-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(6): 1839-1843
doi:10.5923/j.ajmms.20251506.43
Received: May 5, 2025; Accepted: Jun. 3, 2025; Published: Jun. 13, 2025

Clinical and Diagnostic Features of Complicated Chronic Purulent Middle Otitis Media
Khatamov Jhakhongir Abruevich
Samarkand State Medical University, Uzbekistan
Correspondence to: Khatamov Jhakhongir Abruevich, Samarkand State Medical University, Uzbekistan.
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The development of local and intracranial complications in chronic purulent middle otitis media (CPMSO), including fatal cases, necessitates a comprehensive analysis of their occurrence patterns, as well as the development of effective approaches to diagnosis and treatment. We examined 124 CGSA patients with various complications who had been hospitalized for the last 20 years and received complex treatment. The aim of the study is to analyze some indices of endogenous intoxication, to analyze microbial flora of different parts of the middle ear, to assess the sensitivity of these microorganisms to various antibiotics and to identify the degree of hearing loss in CGSA with complications. Infectious processes caused by bacterial agents can lead to an increase in the concentration of fibrinogen in plasma, worsening the rheological properties of blood, disrupting microcirculation and limiting the oxygenation of tissues and organs, which may play a significant role in the pathogenesis of complications of CHSO. At anilysis of blood there is a shift of leukocytic formula to the left, as well as an increase in erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) level. Increased indices of lipid peroxidation products (LPO) and metabolites of endogenous intoxication, which leads to damage to cellular and subcellular structures that in almost all cases to some extent affects auditory perception. Staphylococcus aureus was detected in 63.8% of patients by microbiologic examination. Among them, Staphylococcus aureus was detected in 29.2%, epidermal Staphylococcus aureus in 31.9%, and saprophytic Staphylococcus aureus in 2.7%. Gram-negative flora from the external auditory canal was isolated only in associations of microorganisms (24.9%). Pseudomonas aeruginosa was found in 15.8% of patients and Klebsiella oxytoca in 9.1%. In microbial associations, yeast and mold fungi of the genus Aspergillus spp., Candida spp. and Mucor spp. were detected. Obligate-anaerobic microorganisms were less common, with Peptostreptococcus spp. predominating among them. The combined application of hyperbaric oxygenation with antioxidants and plasmapheresis improves blood biochemical parameters and audiologic characteristics, which can be the basis for further improvement of treatment tactics.
Keywords: Chronic purulent otitis media, Otogenic complications, HBO, Plasmapheresis
Cite this paper: Khatamov Jhakhongir Abruevich, Clinical and Diagnostic Features of Complicated Chronic Purulent Middle Otitis Media, American Journal of Medicine and Medical Sciences, Vol. 15 No. 6, 2025, pp. 1839-1843. doi: 10.5923/j.ajmms.20251506.43.
1. Relevance
- Nowadays, early diagnosis and effective treatment of chronic purulent otitis media and its complications occupy a special place in otorhinolaryngologic practice. The development of local and intracranial complications, including fatal cases, necessitates a comprehensive analysis of the patterns of their occurrence, as well as the development of effective approaches to diagnosis and treatment [2,3,9,10,11,16,17,19,20].Microorganisms, including streptococci, staphylococci, pneumococci, anaerobic bacteria, fungal pathogens and other opportunistic microorganisms, have a significant impact on the development of chronic purulent otitis media with complications. Microbiologic examination of middle ear contents, liquor and purulent foci in the cranial cavity often reveals the presence of mixed microflora [1,7,14,22].Infectious processes caused by viral or bacterial agents can contribute to an increase in plasma fibrinogen concentration, which leads to the development of hypercoagulability, deterioration of blood rheological properties, impairing microcirculation and limiting tissue and organ oxygenation, which can play a significant role in the pathogenesis of complications of CCHO [2,4,5,8,19].As a result of the inflammatory process, there is an increase in endogenous intoxication, an increase in body temperature above 38°C, tachycardia and tachypnea, a leftward shift of the leukocytic formula, and an increase in erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) levels [1,7,12,13,18,20]. Inflammatory processes in the body are caused by damage to cellular and subcellular structures, arising under the influence of lipid peroxidation products (LPO) and metabolites of endogenous intoxication. Disturbance of physiological equilibrium associated with changes in the optimal concentration of these compounds can lead to the development of pathological processes [2].Changes in the rheological properties of blood, hypoxemia and metabolic acidosis play a key role in the pathogenesis of inner ear lesions. Disruption of metabolic processes first leads to a decrease in functional activity, and then to degeneration and death of hair cells, which is the cause of sensorineural hearing loss [3,6,8]. The frequency of inner ear lesions and hearing impairment in CGSA varies from 40 to 80% of cases. Some patients with CGSA with complications are not always able to determine the degree of hearing impairment due to the severe condition and confused consciousness of patients on admission to the clinic [6,12].To reduce the effects of endogenous intoxication syndrome, improve the rheological properties of blood and restore immune defense in inflammatory diseases an effective method is plasmapheresis (PA). Replacement of the removed plasma with donor plasma contributes to the restoration of the body's defense mechanisms, accelerates the healing process and promotes the restoration of homeostasis [5,15,21].Hyperbaric oxygenation (HBO) is effective for stimulation of tissue metabolism in purulent-inflammatory processes by increasing the partial pressure of oxygen and contributes to the reduction of intracranial hypertension, normalization of body temperature and acceleration of surgical wound healing. In this regard, HBO is successfully used in the treatment of chronic purulent-inflammatory processes of the middle ear [3,4,8,13].However, in the available literature there are no substantiated data on the combined use of HBO with antioxidants in combination with plasmapheresis in various clinical variants of CPSO with complications. The aim of our work was to evaluate the effectiveness of complex treatment of chronic purulent otitis media with complications.
2. Material and Methods
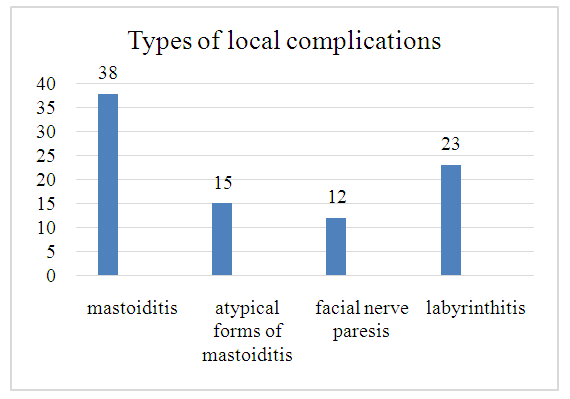
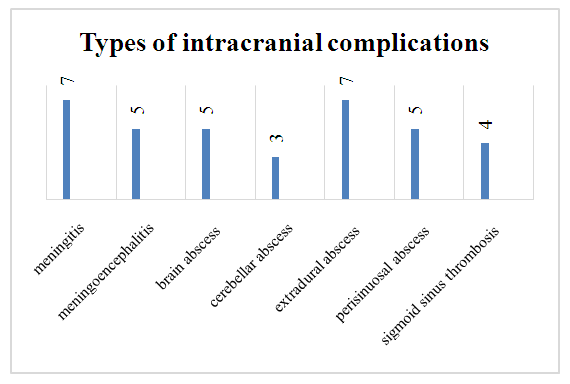
- 124 patients with CGSO with complications who received inpatient treatment in the last 20 years in ENT departments of Samarkand city hospitals were included in the study. Men were 68 (54,8%) and women 56 (45,2%) among the examined patients with CHSO complications. Age of examined patients from 18 to 40 years - 72, from 40 to 60 years - 36 and over 60 years - 16 patients.The study revealed that chronic purulent middle otitis media, epitympanitis was diagnosed in 81 (65,3%) patients, mesotympanitis in 19 (15,3%) and epimesotympanitis in 24 (19,4%) patients. According to the history, the duration of the disease ranged from 3 years to 30 years. The detected complications among the examined patients were local in 88 (73.0%) patients and intracranial in 36 (27.0%) patients. All patients were consulted by an otorhinolaryngologist, neurologist, neuropathologist, neurosurgeon, ophthalmologist, infectious disease specialist, therapist, clinical and laboratory tests, RheoEG, CT and MRI of the mastoid process and brain were performed.Mastoiditis was diagnosed in 38 patients, 15 with atypical forms of mastoiditis, 12 with facial nerve paresis, and 23 with labyrinthitis. Figure 1
 | Figure 1 |
 | Figure 2 |
 | Figure 3 |
3. Results and Discussion
- We conducted a comparative analysis of the dynamics of treatment of patients of groups I and II who were prescribed traditional and modified therapy using HBO with antioxidants in combination with plasmapheresis. After traditional therapy, a decrease in the concentration of MDA and DK, as well as an increase in AOA, was observed only by day 18 of therapy in patients of group I, reaching values of 6.12 ± 0.42 μmol/L, 3.23 ± 0.21 μmol/L and 34.6 ± 1.3, respectively. However, the level of MDA and other indicators did not reach the control. The length of stay of patients in the hospital was 18 ± 2.8 bed-days (p <0.05), and there was a positive dynamics of the inflammatory process. A positive effect was noted in 40.4% of patients, which was manifested in an improvement in speech perception and a decrease in tonal hearing thresholds to 15 dB. All patients showed a slight improvement in blood circulation in the vessels of the brain and pathological changes began to decrease during the RheoEG examination.After complex treatment using HBOT in combination with antioxidant therapy and plasmapheresis in patients of group II, it was possible to reduce the intensity of free radical oxidation processes and restore the functional state of the antioxidant system. The MDA content decreased after correction from 7.86 ± 0.22 to 4.98 ± 0.43 mmol/l, the DC decreased from 4.79 ± 0.09 to 2.48 ± 0.12, and the AOA index increased from 23.9 ± 2.0-3 to 35.9 ± 1.2. The duration of hospitalization of patients was 14.6 ± 1.8 bed-days. The perception of sounds and speech intelligibility in 59.6% of patients showed a decrease in the hearing threshold to 25 dB at high frequencies. The CRP content decreased to 5.7 mg/l in the first group and to 6.9 mg/l in the second group. This significant decrease compared to the initial indicators indicates the regression of the inflammatory process.The leukocyte count decreased to 7.5×10⁹/L in the first group and 8.5×10⁹/L in the second group, which confirms the weakening of the inflammatory response. The ESR (erythrocyte sedimentation rate) decreased to 9.9 mm/h and 11.5 mm/h in the first and second groups, respectively, indicating an improvement in hematological parameters and a reduction in inflammatory activity. The fibrinogen level decreased to 3.3 g/L in the first group and 3.8 g/L in the second group, indicating the restoration of normal blood clotting. The prothrombin index (PTI) also decreased, amounting to 94.1 sec in the first group and 97.8 sec in the second group, reflecting the normalization of the blood’s rheological properties. After performing a series of diagnostic and emergency therapeutic interventions, the patients showed positive dynamics: the headaches, dizziness, nausea, and vomiting decreased, and the body temperature returned to physiological norms. General brain and meningeal symptoms gradually regressed. In patients with meningitis, cerebrospinal fluid pressure gradually decreased, approaching normal values. The use of this method significantly accelerated the process of epithelialization of the trepanation cavity, which contributed to a reduction in the duration of postoperative rehabilitation for the patients.
4. Conclusions
- Thus, early hospitalization of patients at the onset of the disease, comprehensive preoperative preparation, emergency surgical intervention, postoperative intensive therapy with the use of hyperbaric oxygenation (HBO) and antioxidants combined with plasmapheresis, as well as continuous monitoring of vital functions, contribute to achieving positive clinical outcomes. In group I, 40.4% of patients showed a positive effect, with improved speech perception and a decrease in tonal hearing thresholds to 15 dB. Biochemical parameters normalized by the 18±2.8th day of the patients' stay in the hospital. In group II, 59.6% of patients showed improved hearing on speech testing. A decrease in hearing thresholds from 10 to 25 dB at high frequencies was noted. By the 14.6±1.8th day of hospitalization, the biochemical parameters of the patients returned to normal values. The results obtained confirm the effectiveness of the selected comprehensive diagnostic and therapeutic approaches and can serve as a basis for further optimization of treatment strategies.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML