-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(8): 2740-2744
doi:10.5923/j.ajmms.20251508.67
Received: Aug. 6, 2025; Accepted: Aug. 26, 2025; Published: Aug. 30, 2025

Antigen-Binding Lymphocytes as Potential Biomarkers of Exogenous and Endogenous Endophthalmitis
Kamilov Kh. M.1, Maksudova L. M.2, Rustamova K. B.3
1DSc, Professor, Head of the Department of “Ophthalmology” of the Center for the Development of Professional Qualifications of Medical Personnel, Tashkent, Uzbekistan
2DSc, Associate Professor of the Department of “Ophthalmology”, Center for Advanced Medical Personnel Training, Tashkent, Uzbekistan
3Freelance Applicant for the Department of Ophthalmology of the Center for Advanced Medical Personnel Training, Tashkent, Uzbekistan
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Despite advances in medicine over the past 100 years, endophthalmitis is still a serious vision-threatening complication. The aim of the study is to investigate the role of some immunological indicators in the early diagnosis of eye structure damage in exogenous and endogenous endophthalmitis. The study was conducted on 101 patients. To study organ damage and the effectiveness of the therapy, a method of quantitative registration of antigen-binding lymphocytes (ABL) specifically sensitized relative to tissue antigens (TA) of the cornea, sclera, retina and choroid was used. In the conducted comparative analysis of the dynamics of antigen-binding lymphocytes (ABL) to tissue antigens of eye structures in patients with inflammatory diseases of exogenous and endogenous nature, significant features of the course of the inflammatory process and the effectiveness of the treatment were revealed.
Keywords: Endophthalmitis, Antigen-binding lymphocytes, Tissue antigens, Intracellular processes, Exogenous and endogenous
Cite this paper: Kamilov Kh. M., Maksudova L. M., Rustamova K. B., Antigen-Binding Lymphocytes as Potential Biomarkers of Exogenous and Endogenous Endophthalmitis, American Journal of Medicine and Medical Sciences, Vol. 15 No. 8, 2025, pp. 2740-2744. doi: 10.5923/j.ajmms.20251508.67.
1. Introduction
- The relevance of studying endogenous and exogenous inflammatory processes in the structures of the eye is due to their significant impact on vision and quality of life of patients. Inflammatory eye diseases are among the leading ophthalmic pathologies, as they can lead to serious complications such as decreased visual acuity, glaucoma, cataracts, or even blindness [1,2].Endogenous inflammation occurs as a result of internal factors such as autoimmune reactions, systemic diseases, or infections within the body, which requires a deep understanding of the mechanisms of their development for timely diagnosis and adequate treatment [5]. Exogenous inflammation is associated with external influences — trauma, infections, allergens — and requires the development of methods for prevention and rapid response [3,4].Studying these processes is important for identifying pathogenetic mechanisms, determining risk factors, and developing new therapeutic approaches. This helps to reduce the frequency of complications, preserve visual function, and improve the quality of life of patients. In the context of modern medical developments, such research helps to improve methods of diagnosis, prevention, and treatment of inflammatory eye diseases [6,7].The objective of our study was to examine the role of certain immunological indicators in the early diagnosis of endogenous and exogenous damage to eye structures.
2. Methods and Materials
- We carried out our research on 101 patients who were treated at the Republican Clinical Ophthalmological Hospital under the Ministry of Health of the Republic of Uzbekistan from 2022 to 2024 for inflammatory eye diseases of an endogenous (n=60) and exogenous (n=41) nature. hospitalized with a diagnosis of endophthalmitis. All patients complained of pain, redness of the eyes, discharge from the eyes, and blurred vision upon admission.To study organ damage and the effectiveness of the therapy, we used a method of quantitative registration of antigen-binding lymphocytes (ABL) specifically sensitized to tissue antigens (TA) of the cornea, sclera, retina, and choroid, based on the use of the indirect rosette formation reaction (IRFR) according to the method of Garib F.Yu. (1995). All patients underwent ABL testing for TA during the course of the disease at the following time points: upon admission, and at 5, 14, and 30 days of observation. The essence of the method for determining the ABL to TA of various organs is that when an organ of any origin is damaged, intracellular processes are disrupted and destruction develops in its cells. Molecules or fragments of structural and functional proteins with organ specificity enter the internal environment. Tissue proteins and molecules that are “foreign” to the internal environment acquire the status of tissue antigens (TA), triggering an immune response aimed at their neutralization and elimination.In the presence of TA in the internal environment, antigen-binding lymphocytes (ABL) differentiate and circulate in the blood, capable of specifically binding to TA only of a given organ. The level of ABL to TA reflects the intensity of the processes of destruction and necrosis of structures in the organ: an increase in ABL over time indicates an increase, and a decrease in ABL indicates a decrease in the intensity of these processes, which allows one to assess the degree of organ damage, as well as the effectiveness of the therapy being carried out. The value of the method for determining ABL to TA is its high sensitivity and specificity: the ABL content reaches a diagnostic level in the early stages and long before the manifestation of clinical signs of organ damage, which makes it possible to predict the risk of organ failure at an early stage. The determination of ABL with TA in several organs allows the detection of multiple organ damage in the development of pathology.
3. Research Results
- A comparative analysis of the dynamics of antigen-binding lymphocytes to tissue antigens of eye structures in endogenous and exogenous inflammatory processes showed that with a unidirectional nature of the body's response to the treatment, there are differences in the severity and intensity of the decrease in ABL indicators to TAG structures of the eye at different observation times. The analysis of the dynamics of ABL to TAG of the cornea at admission in the patients we examined showed equally high levels of values (25.17±0.73% and 27.81±1.22%, respectively), significantly exceeding the control values by 17.2 and 19.04 times, respectively. On the 5th day of observation, a decrease in the ABL to TAG ratio of the cornea was noted with the same intensity by 1.1 times (23.92±0.76% and 24.58±0.69%, respectively). On the 14th day of treatment and observation in group 2, there was a more expressed decrease (2.3 times, 10.42±0.48%) relative to the previous value than in patients with endogenous inflammation (1.5 times, 15.78±0.55%, respectively) (Fig. 1).
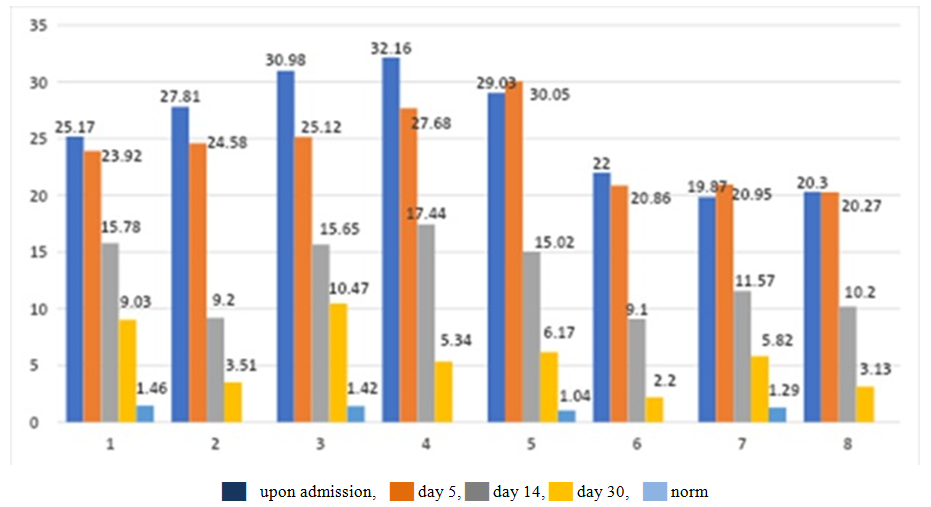 | Figure 1. Dynamics of antigen-binding lymphocytes to TAG in patients with inflammatory diseases of the eye structures of exogenous and endogenous nature |
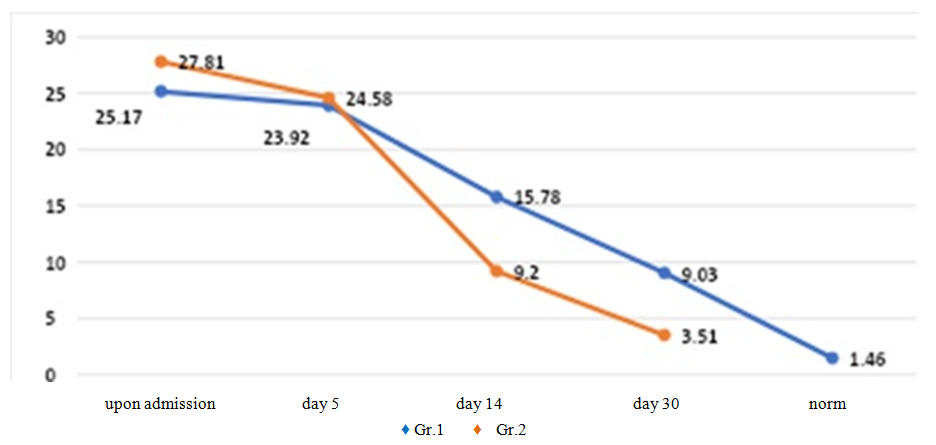 | Figure 2. Dynamics of antigen-binding lymphocytes to corneal TAG in patients with inflammatory diseases of exogenous and endogenous nature |
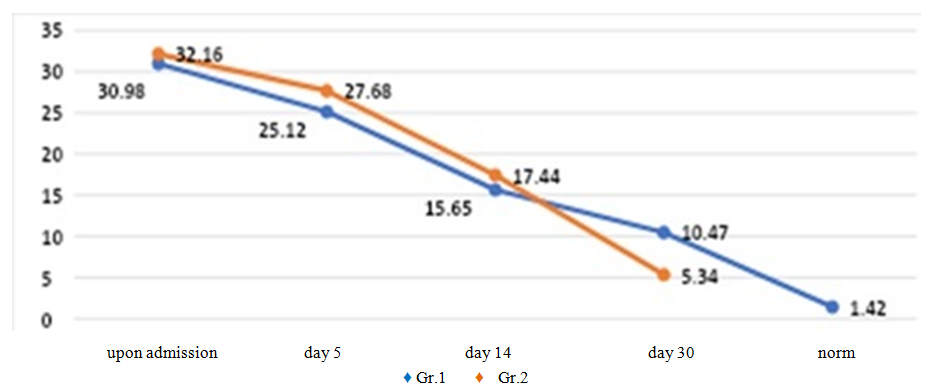 | Figure 3. Dynamics of antigen-binding lymphocytes to TAG of the vascular membrane in patients with inflammatory diseases of exogenous and endogenous nature |
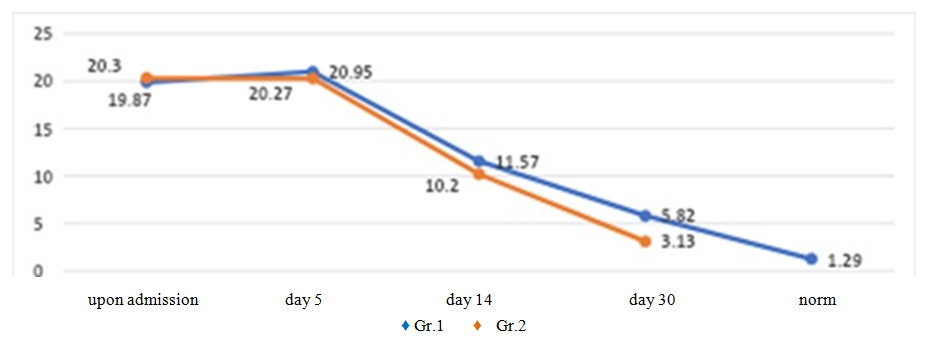 | Figure 4. Dynamics of antigen-binding lymphocytes to retinal TAG in patients with inflammatory diseases of exogenous and endogenous nature |
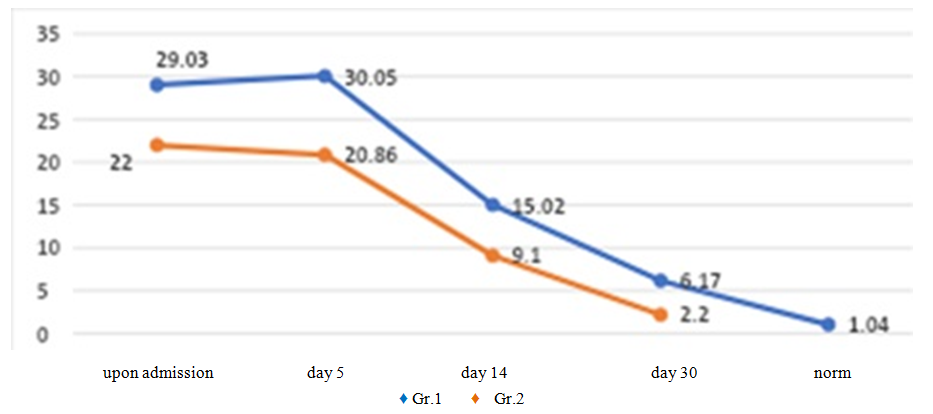 | Figure 5. Dynamics of antigen-binding lymphocytes to TAG of the sclera in patients with inflammatory diseases of exogenous and endogenous nature |
4. Conclusions
- 1. Inflammatory processes in the eye structure in endogenous diseases are characterized by more persistent immune response activity and a slower rate of regression of inflammatory changes compared to exogenous causes.2. The effectiveness of treatment is higher in patients with exogenous inflammation, which is manifested in a more significant reduction in ABL levels to tissue antigens of the eye structures.3. The dynamics of ABL changes can serve as an objective marker for assessing the effectiveness of therapy and the prognosis of inflammatory eye diseases.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML