-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2023; 13(7): 889-891
doi:10.5923/j.ajmms.20231307.08
Received: May 29, 2023; Accepted: Jun. 20, 2023; Published: Jul. 8, 2023

Clinical Value of Echocariography Criteria of Pulmonary Hypertension Crisis in the Early Postoperative Period after Correction of Pediatric Congenital Heart Defects
Ra’no Rakhimova1, Nodirjon Zokirov2, Bobur Shukurov3
1Head of the Department of Ultrasound Diagnostics at Republican Research Center for Emergency Medicine, Uzbekistan
2Cardiologist and Functional Diagnostics at Multidisciplinary Medical Center AKFA Medline, PhD Researcher, Republican Research Center for Emergency Medicine, Uzbekistan
3Senior Researcher, Emergency Surgery Department of the Republican Scientific Center of Emergency Medicine, Uzbekistan
Correspondence to: Nodirjon Zokirov, Cardiologist and Functional Diagnostics at Multidisciplinary Medical Center AKFA Medline, PhD Researcher, Republican Research Center for Emergency Medicine, Uzbekistan.
| Email: |  |
Copyright © 2023 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Study of the pathophysiological response of the heart and echocardiography evaluation of the right ventricle at the beginning and after targeted therapy in pulmonary hypertensive crisis after correction of congenital heart defects. An echocardiography examination was performed in 30 children with a pulmonary hypertensive crisis (PHC) after correction of congenital heart defects in the early postoperative period at the multidisciplinary medical center AKFA Medline. As the main two-dimensional echocardiography parameters for assessing PHC, the diameter of the right atrium and inferior vena cava, the ratio of RV/LV from the parasternal short axis view of the right and left ventricles at the level of papillary muscles, systolic pulmonary artery pressure, measurement of left ventricular end diastolic volume according to the Teicholz method from the parasternal long axis view and systolic excursion of the tricuspid annular plane were obtained. The diameter of the right atrium ranged from 44.76x26.32 mm to 53.24x37.65 mm, on average 48.43x32.54 mm, +3 in 13 children and +3.5 in 17 children according to Z-score. The diameter of the IVC was 2.3 cm in 11 children and 2.5 cm in 19 children, on average 2.4 cm, and the pressure in the right atrium was from 15 mm Hg. up to 22 mm Hg, on average 18.5 mm Hg. The RV/LV ratio figures were >1.3 in 22 patients and >1.5 in 8 children, respectively. In our study, TAPSE was 7 mm to 8.5 mm in 15 children (>-2.5 Z-score), 8 to 10 mm in 12 patients (>-2 Z-score), and 6-6.5 mm in 3 patients (>-3 according to Z-score). Echocardiography provides an indirect measurement of pulmonary artery pressure, which may help in the initial evaluation and follow-up of patients with a pulmonary hypertension crisis after correction of congenital heart defects.
Keywords: Pulmonary hypertensive crisis, Echocardiography, TAPSE, Congenital heart defect
Cite this paper: Ra’no Rakhimova, Nodirjon Zokirov, Bobur Shukurov, Clinical Value of Echocariography Criteria of Pulmonary Hypertension Crisis in the Early Postoperative Period after Correction of Pediatric Congenital Heart Defects, American Journal of Medicine and Medical Sciences, Vol. 13 No. 7, 2023, pp. 889-891. doi: 10.5923/j.ajmms.20231307.08.
1. Introduction
- Pulmonary arterial hypertension (PAH) is a progressive pulmonary vascular disease characterized by elevated mean pulmonary artery pressure (MPAP) and pulmonary vascular resistance (PVR), which ultimately leads to right ventricular failure and death. A simple definition of PAH, which is MPAP greater than or equal to 25 mmHg. at rest, belies the complexity of the underlying pathophysiology. In the intensive care setting, especially in patients with congenital heart disease (CHD), pulmonary vascular disease can complicate the clinical course, even if resting MPAP does not meet the definition of PH [1]. Compared to adults, children with PAH have a different etiology of the disease, including idiopathic PAH and CHD-related PAH. Cause of accurate diagnosis and modern methods of management PAH, the prognosis of children with PAH has improved over the past decades. However, children with PAH still face great challenges in early diagnosis, risk stratification, and effective treatment. [2]. Awareness of the importance of right ventricular function in PAH has increased significantly as it determines the functional state, exercise tolerance and disease outcome in patients. Non-invasive imaging modalities such as echocardiography and cardiac magnetic resonance imaging (MRI) are of paramount importance in the assessment of the right heart function. Given the wide availability and low cost, echocardiography is attractive to both patients with PAH and their physicians. According to the latest European Society of Cardiology guidelines, the usefulness of echocardiography has been limited by two echocardiographic parameters, right atrial end-systolic area and the presence of pericardial effusion, that have been included in routine risk assessment in patients with PAH. However, many echocardiographic measures have been reported to have prognostic value and are increasingly included in clinical practice; however, it is still not clear what precise echocardiographic parameters are required to assess maladaptation and pulmonary hypertension crisis (PHC) and therefore no specific recommendations exist. This raises the interesting question of which aspects of heart function as assessed by echocardiography should be routinely used as parameters in assessing risk in patients with PHC at baseline and during follow-up. [3].The purpose of the trial: Study of the pathophysiological response of the heart and echocardiography evaluation of the right ventricle at the beginning and after targeted therapy in pulmonary hypertensive crisis after correction of congenital heart defects.
2. Materials and Methods
- An echocardiography examination was conducted in 30 children with PHC after CHD correction in the early postoperative period at the multidisciplinary medical center AKFA Medline. The age of the children ranged from 6 months to 1 year, 18 girls and 12 boys. Out of 30 children, 16 children after closure of a ventricular septal defect (VSD) with high PAH, 4 children with correction of total anomalous pulmonary venous drainage (TAPVR), 6 children with double outlet right ventricle (DORV), 3 children after correction of the complete AV canal defect (CAVC) and 1 child after correction of coarctation of the aorta (CoA) with patent ductus arteriosus (PDA) (Diagram 1). Siemens Acuson 2000 Doppler ultrasound with a 2.0-5.0 MHz transducer was used as a diagnostic tool. As the main two-dimensional echocardiographic parameters for assessing PHC, the diameter of the right atrium and inferior vena cava, the ratio of RV/LV from the parasternal short axis view of the right and left ventricles at the level of papillary muscles, systolic pulmonary artery pressure (SPAP), measurement of left ventricular end-diastolic volume (LV EDV) according to the Teicholz method from the parasternal long axis view and tricuspid annular plane systolic excursion (TAPSE). We examined the size of the right atrium (RA) according to the Z-score ranges, which were measured from the apical four chamber view. Increased RA variables > +3 with a Z-score were considered a high probability of PHC. The diameter of the inferior vena cava (IVC) was measured in the subcostal longitudinal view at the confluence of the IVC into the RA. RA pressure can be assessed by the diameter of the IVC and the presence of inspiratory collapse. IVC diameter ≤2.1 cm, collapse > 50% on breathing suggests a normal RA pressure of 3 mmHg. (range 0–5 mmHg). An IVC diameter ≥ 2.1 cm that collapses to <50% on inspiration suggests a high RA pressure of 15 mmHg. (range 10–20 mmHg) and probably a sign of PHC. TAPSE involves taking an apical four-chamber view, placing an M-mode line on the lateral annulus of the tricuspid valve (where the valve leaflet attaches to the wall of the RV), obtaining an M-mode that tracks and measures the height of the annulus movement during systole. TAPSE more than -2.5 on Z-score and SPAP more than 55 mm Hg. can be assessed as a patient with PHC. The end-systolic RV/LV ratio which measured at the papillary muscle level from parasternal short axis view includes RV size and correlates with invasive hemodynamic parameters, and RV/LV end-systolic ratio >1 is associated with PHC in children.
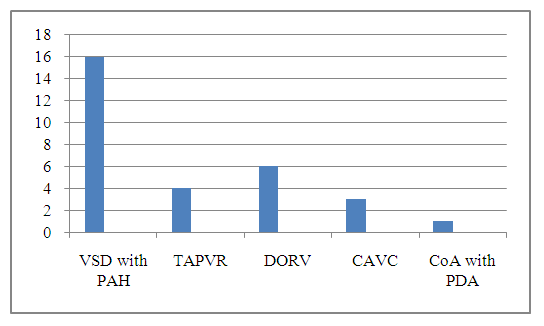 | Diagramme 1 |
3. Results
- Our results showed that the diameter of the RA ranged from 44.76x26.32 mm to 53.24x37.65 mm, on average 48.43x32.54 mm, +3 in 13 children and +3.5 in 17 children according to Z-score. The diameter of the IVC was 2.3 cm in 11 children and 2.5 cm in 19 children, on average 2.4 cm, and the pressure in the RA was from 15 mm Hg. up to 22 mm Hg, on average 18.5 mm Hg. The RV/LV ratio figures were >1.3 in 22 patients and >1.5 in 8 children, respectively. According to our echocardiographic parameters, SPAP was from 57 mm Hg. up to 70 mm Hg in 12 patients and from 65-77 mm Hg. in 18 patients, which indicated the presence of PHC in the child. In our study, TAPSE was 7 mm to 8.5 mm in 15 children (> -2.5 Z-score), 8 to 10 mm in 12 patients (> -2 Z-score), and 6 - 6.5 mm in 3 patients (> -3 according to Z-score). According to our measurements, LV EDV decreased to 6-9 ml in 22 patients (> -2.5 Z-score) and from 8-11 ml in 8 children (> -1.7 Z-score), indicating serious violation of preload on the left ventricle, and indicates to the critical condition of the patient.
4. Discussion
- In our study, the clinical condition of patients correlates well with echocardiography, which is characterized by a sudden decrease in blood pressure, tachycardia with a pulse rate of more than 170, arrhythmias such as ventricular tachycardia, multiple atrial and ventricular extrasystoles (in 24 children), right and left bundle branch blocks, increased mean central venous pressure from 15 to 23 mm Hg, an increase the parameters of artificial lung ventilation, etc. The most critical echocardiographic parameters (RA diameter 53.24x37.65 mm, IVC diameter 2.5 cm, RA pressure 20-22 mm Hg) occurred in children after correction of DORV and CAVC. In children with CHD may develop PHC after surgical treatment. Factors that contribute to the development of postoperative PHC are not yet fully understood, however, endothelial cell dysfunction has been found to be a factor in the preoperative and postoperative periods. [4,5,6]. Inflammatory response to cardiopulmonary bypass and ischemic-reperfusion damage and its effect on heart and lung function contribute to an increase in PVR [7]. Pain, alert reactions in ventilated children, and tracheal discharge can trigger an acute, severe increase in PVR, manifesting as PHC, and potentially leading to cardiocirculatory collapse and death. Echocardiography is the most important tool for assessing ventricular function and RV-LV interaction. Doppler imaging of tricuspid and pulmonary valve regurgitation to characterize estimated RV pressure and biventricular diastolic inflow may assist in monitoring therapy in the intensive care unit. Estimated right ventricular pressure and SPAP must be interpreted in the context of the degree of RV dysfunction. Low pressure gradients across the tricuspid and pulmonary valves may be associated with RV failure; they should be considered in relation to other variables (eg, - TAPSE) and in the presence or absence of pericardial and pleural effusion or ascites. When pulmonary vein obstruction is excluded, in most cases, an increase in the size of the LA determines the postcapillary component of PH and may indicate the need for decompression of pressure in the LA by stenting the interatrial septum. Especially after cardiac surgery, it is necessary to determine and take into account the anatomical and hemodynamic status of the patient. [8]. Previous authors have reported that the ratio of RV diameter to LV diameter, which includes both pathologic septal shift and RV dilatation, is associated with poor outcomes in pediatric PAH. In our study, a higher RV/LV ratio was a statistically significant risk factor for developing PHC. [9,10]. Severe RV dilatation and secondary LV insufficiency play a fundamental role in the initial and progressive stages of PHC, while transthoracic echocardiography can be used to evaluate the effectiveness of emergency treatment.
5. Conclusions
- Echocardiography is a valuable noninvasive method for screening, diagnosing, and evaluating PHK in children. Echocardiography provides an indirect measurement of pulmonary artery pressure, which may help in the initial evaluation and follow-up of these patients. Echocardiographic assessment of RV function is important in this children and may be used for ongoing follow-up of these patients.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML