Yusupov Shukhrat Abdurasulovich1, Atakulov Jamshed Ostonakulovich2, Rustamov Timur Rashidovich3, Kiyamov Azizbek Utkirovich4
1Doctor of Medical Sciences, Head of the Department of Pediatric Surgery No. 1 of the Samarkand State Medical University
2Doctor of Medical Sciences, Professor Department of Pediatric Surgery No. 1 of the Samarkand State Medical University
34th Year Student of the Faculty of Medical Pedagogy of the Samarkand State Medical University
42nd Year Student of the Faculty of Medicine of the Samarkand State Medical University
Copyright © 2023 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Abstract
The analysis of complications of surgical treatment in 216 primary patients with Hirschsprung's disease operated upon by Soave-Lenyushkin method and treatment of 54 patients admitted with various complications and functional disorders after operations in other medical institutions for Hirschsprung's disease is performed in the article, the main operative and technical mistakes depending on a method of radical surgery (Swenson-Hyatt, Duhamel, Soave, Rebane) are revealed [3,4,8]. These operative-technical errors are divided into three groups: incorrect determination of the level of intestinal resection, defects of reductions, and defects of anastomosis creation.
Keywords:
Surgical treatment, Intestinal resection, Reductions, and defects
Cite this paper: Yusupov Shukhrat Abdurasulovich, Atakulov Jamshed Ostonakulovich, Rustamov Timur Rashidovich, Kiyamov Azizbek Utkirovich, Analysis of the Causes of Unsatisfactory Results of Surgical Treatment of Hirschsprung’s Disease in Children, American Journal of Medicine and Medical Sciences, Vol. 13 No. 7, 2023, pp. 879-882. doi: 10.5923/j.ajmms.20231307.06.
Article Outline
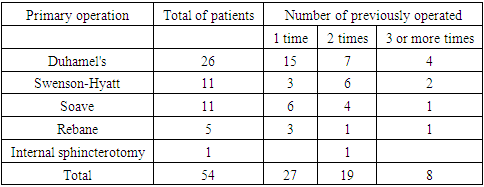
Swenson-Hyatt, Duhamel, Soave, Rebein and their modifications are the most common surgeries in Hirschsprung's disease surgery in children. Although these operations are well developed technically, mortality in the postoperative period remains high (3.7-11.7%). Complications and functional disorders, which require repeated surgeries, reach 25%.We followed up 54 patients (45 boys and 9 girls) aged 3-14 years old with Hirschsprung's disease earlier operated on in other medical institutions. These patients had various complications and functional disorders which required repeated surgical intervention. The distribution of patients according to the method of primary surgery and the number of interventions is shown in Table 1.Table 1. Distribution of patients according to the method of primary surgery and number of interventions
 |
| |
|
The analysis of our observations allows us to name diagnostic, tactical and operative-technical errors among the causes of complications and functional disorders [5,16]. In this paper, we will consider surgical and technical errors that are common and specific for certain methods. They can be grouped into three groups: incorrectly determined the level of intestinal resection, defects of its inferiorization, and defects of anastomosis creation.Incorrect determination of the resection level concerns mainly its proximal border. It is known that there are morphological changes at a certain section of suprastenotic extension underlying functional incompleteness of this section. As a consequence, not only the narrowed aganglionic area but also a part of the dilated section should be removed during radical surgery. However, when determining the volume of intestinal resection, surgeons are guided only by intuition and perform the resection by eye, without having at their disposal objective tests and criteria for assessing the level of resection. Due to this situation, it is quite possible that an incomplete intestinal section may be left, which can cause recurrence of the disease or various functional abnormalities after surgery. We monitored 4 patients who, in addition to other complications, had a narrowed area left during the primary surgery (removed during the reoperation). Recently, to determine the upper border of intestinal resection we use intraoperative registration of biopotentials from different parts of the intestine - the aganglionic zone, the transitional zone and above it. At the level where bioelectrical activity transitions to normal, we perform resection of the intestine.Defects of descending intestine can cause trophic disruption of anastomosed ends, which inevitably leads to anastomosis failure. This danger is real if there is an extensive aganglionic zone, when the whole left half of the colon has to be mobilized. In each particular case during reductions, one has to be particularly careful when laying the intestine in the left mesenteric sinus and the anorectal canal. Mismatch of the diameter of the dilated intestine with the diameter of the canal inevitably leads to some compression of it, and sometimes the surgeon is powerless to eliminate this mismatch. The correct positioning of the mesenteric edge, inadmissibility of tension of the mesentery and its twisting are of particular importance in this situation.Defects of anastomosis creation and related complications should be considered in relation to a particular type of intervention. In Swenson-Heatt and Rebain surgeries, one of the most typical and frequent complications is the development of an inflammatory process in the anastomosis area. This process is almost identical in origin, but differs in severity. Usually we have to make an anastomosis on different diameter ends of the intestine, and the difference is often significant. Circular and even oblique anastomosis is accompanied by corrugation of the proximal end, due to which it is not always possible to achieve tight sutures. The condition of anastomosis worsens considerably if the sutures are tied tightly, as well as if ischemia and trophic disorders of anastomosed intestine occur. Not only reducibility defects but also pressure of pararectal hematoma on the suture line can contribute to trophic disturbances. All these factors determine the development of inflammatory process. In mild cases it is limited to the formation of an infiltrate in the anastomosis area, which can disappear without serious consequences after resorption therapy. Sometimes rough scar tissue remains after the infiltrate and early scar stenosis of the anastomosis develops [7,13]. We observed a child who managed to revive anastomosis stenosis, in all other cases we had to resort to repeated intestinal stenosis.In more severe situations, anastomosis failure occurs with divergence of the intestinal edges, more often along the posterior wall, accompanied by suppuration of the pararectal tissue with fistulas opening to the perineum and stenosis of the anastomosis. There were 3 such patients after Swenson-Hyatt operation. In some cases there is a more serious complication - peritonitis - due to ascending infection of the abdominal cavity. There were 13 such patients with internal and external intestinal fistulas under our observation.It is impossible to predict in which direction the inflammatory process will develop, so in all cases when a complication occurs, it is advisable to switch off the intestine by applying an unnatural anus [6,12,19]. Thereafter, regular daily monitoring of the condition of the sutures by careful finger examination or visually with the help of rectal mirrors is carried out. The inconsistency of anastomosis is a direct indication for drainage of pararectal tissue: an incision is made between the anus and coccyx. General intensive treatment and antibiotic therapy are necessary. It usually takes from 6 months to 1 year to eliminate the consequences of anastomosis failure. It is erroneous to eliminate the unnatural anastomosis before this period, even if the defect has closed. Complete regeneration of the mucosa occurs approximately 4-6 months after the defect is no longer clinically identifiable. Recently, we have operated on 3 children using the Rebein technique. Patients under 3 years of age with a compensated course of the disease when there was no sharp dilation of the intestine above the narrowed area and when rectosigmoidal defect with a well-formed intestinal ampulla was isolated were indicated. These patients had no complications and were discharged on the 10th-11th day with independent stool. Three types of complications are observed in Duhamel type surgeries: external sphincter damage, formation of a rough stenosing scar - "parus", and leaving an excessive rectal stump [1,10,11].Damage to the external sphincter is the result of a gross technical error when the surgeon at the perineal stage of the primary operation makes an incision in the posterior semicircle of the anus along the mucocutaneous junction without retreating 1-1.5 cm inwards. Thus the surgeon destroys the posterior hemisphere of the external sphincter, sometimes for a considerable length, which results in fecal incontinence [2,9]. We observed 12 patients with sphincter damage during primary surgery.Formation of a "sail" is the most common complication that develops after Duhamel surgery. At the place of contact of the posterior wall of the rectal stump with the anterior wall, lowered after the clamps fall off, there remains a rough scar stenosing the anastomosis area. Causes of the "sail" scar occurrence are various errors in anastomosis creation [14]. One of them is excess tissue (pararectal tissue) on the stump of rectum, as a result of which there is no intimate contact of the intestinal walls when clamps are applied. Another reason is insufficiently tight squeezing of the walls. Besides, sometimes between the ends of clamps there is a free area ("track") in which a feeding vessel can pass, and not the whole triangle is necrotized, but only a part of it. Inflammatory process in the anastomosis area plays an important role in this case. As a result of "sail" formation the intestinal lumen turns out to be not only considerably narrowed but also sharply deformed. There were 7 such patients under our observation. B1 usting in these cases is futile as it is impossible to prevent the development of "sail" and moreover to liquidate it by stretching.Leaving of excessive rectal stump - "sac" (according to the terminology of foreign authors) is also one of the typical complications of Duhamel operation. In some cases, a long stump of the type of giant diverticulum is formed because the lumen of the rectum is closed too high, at the level of the transitional fold of the peritoneum, whereas it should be done approximately in the middle third of the ampullary part. In other cases crushing clamps are applied too low, which is due to the lack of control from the abdominal cavity over the application of clamps (their ends should be close to the bottom of the stump). We admitted 3 patients with such pathological changes. Presence of "sac" is usually combined with "sail", therefore intestinal content retention is also observed in the "sac".Case records analysis of 20 patients initially operated on by Soave-Lenushkin method and 8 patients admitted with complications after primary Soave operation, performed in other medical institutions, allowed us to reveal three types of complications: inflammatory process in the rectal canal region, necrosis of dislocated stump, rectal stenosis.Inflammatory process in the rectal canal develops due to violation of asepticity of the operation, mainly during its abdominal stage as a result of mucosal integrity damage, especially if intestine preparation is poor. The outcome of the inflammatory process is two-fold: either the infection remains local (interfacial abscess), or it spreads to the abdominal cavity (peritonitis). Interfutural abscess occurred in 4 of 174 patients who underwent primary surgery in the postoperative period; in 1 of them the process spread to the abdominal cavity and resulted in peritonitis, which required relaparotomy with colostomy placement. Among 11 repeated patients after the primary Soave operation the interfuchal abscess complicated by peritonitis occurred in 7 patients. Prevention of this complication, primarily the cleansing of the intestine from fecal masses before the operation is of great importance. The demucosal rectal canal must be treated with antiseptics during the operation and dry broad-spectrum antibiotics must be poured into it before the bowel descending. In cases of obvious infection of the wound with fecal matter the interfuchal space should be additionally drained. The drainage is placed parallel to the descended colon or through an additional incision between the coccyx and the rectum.Necrosis of the excreted intestine and its spontaneous rejection are associated with a disturbance of the blood supply, resulting from insufficient preservation of the feeding vessels during mobilization of the intestine or their compression in the anal canal. Sometimes the stump is also necrotic in cases when demucosalization is not carried out up to the level of the internal sphincter, but ends much earlier - in the ampullary part of the rectum. The feeding vessels in this situation are subjected to double compression: in the anus canal and above, at the level of incomplete demucosalization [17,18]. Therefore, the sphincter, the tone of which is always elevated in Hirschsprung's disease, must be stretched before the intestine is lowered to the perineum during primary surgery. Demucosalization must not be completed higher than 2-2.5 cm from the mucocutaneous junction, and the surgeon must ensure that the degree of demucosalization is sufficient before completion. Necrosis and detachment occur gradually over several days, most often immediately below the sphincter, the intestine remains viable and the same anatomical relationships are restored after stump detachment as when the stump is detached. However, it is not possible to predict or determine objectively the extent of necrosis, so it is prophylactically advisable to impose an unnatural anus when necrosis is undoubtedly present [15].Sometimes after spontaneous rejection of the necrotized stump there remains excess tissue at the edge of anastomosis, resulting in rectal stenosis. Stump necrosis was observed in 7 primary patients. In 3 of them the stenotic area was resected after 3-6 months, in 4 patients self-amputation occurred at the edge of muco-cutaneous transition and did not require operation. In 4 repeated patients with anastomosis stenosis after Soave operation the stenotic area was dissected transrectally according to Lenyushkin. Apart from the just mentioned reason, stenosis of anastomosis can be caused by two other things: 1) leaving too short residual limb (2-2.5 cm) after the first stage of the operation outside the anus which slips upwards: 2) leaving excessive tissue at the second stage of the operation (residual limb cutting) - almost inevitable in cases of incomplete demucosa at the first stage (in such cases part of the residual limb is "hidden" in the anus canal and above). These complications occurred in 6 patients who were initially operated on by us. The first complication in 4 patients was eliminated during the second stage of the operation, the second in 2 others after a month by excision of excess tissue.
References
| [1] | Атакулов Д.О., Юсупов Ш.А., Суванкулов У.Т., Рахимов А.К. Причины осложнений при аноректальных аномалиях у детей " "Актуальные вопросы, достижения и инновации. 25 января 2021 г. в г. Пенза с. 231-233. |
| [2] | Cувонкулов У. Т., Юсупов Ш. Ш., Сатаев В. У., Шамсиев А.М., Прогнозирование и профилактика послеоперационных внутрибрюшных спаечных осложнений у детей // https://doi.org/10.38096/2181- Экспериментальная и клиническ гастроэнтерология. 2021; 185(1): 127-132. DOI: 10.31146/1682- 8658-eco-185-1-127-132. |
| [3] | Хамраев А.Ж., Атакулов Ж.О. Болалар колоректал хирургияси // Учебное пособие для студентов медвузов Тошкент-2015. 135-176 стр. |
| [4] | Хамраев А.Ж., Атакулов Ж.О. Болалар колоректал хирургияси // Учебное пособие для студентов медвузов Тошкент-2015. 198-237 стр. |
| [5] | Шамсиев А.М., Саидов М.С., Атакулов Д.О., Юсупов Ш.А., Шамсиев Ж.А., Суванкулов У.Т., Хирургическое лечение аноректальных пороков у детей Хирургия детского возраста 2011 г. 40-43 стр. |
| [6] | Шамсиев Ж.А., Саидов М.С., Атакулов Дж.О., Махмудов З.М. Характеристика поздних послеоперационных осложнений и рецидивов аноректальных мальформаций, развившихся после различных видов проктопластик. Проблемы биологии и медицины №2 Том: 127 (2021). |
| [7] | Шамсиев Ж.А., Саидов М.С., Атакулов Д.О., Махмудов З.М. Характеристика поздних послеоперационных осложнений и рецидивов аноректальных пороков развития. «Проблемы медицины и биологии» 2021, №2 (127), -с.177-184. |
| [8] | Шамсиев Ж.А., Атакулов Д.О., Давранов Б.Л., Имамов Д.О., Ибрагимов О.А. Анализ причин наложения стом при врождённой кишечной непроходимости у новорождённых 2021 Детская хирургия 75-76. |
| [9] | Шамсиев А.М., Юсупов Ш.А., Сатаев В.У., Саидов М.С. Состояние нейрорецепторного аппарата прямой кишки после выполнения различных вариантов реаноректоплc’z mастики Проблемы биологии и медицины Узбекистан, СамМИ 2020. №2 (118) с. 134-136. |
| [10] | Юсупов Ш.А., Сувонкулов У. Т., Юсупов Ш. Ш., Сатаев В. У. Прогнозирование и профилактика послеоперационных внутрибрюшных спаечных осложнений у детей Экспериментальная и клиническая гастроэнтерология. 2021; 185(1): 127–132. DOI: 10.31146/1682-8658-ecg-185-1-127-132. |
| [11] | Юсупов Ш.А., Саидов М.С. Частота встречаемости аноректальных мальформации при антенатальной диагностике у детей Самарканда и Самаркандской области Доктор ахборотномаси №2 (94) 2020й. Самарканд с. 107-111. |
| [12] | Юсупов Ш.А., Атакулов Ж.О., Орипов Ф.С., Жовлиев Б.Б., Рахматов А.К. Влияние токсических препаратов на развитие аномалий кишечника и перспективы их хирургического лечения " Вятский медицинский вестник Научно-практический журнал 2(70) 2021 стр. 9-13. |
| [13] | Маrellis C, Ue Blauw J, Brunner H. Chromosomal anomalies in the etiology of anorectal malformations. A review, Amv med.Genet Part A 2021; 9999: 1-13. |
| [14] | Divarci, Ergun, D. General compliatons after surgery for anorectal malformations. Pediatric surgery international, 2020. 36(4), 431-445. |
| [15] | Shamsiyev A., Юсупов Ш.А., Shakhriev A., Djalolov D. The causes of postoperative intra-abdominal abcesses in children and ways of their prevention The scientific heritage №48 (2020) с. 5-9. |
| [16] | Yusupov Sh, Atakulov J, Rakhimov A, Suvankulov U. COMPLICATIONS IN ANORECTAL MALFORMATIONS IN CHILDREN (CLINICAL OBSERVATION) 2021 Проблемы науки 56-58 стр. |
| [17] | Amrish Tiwari, D.C. Naik, P. G. Khanwalkar, S. K. Sutrakar. Histological study of neonatal bowel in anorectal malformations. Int J Anat Res2014; 2(2): 318-24. |
| [18] | Ahemad, S., Abdul Muqtadir, A.M., Wanjari, S., & Vairagad, P. Early after posterior sagittalanorectoplasty outcomes for anorectal malformation. International journal of scientific research. 2022; 37(6): 1232-. |
| [19] | Bischoff A., Levitt M.A., Pena A. Update on the management of anorectal malformations// Pediatr. Surg. Int. 2013. Vol. 29, # 9. P. 899-904. doi: Anderson IM et al. Does posterosagittal 10.1007/s00383-013-3355-z. |
| [20] | Divarci, E., & Ergun, O. General complications after surgery for anorectal malformations. Pediatric surgery international, 2020. 36(4), 431-445. https://doi.org/10.1007/s00383-020-04629-9. |
| [21] | Trajanovska M., Taylor R. Long Term Outcome After Catto-Smith Surgery for Anorectal Malformation, Fecal Incontinence. Causes, and Outcome, 2014 DOI:/http://dx.doi.org/10.5772/57072. |
| [22] | Tiwari A, Naik D.C., Khanwalkar P.G., Sutrakar S.K. Histological study of neonatal bowel in anorectal malformations. Int J Anat Res. 2014; 2: 318- 24. [Google Scholar]. 218 Tonii H. Olrad. |


 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML