-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(8): 2803-2808
doi:10.5923/j.ajmms.20251508.81
Received: Aug. 7, 2025; Accepted: Aug. 25, 2025; Published: Aug. 30, 2025

Analysis of the Effectiveness of the Use of Standard Medical Protocols and Folk Medicine Methods in the Treatment of Chronic Allergic Dermatitis
Karimova F. R.
PhD., Associate Professor, Department of Folk Medicine, Occupational Diseases and Allergology, Bukhara State Medical Institute, Bukhara, Uzbekistan
Correspondence to: Karimova F. R., PhD., Associate Professor, Department of Folk Medicine, Occupational Diseases and Allergology, Bukhara State Medical Institute, Bukhara, Uzbekistan.
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The article presents the results of a clinical and epidemiological study of 298 patients with chronic allergic dermatoses treated according to standard medical protocols and folk medicine methods. The study population included 138 (46.3%) men and 160 (53.7%) women, with an average age of 27.7±1.27 and 30.6±1.13 years, respectively. Patients were analyzed by age categories, sex, and nosological forms, including allergic contact dermatitis, atopic dermatitis, eczema, and other variants. It was revealed that allergic contact dermatitis predominated among women (p<0.05), while atopic dermatitis was more common in men, especially in childhood (p<0.05). Standard treatment protocols were applied in 56.7% of cases, predominantly among women, while 43.3% of patients, mainly men, used traditional folk remedies. A comparative analysis of morphological elements (nodules, blisters, excoriations, fissures, lichenification, scaling, etc.) showed significant age- and sex-specific differences, indicating the polymorphism of clinical manifestations. The obtained results confirm that the course and severity of chronic allergic dermatoses are influenced by gender and age factors, as well as by adherence to treatment protocols. These findings can serve as a basis for optimizing diagnostic and therapeutic strategies and for developing individualized approaches to the treatment of chronic allergic skin diseases.
Keywords: Chronic allergic dermatoses, Allergic contact dermatitis, Atopic dermatitis, Eczema, Folk medicine, Standard medical protocols, Morphological elements, Treatment effectiveness
Cite this paper: Karimova F. R., Analysis of the Effectiveness of the Use of Standard Medical Protocols and Folk Medicine Methods in the Treatment of Chronic Allergic Dermatitis, American Journal of Medicine and Medical Sciences, Vol. 15 No. 8, 2025, pp. 2803-2808. doi: 10.5923/j.ajmms.20251508.81.
1. Introduction
- Chronic allergic dermatoses (CAD) are among the most common dermatological diseases worldwide, significantly reducing the quality of life and leading to prolonged treatment and frequent relapses (Silverberg, 2017; Wang et al., 2020). According to the World Health Organization (WHO, 2021), allergic skin diseases affect up to 20–25% of the global population, with a marked increase in incidence over the past two decades. The most prevalent forms include allergic contact dermatitis (ACD), atopic dermatitis (AD), and eczema, which together account for more than 70% of all chronic allergic dermatoses [1,7].Epidemiological studies indicate that CAD are more common in women of reproductive age, which is associated with hormonal influences, increased exposure to household chemicals, and cosmetic use (Kim et al., 2019). At the same time, atopic dermatitis is more frequent in childhood and adolescence, with higher prevalence among boys [4]. Such gender- and age-related differences require careful analysis to determine risk factors and optimize treatment strategies.Despite the existence of standardized therapeutic protocols, including glucocorticoids, antihistamines, and topical remedies [2], many patients continue to use traditional folk medicine, either independently or in combination with modern approaches. According to several reports, up to 40–45% of patients resort to folk remedies, which may affect the clinical course, delay remission, and increase the risk of complications [6].Clinical manifestations of CAD are diverse and include nodules, blisters, excoriations, fissures, lichenification, and scaling, whose prevalence varies significantly by age and sex. Morphological heterogeneity reflects the chronicity and severity of the disease, and is closely linked to pruritus intensity, immune hyperreactivity, and recurrent inflammation [4,5].In this context, a comprehensive assessment of demographic, nosological, and therapeutic features of chronic allergic dermatoses is of paramount importance. Such data will provide the basis for developing individualized treatment approaches, improving patient adherence, and enhancing the overall effectiveness of therapy.Purpose of the study. The aim of this study was to investigate the age, gender, and nosological characteristics of chronic allergic dermatoses (CAD), as well as to evaluate the effectiveness of standard medical protocols compared with traditional folk medicine methods. Special attention was given to the distribution of patients by clinical forms, age-specific manifestations, and morphological elements of the skin in order to identify patterns that may influence the severity, recurrence, and prognosis of the disease.
2. Materials and Methods
- A comprehensive clinical and epidemiological study was conducted among 298 patients with chronic allergic dermatoses. All participants were selected based on predefined inclusion and exclusion criteria to ensure the accuracy of the results and eliminate the effect of unrelated pathologies.Patients were divided into two main treatment groups:Group I (n=169): Patients treated according to standard medical protocols, including glucocorticoids, antihistamines, and topical agents.Group II (n=129): Patients who predominantly used folk medicine methods, either independently or in combination with modern therapy.The distribution of patients was analyzed by age, gender, and nosological forms, including allergic contact dermatitis, atopic dermatitis, eczema, and other variants. In addition, morphological elements of the skin (nodules, blisters, excoriations, fissures, lichenification, scaling, etc.) were evaluated across different age and sex categories. Statistical analysis included comparisons of prevalence rates, gender differences, and age-related trends, with the aim of identifying clinical and epidemiological features that may guide the development of individualized therapeutic strategies.
3. Results and Discussion
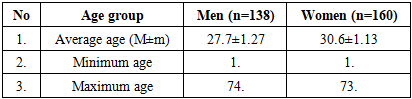
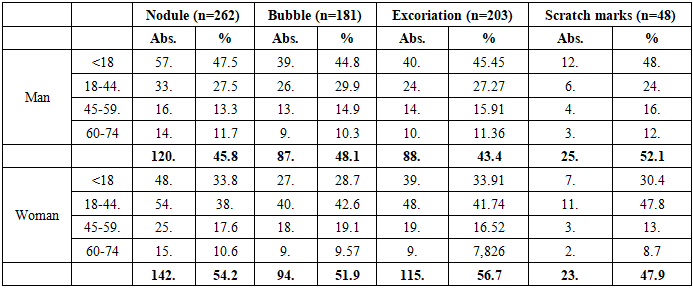
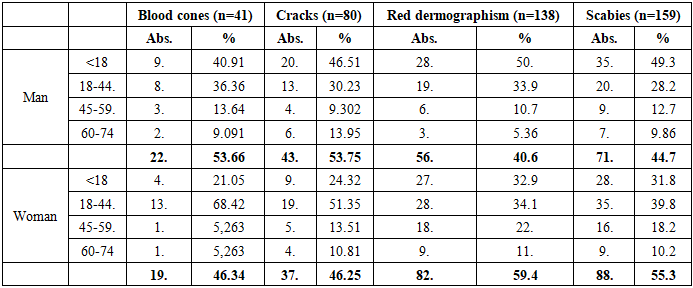
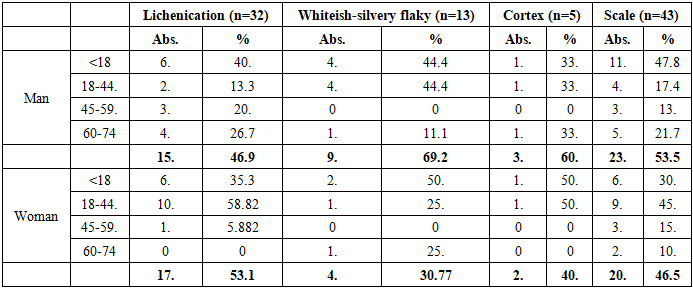
- The study showed that the course and clinical manifestations of chronic allergic dermatoses (CAD) were significantly influenced by age, gender, and the chosen method of treatment. In patients who used standard medical protocols, remission was achieved faster and the severity of symptoms was lower, whereas in patients relying on folk medicine, the disease often had a prolonged and recurrent course.Age analysis revealed that CAD occurred in all categories, from early childhood to older age, but their distribution varied: atopic dermatitis was more common in children and adolescents, while allergic contact dermatitis predominated in adults, especially women of reproductive age. Eczema and other rare forms were mostly observed in middle-aged and elderly patients.The evaluation of morphological elements confirmed these differences. Nodules were most frequent in children, blisters predominated in women of reproductive age, and excoriations were significantly more common in women across almost all groups. Chronic features such as lichenification and scaling were mainly observed in adults, indicating a prolonged and relapsing course of the disease.Analysis of treatment groups demonstrated that patients managed with standard protocols had better outcomes: a lower frequency of excoriations, reduced itching intensity, and fewer chronic morphological changes. By contrast, in patients who predominantly used folk medicine, relapses were more frequent, and elements such as fissures, red dermographism, and scabies were recorded at higher rates.Thus, the results confirm that gender and age factors, combined with the choice of treatment method, significantly influence the clinical course of chronic allergic dermatoses. Standardized therapy ensures more stable remission, while reliance on folk medicine is associated with prolonged disease activity and higher recurrence. These findings highlight the need for patient education and the development of individualized therapeutic strategies.A total of 298 patients were involved in the study. Of these, 138 (46.3%) were men and 160 (53.7%) were women. In chronic allergic dermatoses, a predominance of women was noted. This indicator corresponds to the data recorded in the literature, which indicates a higher frequency of chronic skin allergic diseases in women (p<0.05) (Table 1).
|
|
|
|
|
|
|
4. Conclusions
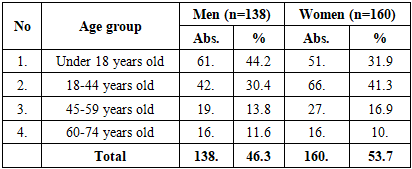
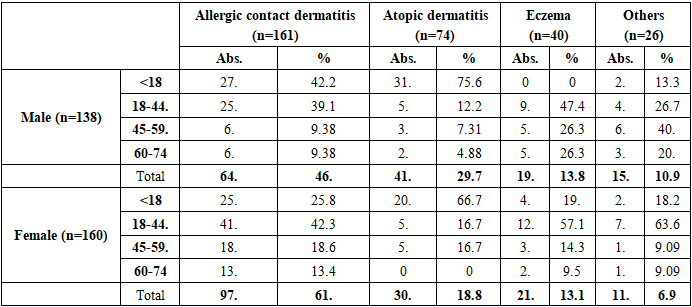
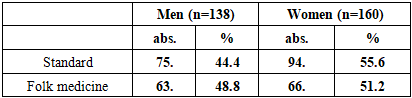
- In the analysis of gender distribution, women predominated among patients with allergic contact dermatitis (61.0%), while atopic dermatitis was more common in men (29.7% versus 18.8% in women). Although gender differences were evident in specific nosological forms, statistical significance was confirmed mainly for allergic contact dermatitis (p<0.05), while in eczema and other rare variants the differences were not significant (p>0.05).When assessing the age structure, patients under 18 years accounted for a significant proportion of cases with atopic dermatitis (75.6% in boys and 66.7% in girls), whereas in the age group of 18–44 years allergic contact dermatitis predominated, particularly among women (42.3%). In the elderly (60–74 years), the distribution of forms was more balanced, without reliable differences between men and women (p>0.05).The analysis of treatment methods revealed that standard protocols were used more frequently by women (55.6%), while folk medicine was more commonly practiced by men (48.8%). Although these differences in distribution did not reach statistical significance for folk methods (p>0.05), the predominance of women in standardized therapy was significant (p<0.05).Morphological manifestations showed clearer differences: nodules predominated in children and adolescents (47.5% in boys and 33.8% in girls, p<0.01), blisters were more common in women of reproductive age (42.6% versus 29.9% in men, p<0.05), and excoriations were significantly more frequent in women across all age groups (p<0.05). Chronic elements such as lichenification were more typical in women aged 18–44, whereas silvery-white flakes were significantly more common in men, especially in childhood and youth (p<0.05).Thus, the study demonstrated that chronic allergic dermatoses exhibit pronounced gender- and age-related features in both clinical forms and morphological manifestations. The use of standard protocols was associated with more favorable outcomes, while reliance on folk medicine correlated with a more prolonged and recurrent course. These findings underline the importance of individualized treatment strategies, patient education, and adherence to evidence-based protocols in the management of chronic allergic dermatoses.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML