-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2024; 14(5): 1385-1388
doi:10.5923/j.ajmms.20241405.51
Received: Apr. 22, 2024; Accepted: May 21, 2024; Published: May 22, 2024

Prevention of Intradialysis Hypotension Episodes in Patients with Programmed Hemodialysis
Abdullaev Ikbol Jamolitdinovich1, Sabirov Maksud Atabaevich2, Umarov Odiljon Makhmudovich3
1Fergana Institute of Public Health Medicine, Fergana, Uzbekistan
2Republican Specialized Nephrology and Kidney Transplantation Scientific and Practical Medical Center, Fergana, Uzbekistan
3Fargona Regional Multidisciplinary Medical Center, Fergana, Uzbekistan
Copyright © 2024 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The aim of the study was the analysis of episodes of intradialysis hypotension in patients on hemodialysis against the background of hemodialysis procedures performed by ultrafiltration methods of different profiles and evaluation of the efficiency of extracorporeal detoxification depending on this process. Coordination and prevention of intradialysis hypotension is important in the practice of extracorporeal detoxification measures. Sixty-five patients undergoing hemodialysis were selected and divided into two study groups in the Extracorporeal Detoxification department of the Multidisciplinary Medical Center of the Fergana region. Episodes of intradialysis hypotension that occurred in patients undergoing hemodialysis against the background of hemodialysis sessions using ultrafiltration methods of various profiles for one month were studied and the efficiency of extracorporeal detoxification was evaluated. It was possible to reduce the number of episodes of intradialysis hypotension and increase the efficiency of hemodialysis by applying the ultrafiltration method of profile 1 to group 2.
Keywords: Chronic kidney disease, Planned hemodialysis, Extracorporeal detoxification, Intradialysis hypotension, URR, Kt/V
Cite this paper: Abdullaev Ikbol Jamolitdinovich, Sabirov Maksud Atabaevich, Umarov Odiljon Makhmudovich, Prevention of Intradialysis Hypotension Episodes in Patients with Programmed Hemodialysis, American Journal of Medicine and Medical Sciences, Vol. 14 No. 5, 2024, pp. 1385-1388. doi: 10.5923/j.ajmms.20241405.51.
Article Outline
1. Introduction
- The negative results of the clinical consequences of hypotension are clearly reflected in patients undergoing hemodialysis with any method of extracorporeal detoxification. This issue is quite controversial due to the fact that there are conflicting opinions in the literature on this topic [1-2]. In the absence of reliable randomized clinical trials, it is recognized that a significantly increased risk of death is inevitable in groups with high (> 180 mmHg) and low (< 110 mmHg) blood pressure (BP) [2]. P.G. Zager et al (1998) suggested that the curve of the influence of blood pressure on the survival of patients undergoing hemodialysis (EH) has a U-shaped characteristic. A.V. Chobanian et al (2003) found that the target BP recommended for EH patients differs from that of general populations. According to their data, the volume of blood pressure (130/80 mmHg) after dialysis is less than the size of predialysis blood pressure (140/90 mmHg), which is explained by the accumulation of fluid in the body during the period between dialysis [3]. According to the clinical guidelines for Chronic kidney Disease (Clinical Practice Guidelines for Chronic Kidney Disease (K/DOQI 2016)), systolic blood pressure is 20 mm. above and below this value is considered intradialysis hypotension (IDH). Usually a decrease in blood pressure by 10 mm. causes a number of clinical symptoms in patients with elective HD (abdominal discomfort, nausea, vomiting, yawning, convulsions, dizziness, etc.). According to clinical observations, the incidence of IDH complications among patients with planned HD is 10-50%, and arterial hypotension occurs in about one in five cases of HD and, of course, requires serious medical intervention [4]. In general, IDH is one of the most common complications that occur during treatment with elective hemodialysis in patients with stage 5 chronic kidney disease (CKD) [5]. Coordination and prevention of intradialysis hypotension is important in the practice of extracorporeal detoxification measures. In the practice of extracorporeal detoxification, the "pure weight" concept is also one of the important gradients. In fact, "pure weight" is the body weight in the normal state of extracellular fluid. In this case, not only the absence of edema in the patient is taken into account, but also body weight measured in routine hemodialysis patients in hemodynamically stable conditions after dialysis. During HD, excess fluid is removed from the patient, and usually the patient's blood pressure remains normal even without antihypertensive drugs [5]. At this stage, it is important to strictly control intravascular blood volume during HD. Therefore, it is extremely important to conduct research on the prevention of IDH episodes during extracorporeal therapy. The aim of the study was the analysis of episodes of intradialysis hypotension in patients on hemodialysis against the background of hemodialysis procedures performed by ultrafiltration methods of different profiles and evaluation of the efficiency of extracorporeal detoxification depending on this process.
2. Material and Methods
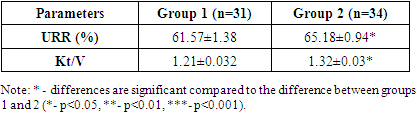
- Sixty-five patients undergoing elective hemodialysis in the extracorporeal detoxification department of the Fergana Regional Multidisciplinary Medical Center were selected for the study. In order to randomize the study groups, patients with diseases directly related to hemodynamic disorders (diabetes mellitus and other endocrine diseases, metabolic syndrome, CKD with hypertensive nephropathy, decompensated heart failure) were not included in the study. Two study groups were formed from them. Group 1 patients (n=31) received scheduled hemodialysis sessions using the standard profile ultrafiltration method. Group 2 patients (n=34) were performed elective hemodialysis sessions according to profile 1 by ultrafiltration method. Basically, hemodialysis sessions were held 3 times a week for 4 hours each [6]. Extracorporeal therapy was performed on a Fresenius Medical Care 4008 S artificial kidney machine.The mean age of Group 1 patients was 46.9±1.53 years, and the duration of hemodialysis was 7.76±1.47 years. The mean age of Group 2 patients made up 46.2±1.72 years, and the duration of hemodialysis lasted 7.92±1.53 years. Follow-up was done for 1 month and IDH episodes occurring during this period were recorded in the chart of the related study group. The efficiency of extracorporeal therapy in each study group was calculated according to the URR index, the Kt/V value was monitored and these results were included in the corresponding table. The obtained results were subjected to statistical processing.
3. Results
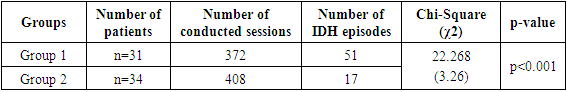
- In our one-month study of the frequency of intradialysis episodes and assessment of the impact and dependence of hemodialysis interventions by different ultrafiltration methods as a risk factor, we obtained the following results (Tab.1).
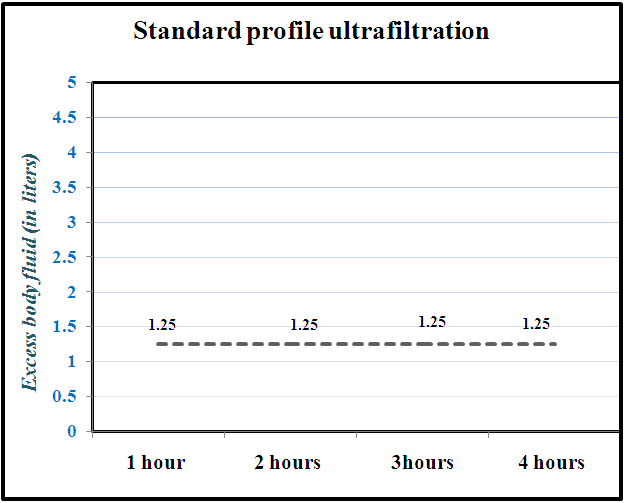 | Figure 1. Ultrafiltration method obtained by Group 1 patients |
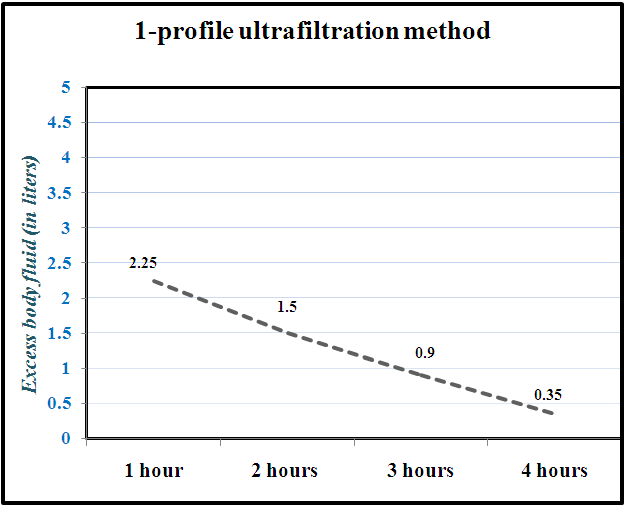 | Figure 2. Ultrafiltration method obtained by patients in Group 2 |
4. Discussion
- According to the rules of extracorporeal detoxification, it is not recommended to remove more than 5% of the patient's body weight in one session of HD. However, in clinical practice, due to a number of reasons (the patient has heart failure, taking more fluid than recommended, etc.), cases of fluid accumulation of more than 5% of body weight during the interdialysis period are quite common. In this case, it is not possible to remove all excess weight from the patient using standard profile ultrafiltration. If this is done, the risk of developing IDH will increase significantly. And the lack of excess fluid in the body leads to the patient experiences hemodynamic disorders, including arterial hypertension, does not get rid of discomfort and has no meaningful improvement in quality of life, in a word, HD does not have sufficient efficiency. In this case, it is advisable to conduct sessions of HD by 1-profile ultrafiltration. Based on the results obtained, the X-index was calculated in order to statistically analyze the influence and dependence criteria of HD sessions performed by different profile ultrafiltration methods as a risk factor for the development of IDH episodes. The X2 criterion was equal to a value of 22.3, which reflected a high degree of reliability (p<0.001) [14]. Also, according to the numerical Pearson coefficient, the standard ultrafiltration risk factor profile and the resulting IDH showed a moderate correlation (Fig.3).
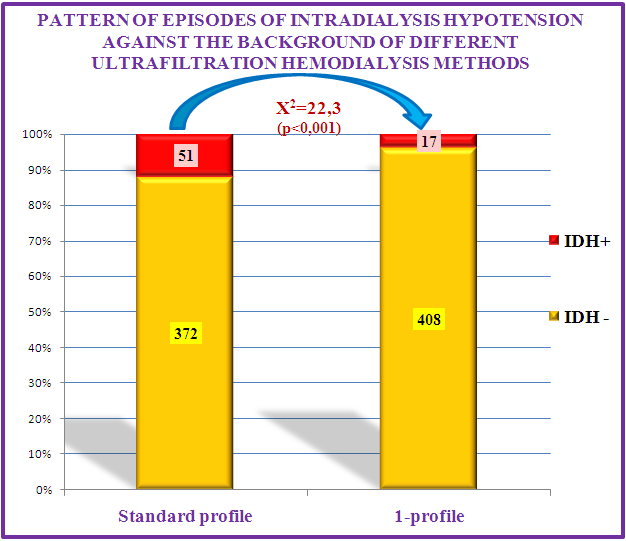 | Figure 3. Influence pattern and correlation of hemodialysis interventions with different ultrafiltration profiles as a risk factor for episodes of intradialysis hypotension |
|
5. Conclusions
- Thus, IDH episodes were more than 3 times more frequent in patients who underwent standard profile ultrafiltration HD procedures than in the study groups who underwent 1-profile ultrafiltration HD procedures. Also, the efficiency of extracorporeal detoxification in group 2 patients with elective HD was higher, although in less reliable (p<0.05) values than in group 1, as reflected in the exact arithmetic numbers of URR and Kt/V gradients, as well as statistical analysis. The results also showed that the profile of ultrafiltration method 1 was distinct.Thus, by using this method in the extracorporeal treatment of patients with elective HD, it will be possible to reduce the number of IDH episodes, improve the efficiency of HD and increase patients' survival rate.
Conflict of Interests Statement
- The authors declare no conflict of interest. This study does not include the involvement of any budgetary, grant or other funds. The article is published for the first time and is part of a scientific work.
ACKNOWLEDGEMENTS
- The authors express their gratitude to the management of the multidisciplinary clinic of Fergana Regional Multidisciplinary Medical Center for the material provided for our study.
References
| [1] | Bradshaw, W. Intradialytic hypotension: a literature review // Renal Society of Australasia Journal. – 2014. – Vol. 10, № 1. – P. 22-29. |
| [2] | Flythe, J.E. Rapid fluid removal during dialysis is associated with cardiovascular morbidity and mortality // Kidney International. – 2015. – Vol. 79, № 2. – P. 250-257. |
| [3] | Chazot C., Deleaval P., Bernollin A.L. et al. Target weight gain during the first year of hemodialysis therapy is associated with patient survival // Nephron. Clin. Pract. 2014. Vol. 126 (3). P. 128–134. doi:10.1160/TH11-08-0587.- PMID 22072293. |
| [4] | Shishkin A.N., Fedorova Yu.Yu. Intradialytic hypotension: factors associated with the hemodialysis procedure // Nephrology. 2014. No. 2. Volume 16. P. 64-68. |
| [5] | Shilo V.Yu., Drachev I.Yu. Hypotensive episodes on program hemodialysis during the dialysis procedure: a modern approach to diagnosis, prevention and correction. Clinician. 2018; 12(3-4): 30-36. https://doi.org/10.17650/1818-8338-2019-12-3-4-30-36. |
| [6] | Appendix 7 to the order of the Minister of Health No. 671 of December 29, 2018 “Clinical instructions for planned hemodialysis treatment of patients with stage 3-5 chronic kidney disease”. |
| [7] | Stetsyuk E.A. Basics of hemodialysis // Moscow GEOTAR-MED 2001. |
| [8] | Martini A., Ammirati A., Garcia C. et al. Evaluation of quality of life, physical, and mental aspects in longevous patients with chronic kidney disease // Int. Urol. Nephrol. 2018 Apr. Vol. 50 (4). P. 725–731. doi:10.1016/j.jacc.2010.01.076. PMID 21029872. |
| [9] | Borodulina E.O. Relationship between blood pressure parameters and chronic heart failure in patients on hemodialysis // Clinical Nephrology. – 2018. – No. 1. – P. 20-25. |
| [10] | McIntyre, C.W. Hemodialysis–associated cardiomyopathy: a newly defined disease entity // Seminars in Dialysis. – 2014. – Vol. 27, № 2. – P. 87-97. |
| [11] | Borodulina E.O. Variability of blood pressure and left ventricular hypertrophy in patients on hemodialysis // Nephrology and dialysis. – 2018. – Vol. 20, No. 1. – P. 56-63. |
| [12] | Karpunin S.A. Cardiac remodeling and pulmonary hypertension in patients receiving hemodialysis // Nephrology and dialysis. – 2016. – Vol. 18, No. 1. – P. 62-68. |
| [13] | Cohen, J.B. Antihypertensive medication in patients pre- and postdialysis: still hazy after all these years // Clinical journal of the American Society of Nephrology. – 2016. – Vol. 11, № 8. – P. 1327-1329. |
| [14] | https://medstatistic.ru/calculators/calchi.html |
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML