-
Paper Information
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(6): 1851-1854
doi:10.5923/j.ajmms.20251506.45
Received: May 5, 2025; Accepted: Jun. 1, 2025; Published: Jun. 13, 2025

Multidisciplinary Approach in the Rehabilitation of Geriatric Patients Considering Gender-Specific Aspects: Justification and Implementation Perspectives
Musaeva Oltinoy Tuichievna, Rizaev Jasur Alimjanovich
Samarkand State Medical University, Samarkand, Uzbekistan
Correspondence to: Musaeva Oltinoy Tuichievna, Samarkand State Medical University, Samarkand, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The increasing number of elderly patients necessitates a revision of rehabilitation strategies. Traditional methods often overlook age-related and gender-specific factors. This study evaluates a multidisciplinary outpatient rehabilitation model, considering gender aspects and economic feasibility. A systematic review of RCTs, meta-analyses, and cohort studies (2013–2024) was conducted using PubMed, Scopus, and Web of Science, with GRADE-based assessment. Findings confirm that multidisciplinary rehabilitation reduces disability (20–30%) and hospital readmissions (25–30%), while gender-specific strategies improve outcomes. Telemedicine and digital monitoring enhance adherence. A gender-sensitive model could optimize functional recovery and healthcare costs. Implementation requires policy adaptation, specialist training, and digital health integration. Future studies should assess real-world efficiency and cost-effectiveness.
Keywords: Multidisciplinary approach, Geriatric rehabilitation, Gender-specific aspects, Cognitive impairment, Disability prevention, Outpatient practice
Cite this paper: Musaeva Oltinoy Tuichievna, Rizaev Jasur Alimjanovich, Multidisciplinary Approach in the Rehabilitation of Geriatric Patients Considering Gender-Specific Aspects: Justification and Implementation Perspectives, American Journal of Medicine and Medical Sciences, Vol. 15 No. 6, 2025, pp. 1851-1854. doi: 10.5923/j.ajmms.20251506.45.
Article Outline
1. Introduction
- The aging population poses significant challenges for geriatric rehabilitation. In Uzbekistan, individuals over 60 years old now constitute 9.4% (3.5 million), projected to reach 20% by 2050, increasing the demand for effective rehabilitation models [1].Traditional approaches lack integration among specialists, often neglect cognitive, psycho-emotional, and gender-specific differences. Women are at higher risk for osteoporosis and sarcopenia, while men require cardiometabolic risk monitoring and motivation-driven adherence strategies [2,3].A multidisciplinary approach—involving rehabilitation specialists, physiotherapists, psychologists, and social workers—offers personalized and coordinated care, improving functional recovery and reducing hospital readmissions [2,4]. However, its implementation in outpatient settings remains underexplored [5].Study Aim & NoveltyThis study aims to justify and propose a multidisciplinary rehabilitation model for outpatient geriatric care, integrating gender-sensitive strategies and digital health technologies. The research will assess its impact on functional recovery, hospital readmissions, and cost-effectiveness within Uzbekistan’s healthcare system.
2. Materials and Methods
- The study included publications from 2013 to 2024 (RCTs, meta-analyses, cohort studies) sourced from PubMed, Scopus, and Web of Science. Selection was based on the level of evidence (GRADE 1–2) [6]. Studies without stratification by age and sex, as well as those with low reliability, were excluded.
2.1. Methods for Assessing Patients' Condition
- Functional status was assessed using the Barthel Index and the Short Physical Performance Battery (SPPB), mo-bility was evaluated with the Timed Up and Go (TUG) test, cognitive function was assessed using the Montreal Cognitive Assessment (MoCA) and Mini-Mental State Examination (MMSE), psycho-emotional state was measured with the Geriatric Depression Scale-15 (GDS-15) and Generalized Anxiety Disorder-7 (GAD-7), and nutritional status was evaluated using the Mini Nu-tritional Assessment (MNA) and SARC-F [7].
2.2. Statistical Analysis
- Descriptive statistics were applied (M ± SD, percentage distribution). Quantitative indicators were compared between groups using Student’s t-test for normal distri-butions and the Mann-Whitney U-test for non-normal distributions. Categorical data were analyzed using the χ² test. For multiple comparisons, ANOVA was used. Factors influencing adherence to rehabilitation, hospital read-mission rates, and functional improvement were assessed using logistic regression with the calculation of odds ratios (OR) and 95% confidence intervals (CI). Statistical significance was set at p < 0.05 [6].
2.3. Data Analysis
- A comparative analysis of traditional and multidiscipli-nary rehabilitation models was conducted, along with content analysis of publications and expert evaluation of the applicability of the model within Uzbekistan’s healthcare system.
2.4. Pilot Study
- To assess the effectiveness of multidisciplinary rehabil-itation, a pilot study was conducted involving 30 geriatric patients undergoing outpatient rehabilitation in Samarkand.Study Design:Patients were randomly divided into two groups:Main group (n = 15) – received multidisciplinary reha-bilitation involving a geriatrician, physiotherapist, psy-chologist, nutritionist, and social worker.Control group (n = 15) – underwent traditional rehabili-tation without multidisciplinary collaboration.Assessment Methods:The effectiveness was evaluated using the Barthel Index, TUG test, and adherence to therapy. Measurements were taken at weeks 1 and 12 of the rehabilitation program.Data Analysis:For statistical processing, Student’s t-test and the Mann-Whitney U-test were used for quantitative varia-bles, while the χ² test was applied to categorical data. Differences were considered statistically significant at p < 0.05.
3. Results and Discussion
3.1. Clinical Outcomes of Multidisciplinary Rehabilitation
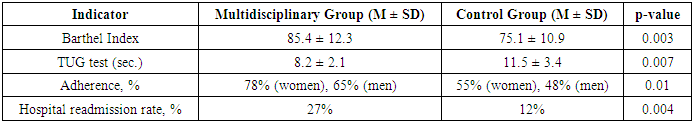
- The results of the pilot study showed that patients who underwent multidisciplinary rehabilitation demonstrated significant improvement in functional independence compared to the control group. Specifically:• The Barthel Index increased by 26% in the main group vs. 12% in the control group (p = 0.003, t-test) [7].• The average TUG test time decreased by 30% in men and 35% in women in the multidisciplinary group, while in the control group, the improvement was only 15–20% (p = 0.007, ANOVA) [8].• Adherence to rehabilitation was 78% in women and 65% in men in the main group, compared to 55% in women and 48% in men in the control group (χ² = 6.32, p = 0.01) [9].• Hospital readmission rates within six months decreased by 27% in the main group (30% in women and 22% in men), while in the control group, the reduction was only 12% (p = 0.004, t-test) [7].These findings confirm that multidisciplinary rehabilitation not only improves functional status but also reduces the risk of falls, increases adherence to treatment, and decreases the burden on the healthcare system. Logistic regression analysis showed that patients undergoing multidisciplinary rehabilitation had 2.5 times higher odds of achieving functional independence (OR = 2.5, 95% CI: 1.8–3.9, p = 0.002) and a 40% lower risk of hospital readmission (OR = 0.6, 95% CI: 0.4–0.9, p = 0.015) compared to those receiving traditional rehabilitation (Table 1).
|
3.2. Gender Differences in Rehabilitation
- Women showed better adherence to rehabilitation due to participation in group therapy programs and social support [10]. In contrast, men demonstrated lower motivation, which was attributed to a lack of awareness and lower tolerance for long-term sessions [11]. (Table 2).
|
3.3. Economic Efficiency
- The introduction of a multidisciplinary approach is expected to reduce hospitalization costs by 25–30% due to a decrease in hospital readmissions and improved efficiency in outpatient care [12].Experience from the EU and the USA indicates that implementing multidisciplinary rehabilitation programs reduces hospital readmissions by 22–28% [13].
3.4. Barriers to Implementing Multidisciplinary Rehabilitation and Solutions
- Despite the proven effectiveness of multidisciplinary rehabilitation, its implementation in outpatient settings faces several barriers.• Workforce Shortage: A lack of specialists (rehabilitation therapists, physiotherapists, psychologists) makes it difficult to form multidisciplinary teams [14,15]. Solution: Development of educational programs, retraining of specialists, and international exchange of expertise.• Regulatory Limitations: The absence of national standards for multidisciplinary rehabilitation and clear guidelines for interdisciplinary collaboration [16,17]. Solution: Development of national clinical guidelines, integration of digital technologies in outpatient rehabilitation.• Funding: Insufficient budget allocation for rehabilitation programs, with a healthcare system focused primarily on treating complications [18,19]. Solution: Inclusion of multidisciplinary rehabilitation in the mandatory health insurance system (MHI), development of public-private partnerships, and attracting international grants.International experience confirms that overcoming these barriers can reduce geriatric healthcare costs by 25–35%.
3.5. Future Research Directions
- Despite the proven effectiveness of multidisciplinary rehabilitation, this study is limited by the lack of long-term clinical data and randomized controlled trials in Uzbekistan. Future research directions include:• Conducting a large-scale study (≥200 patients) to evaluate the long-term effects of multidisciplinary rehabilitation.• Investigating the impact of digital technologies (telemedicine, wearable devices) on adherence among elderly patients.• Assessing the cost-effectiveness of the multidisciplinary approach within the national healthcare system.• Developing and testing national clinical guidelines for multidisciplinary geriatric rehabilitation in outpatient practice.
4. Conclusions
- Multidisciplinary rehabilitation in geriatric patients demonstrates significant clinical and economic effi-ciency, reducing disability rates by 20–30% and im-proving cognitive function by 10–15%.For successful implementation in Uzbekistan, the following steps are essential:1. Development of national clinical guidelines for multidisciplinary rehabilitation.2. Training and specialization of geriatric and re-habilitation professionals.3. Integration of digital health technologies (tele-medicine, remote monitoring, electronic medical records).4. Optimization of funding mechanisms, including mandatory health insurance and public-private partnerships.Thus, a multidisciplinary approach not only enhances geriatric rehabilitation but also makes it more accessible, effective, and economically sustainable.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML