-
Paper Information
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2024; 14(6): 1704-1707
doi:10.5923/j.ajmms.20241406.50
Received: Jun. 10, 2024; Accepted: Jun. 23, 2024; Published: Jun. 26, 2024

Determination of the State of the Sympatho-Adrenal System in Employees of the Company "UZ-AUTO MOTORS" and Measures to Prevent Recognized Violations
Mamazhanova Z. K., Khudzhamberdiev M. A., Kodirova G. I., Tashtemirova I. M., Xoliqova D. S.
Andijan State Medical Institute, Uzbekistan
Copyright © 2024 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Every year, arterial hypertension causes premature death in 7.7-10.4 million people. On average, only a third of hypertensive patients worldwide receive antihypertensive treatment. At the present stage, the main direction of occupational medicine is a comprehensive analysis of the health status of workers and the impact of professional activity on it [1,3]. Difficulties in the implementation of primary and secondary prevention of arterial hypertension are associated with the choice of the most suitable among modern, targeted and effective means of prevention and treatment of the disease and its complications.
Keywords: Antihypertensive treatment, Mexidol, Blood, Treatment
Cite this paper: Mamazhanova Z. K., Khudzhamberdiev M. A., Kodirova G. I., Tashtemirova I. M., Xoliqova D. S., Determination of the State of the Sympatho-Adrenal System in Employees of the Company "UZ-AUTO MOTORS" and Measures to Prevent Recognized Violations, American Journal of Medicine and Medical Sciences, Vol. 14 No. 6, 2024, pp. 1704-1707. doi: 10.5923/j.ajmms.20241406.50.
1. Introduction
- According to official data, 16-20% of pilots have high blood pressure, but in reality these relative figures are much higher, since many (more than 55%) hid the increase in pressure by taking antihypertensive drugs as self-medication [4]. In recent years, foreign and domestic researchers have focused on one of the variants of “arterial hypertension at work,” “stress arterial hypertension” in connection with modern diagnostic and treatment capabilities [2,5]. The prevalence of “occupational hypertension” has been examined in several studies. J. Stork et al. studied the blood pressure of workers at various industrial enterprises using round-the-clock monitoring. In 19% of patients with normal blood pressure, periodic outpatient examinations revealed arterial hypertension at work [2,5]. These results suggest that some patients have higher blood pressure at work than at the doctor's office. Psychosocial stress has been shown to increase cardiovascular morbidity and mortality (E.M. Cottington et al., 2011). This is especially true for people experiencing mental stress at work. In the scientific literature, there have been few studies of the activity of the sympatho-adrenal system in workers of enterprises with a stressful environment.
2. Purpose of the Study
- To determine the activity of the sympathoadrenal system in long-distance communication workers of the UzAvtoMotors company and to prevent identified disorders.From 1744 employees of UzAutoMotors, 661 employees of the quality assurance department and 1,083 employees of the transportation department were assessed for stress using the Minnesota Questionnaire and were divided into 4 groups. Group I (control) - healthy employees working in the quality assurance department (30 people); Group II - employees with hypertension working in the quality assurance department (34 employees), Group III - long-distance employees without hypertension (24 employees), Group IV - long-distance employees with hypertension (84 employees). 36 people with long-term arterial hypertension received Aevit, 1 tablet 2 times a day for 2 months, and 48 people, in addition to the standard drug, received Mexidol, 1 tablet 2 times 2 months.Before taking the test to determine catecholamines in urine, foods such as coffee, bitter tea, and spicy drinks were excluded from the diet. Determination of catecholamines in one portion of urine. If the final percentage of acid concentration is too high, it may cause false results in urine samples. The amount of catecholamines in blood serum was determined by immunoassay using a Mindray fax-2100 device (Germany).The data obtained during the study was statistically processed on a Pentium-IV personal computer based on the Windows 10 operating system, and the data was obtained using the Microsoft Office Excel-2017 software package. In addition, traditional variational parametric and nonparametric statistical methods were used. To determine the reliability of the results obtained, the Student coefficient was used.
3. Results and Discussion
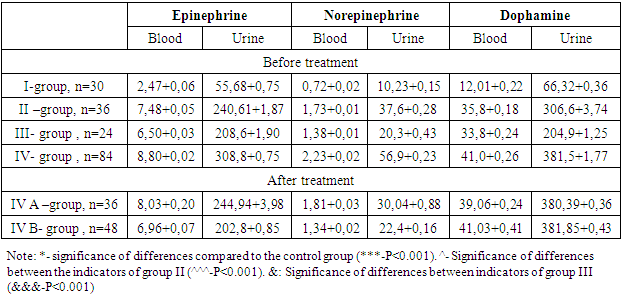
- When studying catecholamines in the blood serum of the examined groups, it was found that the levels of adrenaline, norepinephrine and dopamine in the blood serum were statistically significantly higher in patients with arterial hypertension compared with control groups. For example, in the group of hypertensive patients working in the quality control department, adrenaline was 7.48±0.08 nmol/l, norepinephrine - 1.73±0.02 nmol/l, dopamine - 35.2±0.27, according to compared to the control group - 3.0 times; norepinephrine increased by 2.4 times, dopamine by 2.9 times (P<0.001). In the group of patients without hypertension, serum catecholamine levels were as follows. Adrenaline-6.5±0.04 nmol/l, Norepinephrine-1.38±0.01 nmol/l; Dopamine - 33.8±0.43 nmol/l, adrenaline - significantly exceeded the control group by 63.1%, adrenaline - 15.1% decreased compared to group II.The values of norepinephrine were significantly higher than in the control group by 1.9 times (P<0.001), and the values were 25.3% lower than in group II. Dopamine values were significantly higher than in the control group by 2.8 times; compared to group II, the values decreased by 1.06 times; the values did not differ significantly (Table 1, Diagram 1).A study of the daily excretion of catecholamines revealed a statistically significant increase in the total urinary excretion of adrenaline, norepinephrine, dopamine, including adrenaline in the control group - 55.68±0.75 ng/ml, in patients with office hypertension - 240.61±1, it was 87 ng/ml and was significantly 4.3 times higher than in the control group, adrenaline in patients of group III was 208.6±1.90 ng/ml and was 3.7 times higher than in the control group, and compared to group II it was 1. It was found that excretion decreased by .2 (r<0.001). In group IV, that is, in the group with hypertension at a distance, adrenaline was 308.8±0.75 ng/ml and was 5.5 times higher than in the control group (p<0.001), by 28.3% compared with group II, and in comparison group III it was higher by 48.1% (r<0.001) (Table 1, diagram 1).It was found that the daily excretion of norepinephrine statistically increased. In the control group, norepinephrine was 10.23±0.15 ng/ml. Norepinephrine-37.6±0.28 ng/ml was significantly increased by 3.7 times compared to the control group in employees diagnosed with arterial hypertension (group II). In patients of group III, it was significantly higher by 1.9 times compared to the control group, and compared to group II, these indicators changed, that is, the excretion of norepinephrine significantly decreased by 53.9% (p <0.001).Urinary excretion of biogenic amines was statistically significantly increased in long-distance hypertensive travelers compared with other groups. The dopamine index was 381.5±1.77 and was significantly 5.7 times higher than the control group, 24.1% higher than group II and 86.2% higher than group III (r<0.001) (Table 1, diagram 1).
|
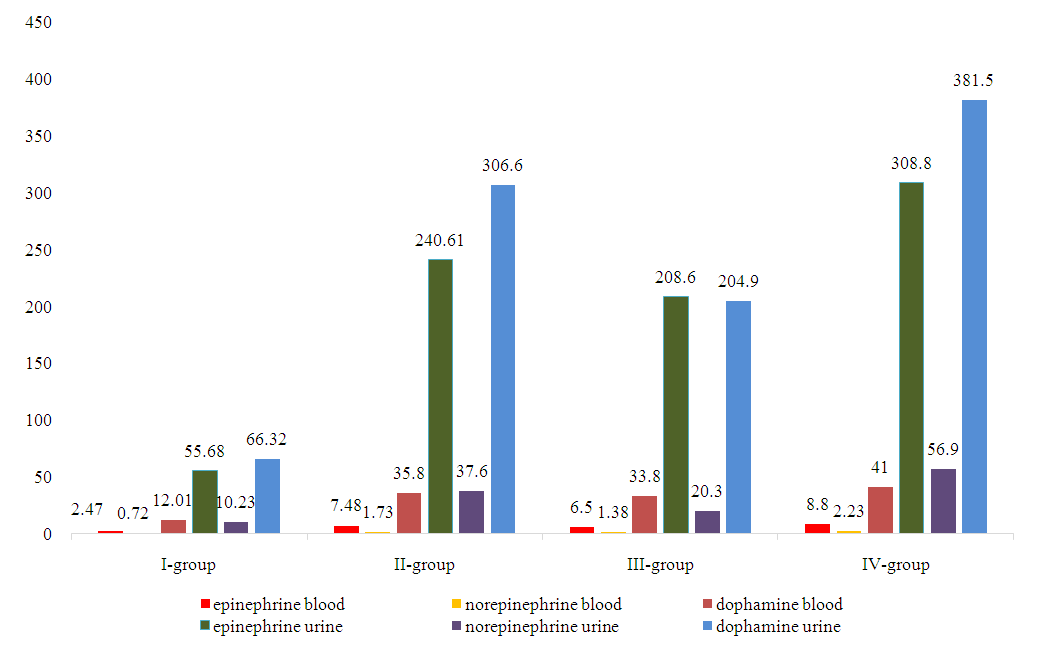 | Diagram 1. The amount of catecholamines in the blood and urine of UZ-AUTO MOTORS employees (* - Р<0,05; ** - Р<0,01; *** - Р<0,001) |
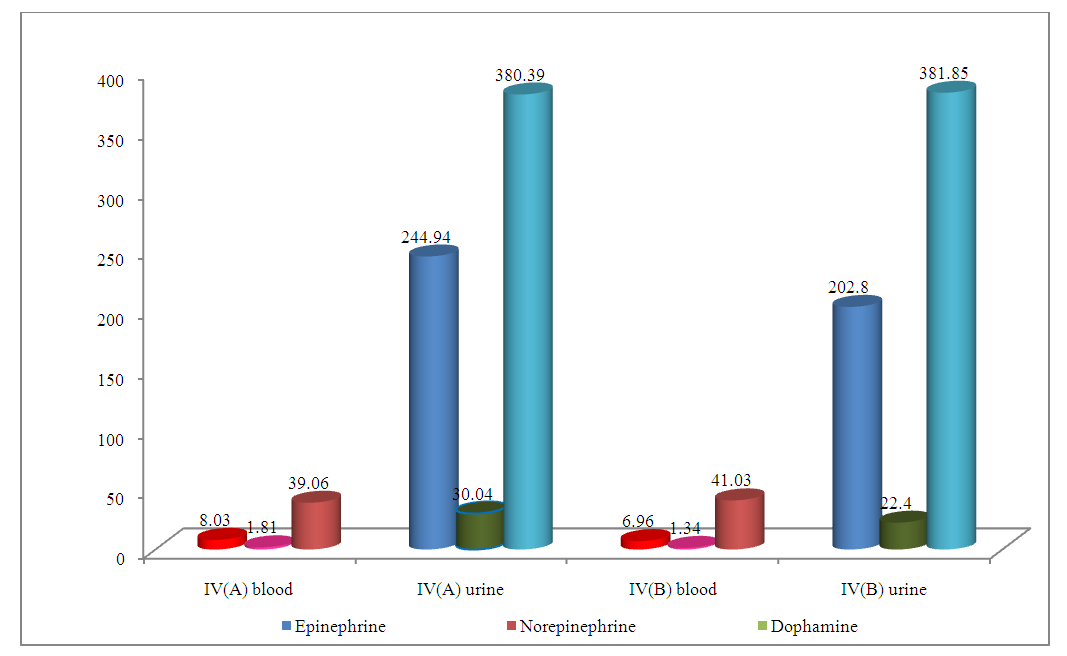 | Diagram 2. The amount of catecholamines after treatment among workers of the transport department of the UZ-AUTO MOTORS company. (* - P<0.05; ** - P<0.01; *** - P<0.001) |
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML