-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2023; 13(8): 1073-1077
doi:10.5923/j.ajmms.20231308.09
Received: Jul. 19, 2023; Accepted: Jul. 29, 2023; Published: Aug. 12, 2023

A Method of Pre-Pregnancy Preparation for Miscarriage in Women with a History of Undeveloped Pregnancy
Ruzimova S. B., Matyakubova S. A.
Urgench branch of Tashkent Medical Academy, Urgench, Uzbekistan
Correspondence to: Ruzimova S. B., Urgench branch of Tashkent Medical Academy, Urgench, Uzbekistan.
| Email: |  |
Copyright © 2023 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

The presence of a woman's history of undeveloped pregnancy (UP) negatively characterizes her reproductive function. The aim of the study was to evaluate the effectiveness of the proposed comprehensivep regravid preparation for the prevention of recurrent UP in women with a history of UP. The analysis of the data of clinical-anamnestic and laboratory-instrumental methods of examination of women with UP in the first trimester was carried out. Special research methods consisted in studying the level of d-dimer and procalcitonin in the blood of women with a history of UP. Pregravid preparation was based on compensation for somatic diseases and rehabilitation of genital and extragenital infections, as well as on the basis of established indicators of d-dimer and procalcitonin content. All patients were recommended to take Omega-3 PUFA. The modified pre-pregnancy preparation of women with a history of UP contributes to the restoration of a woman's reproductive function, a 7.9-fold decrease in the frequency of premature birth and a 4-fold decrease in the development of UP.
Keywords: Undeveloped pregnancy, Miscarriage, Pregravid preparation, Omega-3, D-dimer, Procalcitonin
Cite this paper: Ruzimova S. B., Matyakubova S. A., A Method of Pre-Pregnancy Preparation for Miscarriage in Women with a History of Undeveloped Pregnancy, American Journal of Medicine and Medical Sciences, Vol. 13 No. 8, 2023, pp. 1073-1077. doi: 10.5923/j.ajmms.20231308.09.
Article Outline
1. Relevance
- Nowadays miscarriage is one of the urgent problems in obstetrics. Undeveloped pregnancy (UP) is an integral part of fetal loss syndrome and is one of the pathogenetic variants of miscarriage [7,1,10]. In the structure of reproductive losses, the share of UP is 10-20%, and among spontaneous termination of pregnancy in the first trimester – 45-88% [1].According to many authors, half of spontaneous abortions occur in the first trimester, and 25% of them are habitual miscarriage. The total frequency of undeveloped pregnancies reaches 10-15% of all pregnancies [2,4].The presence of a woman's history of UP negatively characterizes her reproductive function. In the absence of rehabilitation and pregravid preparation, repeated pregnancy loss occurs in every second case, and in 27.4% of cases there are three or more episodes of miscarriage [5,9]. Currently, the genesis of non-developing pregnancy, as well as all reproductive losses, is considered from a multifactorial perspective [2,3,4,5,8].Polyethologicity of miscarriage and its high value in reproductive losses requires the need for a differentiated approach in the pregravid period of preparation for subsequent pregnancy, and, in particular, to patients with two or more undeveloped pregnancies [8].The achievements of medicine in recent years are associated with the introduction into practice of effective and safe methods of treatment, the results of which have been confirmed in serious multicenter clinical studies. In the arsenal of obstetricians and gynecologists, medications of highly purified Omega-3 polyunsaturated fatty acids (PUFA) are becoming increasingly popular. The use of omega-3-PUFA preparations in the pregravid period due to a wide range of its pharmacological effects (anti-inflammatory, antiplatelet, etc.) will contribute to the elimination of chronic inflammatory processes, normalization of immune and endocrine dysfunction, as well as improvement of platelet aggregation ability and stabilization of hemostasis at the onset of planned pregnancy [7,9]. A wide range of clinical and pharmacological effects and the high safety of Omega-3 PUFA makes it possible to effectively use them in pregravid preparation in women with a history of UP. Evidence-based medicine data confirm the expediency of using standardized forms of omega-3 PUFA as part of complex therapy (in particular, with aspirin) for the prevention of spontaneous termination of pregnancy [7].The main functions of PUFA are their participation in the formation of phospholipids of cell membranes and the synthesis of eicosanoids (biologically active substances - tissue hormones): prostacyclines, prostaglandins, leukotrienes and thromboxanes. These substances play an active role in regulating the functions of the entire body, especially the cardiovascular system [6].Omega-3 PUFA-eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) play an important role in ensuring the vital activity of the human body. Omega-3 PUFAs form an adequate response of the body's cells to the action of external pathogenic factors, regulate lipid metabolism, prevent the development of inflammation, the formation of blood clots, cardiac arrhythmias [1,3,4,5].Omega-3 PUFA provides synthesis of tissue hormones, so-called eicosanoids (prostaglandins, prostacyclines, thromboxanes, leukotrienes), regulating local cellular and tissue functions, including inflammatory reactions, functioning of platelets, leukocytes and erythrocytes, vasoconstriction and dilation, etc. [6,10]Normally, with sufficient intake of Omega-3 PUFA into the human body, they displace arachidonic acid (AC) and enter into competitive replacement of AC in phospholipids of cell membranes in the cyclooxygenase and lipoxygenase pathways of metabolism [7].Various functional properties have also been identified with respect to thromboxanes. It has been shown that thromboxane 3 is synthesized from Omega-3 PUFA, which has a pronounced antiaggregational effect [9,10].
2. The Purpose of the Study
- To evaluate the effectiveness of the proposed complex medicamentous pregravid preparation in order to prevent repeated undeveloped pregnancies in women with a history of UP.
3. Materials and Methods of Research
- The study included 72 women with UP in the first trimester of pregnancy. The analysis was carried out by a prospective method in the gynecological department of the Regional Perinatal Center of the Khorezm region in the period from 2021-2022. The age of women ranged from 19 to 44 years, the average age was 28.3 ±0.7 years.The analysis of the data of clinical-anamnestic and laboratory-instrumental methods of examination of women with UP in the first trimester, depending on the frequency of occurrence, was carried out.The diagnosis of UP was established on the basis of ultrasound examination. As a result, 2 types of UP are diagnosed: anembryonia (type I and II) and fetal death.During visualization, there was a lack of motor activity and heart contractions, as well as a discrepancy between the size of the embryo and the term of the expected pregnancy, depending on the last date of menstruation, which was the criteria for the diagnosis of UP.Among the examined women, the incidence of UP in the anamnesis ranged from 1 to 10 cases, the average number of 1.7 ± 0.03 cases. UP up to 6 weeks was observed in the main group in 15.3% of cases (11 out of 72). In other cases, H.B. developed in later terms up to 12 weeks of gestation (Figure 1).
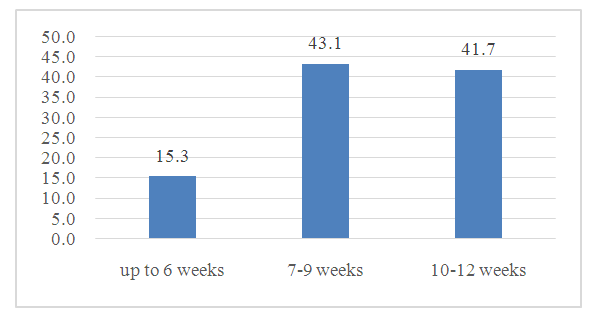 | Figure 1. Gestation periods in the development of UP |
|
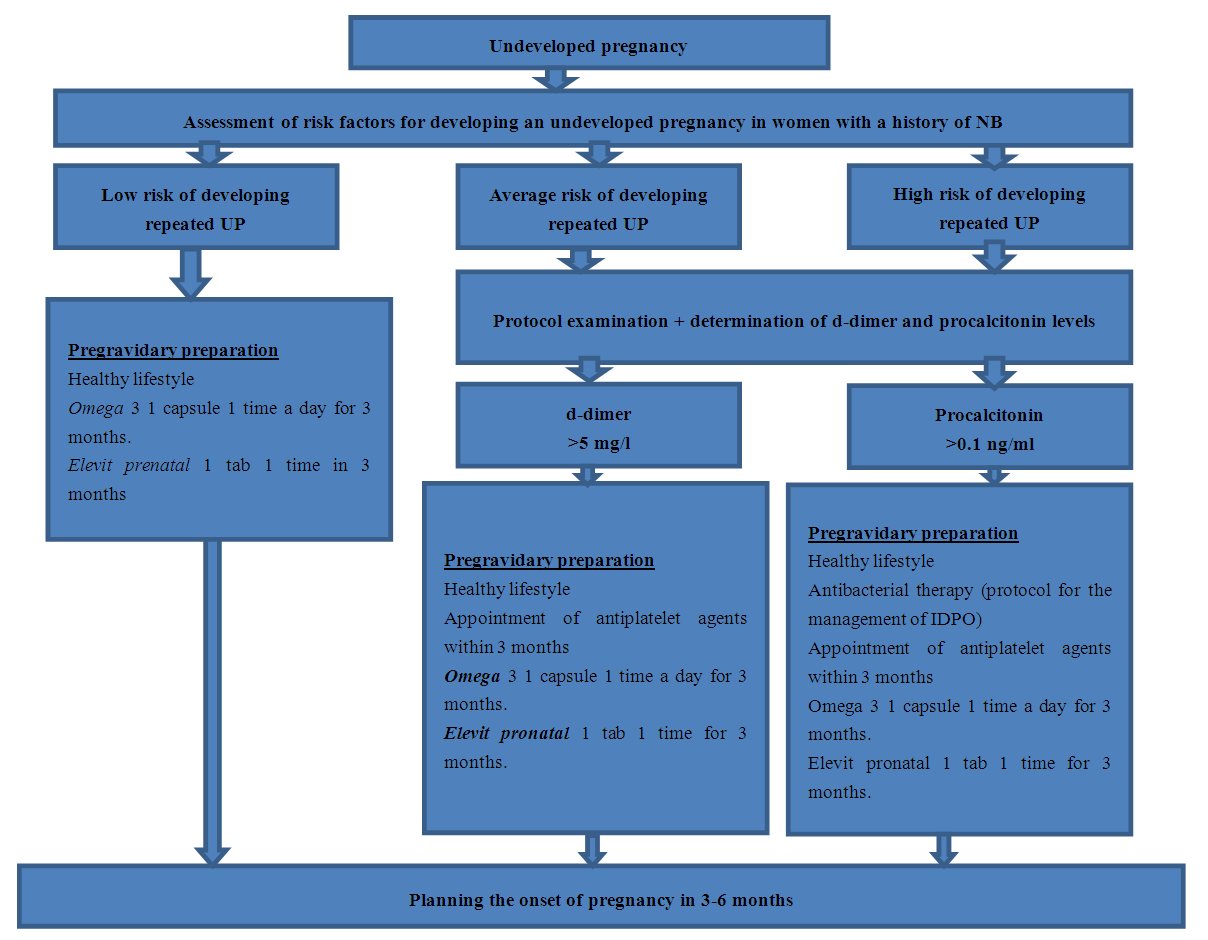 | Figure 2. Algorithm of pregravid preparation of women with UP in anamnesis |
4. Research Results
- Clinically, UP was manifested in 36.1% of cases (26 women), in other cases it was absent. Among the symptoms of UP, spotting discharge from the genital tract, moderate abdominal pain, disappearance of the present signs of pregnancy such as nausea or vomiting, breast swelling were noted.In 61 women (84.7%) with UP, a delay of the deceased fetus was recorded for more than 2 weeks, which was manifested by a characteristic pattern on ultrasound in the form of a delay in embryo development and a lag in its size from the calendar gestation period.During the survey, it was found that 39 women with a history of UP had a low risk of developing UP in subsequent pregnancies, which was 54.2%. The average score scored in this cohort was 3.8± 0.02 points; 16 women with an average score of 8.6± 0.06 formed a group with an average risk of development (22.2%); 17 women scored an average of 18.5± 0.1 points, which indicated a high risk of developing UP in subsequent pregnancies (23.6%).During bacterial seeding among women with a history of UP, conditionally pathogenic microflora (43/72) was sown from the cervical canal in 59.7% of cases, among which Escherichia coli in 38 (52.1%), Enterococcus faecalis in 26 (35.6%), Staphylococcus hemolyticus in 8 (11.0%), as well as other bacterial flora.Baseline hemoglobin values in women with a history of UP were significantly lower than in the control group (108.9±1.31 g/l versus 118.2±1.28 g/l; P<0.05).Analysis of the coagulogram data showed unreliable fluctuations in the fibrinogen level from 2.1 to 4.2 g/l, however, the average values corresponded to those of the control group (P>0.05).A similar pattern was observed with the platelet count in the women of the main group, although there was a tendency to decrease them, so the average level was -209.9± in the main group 3,2x109/l, and in the comparison group – 212.4 ±3.12 x109/l (P>0.05).There was a significantly high level of D-dimer in the women of the main group in relation to the indicators in the control group, which in the main group averaged 1.35±0.29 micrograms/ml (P<0.05). An increase in the level of D-dimer in peripheral blood in women with UP is associated with the activation of fibrinolytic activity. Procalcitonin indices in pregnant women with UP exceeded the reference values (0.05-0.1 ng/ml), which indicates the development of local inflammation, so in the main group this indicator averaged 0.33±0.03 ng/ml, in pregnant women with a normal pregnancy, the average procalcitonin indices were 0.23±0.03 ng/ml (P<0.05).Depending on the proposed algorithm, 50 women with a history of UP underwent individual pregravid preparation.The onset of pregnancy in the first six months after the completion of pregravidar therapy occurred in the vast majority of patients, namely in 31 (43.1%) of 50 women in the main group, in the comparison group in 7 (31.8%) of 22 women after UP. The reliability of the data on the frequency of pregnancies in the period from 3 to 6 months has not been established, but the tendency to increase the frequency in the main group is very noticeable. Reliable data were obtained in the period from 6 to 12 months after UP, so in the main group, pregnancy occurred in 96.0% of women from the main group (48 out of 50), while in the comparison group this frequency was 1.8 times lower and amounted to 54.5% (12 out of 22 women with a history of UP). The analysis of the course of pregnancy and its outcomes was carried out in 48 women from the main group and in 12 from the comparison group.45 pregnant women (93.8%) from the main group carried pregnancy up to 37+6-40 weeks. These women gave birth to full-term viable children. In the comparison group, urgent labor was observed in 8 women (66.7%), which is 1.4 times less. Premature births were registered in 1 (2.1%) women from the main group and in 2 women from the comparison group (16.7), which is 7.9 times higher (P<0.001).In 2 women (4.2%) of the main group, UP developed before 12 weeks of gestation, in the comparison group, this pathology was noted in 16.6%, which is almost 4 times more often (p<0.01). At the same time, I would like to note that all women on the basis of the questionnaire developed by us were in a high-risk group for the development of UP.Thus, the proposed pre-gravidar training of women with a history of UP significantly improves the reproductive function of women, while reducing the frequency of reproductive losses and perinatal mortality.
5. Conclusions
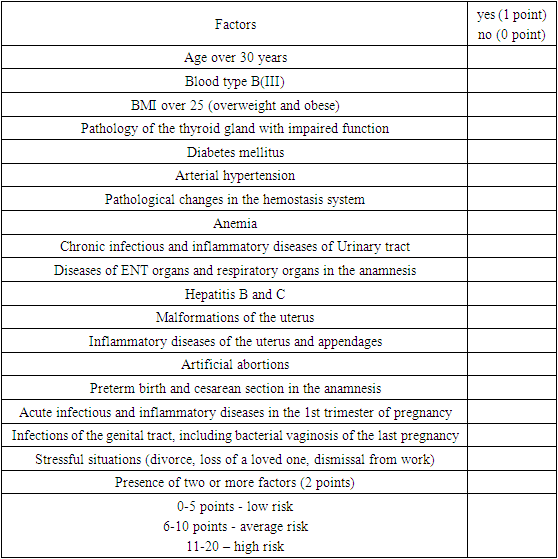
- 1. Among women with a history of UP, according to the developed questionnaire, 54.2% have a low risk, 22.2% have an average risk, and 23.6% have a high risk of developing UP.2. A significantly high content of the D-dimer level was found in the women of the main group in relation to the indicators in the control group, which in the main group averaged 1.35±0.29 micrograms/ml (P<0.05). An increase in the level of D-dimer in peripheral blood in women with UP is associated with the activation of fibrinolytic activity.3. Procalcitonin indices in pregnant women with NB exceeded the reference values (0.05-0.1 ng/ml), which indicates the development of local inflammation, so in the main group this indicator averaged 0.33±0.03 ng/ml, in pregnant women with a normal pregnancy, the average procalcitonin indices were 0.23±0.03 ng/ml (P<0.05).4. Carrying out modified pregravid training for women with a history of UP contributes to the restoration of a woman's reproductive function, reducing the frequency of premature birth by 7.9 times and the development of an undeveloped pregnancy by 4 times.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML