-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(8): 2523-2528
doi:10.5923/j.ajmms.20251508.22
Received: Jul. 9, 2025; Accepted: Jul. 27, 2025; Published: Aug. 4, 2025

Epidemiological Patterns and Nutritional Determinants of Gastrointestinal Diseases in Hot Climates: A Case Study from Surkhandarya, Uzbekistan
Shaykhova Guli Islamovna1, Shoymardonov Bakhtiyor Kholnazarovich2, Avezova Guloyim Sattarovna3
1Head of the Department of Pediatrics, Adolescent Medicine, and Nutrition Hygiene at the Tashkent Medical Academy, Doctor of Medical Sciences, Professor, Tashkent, Uzbekistan
2Assistant at the Department of Microbiology, Public Health, Hygiene, and Management of the Termez Branch of the Tashkent Medical Academy, Tashkent, Uzbekistan
3Department of Propaedeutics of Children’s Diseases, Tashkent Medical Academy, Tashkent, Uzbekistan
Correspondence to: Avezova Guloyim Sattarovna, Department of Propaedeutics of Children’s Diseases, Tashkent Medical Academy, Tashkent, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Background: Gastrointestinal (GI) disorders represent a major public health concern in hot-climate regions such as Surkhandarya, Uzbekistan. Environmental stressors, poor nutrition, and limited public health infrastructure contribute to the high prevalence of GI illnesses. Objectives: This study aims to assess the prevalence and risk factors of GI diseases in the Surkhandarya region, analyze seasonal and demographic dietary patterns, and propose a culturally tailored, preventive nutritional strategy. Methods: A mixed-methods approach was employed, including epidemiological analysis (2017–2024), a case-control study with 600 participants, and seasonal dietary surveys based on SanPin 0007-2020 nutritional guidelines. Statistical analysis was performed using Statistica for Windows 7.0. Results: GI disease prevalence fluctuated over time, with a sharp increase post-COVID-19 due to resumed medical screenings. Poor dietary quality, inadequate hydration, psychosocial stress, and irregular meal patterns were identified as primary risk factors. Nutritional assessments revealed widespread deficiencies in protein, calcium, vitamins A and C, and water intake. A seven-day preventive diet incorporating national dishes and seasonal adjustments is proposed. Conclusions: Addressing the regional burden of GI diseases requires a multifactorial approach integrating dietary reform, public education, and environmental health improvements. The proposed model offers an adaptable strategy for similar hot-climate regions facing nutrition-related chronic diseases.
Keywords: Gastrointestinal diseases, Nutrition, Climate and health, Dietary deficiencies, Preventive diet, Uzbekistan, Surkhandarya, Public health, Seasonal food intake, Hot climate adaptation
Cite this paper: Shaykhova Guli Islamovna, Shoymardonov Bakhtiyor Kholnazarovich, Avezova Guloyim Sattarovna, Epidemiological Patterns and Nutritional Determinants of Gastrointestinal Diseases in Hot Climates: A Case Study from Surkhandarya, Uzbekistan, American Journal of Medicine and Medical Sciences, Vol. 15 No. 8, 2025, pp. 2523-2528. doi: 10.5923/j.ajmms.20251508.22.
Article Outline
1. Introduction
- The preservation and promotion of public health, prevention of chronic diseases, and encouragement of healthy lifestyles remain among the highest priorities for national healthcare systems globally. These objectives become particularly critical in regions with extreme climatic conditions, such as the southern territories of Uzbekistan, including the Surkhandarya region, where gastrointestinal diseases are notably prevalent.The high incidence of digestive system disorders in this region has been attributed to several environmental and lifestyle factors. Among them are suboptimal sanitary and hygienic conditions, prolonged exposure to elevated temperatures that facilitate microbial proliferation, and widespread nutritional imbalances in the local population. These challenges have been previously discussed in both domestic and international literature, highlighting the unique epidemiological profile of gastrointestinal (GI) illnesses in hot climates [1,3,7,12,17].Several researchers have emphasized the crucial role of food safety and nutritional quality in the etiology of GI diseases, particularly under conditions of high temperature and humidity. In Surkhandarya, however, there remains a significant gap in localized studies focusing on traditional dietary habits, food storage practices, and sanitary standards of commonly consumed food products [2,9,10,13,15,19,20].Evidence suggests that the risk of gastrointestinal diseases can be significantly mitigated by tailoring dietary patterns to accommodate epidemiological, toxicological, and hygienic characteristics specific to regional food items [6,8,11,14]. Within the context of Uzbekistan, the development of effective prevention strategies through the integration of national dishes into balanced diets represents a critical and timely area of public health intervention.Despite recent efforts to evaluate local dietary patterns and their health implications, a scientifically grounded preventive nutrition model tailored specifically for Surkhandarya has yet to be established. Addressing this gap is essential to improve regional health outcomes and reduce the burden of chronic digestive disorders.
2. Objectives and Significance
- The primary aim of this study is to investigate the prevalence and risk factors associated with gastrointestinal (GI) diseases among residents living in hot climatic conditions, with a specific focus on the Surkhandarya region of Uzbekistan. Additionally, the study seeks to analyze the actual dietary patterns of the local population and develop a culturally appropriate, nutritionally balanced seven-day meal plan enriched with traditional Uzbek dishes.This research holds both scientific and practical significance:• Epidemiological Relevance: By examining regional trends in GI disease prevalence and associated demographic patterns, this study provides a comprehensive understanding of disease distribution in a climatically vulnerable area.• Public Health Impact: The findings support the development of targeted public health strategies aimed at reducing the burden of chronic digestive disorders through nutritional interventions.• Nutritional Strategy Development: The study offers evidence-based recommendations for dietary planning that align with national food traditions, hygiene standards, and nutritional needs.• Policy and Practice Implications: Results may inform healthcare policy, nutritional guidelines, and community health programs aimed at improving dietary behavior and mitigating climate-related health risks.Ultimately, this work addresses a critical gap in regional healthcare by offering scientifically grounded insights into the interplay between climate, nutrition, and gastrointestinal health, and provides a foundation for effective preventive measures.
3. Materials and Methods
- This study was conducted under the research plan of the Department of Hygiene of Children, Adolescents, and Nutrition at the Tashkent Medical Academy. A multi-phase approach was employed to ensure a comprehensive investigation into the prevalence and dietary risk factors of gastrointestinal (GI) diseases in Surkhandarya.Phase I: Epidemiological AssessmentThe first stage involved analyzing trends in the incidence and prevalence of GI diseases across Surkhandarya from 2017 to 2022. Data were obtained at both regional and district levels, with a focus on hospital admissions, primary healthcare visits, and routine medical examinations. Key districts surveyed included Termez, Angor, Jarkurgan, and Sherabad.Phase II: Clinical Case AnalysisThe second phase focused on healthcare utilization patterns. Patient records from regional medical centers were analyzed to assess the frequency and type of hospitalizations related to GI disorders. Age and gender distributions were examined, and disease severity and comorbidities were recorded.Phase III: Case-Control StudyTo investigate risk factors, a case-control study was conducted involving 300 patients diagnosed with GI disorders and 300 healthy controls. A structured questionnaire was developed to collect data on lifestyle, environmental conditions, and dietary habits. This allowed for identification of behavioral and environmental risk factors specific to the local population.Phase IV: Nutritional EvaluationIn the final phase, the actual dietary intake of patients was assessed across all four seasons. Data were collected over 10-day periods (3 days early month, 4 mid-month, 3 end-month) to account for seasonal variations. Nutritional intake was evaluated using 38 dietary indicators, in accordance with:• SanPin 0007-2020: “Rational average daily dietary norms for the population of Uzbekistan by age, gender, and professional activity.”• Food Composition Tables: To assess caloric and nutrient content.Analytical and Statistical ToolsData were classified according to ICD-10 (International Classification of Diseases, 10th Revision). Statistical analysis was performed using Statistica for Windows 7.0, focusing on prevalence trends, nutritional adequacy, and associations between dietary habits and GI disease risk.
4. Epidemiological Trends in Gastrointestinal Diseases
- Gastrointestinal (GI) disorders encompass a wide spectrum of pathologies, including peptic ulcer disease, liver disorders, pancreatitis, intestinal diseases, and various neoplastic conditions. These diseases fall under Class XI (K00–K93) of the International Classification of Diseases (ICD-10) and present diverse etiological and clinical features.Regional Disease Dynamics (2017–2024). An epidemiological analysis of GI disease prevalence in Surkhandarya from 2017 to 2024 revealed a fluctuating pattern. The incidence rate in 2017 was 768.8 per 10,000 people, decreasing to 439.7 in 2022 — a 56.1% reduction. However, this trend reversed in subsequent years, with rates rising to 582.3 in 2023 and 650.4 in 2024, marking a 32.3% increase over the past three years.This pattern likely reflects two overlapping factors:1. Underreporting during the COVID-19 pandemic (2020–2021), which led to fewer hospital visits and delayed diagnoses.2. Increased screening and check-ups post-pandemic, which unearthed previously undetected latent GI diseases.Age and Gender Distribution. A deeper age-stratified analysis showed varied patterns: Adolescents (15–17 years): GI disease prevalence increased from 45.3 to 75.6 per 10,000. Adults (18–65 years): Rates rose from 272.3 to 480.7 per 10,000, a 58.1% increase. Elderly (>65 years): Although overall lower, prevalence increased by 9.3%, from 35.4 to 38.9 per 10,000.Gender-specific data indicated that men had a higher incidence than women. In 2022, male incidence was 180.8 per 1,000, rising to 220.4 in 2024, marking a 39.6% increase.Disease Comorbidities and Hospital Admissions/ Common comorbid conditions associated with GI diseases included: anemia (37.4%), hepatitis (29.6%), chronic pyelonephritis (21.7%), cholecystitis (7.0%). Less frequent were associations with rheumatism, osteochondrosis, and splenopathy. Hospital admission data showed that 94% of GI-related hospitalizations were due to: chronic pancreatitis, peptic ulcer disease, chronic cholecystitis, gastritis and duodenitis, hepatitis and cirrhosis. These findings underscore the need for improved diagnostics and targeted interventions, particularly in underserved districts of Surkhandarya.
5. Nutritional Assessment and Dietary Analysis
- Methodology of Nutritional Data CollectionTo evaluate the nutritional status and dietary habits of the population, a detailed analysis of actual food consumption was conducted over four seasons—winter, spring, summer, and autumn. Data were gathered over a 10-day period in each season, split into early, mid, and late-month sampling windows. Participants documented their intake using structured food diaries and were surveyed using a specially designed questionnaire addressing:• Frequency of meals• Types of food consumed (meat, dairy, grains, vegetables, sweets)• Intake of refined fats, sugars, and beveragesDaily intake values were compared with the nationally recommended dietary norms (SanPin 0007-2020) for different demographic groups.Key Nutritional Deficiencies IdentifiedThe analysis revealed several critical gaps between actual consumption and dietary recommendations:• Energy intake was 66–88% of the recommended level.• Protein intake was moderately low, meeting only 56–77% of the requirement in some groups.• Fat and carbohydrate intake also fell short of guidelines, particularly in winter-spring.• Micronutrients, including vitamin A, vitamin C, calcium, and iron, showed significant deficiencies.• Water consumption was below optimal levels, especially during colder months.A summary of these findings is presented below:
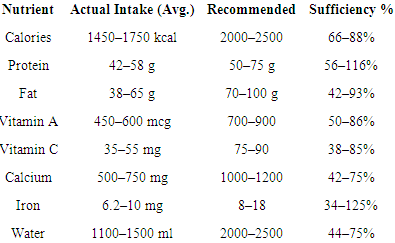 Seasonal Variations in Dietary Patterns• Winter–Spring: Marked by insufficient intake of fresh vegetables, fruits, protein, and fluids, leading to shortages in vitamin C, iron, and calcium.• Summer–Autumn: Increased consumption of fruits and vegetables due to seasonal availability, though protein and calcium remained suboptimal. Water intake improved due to heat-related hydration needs.Food group analysis showed:• Meat and dairy consumption was consistently 35–45% below recommended levels.• Egg consumption reached only 10–20% of the ideal.• Fresh fruits and vegetables intake fell short by 20–40%, especially in colder seasons.Implications of Dietary ImbalanceThe observed nutrient deficiencies contribute to:• Weakened immune response• Increased vulnerability to infections• Poor recovery from GI disorders• Risk of comorbid chronic conditionsA key conclusion is that both the quantity and quality of the local diet must be improved. This includes promoting regular meals, diversifying food choices, increasing fluid intake, and ensuring access to seasonally appropriate, nutrient-rich foods.
Seasonal Variations in Dietary Patterns• Winter–Spring: Marked by insufficient intake of fresh vegetables, fruits, protein, and fluids, leading to shortages in vitamin C, iron, and calcium.• Summer–Autumn: Increased consumption of fruits and vegetables due to seasonal availability, though protein and calcium remained suboptimal. Water intake improved due to heat-related hydration needs.Food group analysis showed:• Meat and dairy consumption was consistently 35–45% below recommended levels.• Egg consumption reached only 10–20% of the ideal.• Fresh fruits and vegetables intake fell short by 20–40%, especially in colder seasons.Implications of Dietary ImbalanceThe observed nutrient deficiencies contribute to:• Weakened immune response• Increased vulnerability to infections• Poor recovery from GI disorders• Risk of comorbid chronic conditionsA key conclusion is that both the quantity and quality of the local diet must be improved. This includes promoting regular meals, diversifying food choices, increasing fluid intake, and ensuring access to seasonally appropriate, nutrient-rich foods.6. Risk Factors and Lifestyle Influences
- The development and progression of gastrointestinal (GI) disorders in the Surkhandarya region are influenced by a complex interplay of medical, social, behavioral, and environmental factors. This study identified both sociodemographic vulnerabilities and nutritional behaviors that contribute significantly to the burden of disease.Medical and Psychosocial Risk FactorsAnalysis of patient interviews and survey data highlighted several prominent medical-social determinants: Family stress and domestic conflicts: Frequently reported as chronic stressors, contributing to both the onset and exacerbation of GI conditions.• Living conditions: Inadequate housing, poor sanitation, and lack of access to clean drinking water were associated with higher disease prevalence.• Mental health: Anxiety and depressive symptoms were common among patients with chronic GI illnesses, suggesting a psychosomatic link.These factors align with global research showing that psychological and environmental stressors can significantly impact gut health, alter motility, and disrupt microbiota balance.Dietary Habits and Nutrition-Related RisksThe study revealed several unfavorable eating patterns that directly influence GI morbidity:• Irregular meal timing and infrequent eating (fewer than 3 meals/day)• Overeating at night or consuming large meals before bed• Low dietary diversity, with monotonous food choices lacking essential nutrients• High intake of spicy, salty, and fatty foods• Excessive consumption of black tea and coffee• Use of refined sugars and processed foods• Low fluid intake, particularly in cooler seasonsIn addition, alcohol consumption, though lower in frequency, was noted in specific demographic groups and contributed to hepatic and gastric complications.Seasonal and Gender-Based Observations. Men showed higher incidence of peptic ulcers, chronic hepatitis, and cirrhosis—linked with both stress and poor dietary regulation. Women had higher rates of gallbladder disease, chronic gastritis, and duodenitis—possibly related to hormonal factors and dietary choices. Seasonal fluctuations in food availability and water intake also influenced disease patterns, with winter-spring periods correlating with increased symptom severity due to nutrient deficiencies.Cumulative Risk Impact. The synergy between psychosocial stressors, poor dietary practices, and environmental hardship amplifies disease risk. This underscores the need for multifactorial interventions—including dietary counseling, stress management, and improvements in sanitation and public awareness.
7. Recommended Preventive Diet and Nutritional Strategy
- Based on the analysis of dietary patterns and the health status of residents in Surkhandarya, a preventive nutritional framework has been proposed. This approach emphasizes seasonal adaptation, nutritional balance, and integration of national culinary traditions, while addressing the deficiencies most commonly observed in the region.Guiding Principles of Preventive Nutrition. The preventive dietary plan was developed in accordance with:• National guidelines (SanPin 0007-2020)• Actual dietary intake data across seasons• Medical needs of patients with chronic gastrointestinal conditionsCore principles include:• Increased meal frequency: From 3 to 4–5 small, balanced meals per day• High water intake: Especially in summer, up to 2.5–4.0 liters daily• Moderate protein: From lean meat, eggs, and legumes• Reduced fats and sugars: With a focus on plant-based oils• High fiber: From whole grains, seasonal fruits, and vegetables• Gentle cooking methods: Emphasizing steaming, boiling, and bakingSeven-Day Preventive Meal PlanA culturally appropriate seven-day meal plan was designed using traditional Uzbek ingredients and recipes, optimized for nutritional value. This includes:• Breakfast: Whole grains (e.g., buckwheat, millet), low-fat dairy, fresh fruit, herbal tea• Lunch: Vegetable-based soups (e.g., shurpa), lean meat with legumes, side salads, flatbread• Dinner: Light porridge or steamed vegetables, yogurt, and fruit• Snacks: Dried fruits, nuts, green tea, low-fat fermented milk products (e.g., katyk)Seasonal ingredients were prioritized—for instance, melons, tomatoes, and cucumbers in summer; root vegetables, dried legumes, and preserved fruits in winter.Nutritional Corrections by SeasonWinter–Spring Adjustments:• Increase consumption of dried fruits, legumes, and vitamin C-rich vegetables (e.g., cabbage, carrots)• Ensure adequate intake of animal protein to compensate for cold-induced energy demandsSummer–Autumn Adjustments:• Emphasize hydration with clean water, ayran, and herbal teas• Favor fresh, water-rich vegetables and fruits• Limit heavy, fatty meals that may impair digestion in hot conditionsSpecial Recommendations for Older AdultsFor individuals aged 50 and older:• Nutrient-dense meals with high calcium (e.g., dairy, leafy greens)• Soft, easy-to-digest preparations to support age-related GI sensitivity• Emphasis on gentle spices and avoiding highly acidic or salty foodsPublic Health IntegrationThis dietary model can be incorporated into local public health campaigns, particularly through:• Community health workshops• Educational materials at primary care clinics• Nutrition counseling at gastroenterology departmentsThese strategies aim to empower individuals with knowledge and access to affordable, culturally relevant food choices that support digestive health in a hot climate.
8. Conclusions and Public Health Implications
- This study provides a comprehensive examination of gastrointestinal (GI) diseases in Surkhandarya, Uzbekistan, revealing critical links between hot climatic conditions, nutritional deficiencies, and lifestyle risk factors.Key Findings1. Epidemiological Fluctuation: GI disease prevalence exhibited a wave-like trend from 2017 to 2024. A marked decrease during the COVID-19 pandemic was followed by a post-pandemic surge in diagnosed cases, reflecting renewed health screenings and the re-registration of latent illnesses.2. Age and Gender Disparities: A significant rise in disease incidence was observed across all age groups from 2022 to 2024, particularly among:ο Adolescents (15–17): +66.9%ο Working-age adults (18–65): +58.1%ο Elderly (>65): +25.2%Men were more frequently affected by ulcerative and hepatic conditions, while women showed higher rates of gallbladder and gastric disorders.3. Lifestyle and Behavioral Risks: Social stress, poor living conditions, irregular meal patterns, consumption of spicy and fatty foods, and low fluid intake were major contributors to GI morbidity.4. Nutritional Gaps: Both seasonal and demographic analysis revealed consistent underconsumption of protein, dairy, vegetables, fruits, vitamins, and water—most severely in winter and among older adults. This imbalance significantly impairs digestive health and immune resilience.5. Therapeutic Recommendations: To accelerate recovery and reduce disease recurrence, patients should adopt a preventive diet with increased meal frequency, fluid intake, and nutrient-dense food choices tailored to their age, health status, and season.6. Dietary Strategy for Hot Climates: For populations in arid regions, particularly those with chronic GI diseases, a light, easily digestible, and hydrating diet is essential. Meals should be prepared using low-fat methods such as boiling or steaming, and seasoning should be used cautiously. Above all, diet should align with medical advice and individual needs.Implications for Public HealthThis research highlights the pressing need for:• Nutritional education campaigns• Development of regional dietary guidelines• Community-based preventive interventions• Enhanced access to balanced, locally sourced foodUnderstanding the relationship between climate, food, and digestive health can inform policy changes that promote long-term well-being in climate-vulnerable populations.By integrating traditional culinary practices with modern nutritional science, and by addressing environmental and behavioral risk factors, it is possible to significantly reduce the burden of gastrointestinal disease and improve quality of life in hot-climate regions such as Surkhandarya.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML