-
Paper Information
- Next Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2025; 15(4): 1080-1084
doi:10.5923/j.ajmms.20251504.46
Received: Jan. 15, 2025; Accepted: Feb. 13, 2025; Published: Apr. 16, 2025

Correction of Neurological Manifestations of Post-Covid Syndrome by Micropolarization of the Brain in Employees of the Ministry of Internal Affairs
Zufar Adambaev1, Elbek Mirjuraev2, Dilrabo Iskandarova3
1Urgench Branch of the Tashkent Medical Academy, Urgench, Uzbekistan
2Center for the Development of Professional Qualifications of Medical Workers under the Ministry of Health of the Republic of Uzbekistan, Tashkent, Uzbekistan
3Sanatorium of the Medical Department of the Ministry of Internal Affairs of the Republic of Uzbekistan, Tashkent, Uzbekistan
Copyright © 2025 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

130 employees of the Ministry of Internal Affairs who had suffered a coronavirus infection with post-covid syndrome were examined. The average age was 37.7 ± 1.0 years. Patients with post-covid syndrome showed asthenic, cognitive, vegetative manifestations, sleep disorders, anxiety and depression in most cases in the form of mild disorders. Comprehensive rehabilitation of employees of the Ministry of Internal Affairs with post-covid syndrome in the form of drug therapy, as well as micropolarization of the brain, massages and exercise therapy contribute to the correction of clinical neurological manifestations of post-covid syndrome.
Keywords: Employees of the Ministry of Internal Affairs, Post-covid syndrome, Serotonin, Comprehensive rehabilitation, Micropolarization of the brain
Cite this paper: Zufar Adambaev, Elbek Mirjuraev, Dilrabo Iskandarova, Correction of Neurological Manifestations of Post-Covid Syndrome by Micropolarization of the Brain in Employees of the Ministry of Internal Affairs, American Journal of Medicine and Medical Sciences, Vol. 15 No. 4, 2025, pp. 1080-1084. doi: 10.5923/j.ajmms.20251504.46.
Article Outline
1. Introduction
- It should be noted that, despite the fact that several years have passed since the end of the coronavirus pandemic, post-COVID syndrome in the form of its neurological manifestations can still be detected in the population [1,2,7,12,13,15,21].The frequency of neurological complications of SARS-CoV-2 is currently unknown, but there is a tendency for patients with severe COVID-19 to have neurological symptoms more often than patients with a mild form [6,14,19].Neurological complications of long COVID are: fatigue, "brain fog", headache, sleep disturbances, cognitive and emotional impairment, dizziness, dysautonomia. In addition, complications of the peripheral nervous system include: muscle weakness, myalgia, anosmia (loss of smell), loss of taste (dysgeusia), hearing loss/tinnitus, sensorimotor deficits, decreased tactile sensitivity (hypoesthesia), malaise (dysesthesia), tremor [1,2,7,12,13,15,21].A meta-analysis of the results of 51 studies (n=18,917, followed for an average of 77 days after discharge) showed that the most prevailing symptoms were sleep disturbances - in 27.4% of patients, fatigue - in 24.4%, cognitive impairment - in 20.2%, anxiety - in 19.1%, depression - in 15.7% of patients. Another meta-analysis (19 studies of 11,324 patients) showed that 3 or more months after the onset of infection, the main symptoms of long COVID were: fatigue - in 37%, "brain fog" - in 32%, memory impairment - in 27%, attention impairment - in 22%, myalgia - in 18%, anosmia - in 12%, dysgeusia - in 11%, headache - in 10% of patients. Neuropsychiatric complications included sleep disturbances in 31%, anxiety in 23%, and depression in 12% [23,24].The interactions between the nervous system and the immune system are very complex and, depending on the context, can have a beneficial or detrimental effect on each other's performance [8,9]. Among neurotransmitters, serotonin plays an important role in the immune system through central and peripheral mechanisms. It should be noted that delirium, confusion, and sleep disturbances are associated with changes in the amount of 5-HT and melatonin (as a product of 5-HT). In addition, it has been shown that viral infections with subsequent cytokine storms can interfere with access to 5-HT and melatonin [11].Serotonin (5-hydroxytryptamine, 5-HT) is a biogenic amine and acts as a neurotransmitter in the nervous system. Another function of this molecule is that it acts as a hormone. In the brain, serotonergic neurons of the raphe nuclei are involved in the regulation of many forms of behavior, sleep processes, thermoregulation, etc. [11].Serotonin is a neurotransmitter involved in several physiological functions, such as mood, sleep, appetite, vomiting, pain perception, body temperature regulation, depression, anxiety, and migraine. Serotonin plays a role in the cardiovascular system, gastrointestinal tract (GIT), respiratory tract, nervous system, and platelets [11].Almost all immune cells express at least one component of the serotonergic system, and several immunomodulatory functions of the body are associated with 5-HT. For example, 5-HT in monocytes/macrophages modulates the secretion of immune mediators and cytokines such as TNF-α, interferon-γ, IL-1β, IL-6, IL-8 and related signaling pathways. In addition, stimulation of neutrophils and T cells by 5-HT may occur. Non-receptor mechanisms of the serotonergic system include the 5-HT transporter, tryptophan hydroxylase-1 and nuclear factor-κB (NF-κB) [22]. A group of researchers previously argued that tryptophan stores in the body of COVID-19 patients are depleted due to a decrease in ACE2, which plays a key role in the absorption of tryptophan from food. In this regard, tryptophan is a precursor for 5-HT synthesis, and its depletion therefore leads to a defect in the production of 5-HT, which is known as an important neuromodulator in olfactory neurons and taste buds, so that smell and taste senses can be lost in most patients with COVID-19 [3,4,22]. It is well known that the neurotransmitter serotonin determines the overall quality of life of a person, which was the basis for studying its concentration in the blood serum of patients with post-COVID syndrome [11,22].Service with employees of the internal affairs bodies is associated with high not only physical, but also psycho-emotional stress. It requires daily stress and dedication, special discipline, increased social and moral responsibility and, as a result, a high degree of risk of loss of health. The peculiarities of the daily work activities of employees, that is, irregular working hours, eating disorders, lack of sleep, frequently observed stressful situations at work, chronic fatigue caused by them, also negatively affect their health indicators. In such conditions, law enforcement officers are required to immediately respond to a variety of external, sometimes contradictory influences and high personal responsibility for decision-making [17].In addition to the above conditions, post-COVID syndrome, occurring with cognitive impairment in employees of the Ministry of Internal Affairs in the context of the current pandemic, are the leading reasons for the inability to perform their professional activities. Periodic rehabilitation of employees helps to prevent this [17].Consequently, passing the acute phase of COVID-19 does not mean a complete recovery. Immunity after coronavirus infection can be very weakened. In addition, almost all organs and systems are subject to overload during the disease. The result is a strong weakening of the body. The SARS-CoV-2 virus is capable of affecting many types of cells in the human body, which subsequently determines the type and severity of post-COVID complications, which deserves serious attention from the scientific and medical communities [10].The development of rehabilitation measures based on the patient's condition with its assessment of effectiveness in different departments of the Ministry of Internal Affairs of the Republic of Uzbekistan is extremely important in the study of clinical manifestations, mechanisms of occurrence, search for methods of treatment and rehabilitation of patients with post-covid syndrome. The variety of neurological symptoms dictates the need to develop comprehensive approaches to this problem. All of the above determined the purpose of this study.
2. Material and Research Methodology
- In the sanatorium of the Ministry of Internal Affairs, 130 employees of the Ministry of Internal Affairs were examined, including 118 men and 12 women who had suffered from coronavirus infection. The average age of the examined was 36.8 ± 0.6 years and the length of service was 9.2 ± 2.2 years.The severity of asthenia, cognitive impairment, vegetative manifestations, sleep disorders, anxiety and depression were determined. The concentration of serotonin in the blood serum.Asthenic manifestations were examined using the "Questionnaire for identifying asthenia", which contains 11 questions: the maximum score is 11, the higher the score, the higher the asthenia [20].We examined vegetative disorders using the "Questionnaire for identifying signs of vegetative changes", according to which vegetative disorders were detected when the score exceeded 15 points [20]. To study cognitive impairment (CI), the Mini-Mental State Examination (MMSE) was used. Interpretation according to this scale: 0-10 points – severe dementia, 11-19 points – moderate dementia, 20-23 points – mild dementia, 24-27 points – cognitive impairment, 28-30 points – no impairment of cognitive functions [20]. Anxiety and depression were studied according to the Anxiety and Depression Questionnaire, which contains 7 questions (for each section) with 4 answers (from 0 to 3 points) – from 0 to 21 points: the higher the score, the less anxiety and depression [20].Sleep disorders were studied using the Epworth Sleepiness Scale, which defines: 1-6 points – normal sleep, 7-8 points – moderate sleepiness, 9-24 points – abnormal (pathological) sleepiness [20].The concentration of serotonin in the blood serum was studied using high-performance liquid chromatography.To study the clinical picture of post-COVID syndrome in employees of the Ministry of Internal Affairs, we divided patients into three groups by type of service and age.Group 1 - 50 patients, the so-called "office workers" - whose work is indoors: operatives, teachers of the Academy of the Ministry of Internal Affairs, investigators, employees of the forensic department, passport office employees, personnel officers. The average age of this group of patients was 38.4 ± 1.0 years.Group 2 - 40 patients whose work is both indoors and outdoors. The average age of this group of patients was 37.7 ± 1.0 years.Group 3 - 40 patients whose work is outdoors: service in prisons and correctional colonies, patrol and guard service employees, National Guard employees, district inspectors, employees ensuring security in the metro. The average age of this group of patients was 33.8 ± 1.0 years. Thus, in terms of age composition, the youngest among the employees of the Ministry of Internal Affairs were in the third group and the oldest in the first group.To determine the effectiveness of the treatment we proposed, we divided our patients into 2 groups: the main group (MG) of 70 patients and the control group (CG) of 60 patients. Patients in the MG and CG received drug therapy: succinic acid preparations, brain metabolizers, stimulating antidepressants, sleeping pills - melatonin and B vitamins. In addition, patients received massage and exercise therapy. And patients in the MG, among other things, received micropolarization of the head in the frontal and occipital areas. The duration of one procedure is 30 minutes. The duration of the course of therapy is 10-12 days. Micropolarization is the effect of ultra-low electric current (up to 1 mA) on the brain, thereby causing a change in the level of polarization of neural and synaptic membranes, which is comparable to natural physiological processes. The mechanism of action of micropolarization is associated with the activating effect on the neurohumoral, axon-dendritic components of the brain and spinal cord, on the autonomic nervous system, there is a change in the level of membrane excitability of neurons, the synaptic apparatus, the sensitivity for the perception of ascending afferent flows increases. In other words, a new structure of interneuronal connections is formed in the damaged brain. Excessive, unnecessary connections disintegrate, and new ones are established in their place, more effective in physiological terms [18].The obtained data were statistically processed using Microsoft Excel 2013 (Microsoft, USA) and STATISTICA v.10.0 (StatSoft, USA) software. The reliability of differences between the control and experimental groups was determined using Student's parametric t-test, and the data were presented as mean ± standard error (M ± m format, where M is the arithmetic mean, and m is the standard error). For all statistical analyses, results with p < 0.05 were considered statistically significant.
3. Research Results
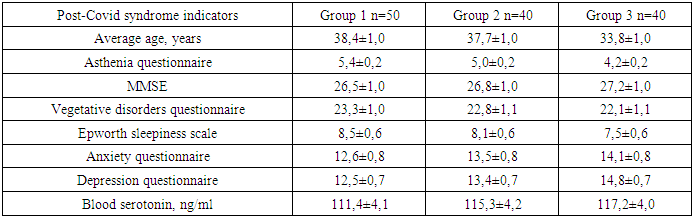
- When examining asthenic manifestations in patients using the "Asthenia Detection Questionnaire", it was found that, on average, our patients had moderate asthenic manifestations. When analyzing the MMSE scale results, our patients had mild cognitive impairments. Studies of autonomic dysfunctions using the " Vegetative disorders questionnaire" revealed, on average, moderate and mild autonomic manifestations in our patients. Sleep disorders in our patients using the "Epworth Sleepiness Scale" revealed mild disorders. Detection of anxiety and depressive manifestations in our patients revealed mild anxiety and mild depressive manifestations (Table 1). Blood serotonin levels also tended to decrease from normal levels. When analyzing the obtained data on clinical manifestations of post-COVID syndrome in our patients depending on age, we found that all clinical indicators on scales and questionnaires have an unreliable tendency for clinical signs to worsen with increasing age of patients (Table 1).
|
|
4. Discussion
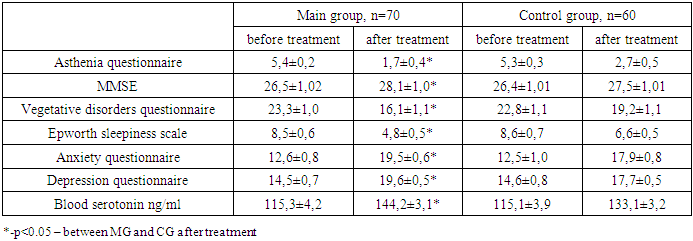
- This can be explained by the fact that micropolarization improves the disrupted neural connections in the brain disrupted by coronavirus infection. Our studies confirm that “... the basis of the persistent effect of brain micropolarization is the physiologically adequate action of low direct current on various areas of the brain with the activation of interstructural and intersystemic relationships, supported by self-regulation mechanisms. As a result of micropolarization, a new functional state of the central nervous system is formed, closer to the norm, with the achievement of a physiological level of dynamic homeostasis disrupted during the pathological process, which ensures a new level of implementation of various types of activities” [18]. In addition, it is possible that micropolarization can somehow stimulate the production of serotonin and through it improve the autonomic nervous system, reduce anxiety and depression, and improve sleep. Or perhaps both mechanisms of action of improving the condition of patients take place.Thus, signs of post-covid syndrome and a decrease in the level of serotonin in the blood are detected in the employees of the Ministry of Internal Affairs who have had COVID-19. Comprehensive rehabilitation in the form of drug therapy, as well as micropolarization of the brain, helps to increase the level of serotonin in the blood and correct the clinical neurological manifestations of post-COVID syndrome.
5. Conclusions
- 1. Asthenic, cognitive, vegetative manifestations, sleep disorders, anxiety and depression in most cases in the form of mild disorders, as well as a decrease in serotonin levels in the blood, which have an unreliable tendency to worsen clinical signs with increasing age of patients, were detected in employees of the Ministry of Internal Affairs with post-COVID syndrome.2. Comprehensive rehabilitation in the form of drug therapy, as well as micropolarization of the brain contribute to an increase in the level of serotonin in the blood and the correction of clinical neurological manifestations of post-COVID syndrome.
ACKNOWLEDGEMENTS
- The authors express their gratitude to the staff of neurology of the Sanatorium of the Medical Department of the Ministry of Internal Affairs of the Republic of Uzbekistan in helping to select patients for diagnosis and treatment; to the Head of the «Global Med System» clinic, MD Adambaev Z.I. for writing an article: to the professor of Mirdzhuraev E.M. of the Center for the Development of Professional Qualifications of Medical Workers under the Ministry of Health of the Republic of Uzbekistan for editing an article. The authors declare that they have no conflicts of interest when writing this article. The work was carried out within the framework of the dissertation work. When carrying out scientific work, their own funds were attracted.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML