-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2024; 4(2): 294-296
doi:10.5923/j.ajmms.20241402.27
Received: Jan. 7, 2024; Accepted: Feb. 3, 2024; Published: Feb. 8, 2024

The Incidence of Pathology of Adnexal Apparatus of the Eye Among Children and Adolescents with Tuberculosis
Mamatkhujaeva Gulnarakhan Najmidinovna
Department of Ophthalmology, Andijan State Medical Institute, Andijan, Uzbekistan
Correspondence to: Mamatkhujaeva Gulnarakhan Najmidinovna, Department of Ophthalmology, Andijan State Medical Institute, Andijan, Uzbekistan.
Copyright © 2024 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Pathology of the adnexal apparatus of the eye is widespread among children and adolescents and remains one of the most pressing problems in pediatric ophthalmology. This article provides information on the incidence of inflammatory diseases of the adnexal apparatus of the eye in children and adolescents with tuberculosis. Studies have shown that the most common pathologies of the adnexal apparatus of the eye in children and adolescents with tuberculosis were blepharitis and chronic conjunctivitis, which amounted to 45.9±1.2%. The incidence of blepharitis was 25.7±1.1%, the incidence of chronic conjunctivitis among children and adolescents with tuberculosis was 20.0±1.0%. Inflammatory diseases of the adnexal apparatus of the eye can cause many complications and reduce the quality of life in children and adolescents with tuberculosis. Therefore, it is necessary to carry out timely diagnosis, treatment and prevention of complications of these diseases.
Keywords: Blepharitis, Chronic conjunctivitis, Incidence, Children, Adolescents, Tuberculosis
Cite this paper: Mamatkhujaeva Gulnarakhan Najmidinovna, The Incidence of Pathology of Adnexal Apparatus of the Eye Among Children and Adolescents with Tuberculosis, American Journal of Medicine and Medical Sciences, Vol. 4 No. 2, 2024, pp. 294-296. doi: 10.5923/j.ajmms.20241402.27.
Article Outline
1. Introduction
- Pathology of the adnexal apparatus of the eye - lacrimal organs, eyelids and conjunctiva - constitutes the largest group of diseases, from 10 to 35% in the overall structure of morbidity of the organ of vision [1,2,5].The peculiar anatomical, topographical and morphological features of the structure of the adnexal apparatus of the eye largely determine the uniqueness of the course of pathological processes in them [3,6]. In addition, despite the successful achievements in modern ophthalmology, the treatment of diseases of the eyelids and conjunctiva of inflammatory origin in children and adolescents with common infectious diseases is still of great relevance [4,9].Blepharitis is one of the most common ophthalmological diseases among children and adolescents, manifested by inflammation of the eyelids. Inflammation of the marginal areas of the eyelids in most cases is a chronic disease that is quite difficult to treat. The persistent recurrent course of blepharitis contributes to the development of conjunctivitis, keratitis and weakened vision in children and adolescents [10].Topicality of the researchis that the incidence of pathology of the adnexal apparatus of the eye is growing due to the increase in their prevalence among children and adolescents [7,8].Purpose of the study: To study the incidence of inflammatory diseases of the adnexal apparatus of the eye among children and adolescents with tuberculosis.
2. Materials and Methods of the Research
- Children and adolescents with tuberculosis at the age of 1 to 17 years who were being treated for tuberculosis at the Andijan regional anti-tuberculosis dispensary were examined. A comprehensive ophthalmological examination included: determination of visual acuity without and with correction, skiascopy, autorefractometry, biomicroscopy, study of binocular functions, direct and reverse ophthalmoscopy.Clinical, biochemical, immunological, microbiological studies and examination by specialists were also carried out.
3. Results and Discussion
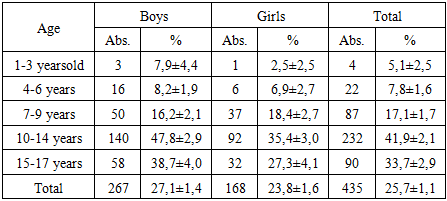
- Out of the 1690 examined children and adolescents with tuberculosis (985 boys and 705 girls) aged from 1 to 17 years, chronic inflammatory diseases of the adnexal apparatus of the eye were identified in 775 children and adolescents with tuberculosis, which amounted to 45.9 ± 1. 2% of the total number of those examined.During the examination, blepharitis was identified in 435 children and adolescents with tuberculosis, which is 25.7±1.1% of the total number of those examined.As can be seen from Table 1, with increasing age there was an increase in the detection rates of blepharitis, and with each age group the increase was more significant.
|
|
4. Conclusions
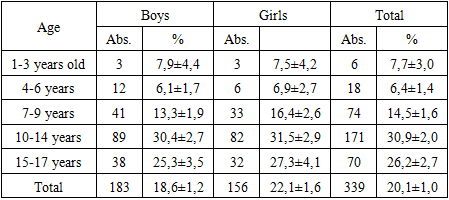
- Thus, our studies have shown that the incidence of chronic inflammatory diseases of adnexal apparatus of the eye among children and adolescents with tuberculosis is 45.9±1.2%. The incidence of blepharitis is 25.7±1.1%, the incidence of chronic conjunctivitis among children and adolescents with tuberculosis is 20.0±1.0%.Inflammatory diseases of the adnexal apparatus of the eye can cause many complications and reduce the quality of life in children and adolescents with tuberculosis. Therefore, it is necessary to carry out timely diagnosis, treatment and prevention of complications of these diseases.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML