D. G. Buribayev, D. B. Tulyaganov, Kh. E. Anvarov, A. O. Kurbanov
Republican Research Center of Emergency Medicine, Tashkent Regional Branch of the Republican Ambulance Service, Tashkent, Uzbekistan
Copyright © 2023 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Abstract
The aim of the study was to improve the treatment results of acute abdominal surgical diseases during the COVID-19 pandemic. The article is devoted to the analysis of providing emergency surgical care to patients at a multidisciplinary specialized infectious hospital, repurposed for the treatment of patients with a new coronavirus infection. A similar period outside of work in the conditions of COVID-19 was taken as a comparison period. Attention was paid to the increase of thrombosis and pneumonia cases.
Keywords:
COVID-19, New coronavirus infection, Diagnostics of COVID-19, Thrombosis, Pneumonia SARS-CoV-2
Cite this paper: D. G. Buribayev, D. B. Tulyaganov, Kh. E. Anvarov, A. O. Kurbanov, Clinical Evaluation of Acute Abdominal Surgical Diseases During the COVID-19 Pandemic, American Journal of Medicine and Medical Sciences, Vol. 13 No. 8, 2023, pp. 1078-1084. doi: 10.5923/j.ajmms.20231308.10.
1. Introduction
A new coronavirus infection caused by the SARS-CoV-2 virus has become a serious problem worldwide. The total number of infected people on the planet during the pandemic period was more than 500 million. The number of deaths as of March 2022 exceeded 6 million people in the world. For comparison, up to 650,000 people worldwide die from the flu every year [1]. These figures continued to grow every day; the peak of the epidemic lasted for a long time [2]. The presence of a new coronavirus infection seriously complicated the course of any diseases and led to high mortality in providing emergency surgical care [3-4].A special role in the pathogenesis of the new COVID-19 coronavirus infection, especially in severe cases, is played by an excessive response of the immune system with a massive release of cytokines — a "cytokine storm", which determines the occurrence and progression of acute respiratory distress syndrome (ARDS) [5-7].The clinical development of interstitial pneumonia at COVID-19 proceeds in three phases. The first phase, or the phase of early infection, occurs after the transmission of viral agents into upper respiratory tract (URT) epithelial cells and type 2 pneumocytes [8-9]. The duration of this phase, as a rule, does not exceed 5 days [10]. The second phase, or pulmonary, is characterized by the direct cytopathic effect of the SARS-CoV-2 virus on type 2 pneumocytes and endotheliocytes of pulmonary vessels, which promotes injury of the alveolar basement membrane and activation of target cells apoptosis [10]. Since the pulmonary phase is characterized by inadequate activation of innate immunity, as the synthesis of biologically active peptides increases the transmission of viral agents through the aerogematic barrier, viremia is developed [11]. The disease passes into the third phase, or the phase of hyperinflammation. The hyperinflammation phase, as a rule, occurs on the 9th-12th day after the appearance of the first clinical symptoms and is characterized by systemic hyperproduction of cytokines: IL-6, IL-1, IL-8, IL-17, TNF-α [8]. Systemic endothelial dysfunction and microvascular hypercoagulation is ddeveloped as a result of the "cytokine storm". Clinically, this phase is manifested by the development of ARDS, septic shock, multiple organ failure, disseminated intravascular coagulation, secondary bacterial infections [7].
2. Material and Methods
The present study was retrospective, based on the analysis of the medical histories of patients hospitalized with clinical manifestations of acute abdominal pathology which was developed against the background of COVID-19 for the period from the beginning of the announcement of the pandemic (March 2020) to July 2022. The object of the study was 200 patients who were randomized into 2 groups: the main group (n=100) with a preliminary diagnosis of acute abdominal surgical pathology and background disease - COVID-19; the control group (n=100) of patients admitted with acute abdominal surgical pathology without background COVID-19. The diagnosis of COVID-19 was verified by a positive COVID-19 PCR test and/or the detection of signs of interstitial pneumonia according to imaging research methods (MSCT and chest radiography). Hospitalized patients in the main group were performed the following emergency surgeries: appendectomy in 35 cases, in one case with laparotomic access. Laparotomy, suturing of a perforated stomach ulcer for a perforated stomach ulcer were performed in 4 cases. Suturing of perforated duodenal ulcers was performed in 8 cases. In one case, resection of the stomach was performed according to Billroth-2 against the background of diffuse peritonitis, in 1 case - duodenotomy with pyloroplasty according to Heineke-Mikulich. Cholecystectomy was performed in 13 cases. 8 cases of operations for acute intestinal obstruction, including those with adhesiolysis, in 7 cases with resection of the small intestine. In 11 cases, an abdominal hematoma was opened. In 8 cases, diagnostic laparotomy, sanitation and drainage of the abdominal cavity were performed for free fluid in the abdominal cavity. In 8 cases, herniolaporotomy was performed, in one case - removal of an ovarian cyst.All the data obtained in the study were entered into the summary tables of the Excell editor for Windows 2007. The arithmetic mean and standard deviation were calculated as the characteristics of the group for parametric data under the condition of a normal distribution. Intergroup comparison was based on Student's t test measurement. The differences were considered reliable when the probability of difference was more than 95% (p<0.05). In the case of a distribution different from normal, the median, minimum and maximum values were calculated. The frequency of occurrence of signs in the group was determined for nonparametric values. Intergroup differences were determined using the tabular chi-square test with an assessment of its reliability according to the tables depending on the number of freedom degrees. The ratio of men and women in the main group was 1:1.1; in the control group - 1.32:1.
3. Results
All patients of the main group were evaluated for the severity of COVID-19 associated pneumonia and the severity of respiratory failure. The vast majority of patients (72%) had no signs of respiratory failure during hospitalization in the surgical department, acute respiratory failure (ARF) of the I and II degrees was less frequent (n=11 and n=14, respectively). ARF III was diagnosed only in 3 patients (Figure 1).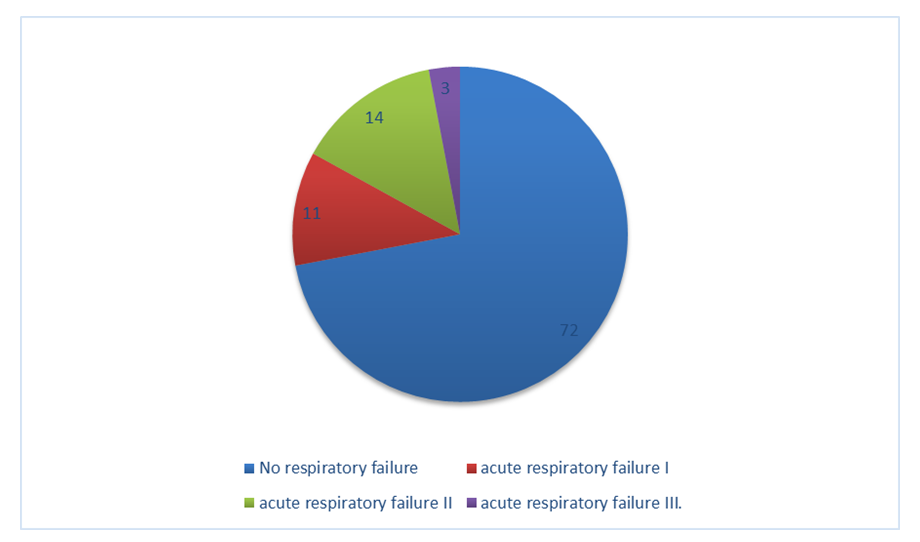 | Figure 1. Distribution of patients of the Main group according to the severity of respiratory failure |
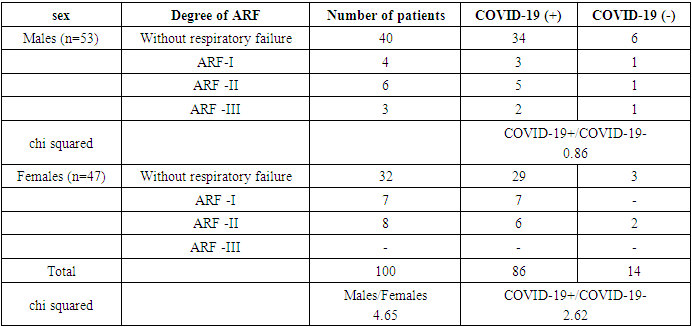
The distribution of patients according to the severity of ARF did not differ among men and women (chi square = 4.65), as well as among patients with positive and negative COVID-19 PCR (chi squared=1.93). The distribution of patients by sex and the result of PCR COVID-19 also did not reveal significant differences in the frequency of occurrence of ARF various degrees (Table 1). Table 1. Distribution of patients of the main group according to the degree of ARF depending on sex and the result of PCR COVID-19
 |
| |
|
Chest MSCT was performed in all patients, radiography was performed in 71 patients. According to imaging methods, pneumonia was detected in 29% of patients using MSCT and in 42% of patients using radiography. Thus, the sensitivity of both methods was comparable (chi squared=3.22) (Figure 2).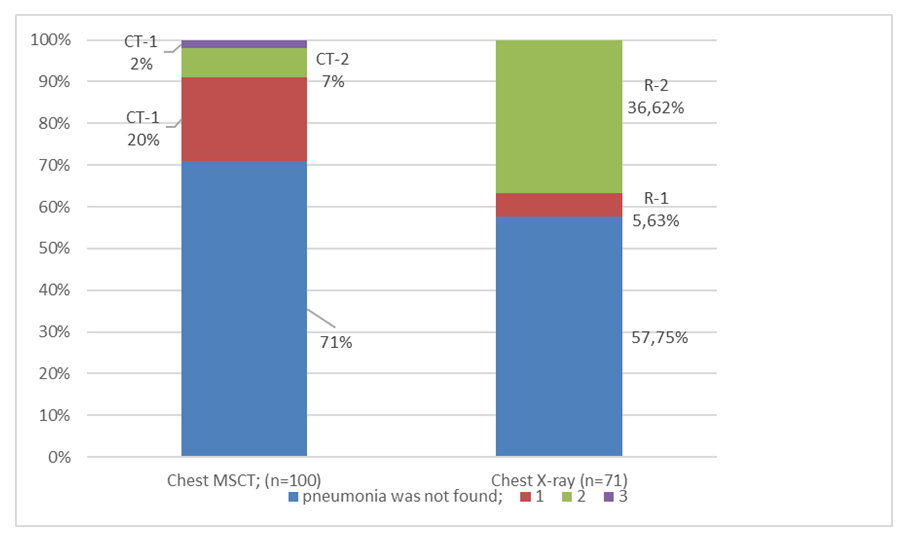 | Figure 2. Comparison of chest examination visual methods results in patients of the Main group |
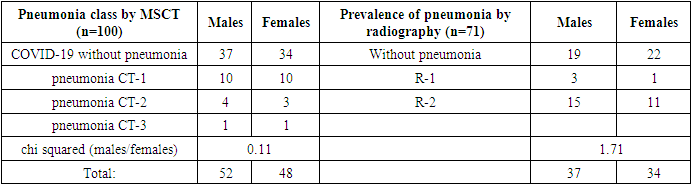
However, the isolation of patients with more widespread lung parenchymal lesions (CT2-3 and R-2 according to MSCT and chest X-ray, respectively) showed that more widespread lung parenchymal lesions were detected radiographically more often (9% and 36.62%, respectively, chi squared=19.46, p<0.001). This is probably due to the limited ability of plain radiography to visualize small lesions, which leads to a decrease in the sensitivity of plain radiography in the aspect of detecting non-spread lesions.The detectability of interstitial pneumonia of various degrees did not differ among males and females, both according to MSCT data and according to radiography (Table 2).Table 2. The frequency of detection of interstitial pneumonia of various degrees according to the results of MSCT and radiography among males and females
 |
| |
|
Patients of the main group were admitted to the surgical department during various periods of COVID-19. The time from the appearance of the first symptoms of COVID-19 was 3.75±1.80 days on average. 57 patients had abdominal pain due to symptoms of COVID-19; in 29 patients COVID-19 was diagnosed against the background of the absence of an obvious clinical picture using PCR; in 14 patients clinical manifestations of infection and acute surgical pathology appeared simultaneously (Figure 3).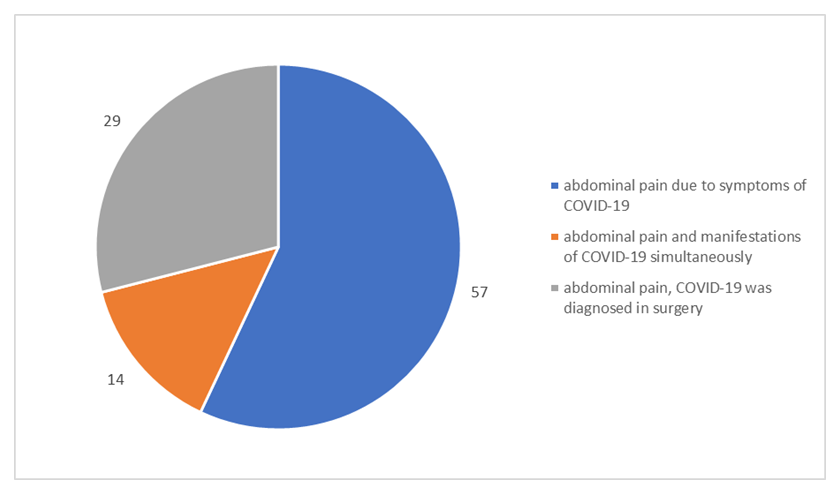 | Figure 3. Distribution of patients of the main group in relation to the time of admission to the surgical hospital and the time of COVID-19 symptoms occurrence |
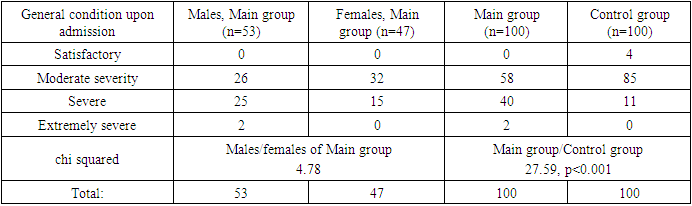
Comparative analysis showed that patients of the Main group were admitted to the surgical department at a significantly later date from the onset of abdominal pain compared with patients of the Control group (2.77±1.30 days versus 1.01±0.87 days, p<0.001). It is probably due to the fact that the clinical manifestations of COVID-19 mask the clinical manifestations of acute abdominal surgical pathology. Another explanation was the heavy burden on the healthcare system, which made it difficult to call and arrive an ambulance in a timely manner, as well as the introduced quarantine regime, which made it difficult to go to a surgical hospital on your own.Upon admission to the surgical hospital in 58 patients of the main group, the condition was estimated as moderate, in 40 patients – as severe and in 2 - extremely severe, while the severity of the condition did not differ in males and females (chi squared=4.78) (Table 3). Table 3. Evaluation of the clinical condition of the Main group patients upon admission to a surgical hospital, depending on sex
 |
| |
|
Saturation averaged 90.41 ± 4.90%, while in 40 patients it did not exceed 90%. In the main group, the condition of patients was evaluated as more severe than in the control group, due to the presence of background COVID-19. The severity of the patients' condition could be due to the activity of systemic inflammation or organ failure. COVID-19 is associated with active systemic inflammation to the extent of a "cytokine storm", as well as the development of acute respiratory failure and a violation of the hemocoagulation system by the type of DIC-syndrome. Therefore, the presence of COVID-19 significantly aggravates the general condition of patients admitted due to surgical pathology.Physical examination of the abdomen upon admission to the surgical hospital in 7 patients of the Main group and 2 patients of the Control group revealed no signs of irritation of the peritoneum (according to the description "the abdomen is soft, painless on palpation in all parts", chi squared = 3.03). The rest of the patients had tension in the abdominal muscles - diffusely or locally, positive symptoms of peritoneal irritation, pain on deep palpation of the abdomen locally, inaccessibility of deep palpation.Upon admission to the surgical hospital, BP in the Main group was significantly lower, and the pulse was significantly higher than in the Control group. This was probably due to a more pronounced systemic inflammatory reaction against COVID-19, associated with activation of neutrophilic NO-synthase, peripheral vasodilation and reactive tachycardia. In addition, tachycardia is explained by the redistribution of iron and the use of iron in inflammatory effector cells for the synthesis of matrix metalloproteinases, which reduces the availability of iron for erythrocytes, myoglobin and cytochromes, reduces the efficiency of cardiomyocytes and the efficiency of cardiac output (Figure 4). 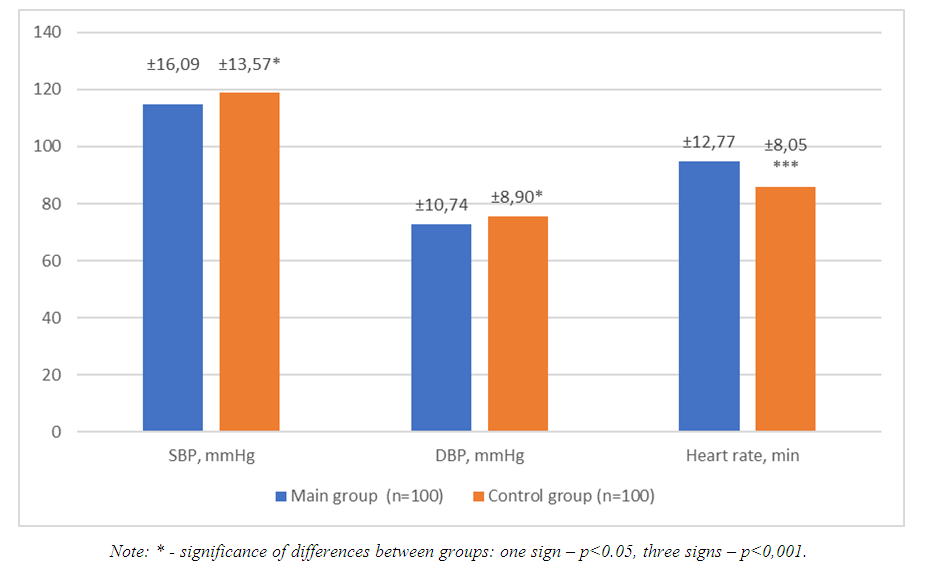 | Figure 4. Hemodynamic features of the study groups |
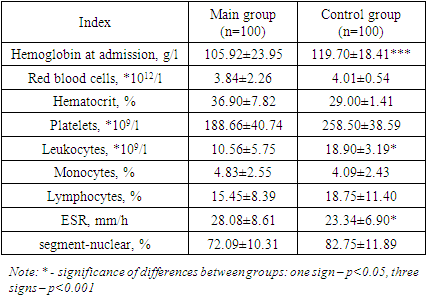
Laboratory data obtained upon admission to the surgical department revealed the following patterns: in the Main group of patients, compared with the Control group, the hemoglobin level of peripheral venous blood was significantly reduced (p<0.001), with a comparable concentration of erythrocytes and hematocrit level. This indicates the development of hypochromic anemia in patients whose acute surgical pathology was developed against the background of COVID-19. Pathogenetically hypochromic anemia in COVID-19 patients may have a redistributive character: the use of iron depot for the synthesis of inflammatory enzymes, or to be associated with interleukin-induced hyperexpression of hepcidin binding ferroportin with impaired iron transport from enterocytes. The concentration of platelets in peripheral venous blood in the representatives of the Main group was lower than in the Control one, without achieving statistical significance, although it remained within the reference norm (180-320*109/l). The reason for the differences may be excessive consumption of platelets due to endothelial dysfunction and platelet activation with the development of intravascular thrombosis, which is characteristic of the clinical course of COVID-19. The concentration of leukocytes in both groups of patients included in the study was increased relative to the reference norm (4-9*109/l), which is associated with the activation of a non-specific link of immunity characteristic of acute purulent process. This fact was confirmed not only by lymphocytosis, but also by a shift of the leukocyte formula to the left and relative lymphocytosis (without statistical reliability). The increase in leukocyte concentration was significantly less pronounced in the Main group, than in the Control group (p<0.05), which is a characteristic phenomenon for COVID-19 and is more associated with absolute lymphopenia. ESR was increased in both groups of patients to a greater extent in patients of the main group, reflecting severe systemic inflammation (p<0.05) (Table 4).Table 4. Complete blood count in patients depending on the presence of background COVID-19
 |
| |
|
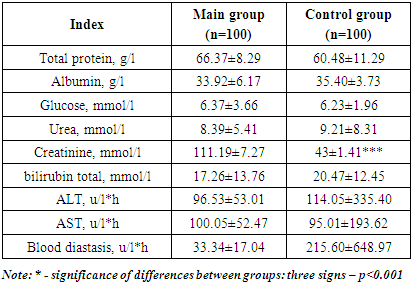
Biochemical blood analysis revealed an increase in blood creatinine concentration in the patients of the Main group, which may be associated with acute kidney injury against the background of hemorheological disorders characteristic of COVID-19 (the reliability of the difference with the Control group is p<0.001). Also, increased transaminase activity in peripheral blood serum was found in both groups of patients, comparable in both study groups (Table 5).Table 5. Биохимический анализ крови у больных с острой абдоминальной хирургической патологией в зависимости от наличия фоновой COVID-19
 |
| |
|
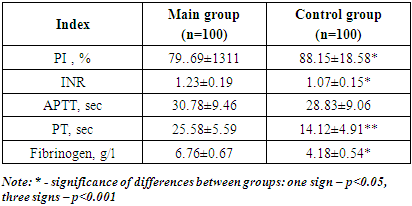
Comparison of the results of the coagulogram in the main and control groups revealed a significantly lower prothrombin time in the main group (p<0.01), as well as a lower value of the prothrombin index and a higher value of the international normalized ratio (p<0.05). The concentration of fibrinogen in the Main group was significantly higher than in the Control group, which is a reflection of the activation of systemic inflammation characteristic of COVID-19 (Table 6).Table 6. Coagulogram in patients with acute abdominal surgical pathology depending on the presence of background COVID-19
 |
| |
|
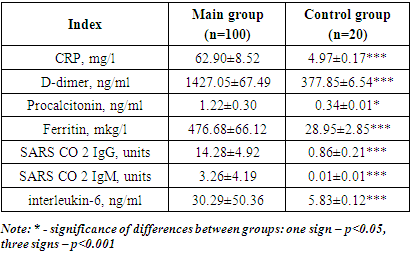
All patients of the main group, taking into account the pathogenetic features of COVID-19, were evaluated for the activity of systemic inflammation, the concentration of procalcitonin, D-dimer and antibodies to SARS CO 2 IgG and M. The results were compared with the results obtained in a group of 20 healthy volunteers who did not carry COVID-19 and were not vaccinated with COVID-19. The analysis confirmed the high activity of systemic inflammation, the markers of which were not only ERS, the concentration of leukocytes and fibrinogen, but also the concentration of C-reactive protein (CRP), ferritin and interleukin-6. Also, in patients included in the main study group, the concentration of D-dimer, which is a marker of intravascular thrombosis, and the concentration of procalcitonin, a marker of anti-infective protection, were increased. There was a high concentration of antibodies to the COVID-19 virus, characteristic of both the acute and long-term phases of infection in this group of patients (Table 7). Table 7. Comparative characteristics of the systemic inflammation activity, intravascular thrombosis and anti-infective response in patients of the Main group
 |
| |
|
4. Conclusions
Thus, our study showed that in the conditions of COVID-19, the admission of patients with acute abdominal surgical pathology to surgical departments was delayed. Patients whose acute abdominal surgical pathology was developed against the background of COVID-19 were characterized by a more severe clinical condition, impaired hemodynamics, the presence of signs of ARF, hypochromic anemia, thrombocytopenia, lower severity of leukocyte reaction and greater activity of systemic inflammatory reaction.The authors declare no conflict of interest. This study does not include the involvement of any budgetary, grant or other funds. The article is published for the first time and is part of a scientific work.
References
| [1] | Flu. Newsletter of the World Health Organization. (Electronic resource.) URL: https://www.who.int/ru/news-room/fact-sheets/detail/influenza- (seasonal) (access date: 16.10.2020) (in Russ.). |
| [2] | Online map of the spread of coronavirus. (Electronic resource.) URL: https://coronavirus-monitor.ru (аccess date: 16.10.2020) (in Russ.). |
| [3] | Gabriel S. A., Markov P. V., Durleshter V. M. et al. Intermediate results of treatment of patients with surgical pathology in a redesigne multidisciplinary hospital to provide care to patients with COVID-19 // Scientific Bulletin of Kuban Health. 2020; 3(69): 14–22. |
| [4] | Ionov S. N., Saidov S. S., Abanina O. V. et al. Coronavirus infection in obesity // Bulletin of the medical institute «REAVIZ»: rehabilitation, doctor and health. 2021; 3(51): 13–19. Doi: 10.20340 / vmirvz.2021.3.COVID.2. |
| [5] | Soy M., Keser G., Atagündüz P. et al. Cytokine storm in COVID-19: pathogenesis and overview of anti-inflammatory agents used in treatment. Clin Rheumatol. 2020; 39(7): 2085–2094. DOI: 10.1007/s10067-020-05190-5. |
| [6] | Hu B., Huang S., Yin L. The cytokine storm and COVID-19. J Med Virol. 2020; 10.1002/jmv.26232. DOI: 10.1002/jmv.26232. |
| [7] | Ragab D., Salah Eldin H., Taeimah M. et al. The COVID-19 Cytokine Storm; What We Know So Far. Front Immunol. 2020; 11: 1446. DOI: 10.3389/fimmu.2020.01446. |
| [8] | Robert J. Mason. Pathogenesis of COVID-19 from a cell biologic perspective. Eur Respir J. 2020 Apr 9: 2000607. doi: 10.1183/13993003.00607-2020 |
| [9] | Stefano Romagnoli, Adriano Peris, A. Raffaele De Gaudio et al. SARS-CoV-2 and COVID-19: From the Bench to the Bedside. Physiol Rev. 2020 Oct 1; 100(4): 1455–1466. doi: 10.1152/physrev.00020.2020. |
| [10] | Sumanth Khadke, Nayla Ahmed, Nausheen Ahmed et al. Harnessing the immune system to overcome cytokine storm and reduce viral load in COVID-19: a review of the phases of illness and therapeutic agents. Virol J. 2020; 17: 154. doi: 10.1186/s12985-020-01415-w. |
| [11] | Francois Henri Jacques and Erik Apedaile. Immunopathogenesis of COVID-19: Summary and Possible Interventions. Front Immunol. 2020; 11: 564925. doi: 10.3389/fimmu.2020.564925. |






 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML





