-
Paper Information
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2023; 13(10): 1409-1416
doi:10.5923/j.ajmms.20231310.11
Received: Sep. 14, 2023; Accepted: Sep. 26, 2023; Published: Oct. 6, 2023

Analysis of the Results of Complex Treatment of Patients with Pancronecrosis Complicated with Sepsis
Tokhir Musoev
Bukhara Branch of the Republican Scientific Center for Emergency Medical Care, Bukhara State Medical University, Uzbekistan
Correspondence to: Tokhir Musoev , Bukhara Branch of the Republican Scientific Center for Emergency Medical Care, Bukhara State Medical University, Uzbekistan.
| Email: |  |
Copyright © 2023 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

A retrospective cohort study of the results of a comprehensive examination and treatment of 97 patients with pancreatic necrosis was carried out. Analysis of the results of traditional methods of treatment of pancreatic necrosis complicated by sepsis showed a high level of complications of the disease of 38.1% and mortality of 30.9% due to the lack of objective criteria for predicting the development of pancreatogenic sepsis and multiple organ dysfunction syndrome, which requires detailed studies of the pathogenetic mechanisms of this formidable disease.
Keywords: Pancreatic necrosis, Systemic inflammatory response syndrome, Sepsis as a complication of pancreatic necrosis, Conservative treatment, Surgical treatment, Immediate and long-term results
Cite this paper: Tokhir Musoev , Analysis of the Results of Complex Treatment of Patients with Pancronecrosis Complicated with Sepsis, American Journal of Medicine and Medical Sciences, Vol. 13 No. 10, 2023, pp. 1409-1416. doi: 10.5923/j.ajmms.20231310.11.
Article Outline
1. Introduction
- There are many factors that determine the choice of treatment for pancreatic necrosis, among them the most significant are the speed and area of development of the necrobiotic process, both in the pancreas itself and around it [1,2,6,9]. Meanwhile, one of the current priority approaches in choosing tactics for treating pancreatic necrosis is taking into account the phases of the inflammatory process. Based on this approach, the following principles for choosing treatment tactics have taken root in modern pancreatology: use purely conservative therapy as a priority; conservative therapy with active wait-and-see tactics and use surgical treatment according to strict indications (uncertainty in diagnosis, the presence of progressive peritonitis and/or shock, progressive jaundice); actively use the surgical method of treatment, considering conservative therapy only a period of preoperative preparation [3,10,29,30]. An analysis of the literature over the past 10 years has shown that there are more and more supporters of conservative treatment of pancreatic necrosis with active expectant management. To increase the effectiveness of diagnostic and treatment tactics, proponents of this approach offer complexes of algorithms based on: combating pain and problems with bile outflow; suppression of secretory activity of both the pancreas itself and the stomach; complex anti-enzyme, anti-inflammatory and detoxification therapy; prevention of infection of the pancreas and correction of vascular changes in this organ [1,3,6,7,9,10,13,14].The basis of the leitmotif of using a surgical method for treating pancreatic necrosis is to prevent the death of the patient. Proponents of active wait-and-see tactics, using the entire available arsenal of conservative therapy, begin to use surgical techniques in patients with pancreatic necrosis with only one goal - to prevent further rapid progression of pancreatic necrosis. In this regard, many issues related to the indications and timing of surgical interventions in patients with pancreatic necrosis remain far from resolved and sometimes even controversial [4,6,9]. The absolute indication for surgical treatment of pancreatic necrosis is its purulent-necrotic complication. On this issue, most surgeons are of the same opinion. However, in the matter of surgical treatment of sterile pancreatic necrosis, many aspects related to the timing and volume of surgical intervention still remain scattered. And this is one of the main issues that are discussed at specialized conferences and congresses on pancreatology. Is surgical intervention necessary for a sterile form of pancreatic necrosis?Complications of the disease such as infection, abscess formation, and biliary pancreatic necrosis that is not amenable to endoscopic intervention are considered generally accepted direct indications for the use of surgical treatment methods. However, the options for complications of pancreatic necrosis in the form of a progressive deterioration of the patient’s condition, the development of multiple organ failure, progressive necrosis of the pancreas, as well as with its total damage with focal infection remain controversial [11]. Other authors prioritize general changes in the body and believe that direct indications for surgical treatment should be the presence of purulent peritonitis, progressive multiple organ failure syndrome, ineffectiveness of conservative therapy, and even the possible development of sepsis syndrome [12]. But there is also a group of third opinions, when indications for surgical treatment methods should be individual cases that go beyond the general rules of limitation. As an example, we can cite the opinion of researchers regarding the indications for surgery in the development of a clinical picture of peritonitis, even with only infiltrative changes in the pancreas [9].Such versatility of modern information prompted us to conduct a study to evaluate the immediate and long-term results of complex traditional treatment of patients with pancreatic necrosis complicated by sepsis.
2. Material and Methods
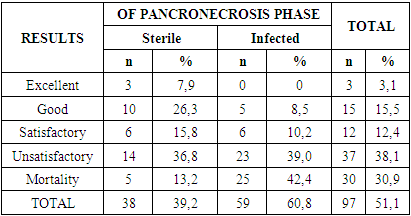
- A retrospective cohort study of the results of a comprehensive examination and treatment of 97 patients with pancreatic necrosis was conducted. All patients were treated and examined at the Bukhara regional branch of the Republican Scientific and Practical Medical Center for Emergency Medical Care from 2013 to 2017. In 38 (39.18%) cases, pancreatic necrosis was pregnant, and in the remaining 59 (60.82%) cases, it was infected. Moreover, among patients with infected pancreatic necrosis, in 20.62% of cases, infected pancreatic necrosis occurred against the background of severe sepsis, and in 4.12% of cases - septic shock. Thus, the patients were divided into 3 subgroups: Subgroup I – patients with sterile pancreatic necrosis (38 patients; 39.18%), Subgroup II – patients with infected pancreatic necrosis (35 patients; 36.08%), Subgroup III – patients with infected pancreatic necrosis, complicated by sepsis (24 patients; 24.74%). There were 62.9% male patients and 37.1% female patients. The base contingent consisted of patients of the most working age. Alcohol etiology of the disease accounted for 28.9% of patients. In 43 (44.3%) patients, the cause of pancreatic necrosis was cholelithiasis. The gastrogenic origin of the disease was identified in 25 (25.8%) patients. In 1 patient (1.03%), the etiological cause of pancreatic necrosis could not be determined. Patient visits to the clinic from the onset of the disease were not unambiguous, but there was a certain pattern among subgroups. In the group of patients, active surgical tactics were predominantly used, consisting of early laparotomies, despite the phase (sterile or infected) of the pathological process and the form (fine-focal, large-focal, subtotal, total) of the necrotic lesion. The main indications for surgical operations were negative dynamics of the disease despite conservative therapy and/or the presence of signs of peritonitis.If laparotomy was performed during the sterile phase of pancreatic necrosis, at the first stage an inspection of the abdominal organs was performed. If the development of pancreatic necrosis was suspected, the omental bursa was opened and a visual inspection was performed. The operation was completed with sanitation and drainage of the omental bursa and abdominal cavity with several drains. In the case of the presence of dead areas of the pancreas, necrotic tissue was removed using blunt and sharp means. This procedure was sometimes very dangerous due to the possible development of arrosive bleeding or the formation of digestive fistulas. In case of biliary origin of pancreatic necrosis, interventions were performed on the gallbladder and bile ducts. In case of infected pancreatic necrosis, the main purpose of laparotomy was the timely and complete implementation of necrosequestrectomy, drainage of purulent cavities of parapancreatic tissue for subsequent sanitation. The omental bursa and all possible cavities formed, which are filled with pus, were opened. Necrotic tissue of the pancreas and retroperitoneal space was removed using blunt and sharp methods. The latter was necessarily subjected to a thorough digital revision. Drainage was performed in the retroperitoneal space, omental bursa, and abdominal cavity.To assess the condition of a patient with acute infected pancreatic necrosis complicated by sepsis, a gradation scale was used, consisting of the following criteria: dynamics and frequency of development of multiple organ dysfunction syndrome; frequency and severity of purulent complications in the general structure of treatment measures. The immediate results of treatment of patients with pancreatic necrosis were assessed according to four standard groups of results: excellent, good, satisfactory and unsatisfactory. An excellent result was characterized by the preservation of the anatomical integrity and functional usefulness of the pancreas in the absence of any inflammatory phenomena. A good result was characterized by a violation of the anatomical integrity of the pancreas in the presence of compensated functional activity, which did not require drug correction. There are no inflammatory phenomena. A satisfactory result was characterized by a violation of the anatomical integrity of the pancreas, the presence of local complications that do not require special surgical interventions and tend to heal independently or scar in the short term. The functional activity of the pancreas is preserved or compensated by medication. Temporary local inflammatory phenomena associated with the course of the above complications are possible. The unsatisfactory result was characterized by a violation of the anatomical integrity of the pancreas. The presence of local complications requiring repeated surgical interventions, the presence of arrosive bleeding requiring special intervention. The functional activity of the pancreas is impaired with no prospect of recovery. Long-term drug compensatory (replacement) therapy is required. Inflammatory phenomena associated with ongoing necrosis of the pancreatic parenchyma persist, but with a tendency to be limited. The death of the patient as a criterion for the outcome of treatment could be classified as unsatisfactory, however, given the high frequency of this outcome in the treatment of patients with pancreatic necrosis, we highlighted this point separately.To study the long-term results of treatment and the quality of life of patients who suffered pancreatic necrosis, the following methods were used: questionnaires using the GIQLI questionnaire, clinical examination, ultrasound and computed tomography of the abdominal organs, magnetic resonance imaging.
3. Research Results and Discussion
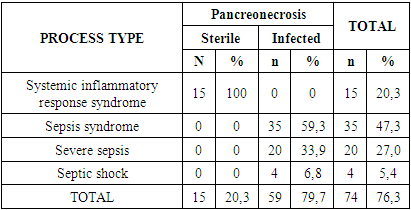
- According to archival material, acute pancreatitis was diagnosed only in 68 (71.1%) patients. In the remaining cases (28.9%), before hospitalization in our clinic, diagnoses of acute cholecystitis (15.5%), perforation of a gastroduodenal ulcer (7.2%), acute intestinal obstruction (4.1%) and acute appendicitis (3) were established., 1%). In the medical history at the time of hospitalization of the patients, 687 pathological signs were described. Of these, 26.6% were in patients of subgroup I, 39.7% in patients in subgroup II and 33.6% in patients in subgroup III. The distribution of these pathological signs showed that pain was predominant (it was noted in all 100% of cases). The pain was localized in the epigastrium, right or left hypochondrium; in most cases, the pain radiated to the left costovertebral angle, and then, in descending order, to the left shoulder, behind the sternum, between the shoulder blades. Pain was the flagship among the pathological manifestations of the disease in all analyzed subgroups. Dyspeptic disorders are a constant companion of destructive pancreatitis. They were in second place in terms of frequency of registration after pain syndrome and accounted for 93.8%. Among the types of dyspeptic disorders, nausea, indomitable vomiting that did not bring relief, constipation, flatulence and bloating prevailed. Moreover, in subgroups II and III, this symptom complex was noted in all patients, while in patients of subgroup I they bothered patients only in 84.2% of cases.Local symptoms of acute pancreatitis were positive in 90.7% of cases. Local symptoms characteristic of acute pancreatitis occurred in all patients. Tension of the muscles of the anterior abdominal wall and symptoms of peritoneal irritation were noted in 100% of cases in patients of subgroups II and III, whereas among patients of subgroup I they occurred only in 29 (76.3%) patients. Almost half of the patients with destructive pancreatitis (43.3%) had icterus of the sclera and skin upon admission. Among patients of subgroup I there were 34.2% of them, among patients of subgroup II - in 40.0% of cases and among patients of subgroup III - in 62.5% of cases. Pathological signs of the cardiovascular system were in the form of tachycardia, recorded in 90.7% of cases, and a decrease in systolic blood pressure below 100 mm Hg. Art. in 68.0% of patients. Tachycardia was recorded in 100% of cases among patients of subgroups II and III, while in patients of subgroup I, increased heart rate was recorded only in 76.3% of cases. It should be noted that tachycardia and a decrease in systolic blood pressure were noted by us in the early stages of the development of destructive pancreatitis. An increase in body temperature above 37 0C was recorded in 75 (77.3%) cases. Moreover, among patients of subgroups II and III, as in the previous case, hyperthermia was noted in all cases, whereas in patients of subgroup I only in 16 (42.1%) cases. We noted disorders of the respiratory system in 70 (72.2%) patients. In subgroup I, patients with shortness of breath were 36.8%, in subgroup II – 91.4%, in subgroup III – in 100% of cases. The identified pathological manifestations of the genitourinary system were presented in the form of hematuria, proteinuria, cylindruria or a combination thereof. In total, there were 37 (38.1%) patients with such disorders. There was only one patient in subgroup I, 12 (34.3%) patients in subgroup II, and all 24 patients in subgroup III. Mental and nervous system disorders upon admission were identified in 33 (34.0%) patients. They manifested themselves in 22 (22.7%) patients in the form of euphoria, anxiety and negativism. Psychomotor agitation and hallucinations were diagnosed in 9 (9.3%) patients. Severe mental depression, sometimes even to the point of coma, was diagnosed in 2 (2.1%) patients.Diagnostic laparoscopy was performed in 48 (49.5%) patients. On the 1st day of hospitalization it was used in 19 patients, on the 2nd day – in 10 patients, on the 3rd day – in 8 patients, on the 4th day – in 7 patients and on the 5th day – in 4 patients. The average duration of this intervention was 3.1±1.1 days. Clinical and morphological parallels revealed a predominance of patients with total (32.0%) and subtotal (26.8%) necrotic lesions of the pancreas. With subtotal damage, the head and body of the pancreas were predominantly affected. In 40 (41.2%) patients, necrotic lesions of the pancreas were focal. Moreover, in 21.6% of cases there is a large-focal lesion, and in 19.6% of cases there is a small-focal lesion. A comparative analysis between sterile and infected forms of pancreatic necrosis revealed that in the first case, focal (13.9 times) prevailed, and in the second case, widespread (46.6 times) necrotic lesions of the pancreas prevailed. The average severity of damage by acute pancreatic necrosis was 8.4±1.1 points.The dispersion of the average value decreased from 10.1±0.9 points for total pancreatic necrosis to 6.8±2.9 points for small-focal pancreatic necrosis (p<0.05). In the infected form of pancreatic necrosis, the lesion severity index was 1.9±0.3 points higher than in patients with a sterile form of pancreatic necrosis (p<0.05).As can be seen from the description of the course of surgical interventions, there were several types per patient. In total, according to the operation protocols, 451 surgical interventions were performed. At the same time, an average of 4.6±1.1 technical stages were performed for each patient. The leaders in these stages were drainage interventions (215), which amounted to 47.6%. At the same time, in 23.9% of cases, the omental bursa was drained and in 23.7% of cases, the abdominal cavity was drained. It should be noted that drainage of the abdominal cavity was performed without drainage of the omental bursa. But drainage of the omental bursa was carried out repeatedly, which causes the difference in values. Necrosequestrectomy was performed in 13.7% of cases (62 times). Omentobursostomy and marsupialization of the omental bursa was performed in 13.5% of cases (61 times). Parapancreatic cage drainage was performed 48 times (10.6%). Interventions for cholelithiasis were limited to cholecystostomy (1.3%) and cholecystectomy with drainage of the bile ducts (8.2%). In 22 (4.9%) cases, the suppurating pancreatic cyst was opened and drained. The volume and nature of surgical interventions performed in the context of the pancreatic necrosis phase showed a 4.4-fold prevalence in patients with infected pancreatic necrosis. In the phase of sterile pancreatic necrosis, there was an average of 2.2 ± 1.0 types of surgical intervention per patient, and in the infection phase this value was 2.8 times higher.An analysis of the distribution of surgical interventions performed in the sterile phase of pancreatic necrosis depending on the morphostructural nature of the pancreatic lesion showed that drainage surgical interventions prevailed in small-focal and large-focal pancreatic necrosis. In case of subtotal damage to the pancreas, the volume of surgical interventions was distributed evenly between drainage of the abdominal cavity, drainage of the omental bursa, cholecystostomy, cholecystectomy with drainage of the ducts, and omentobursostomy with marsupilization of the omental bursa. In patients with small focal necrosis of the pancreas in the sterile phase of pancreatic necrosis, an average of 1.8±0.3 types of surgical interventions were performed. For large-focal lesions this value was 2.2±1.2, and for subtotal lesions of the pancreas - 5.0±1.1 stages of surgical intervention. Cholecystectomy with drainage of the bile ducts prevailed among patients with small focal pancreatic necrosis in the sterile phase of the disease. This nature of the surgical intervention is due to those cases where the operation was performed for acute calculous cholecystitis, but intraoperative findings revealed small-focal pancreatic necrosis. In such cases, after cholecystectomy, it was mandatory to drain the bile ducts and drain the omental bursa, followed by targeted conservative therapy for pancreatitis. In the infected phase of pancreatic necrosis in patients with large-focal lesions of the pancreas, there were an average of 5.8 ± 1.5 surgical stages of the operation per 1 patient, with subtotal lesions - 5.9 ± 1.0, and with total lesions - 6.6 ± 2, 1. The variety of surgical techniques performed in the infected phase of pancreatic necrosis was more diverse than in the sterile phase. Most patients (up to 82.3%) were operated on within the first week, while 45.9% of patients were operated on within the first 2 days from the onset of the disease; in this group of patients, the tactics of early operations for pancreatic necrosis were predominant. The cohort retrospective study was based on data defining the final verification diagnosis. In a number of patients, during relaparotomy, performed 2-3 weeks after the first operation, there were pathomorphological manifestations of an already infected form of pancreatic necrosis. These patients had formed necrotic sequestra and abscesses of the omental bursa. Therefore, during the analysis, we took as a basis the final version of the diagnosis verification. In total, 58 patients underwent relaparotomy. Moreover, in 8 they were performed twice, and in 4 – three times. In one patient, relaparotomy was performed 4 times.In most cases, pancreatic necrosis occurred with various complications, which were often combined and thus could manifest in several ways in the same patient. It is they who determine the urgency of surgical intervention and tactics for pancreatic necrosis. Peritonitis was detected in 49 (55.5%) patients. Local peritonitis was diagnosed in 16.3% of patients, diffuse - in 22.4% and diffuse - in 61.2% of patients. The serous nature of the effusion was noted in 18.4% of patients, hemorrhagic - in 32.6%, purulent - in 14.3% and fibrinous-purulent - in 34.7% of patients.Of course, it should be taken into account that peritonitis in patients was an indication for surgical intervention. However, given the fact that if the exudate was serous or hemorrhagic, minimally invasive interventions would have been very effective, nevertheless, during that period of medical care, the more complex and traumatic laparotomy remained the main surgical technique. And laparoscopy was performed only for diagnostic purposes and verification of the final diagnosis of the disease. Moreover, exactly half of the deceased patients had peritonitis. And here it should be noted that peritonitis was one of the frequent complications of pancreatic necrosis. Phlegmon of the retroperitoneal space was in 2nd place (34.0%) after peritonitis. This type of complication of pancreatic necrosis was detected at various times from the onset of the disease, on average 7.2±3.8 days. Damage to the right half of the retroperitoneal space was noted by us in 24.2% of patients, the left half - in 63.6% of patients, and total - in 12.1% of patients. Moreover, in 28.9% of patients, lesions of the retroperitoneal space were determined only by infiltration without signs of suppuration at the time of intraoperative verification. However, during repeated surgery, pancreatic abscesses were diagnosed in 11.3% of patients. The nature of complications characterizing the generalization of the purulent-inflammatory process in patients with different phases of pancreatic necrosis was unusual (Table 1).
|
|
|
4. Conclusions
- 1. Analysis of the results of traditional methods of treating pancreatic necrosis complicated by sepsis showed a high level of disease complications of 38.1% and mortality of 30.9%.2. The high percentage of complications and mortality is due to the lack of objective criteria for predicting the development of pancreatogenic sepsis and multiple organ dysfunction syndrome, which requires detailed studies of the pathogenetic mechanisms of this terrible disease.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML