-
Paper Information
- Next Paper
- Previous Paper
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Medicine and Medical Sciences
p-ISSN: 2165-901X e-ISSN: 2165-9036
2023; 13(7): 883-888
doi:10.5923/j.ajmms.20231307.07
Received: Jun. 13, 2023; Accepted: Jul. 2, 2023; Published: Jul. 8, 2023

Features of the Clinical Course of COVID-19 Depending on the Presence of Arterial Hypertension
Tashkenbaeva Eleonora Negmatovna, Mukhiddinov Abdumalik Inoyatovich, Abdieva Gulnora Alievna, Ergashev Arslonbek, Ellamonov Sukhrobjon Numonovich
Department of Internal Diseases and Cardiology No2 of Samarkand State Medical University, Samarkand, Uzbekistan
Copyright © 2023 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

This analysis will not only more accurately determine the nature of the development of arterial hypertension, but will also help to identify the impact of 2019-nCoV infection on arterial hypertension (AH). Objective: to study features of the clinical course of COVID-19 depending on the presence of arterial hypertension. The object of the study was 147 patients, who received treatment in a COVID specialized center. The subject of the study is the blood and blood serum of patients with coronary artery disease for the quantitative determination of the main biochemical parameters (lipid spectrum). Conclusions: A feature of the clinical course of AH in patients with COVID-19 is frequent high blood pressure, cases of tachycardia, impaired rhythm variability in the form of ventricular extrasystoles, complete blockade of the left bundle branch block, ST segment elevation on the ECG, increased T-wave inversion, progression unstable angina pectoris. In patients with AH and COVID-19, an increase in the atherogenic index, mean TG level, and a decrease in mean values of serum HDL concentration.
Keywords: COVID-19, Arterial hypertension, Blood pressure, Comorbidity, Cardiovascular complications
Cite this paper: Tashkenbaeva Eleonora Negmatovna, Mukhiddinov Abdumalik Inoyatovich, Abdieva Gulnora Alievna, Ergashev Arslonbek, Ellamonov Sukhrobjon Numonovich, Features of the Clinical Course of COVID-19 Depending on the Presence of Arterial Hypertension, American Journal of Medicine and Medical Sciences, Vol. 13 No. 7, 2023, pp. 883-888. doi: 10.5923/j.ajmms.20231307.07.
Article Outline
1. Introduction
- At the end of 2019, with the appearance in the world of a new coronavirus called SARS-CoV-2, which causes Covid-19, a global threat with severe consequences loomed over humanity [6]. Today, despite the worldwide unified search for methods and countermeasures, the disease is still spreading, new unfavorable variants of the course are observed against the backdrop of an overloaded healthcare system [7].A larger and deeper study of the etiopathogenetic and clinical manifestations of Covid-19 in individuals with chronic lesions of various organs and systems confirms the pattern of adverse outcomes and prognosis [1,2]. The emerging complications in patients infected with SARS-CoV-2, both with overt clinical manifestations and asymptomatic carriage, are of interest to the scientific community.According to the results of a meta-analysis that combined data from 8 studies (46248 patients), the most common comorbidity was hypertension (17%), along with diabetes mellitus (DM) (8%), cardiovascular disease (CVD) (5%) and bronchopulmonary pathology. (2%). Similar conclusions were reached by the authors of another meta-analysis, which included 6 studies with a total number of patients 1527 (AH 17.1%; CVD 16.4%; DM 9.7%). At the same time, among patients with a severe course who required transfer to the intensive care unit, AH was recorded in 28.8% versus 14.1% among patients with a severe course observed in a regular ward. An almost threefold ratio was also established for CVD and AH. F. Zhou et al published the results of a retrospective analysis of 191 cases of laboratory-confirmed coronavirus infection with a known outcome, registered in two specialized hospitals in Wuhan from December 29 to January 31, 2020. Hypertension was the most common comorbidity in patients in this sample, and deaths were more often recorded in individuals with concomitant diseases (AH 48% versus 23%, p = 0.0008; DM 31% versus 14%, p = 0.0051; coronary heart disease (CHD) 24% versus 1%, p<0.0008). It should be noted that the deceased were significantly older than those who recovered (69 (63–76) versus 52 (45–58) years), which may in itself determine a greater number of comorbid conditions in the group of adverse outcomes. An important aspect of COVID-19 is the course of infection in patients with aggravated premorbid background [3], while the role of hypertension as a risk factor for severe forms of the disease is noted [9]. To date, risk factors for damage to the lower respiratory tract and severe course of COVID-19 in patients with hypertension have not been identified. The role of genetic polymorphisms in the pathogenesis of this infectious process in patients with hypertension and their impact on prognosis remains unexplored. The persisting incidence rate, the emergence of new strains, and the escape of mutant strains from post-infection immunity dictate the need to study a new coronavirus infection in patients with hypertension.Commonality of the pathogenesis of arterial hypertension and COVID-19The question of the possible role of hypertension as one of the clinical factors in the severity of COVID-19 arose based on the existence of common pathogenetic links [8,11,15,16]. AH is a multisystemic and multifactorial disease involving complex interactions between genetic, environmental, and pathophysiological factors [17]. One of the central places in the pathogenesis of AH is assigned to the immune system [13,14]. Remodeling of arterial vessels in AH occurs with the participation of oxidative stress, which causes a destructive cascade in the endothelium and chronic inflammation [18,19]. Inflammation and endothelial dysfunction underlie the pathogenesis of both diseases [15,16]. In addition, the SARS-CoV-2 virus enters cells through angiotensin-converting enzyme 2 (ACE2), which is a key element of the RAAS involved in the pathogenesis of AH [20].A survey of patients who underwent COVID-19 (mean age 46.5±12.7 years) found in some cases the onset of arterial hypertension after an average of 31.6±5.0 days (p<0.001) [21]. These data do not exclude that COVID-19 may potentiate the onset of hypertension [25]. According to the results of the analysis of data from the register of the Eurasian Association of Therapists, which includes more than 7500 patients with past COVID-19, newly diagnosed hypertension was detected in 2.6% of patients with past COVID-19 [22], which confirms this hypothesis. Higher rates of development of new-onset hypertension were obtained in previously normotensive patients with a history of pneumonia [23,25-29]. After 6 months, the incidence of hypertension in this group was 12% [30]. With excess body weight in certain places in the body, a depot of adipose tissue is formed, mainly in subcutaneous adipose tissue, visceral adipose tissue, yellow bone marrow, mammary glands, and omentum. An increase in the mass of adipose tissue potentiates the systemic action of tissue angiotensin II, which ultimately disrupts microcirculation, the elasticity of the vascular wall and leads to different complications of cardiovascular system [10-12].Hypertension and post-covid syndromeCurrently, according to official statistics, the number of recovered COVID-19 is about 230 million people [24]. The consequences of the transferred coronavirus infection continue to be a topic for comprehensive study due to the many controversial and unresolved issues [31-33]. A systemic inflammatory disease, which is COVID-19, in some cases potentiates the development of post-COVID syndrome involving the cardiovascular system [34]. Damage to the vascular endothelium in COVID-19 and the development of endothelial dysfunction as one of the long-term effects of COVID-19 will contribute to an increase in mortality from cardiovascular disease worldwide [40].Based on the knowledge of the common pathogenesis of diseases, it can be assumed that patients with AH are most vulnerable to post-COVID syndrome. In one study, a study of patients with post-COVID syndrome revealed a higher number of post-COVID symptoms in the group of patients with hypertension (mean: 2.1, SD: 1.4) (IRR1.16, 95% CI 1.03-1.30, p= 0.012) than in the normal BP group (mean: 1.8, SD: 1.4) [35]. The most common post-COVID symptoms were fatigue, dyspnea at rest, and dyspnea on exertion [36]. Patients with AH had more comorbidities than patients with normal BP (X2: 56.340, p<0.001) [37]. These patients were more likely to have diabetes mellitus, obesity, and cardiovascular pathology (all p<0.01) [38].It is estimated that about 10% of the general population will suffer from post-covid hypertension [39]. To identify this category of patients, given the long-term asymptomatic course of hypertension, it is proposed to examine all patients who have undergone COVID-19 6–12 months after infection [24].One of the manifestations of the post-COVID syndrome in AH, apparently, is the destabilization of blood pressure. Analysis of data from the register of the Eurasian Association of Therapists revealed that 3 months after suffering COVID-19, 20.1% of the examined patients had uncontrolled hypertension [22].It has been reliably studied that the causative agent of a new coronavirus infection enters the human body through the entrance gate, which is the epithelium of the upper respiratory tract and the epithelial cells of the stomach and intestines. Adipose tissue has a high concentration of ACE2 receptors, which facilitates penetration into the cells of the SARSCoV-2 coronavirus [4,5,8].In view of the number of complications with which patients with MS infected with SARS-CoV-2 needed not only hospitalization, but also resuscitation, the problem of MS is even more acute than in the “favorable” period, before the spread of a new coronavirus infection.
2. Materials and Methods of Research
- During the study, 147 people over 18 years of age were examined with a virus infection and all patients were distributed as follows: the main group, which included 59 patients with COVID-19 and AH; the comparison group, which included 58 patients with COVID-19 without AH, the control group consisted of 30 healthy individuals.The determination of the interdependence of the considered parameters of the samples using the Student's test and the Pearson chi test (χ2) was carried out using the test of its significance.
3. Results of the Study and Their Discussion
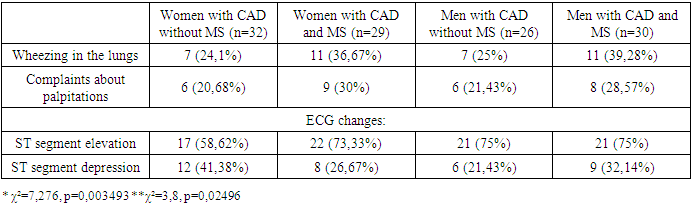
- We examined 147 patients hospitalized in the COVID Specialized Center and the Samarkand Regional Infectious Diseases Hospital with a verified diagnosis of COVID-19. Of these, patients with AH were 59 (30 men and 29 women) and 58 patients without AH (26 men and 32 women). Table 1 presents the complaints of hospitalized patients, anamnesis indicating the presence of bad habits (smoking), physical and ECG data.As the results of the study showed, in women with COVID-19 and AH, painless forms of coronary artery disease were 26.4% more common than women without MS. Among men, more than 50% were smokers and anamnesis showed an earlier onset of CAD.
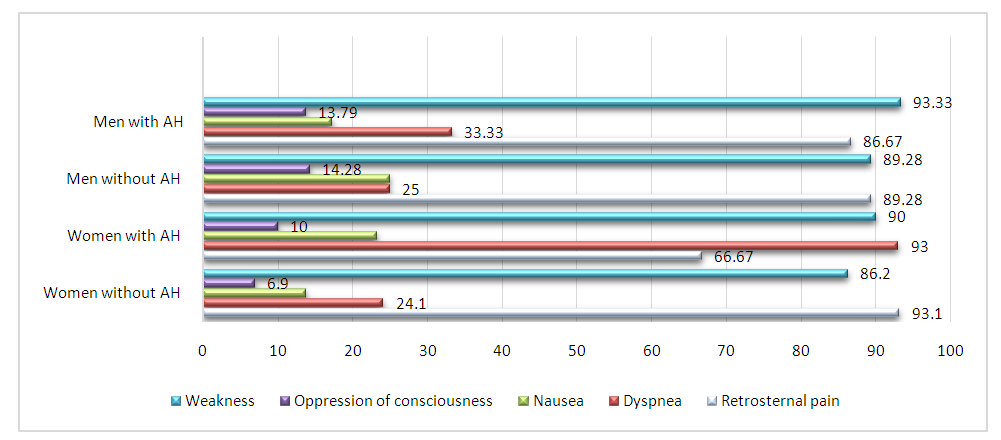 | Figure 1. Distribution of symptoms among patients |
|
|
|
|
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML