Zulfiya A. Khodjaeva 1, Amangaldi Kh. Khojaev 2
1Doctor of Philosophy in Medicine, Asia Med Center LLC, Uzbekistan
2Doctor of Philosophy in Medicine, Monada-Amon Clinic LLC, Uzbekistan
Copyright © 2022 The Author(s). Published by Scientific & Academic Publishing.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/

Abstract
Complex therapy with the inclusion of (Shock-wave therapy) SWT and vitamin D significantly increases the effectiveness of therapy in patients with Neck pain (NP) and Back pain (BP) and minimizes the risks of chronic disease. The maximum subjective satisfaction from the therapy received by patients with dorsalgia who received along with standard pharmacotherapy received SWT and vitamin D in therapeutic and prophylactic doses.
Keywords:
Dorsalgia of non-inflammatory genesis, Treatment, SWT therapy
Cite this paper: Zulfiya A. Khodjaeva , Amangaldi Kh. Khojaev , The Role of Shock Wave Therapy in the Treatment of Non-Inflammatory Dorsalgia, American Journal of Medicine and Medical Sciences, Vol. 12 No. 2, 2022, pp. 234-239. doi: 10.5923/j.ajmms.20221202.37.
1. Introduction
Back pain or neck pain (dorsalgia) is experienced during the life of the vast majority of the world’s population, dorsalgia is in second place in terms of prevalence, second only to colds [2.73-78].Depending on the mechanism of pain, there are nociceptive - local, reflected (projective, reflex); neuropathic – radicular (radiculopathy) and non-radicular, psychogenic (psychalgia) pain [7.35-44].Among the adult population, up to 43% experienced back pain in the last month, up to 65% in the last year, and about 84% suffered from back pain at least once in their lives [10]. Back and neck pain is one of the most common causes of disability in people aged 40–60 [6.1290-1294].
2. The Main Findings and Results
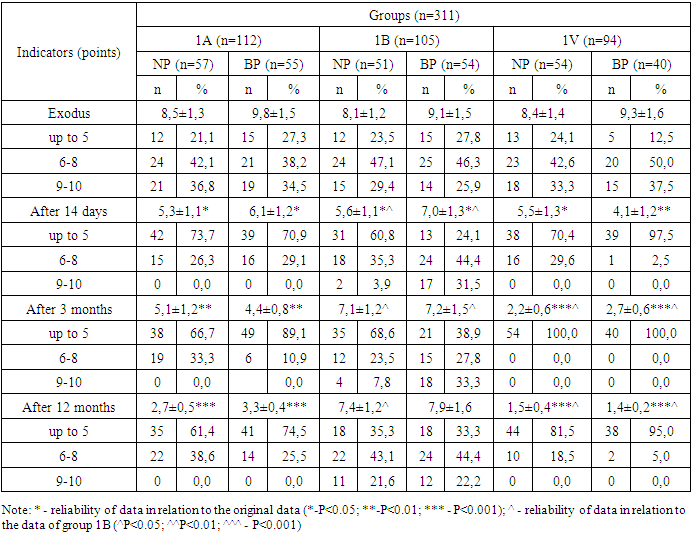
Due to chronic dorsalgia, people over 25 years of age are unable to work from a week a year for a third of the world’s population [12,14], over 40 years old - two thirds, and the therapy of such a contingent of patients reaches 80% of the health care costs in developed countries, more than 70% of them are due to back pain [14].Often, episodes of dorsalgia are nonspecific, predominant in the cervical and lumbosacral regions, and adequate therapy normalizes the condition in 4 weeks in 90% of patients [16]. However, in some patients, the pain syndrome persists for a long time, leading to disability [4.33-40,13]. A short-term episode of dorsalgia in every fourth patient leads to chronic pain, causing long-term disability [1,5].More than half of patients with cervical dorsalgia state a decrease in the strength of the pain syndrome after 7 days, 40% note a significant improvement after 2 months, about 10% of patients state pain within six months, 70–90% of patients note recurrences of episodes of neck pain after some time [11,15].Dorsalgia often occurs at the age of 20-50 years, the maximum pain syndrome occurs at the age of 50-64 years; at the age of 20-64, 24% of men and 32% of women state neck pain or back pain [8,9]. The most interesting thing is that 12–26% of children and adolescents also state the presence of neck pain or back pain [10,14].In the treatment of chronic dorsalgia, a maximally differentiated personalized approach to each patient is required due to the lack of universal effective methods of therapy [14]. Thus, non-steroidal anti-inflammatory drugs (NSAID), muscle relaxants, blockades for the relief of acute pain in chronic dorsalgia are practically ineffective and are used exclusively for exacerbations [3.46-50].In the literature, there are isolated reports on the method of treating myofascial pain syndrome (MFPS) by SWT and indicate a high efficiency of SWT treatment, all authors state the absence of complications and a significant reduction in the frequency of recurrence [6.1290-1294,7.35-44,9,10,12].All this leads to the idea of the possibility, effectiveness and high prospects of using SWT in the complex therapy of MFPS, especially in case of muscle overload against the background of degenerative diseases of the spine.Purpose of the study: To study the clinical efficacy of SWT and vitamin D in the treatment of non-inflammatory dorsalgia.Materials and methods of research: The study was based on examination data of 311 patients with dorsalgia without inflammatory genesis of dorsalgia, including 162 patients with neck pain (NP) and 149 patients with back pain (BP), aged 21-66 years (36.2±6.7 years).We conducted a comprehensive clinical and neurological examination with active identification of complaints and anamnesis, applied research scales: Visual Analogue Pain Scale (VAPS), Muscle Syndrome Index (MIS), Hospital Anxiety and Depression Scale HADS, Vernon and Major test. Radiological research methods were also used - CT and MRI.All patients received treatment in a physiotherapy private clinic for at least 10 days.Patients were divided into subgroups depending on the treatment regimen:Group 1A - differentiated therapy of dorsalgia without inflammatory genesis with the appointment of SWT - 112 patients (57 - NP and 55 - BP);Group 1B - differentiated therapy of dorsalgia without inflammatory genesis without the inclusion of SWT - 105 patients (51 - NP and 54 - BP).Group 1B - differentiated therapy of dorsalgia without inflammatory genesis with the appointment of SWT and vitamin D in therapeutic (10000 IU x 1 time in the morning after meals for 1-3 months) and prophylactic doses (4000 IU x 1 time in the morning after meals for 1-3 months) - 94 patients (54 - NP and 40 - BP).The effectiveness of treatment was assessed before the start of treatment, after 3 months, 6 months and a year from the start of treatment (12 months). A decrease in pain intensity by 10-20% was considered minimally significant, 30% - clinically significant, and more than 50% - a significant improvement [2.73-78,8].Results of the study: the intensity of pain at baseline and after complex therapy after 3 and 12 months according to the VAS scale is shown in Table 1.Table 1. Dynamics of VAS parameters during the treatment among patients with dorsalgia without an inflammatory component
 |
| |
|
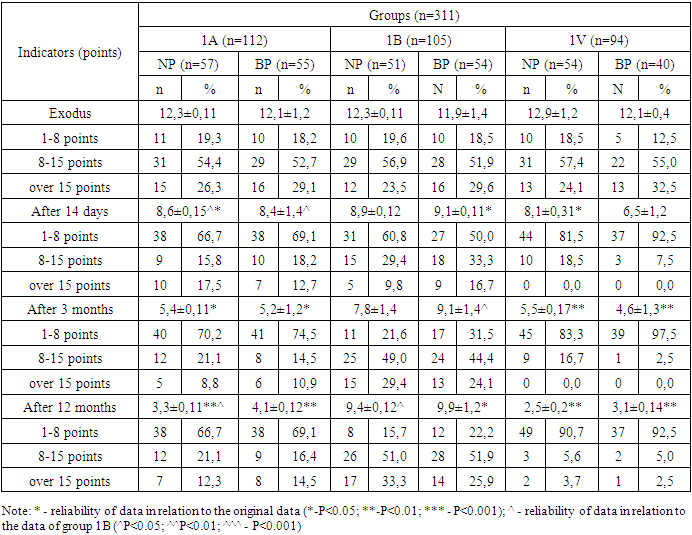
As can be seen from the table in group 1A with NP and BP, the initial average values were 8.5±1.3 and 9.8±1.5 points, we noted a significant decrease in VAS scores already on the 14th day of treatment, after 3 months and For 12 months, the positive effect persisted, which was confirmed by a persistent decrease in mean scores (2.7±0.5 and 3.3±0.4 points, respectively).In group 1B, among patients with NP and BP, regression of the pain symptom was observed during the first 14 days of treatment (5.6±1.1 vs. 7.0±1.3 points; P<0.01), while in the long-term period after 3 months and 12 months there is an increase in the average scores on the VAS scale (7.1±1.2; 7.2±1.5 and 7.4±1.2 and 7.9±1.6 points).In group 1 patients with NP and BP, after 14 days of treatment, there was an almost 2-fold decrease in the mean VAS scores (8.4±1.4 and 9.3±1.6 versus 5.5±1.3 and 4, 1±1.2 points; P<0.05), in the long-term period after 3 and 12 months, pain relief was observed in all patients, while the average scores significantly decreased in relation to the initial data (2.2±0.6 and 2.7±0.6 points versus 1.5±0.4 and 1.04±0.2 points; P<0.001). The study of the long-term period showed stable positive dynamics among patients with NP and BP when SWT and vitamin D were prescribed in the complex therapy.The most pronounced relief of the muscular-tonic syndrome was observed in group 1B in patients with NP and BP, i.e. in patients in whose complex of treatment SVT and vitamin D were prescribed. In the analysis of the initial indicators, MIS in group 1A, both with NP and BP, corresponded to the III degree of severity, while after the treatment of the I degree (mild) (Table 2).Table 2. Dynamics of MIS indicators during treatment in patients with dorsalgia without an inflammatory component
 |
| |
|
Mean values on the MIS scale on day 14 in group 1A in patients with NP significantly decreased (12.3±0.12 versus 8.6±0.15 points). In the long-term period, symptom relief in this group reached 3.3±0.11 points.With BP in group 1A, the average MIS score after 14 days of treatment was 8.4±1.4 points, which is significantly lower than the initial data. After 3 and 12 months, there is a stable relief of the muscular-tonic syndrome (5.2±1.2 and 4.1±0.12 versus 12.1±1.2 points; P<0.05).In group 1B, in patients with NP, positive dynamics of MIS indicators was noted on day 14, in the long-term period, the average MIS indicators increased and most patients reached the initial data or higher. Among patients with BP in group 1B, there is a similar picture. The data obtained in the 1B group indicate that the relief of the muscular-tonic syndrome is unstable and in the long-term period, the majority of patients experience repeated cases of the disease.In group 1C, the most pronounced positive dynamics of relief of the muscular-tonic syndrome was registered with the preservation of a stable effect in the long-term period compared with the indicators of groups 1A and 1B. So, 14 days after treatment, there was an almost 2-fold decrease in the average scores (P<0.05) according to MIS, while after 3 months, a decrease in the average scores was noted by 2.4 times (P<0.05), and after 12 months 3.9 times (P<0.01) in relation to the original data. The study of the long-term period showed a stable positive trend among patients with BP when prescribing SWT and vitamin D in the complex therapy.The average sum of pain self-assessment scores among patients with NP in the course of follow-up varied from 23.1±1.9 to 5.1±0.4 points in group 1A, from 22.6±1.6 to 18.2±1, 5 points - in group 1B and from 23.5±1.9 to 3.1±0.3 points in group 1C, which reliably indicated a decrease in the quality of life of patients with NP and corresponded to moderate disability at the beginning of treatment in all groups and a small limitation in 1A and 1B groups after treatment in the long-term period (p<0.05). A more detailed analysis is presented in fig. 1.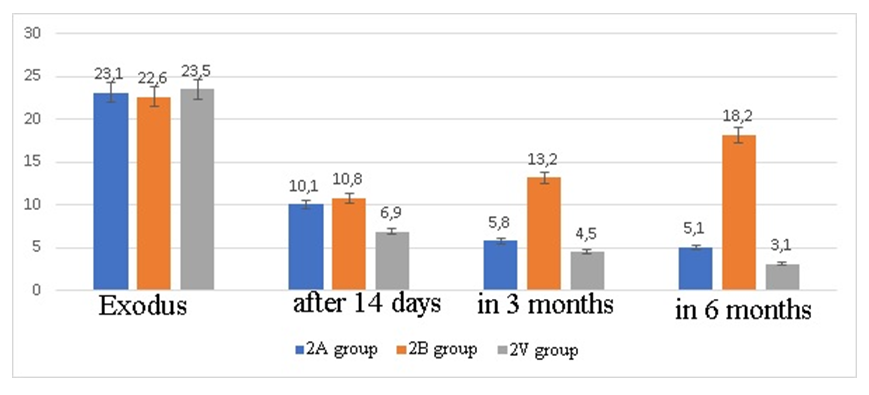 | Figure 1. The degree of disability according to the test of Vernon and Major in patients with cervical dorsalgia without an inflammatory component (n=162) |
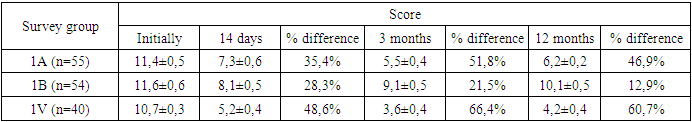
As can be seen from the diagram, the improvement in the quality of life of patients is most pronounced in group 1B, in these patients with NP in the long-term period there were no movement restrictions, which indicates the expediency of prescribing SWT and vitamin D in the complex treatment of patients with NP of inflammatory origin.Recovery of functioning according to Roland-Morris in patients with BP is presented in Table 3.Table 3. Restoration of functioning according to Roland-Morris in patients with BP (M±m)
 |
| |
|
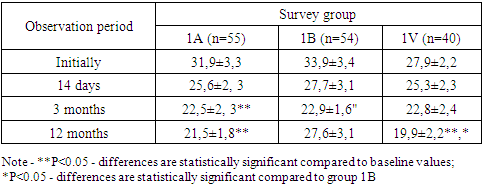
Exacerbation was resolved within 2 weeks in group 1A by 35.4%, in group 1B by 28.3%, in group 1C by 48.6%, which confirms the significant analgesic effect of SWT and vitamin D in early use. In the 1B group, the restoration of functioning was stated to be the worst relative to the 1A and 1C groups.The main goal of therapy was to improve the quality of life (QOL) of patients using medication and non-pharmacological methods while monitoring the condition using the modified Oswestry questionnaire (Table 4).Table 4. Quality of life in patients with BP according to the Oswestry questionnaire (M±SD)
 |
| |
|
In patients of groups 1A and 1B, an improvement in QOL was recorded throughout the duration of the study with a predominance of progressively milder forms of functioning disorders with a simultaneous statistically significant decrease in the intensity of disorders. However, after 3 months and 1 year in group 1B, a general deterioration in QOL and an increase in the total scores according to the Oswestry questionnaire were again recorded, in contrast to groups 1A and 1C, and the maximum QOL after 1 year was recorded in group 1B: 22.8±2.4 and 19.9±2.2%, respectively, which indicates a positive effect of the administration of SWT and vitamin D during the first exacerbation in the long-term period of the disease.In the dynamics of observation, in most cases in the long-term period after 3 and 12 months of observation, patients noted minimal impairment of life (92.5%, respectively). The number of patients with moderate disability slightly increased in relation to the 14th day after treatment. In the dynamics of observation in patients of this group, according to the questionnaire, a disabling quality of life was not established, i.e. lower back pain worsening all aspects of the patient's life, however, before treatment it was noted in 12.5% of patients.At a further stage, we evaluated the data on the scale of the overall clinical impression - improvement (CGI-I), we assessed the condition of patients with NP and BP to what extent it improved or worsened compared to the initial state at the beginning of treatment.In group 1B of patients with BP, 14 days after treatment, 20.4% had a “very strong improvement” and “significant improvement” - 48.1%, “minimal improvement” was noted by 14.8%, no change - 16.7%. In the follow-up dynamics after 3 months, when surveying patients with BP, the improvement indicators decrease, and in 9.3% of cases there is a deterioration in the condition, after 12 months, 11.1% of patients with BP notice a deterioration in the condition, which is 2.5 times higher (Р< 0.05) previous subjective assessment of the condition.In group 1B, when assessing a “strong improvement” in the condition after 14 days, 75.0% of patients with BP were noted, which is higher than group 1A by 4.1%, and 1B - by 54.6%. In the dynamics of observation in group 1B of patients with BP, a positive trend in the assessment of the overall clinical impression-improvement persists; at 3 and 12 months of the dynamics of observation, deterioration was recorded in 6 patients.The maximum subjective satisfaction from the received therapy of patients with BP was statistically significantly (p<0.05) stated in group 1B before other groups: 2 weeks after the end of SWT procedures and vitamin D intake, all representatives of group 1B noted a significant improvement. In group 1A, there are significantly fewer such patients (p<0.05). And by the end of the study, the maximum subjective effectiveness of therapy in all representatives of groups 1B and 1A, and 15 (29.4%) patients of group 1B stated that there was no effect from the received treatment. Excellent efficiency in group 1A was achieved in 71.9%, in group 1B - in 77.8%, and in group 1B - in 17.6% (P<0.01).Thus, the maximum subjective efficacy of therapy was stated in patients who, along with standard pharmacotherapy, received SWT and vitamin D in therapeutic and prophylactic doses.The number of relapses per year is statistically significantly (p<0.05) less in group 1C with BP - 1.1 ± 0.06 times, and with NP - 0.94 ± 0.05 times relative to groups 1A and 1B, which is clearly demonstrated in figure 2.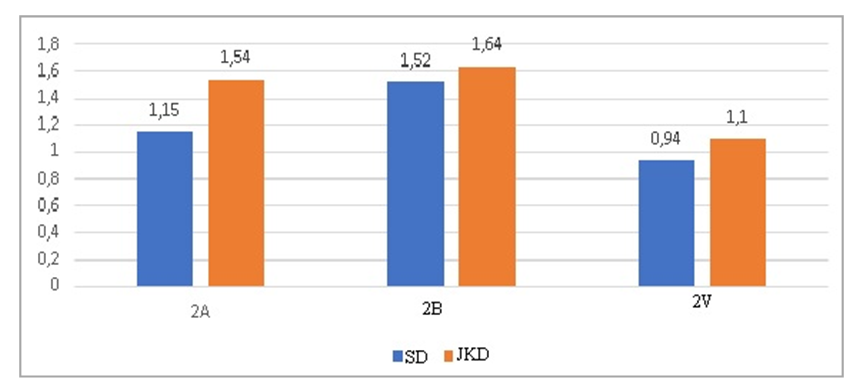 | Figure 2. The number of repeated exacerbations in the examined patients |
Thus, after analyzing the effectiveness of SWT and vitamin D in the complex treatment of patients with dorsalgia, we came to the conclusion that the use of SWT is safe and effective, has an analgesic systemic effect: own analgesic effect, decongestant, anti-inflammatory, reparative, antioxidant action, which normalizes local microcirculation.
3. Сonclusions
1. Complex therapy with the inclusion of SWT and vitamin D significantly increases the effectiveness of therapy in patients with NP and BP and minimizes the risks of chronic disease.2. The maximum subjective satisfaction from the therapy received by patients with dorsalgia who received along with standard pharmacotherapy received SWT and vitamin D in therapeutic and prophylactic doses.
References
| [1] | Aleksandrov V.V., Demyanenko S.A., Mizin V.I. Fundamentals of restorative medicine and physiotherapy - Moscow: GEOTAR-Media, 2018. – P. 208. |
| [2] | Boytsov I.V. Dorsopathies of the cervical, thoracic, lumbar spine: features of neurological complications (literature review). // Ref. general practitioner. 2018. - No. 5. – P.73–78. |
| [3] | Vorobieva O.V., Akarachkova E.S. The role of depression in the chronicity of dorsalgia: approaches to therapeutic correction // Journal of Neurology and Psychiatry. - 2004. - No. 8. - P. 46-50. |
| [4] | Kozelkin A.A., Medvedkova S.A., Lisovaya O.A. Manual therapy of vertebral thoracic neurological syndromes // International neurological journal. - 2019. - No. 5 (107). - P. 33-40. |
| [5] | Kotelnitsky A.V. Manual reflexology. - Moscow: Binom, 2019. - 168 p. |
| [6] | Manvelov L.S., Tyurnikov V.M. Lumbar pain (etiology, clinic, diagnosis and treatment). // Rus. honey. magazine 2019, - No. 20. – P.1290–1294. |
| [7] | Merkushkina I.V. Problems of discogenic dorsalgia: pathogenesis, clinic, treatment. // Farmateka. 2019. - No. 19. – P.35–44. |
| [8] | Coskun Benlidayi I. I have back pain! Rheumatol Int. 2018 Nov; 38(11): 2163-2164. doi: 10.1007/s00296-018-4162-6. Epub 2018 Oct 6. PMID: 30293154. |
| [9] | Gupta L, Zanwar A, Misra DP, Agarwal V. Approach to non-compressive back pain. Neurol India. 2019 May-Jun; 67(3): 671-678. doi: 10.4103/0028-3886.263183. PMID: 31347533. |
| [10] | Henn L, Hardt J. Therapy of Chronic Back Pain Considering Psychosocial Aspects. // Psychother Psychosom Med Psychol. 2019 Aug; 69(8): 313-322. doi: 10.1055/a-0813-2086. Epub 2019 Jan 14. PMID: 30641598. |
| [11] | Jiménez-Juan C, Bernabeu-Wittel M, Ternero-Vega J, García-Serrano R. Back pain after endoscopic retrograde cholangiopancreatography. Gastroenterol Hepatol. 2020 Nov; 43(9): 524-525. English, Spanish. doi: 10.1016/j.gastrohep.2020.03.002. Epub 2020 May 6. PMID: 32386895. |
| [12] | Kiltz U, Baraliakos X, Regel A, Bühring B, Braun J. Causes of pain in patients with axial spondyloarthritis. Clin Exp Rheumatol. 2017 Sep-Oct; 35 Suppl 107(5): 102-107. Epub 2017 Sep 29. PMID: 28967358. |
| [13] | Padiyar A, Pandipati S, Kim T, Haig AJ. An objective review of consumer books about back pain. // J Neurosci Nurs. 2021 Dec; 33(6): 326-37. doi: 10.1097/01376517-200112000-00007. PMID: 11776715. |
| [14] | Schiltenwolf M, Schwarze M. Diagnostics and therapy of back pain: what is advisable? What should be avoided and why is it still done? // Federal Health Gazette Health Research Health Protection. 2020 May; 63(5): 527-534. doi: 10.1007/s00103-020-03121-y. PMID: 32189043. |
| [15] | Szulc P. Vertebral Fracture: Diagnostic Difficulties of a Major Medical Problem. J Bone Miner Res. 2018 Apr; 33(4): 553-559. doi: 10.1002/jbmr.3404. Epub 2018 Mar 5. PMID: 29419882. |
| [16] | Vining R.D., Shannon Z.K., Minkalis AL, Twist EJ. Current Evidence for Diagnosis of Common Conditions Causing Low Back Pain: Systematic Review and Standardized Terminology Recommendations. J Manipulative Physiol Ther. 2019 Nov; 42(9): 651-664. doi: 10.1016/j.jmpt.2019.08.002. Epub 2019 Dec 20. PMID: 31870637. |




 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML


