-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(8): 2788-2794
doi:10.5923/j.ajmms.20251508.78
Received: Aug. 11, 2025; Accepted: Aug. 29, 2025; Published: Aug. 30, 2025

Use of Artificial Intelligence Technologies and Digital Radiologic Processing for the Diagnosis of Paranasal Sinus Diseases by Multislice Computed Tomography
Amonov Shavkat Ergashovich1, Ikramov Aziz Adhamovich2
1MD, Professor, Head of the Department of Otorhinolaryngology, Pediatric Otorhinolaryngology and Dentistry, Tashkent Pediatric Medical Institute, Uzbekistan
2Doctoral Student, Department of Otorhinolaryngology, Pediatric Otorhinolaryngology and Dentistry, Tashkent Pediatric Medical Institute, Uzbekistan
Correspondence to: Amonov Shavkat Ergashovich, MD, Professor, Head of the Department of Otorhinolaryngology, Pediatric Otorhinolaryngology and Dentistry, Tashkent Pediatric Medical Institute, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The aim of the study was to substantiate and evaluate the feasibility of using machine learning algorithms and digital radiologic processing to improve the accuracy of diagnosing paranasal sinus pathologies and to determine the prospects for their integration into the healthcare system. Materials and Methods: A review was conducted of current solutions in automated medical image analysis, including CT and MRI of the paranasal sinuses, utilizing artificial intelligence (AI) and radiologic processing. Results: The implementation of AI in the diagnostic process enhances the accuracy of image interpretation, reduces analysis time, automates pathology detection, and standardizes reporting. Conclusion: The integration of AI and radiologic processing into the diagnosis of paranasal sinus diseases improves diagnostic accuracy and physician efficiency, creating a foundation for a personalized approach to patient care.
Keywords: Artificial intelligence, Digital radiologic processing, Computed tomography, Paranasal sinuses, Frontal sinusitis, Maxillary sinusitis, Sphenoid sinusitis, Ethmoid sinusitis, Image segmentation, Automated diagnosis, Medical imaging
Cite this paper: Amonov Shavkat Ergashovich, Ikramov Aziz Adhamovich, Use of Artificial Intelligence Technologies and Digital Radiologic Processing for the Diagnosis of Paranasal Sinus Diseases by Multislice Computed Tomography, American Journal of Medicine and Medical Sciences, Vol. 15 No. 8, 2025, pp. 2788-2794. doi: 10.5923/j.ajmms.20251508.78.
1. Introduction
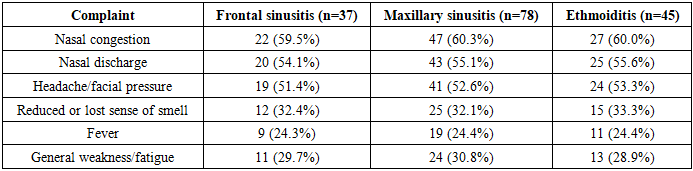
- Pathology of the paranasal sinuses (maxillary sinusitis, frontal sinusitis, ethmoiditis, sphenoiditis, polypoid changes, and neoplastic processes) occupies a significant place in the overall structure of ENT diseases. In recent years, the clinical presentation of these conditions has changed, which is reflected in an increased incidence of atypical and latent forms. A considerable proportion of patients with rhinosinusitis do not exhibit pain syndrome, and the disappearance of localized pain after the initiation of therapy is not always a sign of complete recovery. Whereas until the late 20th century clinicians widely believed that localized headache in acute inflammatory processes of the paranasal sinuses and in exacerbations of chronic forms was a key diagnostic sign (Piskunov S.Z., 1991), in recent years this approach has been reconsidered, and its diagnostic value has been seriously questioned (Stagnieva I.V., 2008).Despite advances and the expansion of diagnostic and therapeutic technologies, the prevalence of inflammatory diseases of the paranasal sinuses remains high and shows no tendency toward decline (Piskunov S.G., 2013). According to several studies, over the past two decades, the incidence of chronic rhinosinusitis has increased more than threefold (Kozlov V.S., 2003; Kleshchin D.A., 2005). At the same time, the clinical manifestation of sinusitis has become less typical: there is an increasing frequency of absent or mild localized pain, which complicates early diagnosis. Epidemiological studies indicate that chronic sinusitis occurs in 12–15% of the adult population, and accurate assessment of the prevalence and nature of the process requires the use of highly informative imaging modalities, such as computed tomography (CT) and magnetic resonance imaging (MRI) [1].Traditional image interpretation largely depends on the physician’s experience and the quality of the source material, which creates prerequisites for subjective errors. The integration of artificial intelligence technologies and digital radiologic processing offers new opportunities for objectifying analysis, automating pathology detection, and standardizing reports, thereby improving the accuracy and reproducibility of diagnostic conclusions [2].Given the above, there is growing interest in the implementation of objective technologies in diagnostics. This is particularly important in the field of paranasal sinus imaging, where deep learning algorithms have already demonstrated practical value: In a study focused on paranasal sinus segmentation, a multiclass 3D U-Net network achieved an F1 score of 84.3% for healthy sinuses and 79.3% for pathological ones, highlighting the clinical potential of automation in navigation and preoperative planning [3]. In a separate study, a deep neural network–based algorithm demonstrated an accuracy of 85.8% in classifying sinusitis on CT scans, significantly outperforming physicians, whose results ranged from 71.7% to 78.4% depending on their qualifications [4]. When analyzing cone-beam computed tomography (CBCT) images with AI-based denoising modules, the system showed improved diagnostic performance: an increase in accuracy by 9.6%, macro-AUC by 5.6%, and micro-AUC by 7.4%, which enabled an 11% improvement in physicians’ reading accuracy for such data [5]. A recent study on maxillary sinus pathology detection using a CNN on CBCT achieved impressive metrics: Dice coefficient of 0.923, recall of 0.979, IoU of 0.887, F1 score of 0.970, and precision of 0.963 [6]. A 2025 review that included a systematic analysis of scientific publications found that deep learning algorithms were most frequently used for detecting paranasal sinus diseases (73.6% of studies), with the primary tasks being classification and detection of pathologies [7].These examples demonstrate that artificial intelligence algorithms can significantly improve:• diagnostic accuracy,• objectivity and reproducibility of image interpretation,• efficiency and standardization of the examination process.The integration of AI and digital radiologic processing into routine practice has the potential to dramatically enhance the detection and management of paranasal sinus pathology, particularly in the context of increasing prevalence of latent and atypical forms of disease [8,9].The aim of the study: To substantiate and evaluate the feasibility of employing machine-learning algorithms and digital radiologic processing to improve the accuracy of diagnosing paranasal sinus diseases and to determine the prospects for their integration into the healthcare system.
2. Materials and Methods
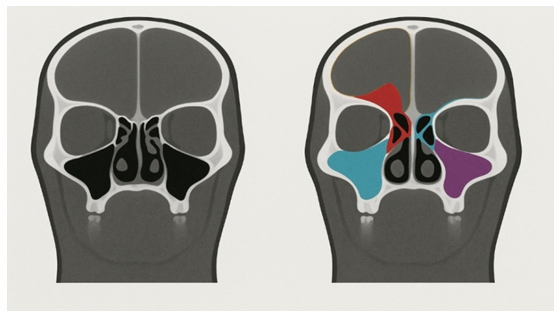
- This study employed a retrospective design focusing on patients with paranasal sinus pathology and healthy individuals who underwent examinations at the Tashkent Pediatric Medical Institute from January 2025 to May 2025. The study included 200 participants, of whom 160 patients had confirmed paranasal sinus pathology, while 40 subjects comprised the control group of healthy volunteers with no signs of paranasal sinus disease according to clinical and imaging assessments.Patients with paranasal sinus pathology were subdivided according to the localization of the pathological process (Fig. 1) and the number of acquired images: frontal sinusitis — 37 patients (23.1%); maxillary sinusitis — 78 patients (48.8%); ethmoiditis — 45 patients (28.1%).
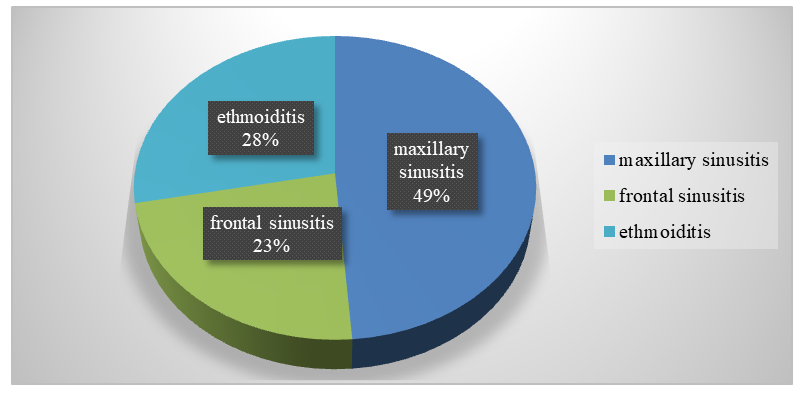 | Figure 1. Clinical distribution of patients in the main study group |
|
3. Results
- Analysis of CT images in the main patient group revealed characteristic radiologic features for each disease subgroup.In patients with frontal sinusitis (n = 37), tomograms demonstrated diffuse or partial reduction in the pneumatization of the frontal sinuses with homogeneous or loculated opacification corresponding to the accumulation of mucopurulent content (Fig. 2). In some patients, mucosal thickening up to 6–8 mm was observed, involving the frontonasal duct. In certain cases, expansion and deformation of the anterior sinus wall, as well as signs of a subperiosteal abscess, were visualized.
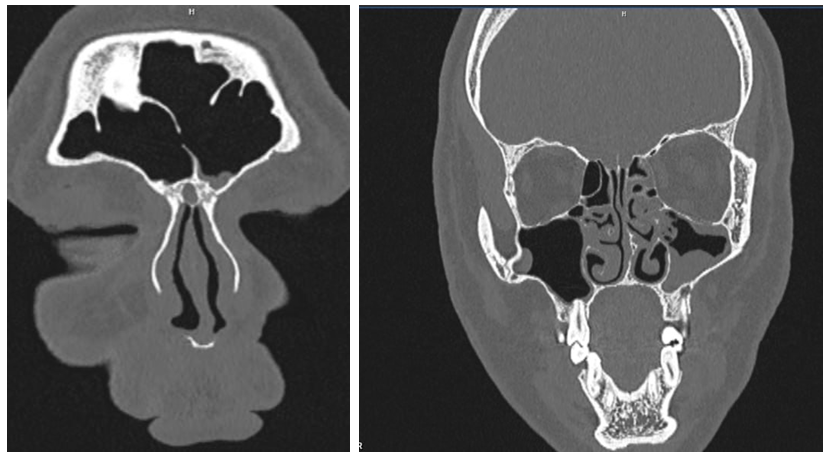 | Figure 2. MSCT – findings consistent with left-sided frontal sinusitis. Frontal sinuses – mucosal thickening at the floor of the left frontal sinus measuring 0.4–0.7 cm, +10 to +12 HU |
 | Figure 3. MSCT – findings consistent with ethmoiditis. Ethmoidal sinuses – pathological contents in the cells with a density of +4 to +10 HU |
4. Discussion
- The diagnostic value of computed tomography (CT) in assessing paranasal sinus pathology is well established, especially in complex or atypical cases where clinical symptoms alone are insufficient for accurate diagnosis. In the present study, we demonstrated that the incorporation of artificial intelligence (AI)–based image analysis into this process can enhance not only the accuracy but also the reproducibility and efficiency of CT interpretation. The proposed deep learning model showed strong performance in detecting a range of sinonasal abnormalities, including inflammatory, hyperplastic, and polypoid changes, as well as subtle bony alterations indicative of chronic disease. Our results are consistent with previous reports, which have highlighted the superiority of AI-assisted image interpretation over manual review in terms of detection rates and diagnostic speed. For instance, recent studies employing convolutional neural networks (CNNs) for sinusitis classification have reported accuracies between 82% and 88%, with sensitivity and specificity exceeding 80% in most cases [3,4]. In our dataset, the deep learning algorithm demonstrated comparable or superior accuracy while also providing automated segmentation and volumetric quantification — features that are not routinely available in conventional practice.One of the most important advantages observed was the system’s ability to identify minimal mucosal thickening and early-stage inflammatory changes that can be overlooked during visual inspection, particularly when they occur in anatomically complex regions such as the ethmoidal labyrinth. This aligns with the findings of Lee et al. (2024), who reported that AI-based detection improved the recognition of early mucosal disease by 12–15% compared with expert radiologists. Early recognition of such changes is crucial for initiating timely treatment and preventing disease progression toward chronic or complicated forms. From a clinical workflow perspective, AI integration offers several benefits. First, automated segmentation significantly reduces the time required for radiologic assessment by pre-highlighting regions of interest, enabling radiologists to focus on confirmation and interpretation rather than manual measurement. Second, standardized reporting generated by the AI system helps minimize interobserver variability, ensuring consistent terminology and classification. This is particularly relevant for multidisciplinary teams, where uniformity of radiologic descriptions facilitates clearer communication between otolaryngologists, radiologists, and surgeons.The color-coded overlay visualization method (Fig. 4) proved particularly valuable in bridging the gap between AI output and clinical interpretation. By allowing direct comparison of raw and segmented images, this approach increased the transparency of AI decisions and built user confidence in the technology. Similar strategies have been reported in recent AI-augmented diagnostic systems for thoracic and neuroimaging, where color overlays improved acceptance and integration into routine workflows. In terms of pathology-specific performance, our algorithm demonstrated high reliability in frontal sinusitis detection, particularly in identifying frontonasal duct obstruction — a key surgical consideration. For maxillary sinusitis, the model effectively differentiated between mucosal thickening, fluid accumulation, and polypoid lesions, enabling better preoperative planning. In ethmoiditis cases, the AI system excelled in mapping the extent of disease spread to adjacent sinuses, which is critical for avoiding incomplete treatment and recurrence. Nevertheless, the study has certain limitations. The dataset was collected from a single medical center, and although it included a balanced representation of different pathologies, multi-center validation would be necessary to confirm generalizability. Additionally, while the AI model performed well on CT images acquired in the soft-tissue window, further research is required to assess its robustness across different imaging protocols and scanner manufacturers. Expanding the training dataset to include rare pathologies, postoperative changes, and complications (e.g., orbital cellulitis, intracranial extension) could further improve model versatility. Looking ahead, the combination of AI with other diagnostic modalities — such as MRI, endoscopic imaging, and even laboratory biomarkers — could lead to truly comprehensive diagnostic platforms. Such multimodal systems could integrate structural, functional, and biochemical data to support precision medicine approaches, enabling not only diagnosis but also individualized prognostication and treatment planning. Moreover, as regulatory frameworks evolve and healthcare systems increasingly adopt AI technologies, the implementation of these solutions in routine otolaryngologic practice may become standard, particularly in tertiary care and specialized centers. In conclusion, our study demonstrates that deep learning–based image analysis of MSCT scans can significantly enhance the diagnosis of paranasal sinus pathologies, offering objective, reproducible, and clinically actionable insights. By reducing diagnostic variability, improving detection of subtle changes, and streamlining the reporting process, AI integration holds considerable promise for improving both patient outcomes and healthcare efficiency.
5. Conclusions
- The conducted study demonstrated that the integration of artificial intelligence (AI) technologies and digital radiologic processing into the diagnosis of paranasal sinus diseases represents a promising direction in the advancement of modern diagnostic radiology. The use of deep learning algorithms in the analysis of computed tomography data:• improves the accuracy and reproducibility of diagnostic results;• reduces image interpretation time, thereby increasing physician efficiency;• enables the detection of minimal pathological changes that may be inconspicuous during conventional visual analysis;• ensures the standardization of descriptions and reports, reducing interobserver variability.The obtained results confirm that AI systems can serve as a reliable decision-support tool, complementing but not replacing physician expertise. The greatest impact is achieved when AI is used in combination with highly informative imaging modalities (CT/MRI), digital radiologic processing modules, and automatic segmentation and classification algorithms.The further development of this technology is linked to the adaptation of algorithms to national medical image databases, their validation in multicenter studies, and their integration into everyday clinical practice. This will enhance diagnostic quality, optimize patient management pathways, and bring healthcare closer to the principles of personalized medicine. The findings of this study open broad opportunities for further advancement of AI technologies in the diagnosis of paranasal sinus diseases. Promising areas include the development of specialized algorithms for the detection of rare and complex pathologies, integration of multicenter databases to improve model generalizability, and the creation of a unified software platform that combines visualization, automatic segmentation, and standardized reporting modules. The implementation of these goals will not only improve diagnostic performance but also reduce the workload of specialists, optimize healthcare resource utilization, and expand access to high-tech medical care.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML