-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(8): 2753-2755
doi:10.5923/j.ajmms.20251508.70
Received: Aug. 4, 2025; Accepted: Aug. 23, 2025; Published: Aug. 30, 2025

Molecular Genetic and Biochemical Diagnostics of Cervical Cancer
Kurbonova Zumrad Chutbayevna1, Karimova Aziza Anvarovna2
1Associate Professor (DSc.), Department of Hematology, Transfusiology and Laboratory Work of the Tashkent Medical Academy, Tashkent, Uzbekistan
2Assistant, Department of Hematology, Transfusiology and Laboratory Work of the Tashkent Medical Academy, Tashkent, Uzbekistan
Correspondence to: Kurbonova Zumrad Chutbayevna, Associate Professor (DSc.), Department of Hematology, Transfusiology and Laboratory Work of the Tashkent Medical Academy, Tashkent, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

This study investigates the significance of molecular genetic and biochemical analyses in diagnosing cervical intraepithelial neoplasia (CIN) among climacteric women aged 50 to 75 years. Human Papillomavirus (HPV), particularly high-risk genotypes such as HPV 16, 18, 31, and 39, plays a critical role in the development of cervical cancer and its precancerous conditions. The presence of HPV was detected in 98% of women with cervical dysplasia. Biochemical markers including alkaline phosphatase, gamma-glutamyl transferase, total protein, and albumin were evaluated. Results showed significant increases in alkaline phosphatase and lactate dehydrogenase (LDH) in patients with high-grade squamous intraepithelial lesions (HSIL) and cervical cancer, while total protein and albumin levels decreased. Although these biochemical indicators are useful as diagnostic and prognostic markers, their effectiveness for early detection of precancerous lesions is limited.
Keywords: HPV, Cervical cancer, Cervical intraepithelial neoplasia (CIN), Alkaline phosphatase, Gamma-glutamyl transferase (GGT), Total protein, Albumin, Polymerase Chain Reaction (PCR), Cytological analysis
Cite this paper: Kurbonova Zumrad Chutbayevna, Karimova Aziza Anvarovna, Molecular Genetic and Biochemical Diagnostics of Cervical Cancer, American Journal of Medicine and Medical Sciences, Vol. 15 No. 8, 2025, pp. 2753-2755. doi: 10.5923/j.ajmms.20251508.70.
1. Introduction
- HPV viruses are a heterogeneous group, possessing double-stranded DNA in a closed, circular form. Not only cervical cancer, but also 5% of all cancer types are associated with HPV. High-risk HPV (hrHPV) causes nearly all cases of cervical cancer. However, the virus alone is not sufficient for the development of neoplastic processes. In 80-95% of cases where the virus is present, it is observed to disappear spontaneously by chance. In 10-15% of cases, cervical intraepithelial neoplasia can progress to invasive cervical cancer [9]. Overall, worldwide, cervical cancer arises due to persistent infection with one of 13 carcinogenic human papillomavirus (HPV) genotypes: They are genotypes 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, and 68 [8]. However, recent analyses of nearly a thousand cervical cancer cases from different regions of the world have shown that in patients, the HPV16 genotype is the most widespread type. Additionally, HPV16, HPV18, HPV31, or HPV45 have been identified in approximately 80% of cancers [4]. The scope and duration of HPV infection can be prolonged due to the following factors: Type of HPV and duration of infection, weakened immunity, poor nutrition, HIV infection, smoking, vitamin deficiencies, use of hormonal contraceptives, early age at first sexual intercourse, multiple sexual partners, disruption of the vaginal microbiome stability [2].Scientific observations show that having the first sexual intercourse before the age of 20 affects the frequency of cervical intraepithelial neoplasia. Theoretically, in women under 20 years old, the columnar cells of the cervix are more susceptible to metaplastic changes therefore, these cells have a five times higher risk of turning into cervical cancer [1]. Another factor that causes neoplastic changes in the cervix is smoking. The chemical carcinogenic effect of tobacco smoke on cells has been proven by several scientific studies. The direct effect of tobacco smoke on the cervical epithelium has not been fully proven, but statistical data show that neoplastic changes in the cervix occur more frequently in smoking women compared to non-smoking women [3].Women with acquired immunodeficiency virus (HIV) have a higher susceptibility to neoplastic changes in the cervix. This is manifested through immune suppression caused by HIV infection. Additionally, HPV is frequently found in women infected with HIV. In women with weakened immunity, it takes 10–20 years for HPV to cause neoplastic changes. In women with HIV, these neoplastic changes develop more rapidly. The World Health Organization’s guidelines for cervical cancer control recommend starting screening for cervical neoplastic processes immediately upon the detection of HIV infection, regardless of the age of girls or women [8].There are several factors besides HPV that contribute to the development of cervical cancer. An increasingly recognized cofactor in cervical carcinogenesis is the local microbiome [7]. Additionally, the composition of the vaginal microbiome plays a key role in the development of cervical intraepithelial neoplasia caused by HPV. In a healthy vaginal microbiome, there is a high amount of Lactobacillus, which produces lactic acid and creates an acidic environment. This helps maintain vaginal stability and prevents sexually transmitted infections [5].Purpose of the study: To study the importance of molecular genetic and biochemical analyses in the diagnosis of cervical intraepithelial neoplasia in women of climacteric age.
2. Materials and Methods of the Study
- The studies were conducted at the Multidisciplinary Clinical Consultative Polyclinic of the Tashkent Medical Academy during 2022–2024. During the study, We selected women aged 50 to 75 years in the climacteric period with cytological diagnoses of Atypical Squamous Cells of Undetermined Significance (ASCUS, group 1), Low-Grade Squamous Intraepithelial Lesion (LSIL, group 2), Atypical Squamous Cells, cannot exclude High-grade squamous intraepithelial lesion (ASC-H, group 3), High-Grade Squamous Intraepithelial Lesion (HSIL, group 4) and cervical cancer (CC, group 5) In these women, alongside cytological analysis, polymerase chain reaction (PCR) and biochemical tests were performed.
3. Results
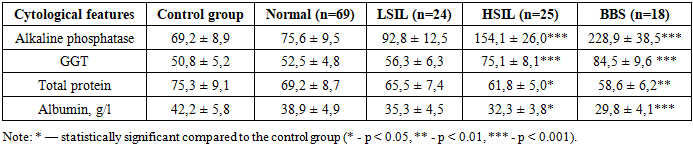
- HPV was detected in 98% of women diagnosed with cervical dysplasia. The most frequently detected HPV genotype 16 was found in 1 woman (2%) in groups 1 and 2, in 3 women (3%) in group 3, in 20 women (20%) in group 4, and in 17 women (17%) in group 5, totaling 42% of the women. HPV genotype 18 was detected in 8% of women, including 1 woman (1%) in group 3, 4 women (4%) in group 4, and 3 women (3%) in group 5. HPV genotype 39 was found in 7% of women, specifically 1 woman (1%) in group 2, and 2 women each (totaling 7%) in groups 3, 4, and 5. HPV genotypes 31, 33, 45, and 59 were detected in 4 women each, totaling 16% of the women, while HPV genotype 35 was found in 2 women. In women of climacteric age with precancerous conditions and cervical cancer, biochemical indicators such as alkaline phosphatase, gamma-glutamyl transferase, total protein, and albumin levels were examined. Alkaline phosphatase showed elevated levels mainly in HSIL and cervical cancer cases.
|
4. Conclusions
- Conclusion, alkaline phosphatase and LDH significantly increase in cervical cancer and HSIL, while total protein and albumin decrease. These indicators can be used as diagnostic and prognostic markers, However, their effectiveness for early diagnosis of precancerous cervical conditions is low. Biochemical analyses can also be used as diagnostic markers, but their effectiveness for early diagnosis of precancerous cervical conditions is low. HPV genotypes 16, 18, 31, and 39 are mainly observed in patients diagnosed with severe dysplasia and cervical cancer. However, the presence of HPV viruses does not always correspond to cytological changes, Therefore, although the presence of HPV is significant as a prognostic marker, it may not be accurate as a diagnostic marker for cervical cancer (CC) and HSIL.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML