-
Paper Information
- Paper Submission
-
Journal Information
- About This Journal
- Editorial Board
- Current Issue
- Archive
- Author Guidelines
- Contact Us
American Journal of Dermatology and Venereology
2014; 3(5): 81-83
doi:10.5923/j.ajdv.20140305.01
The Prevalence of Occupational Dermatosis among Workers in Khartoum State’s Tanneries
Kamal El-Din Hussein El-Hassan1, Yousif M El-Kordofani1, Anilkumar Mithani1, Tayseer E. E. Diab2, Zuhair A. A. Babikir3, Ali Thoulifkar A. Imeer4, Gamal O. Elhassan5, Abdel Khalig Muddathir6, Khalid O. Alfarouk6, Adil H. H. Bashir6
1Faculty of Medicine, University of Bahri, Bahri, Sudan
2Faculty of Medicine, Al-Neelain University, Khartoum, Sudan
3University of Medical Sciences and Technology, Khartoum, Sudan
4School of medicine, AL-Yarmouk College, Khartoum, Sudan
5Uneizah Pharmacy College, Qassim University, KSA
6Institute of Endemic Diseases, University of Khartoum, Khartoum, Sudan
Correspondence to: Adil H. H. Bashir, Institute of Endemic Diseases, University of Khartoum, Khartoum, Sudan.
| Email: |  |
Copyright © 2014 Scientific & Academic Publishing. All Rights Reserved.
Introduction: Occupational skin disease is any skin disorder which is caused by a person’s work. An existing skin disorder becoming worse by work activities is also considered as occupational skin diseases. Objective: To identify the pattern of occupational dermatosis and other skin diseases in Khartoum State’s tanneries in the period from May to June 2002. Patients & methodology: The survey was performed at Khartoum tannery and White Nile tannery; both located in the central part of Khartoum State. This is a descriptive, cross-sectional study. Conclusions: The prevalence of skin diseases collective prevalence 67.4% in Khartoum tannery and White Nile tannery (p>0.05). The prevalence of skin diseases was more in two departments, tanning department and engineering & maintenance department. Skin diseases’ prevailed in the following order: contact dermatitis, urticaria, hand eczema, fungal infection and atopic eczema. This result is consistent with the studies from other counties. These skin diseases were easy to treat, ameliorate and prevent by applying simple measures.
Keywords: Occupational Dermatosis, Khartoum tannery, White Nile tannery
Cite this paper: Kamal El-Din Hussein El-Hassan, Yousif M El-Kordofani, Anilkumar Mithani, Tayseer E. E. Diab, Zuhair A. A. Babikir, Ali Thoulifkar A. Imeer, Gamal O. Elhassan, Khalid O. Alfarouk, Adil H. H. Bashir, The Prevalence of Occupational Dermatosis among Workers in Khartoum State’s Tanneries, American Journal of Dermatology and Venereology, Vol. 3 No. 5, 2014, pp. 81-83. doi: 10.5923/j.ajdv.20140305.01.
1. Introductions
- An occupational skin disease is any skin disorder which is caused by a person’s work. An existing skin disorder becoming worse by work activities is also considered as occupational skin diseases [1].Occupational dermatosis and other skin diseases (23.4%) are very common, being among the many work-related health hazards encountered by doctors [2–4], ranking second only to musculoskeletal problems (45.3%) [5]. Therefore, there is a pressing need for greater awareness among all those who are in contact with patients having occupational skin disorders; including paramedics, safety representatives and nurses as well as dermatologists and occupational physicians.Accurate figures for the frequency of occupational contact dermatitis in the general population are not known. Some authors estimate the frequency as approximately 10/10000 per year [3]. There are many published surveys, studying the prevalence of contact dermatitis in factories where there have been dermatitis problems [4]. In certain wet-work jobs such as Lithography, prevalence of low-grade contact dermatitis of the hands is approximate 10% [6–8].In a Swedish survey, high figures as 21.3% were found for hand dermatitis in cleaners, compared with other occupations of approximately 11% [6]. However, the prevalence of hand dermatitis in women was twice as much as for men. The UK surveillance-reporting scheme for occupational skin diseases (1993-1995), provided these figures: contact dermatitis 79.8%, neoplasias 13.2%, contact urticaria 3%, infective 1.6% and others 4.6%. Also, showed occupations with the highest risk rate (10,000 per year), as follows: hairdressers 10.9, printers 7.1, foundry workers 6.2, beauticians 5.1 and machine tool operators 4.9 /10,000 per year [2].There is no doubt that occupational contact dermatitis is also very costly to society as a whole, in terms of money and disablement. In the USA alone it has been estimated that the annual cost of disease due to lost productivity, including medical care and disabled payments, may range from $222 to $1000 millions [8]. In the UK it has been estimated that four million working days are lost each year due to employees taking time off work because of skin disorders. Tannery industry has a long history in Sudan. A lot of traditional units for tannery have been established in almost all States of Sudan where Garrard is used as tonnage material. However, we didn't find any work dealing with occupational dermatosis in tanneries; therefore this work could be the first in this domain.
2. Patients and Methods
- • This is a descriptive, cross-sectional study, done in Khartoum State’s tanneries from May to June 2002, during the working hours.• The subjects were fully informed of the purpose and procedure of the survey. All workers were screened for skin diseases by three medical students of the fifth year, and they filled the demographic part of the questionnaire, even minor skin conditions were included, i.e. total coverage of study population. In order to enhance the reliability of the interview a consultant dermatologist and a registrar examined the subjects, performed the dermatological examination and completed the clinical part of the questionnaire.Study area:Khartoum tannery is one of the oldest Sudanese modern tanneries, founded in 1959 and its production started in 1962 [3]. The main production is tanned cattle hides, sheep and goat skins, also reptile skins, i.e. snakes, lizards and crocodiles, now there is tanning and finishing of small amounts for exhibition and shows.White Nile tannery is the largest tannery in Sudan, it started production in 1975 as public sector tannery, privatized in 1992 and was then rehabilitated [3]. Its daily capacity is 6000 pieces light leather (sheep or goat) and 1000 pieces of heavy hides (cow) [3].In both Khartoum and White Nile tanneries, there was a health unit staffed by one medical assistant and limited amount of drugs as well as there were no laboratories in the tanneries.Study population:The number of workers in Khartoum tannery was 200 workers, distributed in 4 departments as follows:
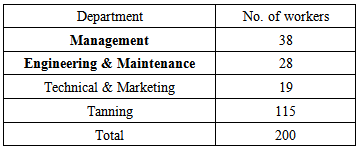 White Nile tannery has a force of 100 worker distributed in the 4 departments as follows:
White Nile tannery has a force of 100 worker distributed in the 4 departments as follows: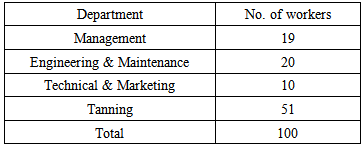 Tools and instruments:Questionnaire was filled for each case with skin lesion (70 and 25 cases for Khartoum and White Nile tanneries respectively, total coverage was 95 cases). Data analysis:The questionnaire has been designed in a way that facilitates for computer-based analysis using SPSS.
Tools and instruments:Questionnaire was filled for each case with skin lesion (70 and 25 cases for Khartoum and White Nile tanneries respectively, total coverage was 95 cases). Data analysis:The questionnaire has been designed in a way that facilitates for computer-based analysis using SPSS.3. Results
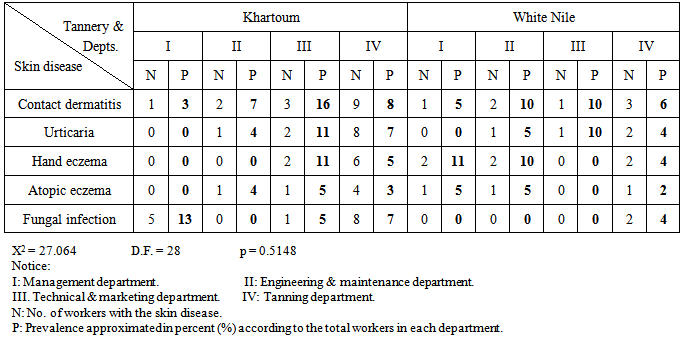
- Others include: Miliaria, heat rash, nail discoloration, dematography, angioedema, leishmania, keratoacanthoses, neavi, acne vulgaris, keloids scar, irritant eczema, chronic eczema, epidermal cyst, erythrasma, viral warts, seborrheic dermatitis & photo dermatitis.The percentages of number of workers were taken from the total number of workers with skin lesions each in their own tannery.The prevalence was taken from the total number of workers in each factory i.e. 200 worker in Khartoum tannery and 100 in White Nile tannery.Pompholyx eczema, tumors & Argyria were not found in both tanneries. The order of skin lesions’ prevalence in the main department affected i.e. tanning department, was found to be in Khartoum tannery firstly contact dermatitis (8%), then urticaria and fungal infection (7%), hand eczema (5%) and finally atopic eczema (3%). While in White Nile tannery it was found to be firstly contact dermatitis (6%), then urticaria, hand eczema and fungal infection (4%) and lastly atopic eczema (2%). No statistical difference in the order of skin lesions’ prevalence was found between the two tanneries (p>0.05).
|
|
4. Recommendations
- Occupational dermatitis is widely preventable if proper control measures were adapted as:− The workers should be given adequate protection against the direct contact with the skin hazards, such as gloves, boots, aprons and emollients. Protective clothing should be continuously washed and kept in good order. A clean work environment with good ventilation is obligatory.− Strengthening the health units in tanneries by establishing well-equipped laboratories, supplying enough dermatological, drugs, training of medical assistants for tackling major dermatological problems encountered in work, and if possible a dermatologist should be available at least two days per week.− National legislations to limit the contents of water soluble chromate and other irritant and/or allergic chemicals.
ACKNOWLEDGMENTS
- This work has been supported by Alfarouk Biomedical Research LLC.
 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-text HTML
Full-text HTML