facilities of the Research Institute of Hematology and Blood Transfusion provided the opportunity to conduct laboratory and clinical examinations. To assess the severity, the classification by L.S. Lyubimova et al. was used.Comprehensive examination included: eliciting patients' complaints, collecting medical history, visual inspection of the oral cavity, and index assessment.Patient questioning involved: eliciting the patient's complaints about discomfort, itching, gum pain, bleeding when mechanically irritated (when eating hard food, brushing teeth, or spontaneously), bad breath, presence of lesions in the oral cavity; disease history; family history: presence of general somatic diseases. The examination of the oral cavity was conducted under natural light using examination instruments. The condition of the vermilion border of the lips and corners of the mouth, as well as the oral mucosa, was assessed.
3. Research Results
- Patients' complaints varied depending on the specific therapy administered and the extent of dental care provided. Upon admission to the clinic, patients primarily complained of bleeding gums, dry mouth, and pain while eating. After oral cavity treatment and specific therapy, patients' complaints increased, with tooth mobility appearing alongside increased bleeding. If bleeding was associated with mechanical side effects of dental prostheses, it decreased after correction or removal of the prostheses. Patients with acute leukemia complained of dental hypersensitivity and impaired taste sensation.In both acute and chronic forms of leukemia, patients complained of a foul odor from the mouth and loss of appetite.Upon examination of the oral cavity, changes were observed in almost all patients. Mucosal changes in the form of ulcerative, ulcerative-necrotic, hemorrhagic, atrophic, or hypertrophic lesions typically reflected the severity of the underlying disease. During treatment of the underlying disease with chemotherapy, corticosteroids, and high doses of antibiotics, these changes worsened.Stomatoscopic examination of the mucous membranes of the gums, lips, and cheeks was conducted in both the control and main groups. When examining the mucous membrane of the alveolar ridge in practically healthy individuals, capillary networks are clearly visible against a pink background. Capillaries consist of arterial and venous parts. The venous part is darker in color and significantly wider than the arterial part. The subcapillary part is not visible. Closer to the transitional fold, the mucosal color is darker with a distinct pattern of venous network, where the subcapillary network is clearly visible. In this zone, arterioles, precapillaries, capillaries, postcapillary venules, and main veins are clearly visible.Superficial blood supply is rich in straight arterioles, slightly winding capillaries, and moderately winding venules. Uniform blood flow is observed in both arterioles and venules. In the latter, aggregation of erythrocytes with a fine-grained character is sometimes observed.The stomatoscopic picture of the alveolar ridge mucosa in patients with leukemia differs from the control group by a high degree of variability in both vascular and non-vascular changes.In acute leukemias, the mucous membrane of the alveolar ridge is pale, often without signs of gingivitis. Properly arranged capillaries have almost the same diameter in both the arterial and venous sections. The capillaries are pink in color. The capillary network is clearly visible in both the transitional fold and the mucous membrane of the upper lip. The mucous membrane of the lower lip is darker in color with signs of congestion (stasis).Hyperplasia with bleeding is observed on the surface of the gum mucosa, the background color is pale with a bluish tinge, sometimes purple. Capillaries are short and thickened. The subcapillary network is not visible. As mentioned above, blood stasis in the capillaries, perivascular edema, and numerous microhemorrhages are observed.Often, hypertrophic gingivitis is accompanied by a cloudy appearance of the mucosa in the area of the transitional fold. The capillary network is unclear with pronounced pericapillary edema, the subcapillary network is poorly visible, with a large number of hemorrhages.In some patients, atrophied gingival mucosa with a pale yellow tinge is observed. Capillaries are poorly visible; they are thin, short, and winding.In patients with chronic leukemia, a stomatoscopic examination revealed a clinical picture of the oral cavity similar to that of acute leukemia. However, a characteristic feature of chronic leukemia is hypertrophic gingivitis.The papillae between the teeth are swollen with a dark blue, and sometimes purple, coloration. A grayish-yellow discharge with a foul odor is observed coming from beneath the papillae. The capillaries on the surface of the papillae are convoluted with signs of stasis. Petechial hemorrhages are common.On the surface of the mucous membrane of the transitional folds, the vascular network is clearly visible; however, it is difficult to identify all components of the microcirculatory bed. Perivascular edema is observed.It should be noted that upon admission to the clinic, patients with chronic leukemia often exhibit thrombosis, stasis, and venules with a diameter three times larger than that of arterioles. All this indicated the predominance of vascular changes in the form of venous congestion. After several courses of specific treatment, the perivascular changes intensified. The mucous membrane of the alveolar ridge became pale yellow and cloudy bluish, with poorly visible capillaries and superficial vascular network. Hemorrhagic foci became more prevalent.Minor mechanical injuries facilitated bleeding.Thus, specific treatment of the underlying disease in conjunction with chemotherapy exacerbated the stomatoscopic appearance of the oral mucosa in chronic leukemias. However, upon achieving remission of the underlying disease with restoration of normal cellular composition in peripheral blood, most patients showed improvement in the stomatoscopic picture of the oral cavity. The mucous membrane acquired a pale pink hue, the capillary network became clearly visible, and blood flow became even. Perivascular edema was not visible.Isolated foci of hemorrhage were observed. Analysis of clinical and stomatoscopic studies indicates that changes in the microcirculatory bed occur in both acute and chronic forms of leukemia. Pronounced changes in microcirculation were observed in the terminal stage of the disease.During clinical and hematological remission, an improvement in the stomatoscopic picture of the oral cavity was noted, with restoration of its functional parameters.Candidal lesions of the oral mucosa were observed in 80% of patients. These patients received nystatin concurrently. In both chronic and acute leukemias, oral mycoses caused dry mouth and burning sensation of the tongue and lips. Upon examination, areas of the mucous membrane with white spots were observed (Fig. 2).
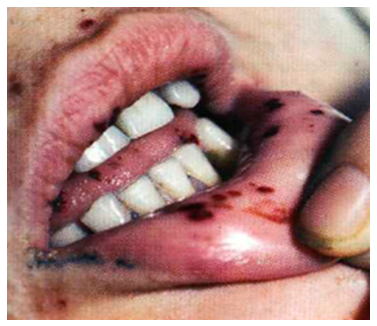 | Figure 1. Patient from group 3. Hemorrhagic and anemic syndrome |
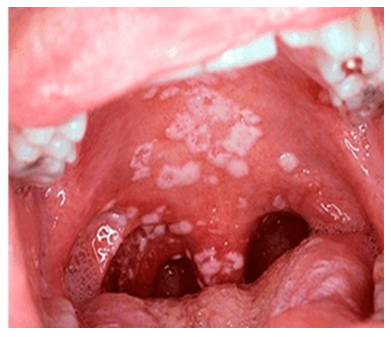 | Figure 2. Patient with chronic leukemia. Candidiasis |
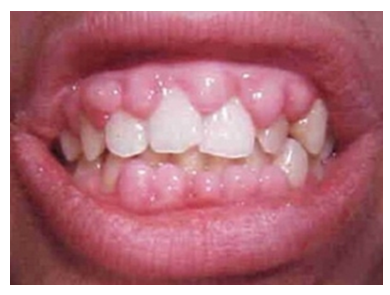 | Figure 3. Patient with acute leukemia |
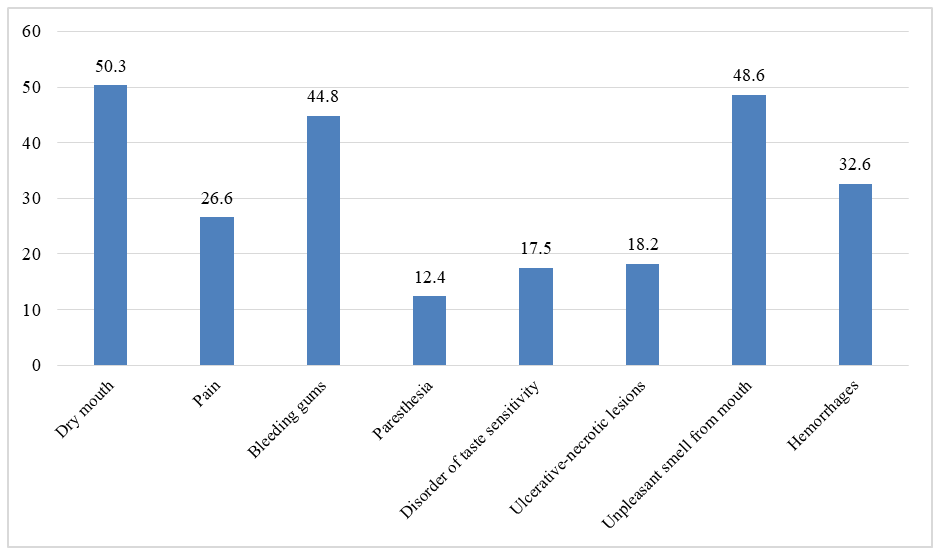 | Figure 4. Frequency of various complaints in patients |
4. Conclusions
- A correlation was revealed between the development of ulcerative-destructive lesions of the oral mucosa against the background of acute leukemia and the ongoing polychemotherapy. In 28 (68%) patients, stomatitis developed on average 3.8 ± 3.7 days after a course of cytostatic therapy, in 13 (32%) patients - during the treatment. The ulcerative-destructive lesions of the oral mucosa persisted for 8-30 days and averaged 18.96 ± 3.48 days.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML