-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(7): 2391-2396
doi:10.5923/j.ajmms.20251507.63
Received: Jun. 18, 2025; Accepted: Jul. 12, 2025; Published: Jul. 30, 2025

A Comprehensive Study of Cognitive and Physical Changes in Dementia
Gulnara S. Rakhimbayeva1, Mukhaddas R. Kamilova2, Dildora R. Sobirova3
1Head of the Department of Neurology and Medical Psychology, DSc, Professor of Tashkent Medical Academy, Uzbekistan
2Scientific Researcher of the Department of Neurology and Medical Psychology, Tashkent Medical Academy, Uzbekistan
3Associate Professor of the Histology and Medical Biology Department, PhD, Tashkent Medical Academy, Uzbekistan
Correspondence to: Gulnara S. Rakhimbayeva, Head of the Department of Neurology and Medical Psychology, DSc, Professor of Tashkent Medical Academy, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Relevance: Dementia is one of the most pressing and serious medical issues, given its impact on patients' quality of life and the burden it places on healthcare systems. Research aimed at understanding the relationship between physical and cognitive changes in dementia is crucial for developing effective methods of diagnosis, treatment, and rehabilitation. It is important to recognize that changes in body weight, body image perception, and cognitive functions can mutually influence one another, requiring a comprehensive approach to treating patients. Aim of the Study: The aim of this study was to examine changes in body weight, cognitive functions, functional abilities, and body image perception in patients with dementia over a 90-day period, as well as to explore the relationships between these factors. Methods and Materials: The study included 20 dementia patients who were observed at three visits: at baseline (first visit), after 30 days (second visit), and after 90 days (third visit). Body weight was measured using standard scales, cognitive functions were assessed using the MMSE (Mini-Mental State Examination), functional abilities were evaluated using the CDR (Clinical Dementia Rating), and body image perception was measured using the Image Evaluation scale. Statistical analysis involved evaluating the dynamics of each parameter over the study period. Results: The results showed a significant decrease in body weight in patients, while cognitive functions and functional abilities either improved or remained stable. Body image perception also demonstrated positive dynamics. These findings highlight the complex interrelationship between physical state, cognitive functions, and body image perception in dementia patients. Conclusions: The results of the study emphasize the importance of a comprehensive approach in diagnosing and treating dementia patients. Despite the decrease in body weight, the improvement in cognitive functions and body image perception suggests that there may be a possibility of compensating for some symptoms of the disease with proper care and therapy. Further research is needed to gain a deeper understanding of the mechanisms behind these changes.
Keywords: Dementia, Body weight, Cognitive functions, Functional abilities, Body image perception, MMSE, CDR, Image Evaluation
Cite this paper: Gulnara S. Rakhimbayeva, Mukhaddas R. Kamilova, Dildora R. Sobirova, A Comprehensive Study of Cognitive and Physical Changes in Dementia, American Journal of Medicine and Medical Sciences, Vol. 15 No. 7, 2025, pp. 2391-2396. doi: 10.5923/j.ajmms.20251507.63.
Article Outline
1. Introduction
- Instead of being a single illness, dementia [1] is a collection of conditions marked by progressively worsening cognitive abilities like memory, attention, planning, and decision-making. These cognitive deficits significantly impact patients' daily lives and their ability to perform self-care activities. This group of diseases, which includes Alzheimer’s disease [2], vascular dementia, and other neurodegenerative conditions, presents a serious challenge in both healthcare and social sectors, given the age-related nature of the disease and the high demand for long-term care and treatment [3,4]. In recent decades, scientific attention has increasingly focused not only on traditional aspects of dementia diagnosis and treatment but also on various additional factors that may influence the development and progression of the disease, as well as its severity. Among these factors are physical parameters, such as body mass and changes in body image, which may be related to neurodegenerative processes [5-7].Body mass and body image perception play an important role in dementia research because changes in these indicators can serve as key markers of cognitive decline and overall health deterioration [8]. In dementia patients, various patterns of body weight changes are often observed, such as weight loss or, conversely, weight gain. These changes may be linked to dysfunctions in the hypothalamus or disturbances in metabolic processes characteristic of neurodegenerative diseases [9]. Therefore, body mass is not only an indicator of general health but also an important marker for assessing the disease’s prognosis. Studying the relationship between changes in body mass and cognitive impairments can provide valuable insights into the physiological changes occurring in the patient’s body. This, in turn, may aid in the development of new methods for early dementia diagnosis and monitoring its progression.Body image assessment is another crucial aspect of dementia research, as changes in body perception in patients can be associated with cognitive and emotional disturbances. Patients with dementia often experience dysfunctions in how they perceive their own bodies, such as distorted body image, an inability to assess the size and shape of their body accurately, and changes in their attitude toward their appearance. These alterations may be related to neurodegenerative processes in the brain as well as cognitive decline, where patients lose the ability to accurately perceive the world around them and their place in it. Research indicates that shifts in how people see their bodies can have an impact on their emotional and psychological well-being, which makes them a crucial component of a thorough dementia diagnosis and treatment plan [10,12,13,14].Therefore, a significant and little-studied factor that may help with dementia diagnosis and therapy is the relationship between physical characteristics like body mass and alterations in body perception in dementia patients. Future studies in this field will contribute to a greater understanding of the cognitive and physiological processes that underlie dementia. They may also help create new therapeutic approaches that will reduce the disease's course and improve patients' quality of life.To find potential markers for early diagnosis and disease progression monitoring, the study will investigate the association between body mass, body image evaluation, MMSE, and CDR scores in patients with pre-dementia.
2. Method and Materials of the Study
- Methodology: This study is a prospective observational research aimed at examining changes in body mass and its relationship with dementia in patients undergoing treatment and monitoring over a period of 90 days. The study employed clinical observation, questionnaires, and instrumental diagnostics. Participants' body mass was measured at three visits - at the first (Visit 1), second (after 30 days), and third (after 90 days) visits. Standard scales with an accuracy of 0.1 kg were used for body mass measurement. Dementia was diagnosed using standardized tests such as the MMSE (Mini-Mental State Examination) and CDR (Clinical Dementia Rating) scales, which allowed for assessing cognitive functions and the degree of dementia in participants. Additionally, the GDS (Geriatric Depression Scale) was used to assess the psychological and emotional state of participants.MMSE (Mini-Mental State Examination) is a widely used tool to assess cognitive impairment in patients with dementia. It comprises 30 questions that assess many facets of cognitive function, such as language, memory, attention, time and place orientation, and the capacity to carry out productive tasks. The MMSE score ranges from 0 to 30, with a score of 30 indicating no cognitive impairment, while lower scores indicate varying degrees of cognitive dysfunction. The interpretation of the MMSE score is as follows: 24-30 points - normal cognitive function, 18-23 points - mild cognitive impairment, 0-17 points - severe cognitive impairment.CDR (Clinical Dementia Rating) is used to assess the severity of dementia based on clinical manifestations. The scale includes 5 categories: personal care, communal affairs, memory, orientation, and judgment and problem solving. Five-point ratings are used for each category: 0 indicates no impairment, 0.5 indicates dubious impairment, 1 indicates mild impairment, 2 indicates significant impairment, and 3 indicates severe impairment. The CDR scale's results yield an overall score that divides patients into the following groups:- CDR 0 - no dementia (normal state),- CDR 0.5 - pre-dementia (mild cognitive impairment),- CDR 1 - mild dementia,- CDR 2 - moderate dementia,- CDR 3 - severe dementia.Statistical analysis of the data included calculating the average body mass, standard deviations, and assessing the dynamics of changes over the 90-day period. Specialized software was used to process the data.Materials of the Study: The study included 20 participants with dementia who consented to participate and completed all three visits. The average age of the participants was 62.3±1.07 years, with an age range of 60 to 85 years. Among the participants, 8 were men and 12 were women. Participants' body mass was measured using digital scales. Cognitive functions were assessed using the MMSE scale, and the degree of dementia was assessed using the CDR scale. In addition to body mass data, coexisting conditions such as hypertension and diabetes were taken into account, as well as therapeutic interventions that could affect the study results.
3. Results and Discussion of Own Research
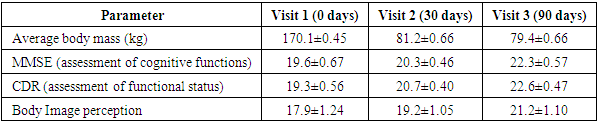
- During the conducted study, changes in body weight, cognitive functions, and body image perception were recorded in patients with dementia over a 90-day observation period. Data were collected at three visits: at the baseline (first visit), after 30 days (second visit), and after 90 days (third visit). The results show interesting and important changes that may be associated with both the progression of the disease and other physiological processes.Body Weight:At the first visit, when the observation process began, the average body weight of the participants was 170.1±0.45 kg. This figure reflects the initial physical condition of the participants, which could have been influenced by various factors, such as lifestyle, diet, physical activity, and the presence of comorbid conditions such as hypertension, diabetes, and other chronic disorders. Given that most participants suffered from dementia, it is also important to note that age-related metabolic changes, reduced physical activity, and cognitive impairments can affect their initial physical state.
|
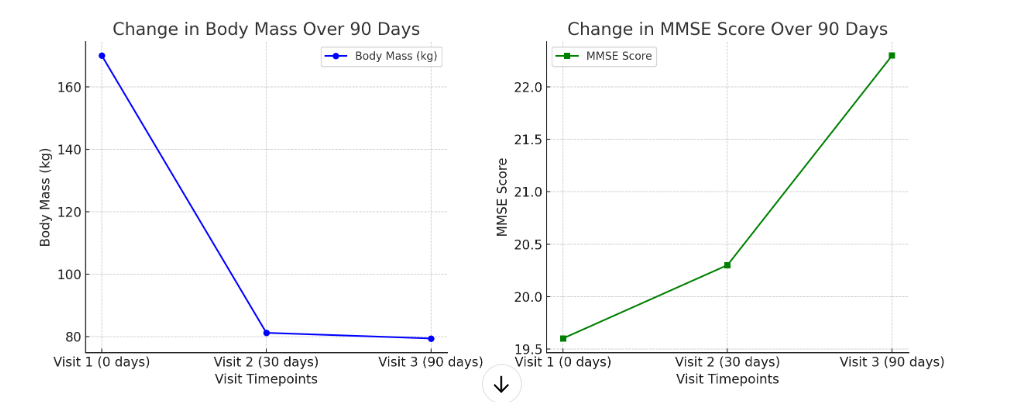 | Figure 1 |
4. Conclusions
- The study's findings show that, in spite of the weight loss seen in dementia patients, cognitive function as assessed by the MMSE scale, did not significantly deteriorate and even showed a trend toward improvement over the 90-day observation period. This suggests that, while physical changes such as weight loss can occur in patients with dementia, these changes do not always correlate directly with a decline in cognitive abilities. In fact, the improvement observed in the MMSE scores could indicate a temporary stabilization or slight recovery of cognitive functions, possibly due to therapeutic interventions or other factors such as psychological adaptation or changes in disease progression.In parallel with the cognitive function assessment, improvements in functional abilities were observed, as indicated by the CDR scale scores. The positive changes in functional capacity are particularly important as they reflect the patient's ability to perform daily activities, which is a critical aspect of dementia care. The improvement in functional abilities suggests that despite the physical decline observed through weight loss, there may be other factors - such as targeted therapies, supportive care, or even a period of adaptation - that can help maintain or even improve functionality in dementia patients. This highlights the importance of a comprehensive approach to dementia care that focuses not only on cognitive decline but also on maintaining and enhancing daily living skills.Moreover, it is crucial to recognize that weight loss, despite its generally negative trend, is not always a clear-cut indicator of deterioration in the patient’s condition. In dementia, weight loss can occur due to various reasons, including changes in appetite, metabolism, or the inability to recognize hunger. However, its effects on cognitive function may be more multifaceted than initially assumed. The relationship between weight loss and cognitive decline is complex and may not always be linear, suggesting that further research is needed to explore these connections in more depth.The results of this study also emphasize the intricate relationship between physical health, cognitive functions, and body image perception in dementia patients. The observed improvements in body image perception, as measured by the Image evaluation scale, reflect the patients' emotional and psychological adaptation to their physical changes. These findings suggest that patients with dementia may, over time, adjust to the changes in their physical state and come to a more positive or stable perception of their bodies, even in the face of cognitive and physical decline. Future research must examine these aspects more thoroughly in order to better understand the underlying mechanisms and offer a more comprehensive approach to dementia care, as evidenced by the intricate relationship between physical health, cognition, and body image.In conclusion, while weight loss and cognitive decline are common in patients with dementia, the study suggests that the relationship between these factors is not always straightforward. The improvements in cognitive function, functional abilities, and body image perception observed during the study point to the possibility of partial compensation or stabilization, even in the context of physical decline. This reinforces the importance of tailored therapeutic strategies and comprehensive care that address not only cognitive and physical health but also the emotional and psychological well-being of dementia patients. Further research is essential to fully understand these complex processes and to refine care models that optimize outcomes for individuals with dementia.
5. Findings
- The study's conclusions show that while dementia patients experienced a significant decrease in weight during the 90-day observation period, cognitive function as assessed by the MMSE scale, did not deteriorate significantly. In fact, a slight trend toward improvement in cognitive abilities was observed. This suggests that the relationship between weight loss and cognitive decline in dementia is not straightforward. Furthermore, functional abilities as measured by the CDR scale increased throughout the trial, emphasizing how crucial it is to preserve patients' capacity to carry out everyday tasks. Additionally, improvements in body image perception, as evaluated by the Image evaluation scale, were recorded, indicating that dementia patients can experience positive psychological and emotional changes, even in the context of cognitive and physical decline.These results emphasize the complexity of dementia, where physical decline, such as weight loss, may not necessarily correlate with worsening cognitive functions. The study also suggests that functional abilities and body image perceptions can improve or stabilize with appropriate care, despite cognitive or physical challenges. This complexity necessitates a more integrated and multifaceted approach to dementia care.
6. Practical Recommendations
- 1. Comprehensive Care Approach: Based on the findings, a holistic care approach should be adopted for dementia patients. It is essential to regularly assess cognitive functions, physical health, and psychological well-being. A comprehensive care plan that addresses these areas will be more effective in managing dementia and improving patients' quality of life.2. Addressing Weight Loss: Although weight loss is often seen as a sign of physical decline, it should not automatically be interpreted as a negative indicator of cognitive function deterioration. Healthcare professionals should investigate the underlying causes of weight loss, such as changes in appetite, difficulty in eating, or metabolic alterations. Tailored interventions, including nutritional support, should be implemented to manage weight and prevent further complications.3. Support for Emotional and Psychological Health: Considering the positive changes in body image perception observed in this study, it is crucial to address the emotional and psychological needs of dementia patients. Offering psychological counseling, emotional support, and therapies designed to enhance body image perception can significantly improve patients' self-esteem and overall mental health, which are key to their well-being.4. Multidisciplinary Team Approach: Healthcare professionals must work together across disciplines due to the complexity of dementia care. A multidisciplinary team comprising doctors, psychologists, occupational therapists, and dietitians can offer a holistic approach to dementia care, attending to every facet of the patient's need.5. Continuous Monitoring and Long-Term Care: Ongoing monitoring is critical for dementia patients, especially as cognitive, physical, and emotional changes can fluctuate over time. Regular follow-ups and assessments allow healthcare providers to adjust care plans as needed, ensuring that early signs of decline are addressed promptly. This proactive approach can significantly enhance the patient's quality of life.Future Research Directions:The results of this study underline the need for further research to better understand the complex relationship between cognitive decline, physical health, and emotional well-being in dementia. Future studies should focus on identifying the underlying mechanisms that lead to improvements in body image perception, functional abilities, and cognitive function. Additionally, investigating the role of weight loss and its impact on dementia progression will be crucial in developing targeted interventions to prevent or mitigate its effects.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML