-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(4): 1090-1093
doi:10.5923/j.ajmms.20251504.48
Received: Feb. 17, 2025; Accepted: Mar. 12, 2025; Published: Apr. 16, 2025

Correlation Between Vitamin D Levels and Non-developing Pregnancy in the Epidemiological Setting
Xusain Xamroqulovich Buriyev1, Lagiya Mirzatillayevna Abdullayeva2
1Resercher, Ministry of Health, Department for the Protection of Motherhood and Childhood, Tashkent, Uzbekistan
2Doctor of Medical Sciences, Professor of the Department of Obstetrics and Gynecology, Tashkent Medical Academy, Tashkent, Uzbekistan
Correspondence to: Lagiya Mirzatillayevna Abdullayeva, Doctor of Medical Sciences, Professor of the Department of Obstetrics and Gynecology, Tashkent Medical Academy, Tashkent, Uzbekistan.
| Email: |  |
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Non-developing pregnancy is currently one of the most important issues in practical obstetrics and gynecology. The aim of the study was to investigate the correlation between vitamin D levels and non-developing pregnancy. The results showed that women with non-developing pregnancy had higher instances of vitamin D deficiency and insufficiency. In the comparison group, a statistically significant increase in 25-hydroxyvitamin D levels was observed, and a concentration of 25-hydroxyvitamin D in the blood serum higher than 27,5 ng/ml was associated with a reduced risk of non-developing pregnancy. In conclusion, the use of vitamin D during pre-gravid preparation in women under epidemiological adverse conditions has a positive effect on the progression of pregnancy and childbirth.
Keywords: Non-developing pregnancy, Vitamin D, 25-hydroxyvitamin D, Reproductive losses, COVID-19
Cite this paper: Xusain Xamroqulovich Buriyev, Lagiya Mirzatillayevna Abdullayeva, Correlation Between Vitamin D Levels and Non-developing Pregnancy in the Epidemiological Setting, American Journal of Medicine and Medical Sciences, Vol. 15 No. 4, 2025, pp. 1090-1093. doi: 10.5923/j.ajmms.20251504.48.
1. Introduction
- Pregnancy losses up to the 12th week of gestation (non-developing pregnancy, spontaneous abortion) account for 80% of all early reproductive losses [1,2]. Non-developing pregnancy, especially in an epidemiologically adverse situation, is considered to be related to disturbances in vitamin D status, similar to other pathologies during the gestational period [3,4]. In women with non-developing pregnancy, a decrease in the levels of vitamin D in the blood serum has been observed, and these indicators may be considered as markers of non-developing pregnancy. Vitamin D is essential for maintaining the level and activity of interferon-dependent proteins in immune defense, reducing the effects of the "cytokine storm," and compensating for comorbid pathologies [5,6].Vitamin D is equally important for the fetus, especially during the early stages of its development [7,8]. Currently, there is increasing evidence regarding the pleiotropic effects of vitamin D, particularly its impact on pregnant women and the developing fetus. It has been established that adequate levels of vitamin D are essential from the stages of implantation and placenta formation throughout the entire pregnancy. Vitamin D plays a crucial role in the proper functioning of the “mother-placenta-fetus” system and positively influences the processes of embryogenesis, as well as the intra- and postnatal periods [9,10]. Recent research has demonstrated the effects of calciferols on the embryo’s genetics. A deficiency of these substances in the body increases the risk of failure during the process of reading genetic information and forming new cells [11]. WHO experts have identified vitamin D deficiency and insufficiency as a new pandemic of the 21st century. Further research is required to clarify the mechanism by which vitamin D deficiency contributes to the development of pregnancy complications. Identifying risk factors associated with the increase in non-developing pregnancy among early reproductive losses and subsequent adverse outcomes is an urgent public health issue [12,13].Aim of the study: The aim of the study was to investigate the levels of vitamin D in women with non-developing pregnancy.
2. Materials and Methods
- Based on the objectives and tasks of the study, 100 women with non-developing pregnancy (NDP) and 30 women with physiologically progressing pregnancy were studied and divided into three groups:1. Main group – 50 women with NDP up to the 13th week of gestation (those who developed NDP after having had COVID-19).2. Comparison group – 50 women with NDP up to the 13th week of gestation, who had no history of COVID-19 infection.3. Control group – 30 women with physiologically progressing pregnancy.The three groups of women did not show significant differences in clinical indicators. The age of women with non-developing pregnancy ranged from 18 to 40 years in all groups. The average age of the groups did not differ significantly (P>0,05). The average age of women in the main and comparison groups was 25,7±0,7 years, while in the control group it was 26,2±0,8 years.Our study aimed to investigate the epidemiological characteristics of non-developing pregnancy (NDP) up to the 13th week of gestation in 50 women who had developed NDP after having had COVID-19. The time interval between COVID-19 infection and the diagnosis of NDP was examined. Among the 50 women included in the study, 32 (64%) had COVID-19 during the early stages of pregnancy, specifically between 4 and 8 weeks of gestation.The assessment of vitamin D levels in pregnant women was based on the following parameters: serum 25(OH)D levels of ≤20 ng/ml were classified as “deficiency,” levels between 21 and 29 ng/ml were considered “insufficiency,” and levels ≥30 ng/ml were regarded as “sufficient.”Chemiluminescent analysis was used to determine serum 25-hydroxycalciferol (25(OH)D) levels. Venous blood samples were collected using standard procedures. Serum was separated by centrifugation. To measure 25-hydroxycalciferol concentrations in the serum, a chemiluminescent method was applied using reagent kits and calibrators from Roche Diagnostics (Germany).Primary data were statistically processed using the “Statistic 10” software in the “Microsoft Excel 2010” database. Fisher’s χ² test was applied for the comparison of discrete variables. Linear regression and correlation analysis methods (Pearson and Spearman correlation coefficients) were used to assess relationships between quantitative indicators. Linear and multivariate regression analysis was applied to identify multiple variables. Differences and correlations were considered statistically significant at p<0,05. The significance of differences between groups, as well as the reliability of distribution differences in the studied indicators, was evaluated using Fisher’s exact test (two-tailed variant).
3. Results and Discussion
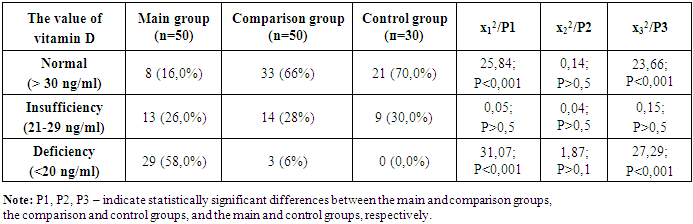
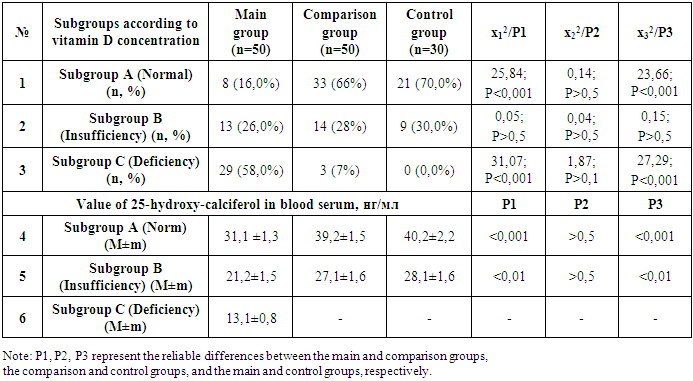
- The study revealed the following findings: In the main group, which included women with a history of COVID-19 and non-developing pregnancy (NDP), vitamin D levels were within the normal range in 16% of cases, insufficient in 26%, and deficient in 58%. In the comparison group, vitamin D levels were normal in 66% of cases, insufficient in 28%, and deficient in 7%. In the control group, consisting of women with physiologically progressing pregnancies, vitamin D levels were normal in 70% of cases and insufficient in 30%, while no cases of vitamin D deficiency were observed in this group (Table 1).
|
|
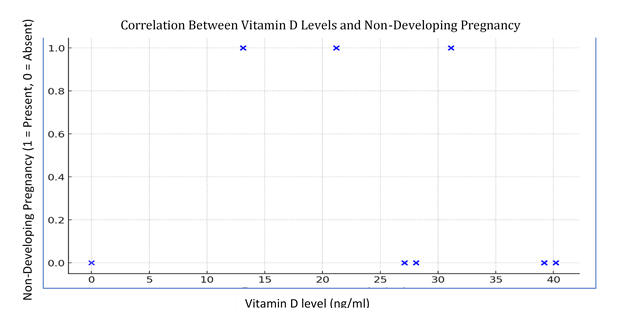 | Figure 1. Correlation between Vitamin D levels and non-developing pregnancy |
4. Conclusions
- The conducted study demonstrated that the incidence of vitamin D deficiency and insufficiency among women in the main group was 3,2 times higher compared to the comparison group. In the comparison group, a statistically significant increase in serum 25-hydroxyvitamin D levels was observed, and when the concentration of 25-hydroxyvitamin D in blood serum exceeded 27,5 ng/ml, the risk of non-developing pregnancy (ND) was significantly lower.According to our results, during epidemiologically unfavorable situations, the use of vitamin D during preconception preparation has a positive impact on the course of pregnancy and childbirth. In epidemiologically challenging times, particularly during the "COVID-19" pandemic, special attention should be given to vitamin D.Vitamin D deficiency can lead to metabolic diseases in pregnant women, complications of pregnancy, and the development of severe pathological changes. The analysis of the obtained results shows that in women who have had "COVID-19" and experienced non-developing pregnancy, as well as in women in the comparison group, somatic pathology is more common compared to the control group. Additionally, obstetric and gynecological histories are more complicated, suggesting that somatic and gynecological pathologies may negatively influence embryonic development.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML