Maytham M. Al-Hilo1, Shakir J. Al-Saedy1, Ahlam I. Alwan2
1MBChB, FICMS DV, Consultant Dermatologist and Venereologist, Al-Kindy Teaching Hospital, Baghdad, Iraq
2MBChB, DVD, DLM, Department of dermatology & Venereology, Al-Kindy Teaching Hospital, Baghdad, Iraq
Correspondence to: Maytham M. Al-Hilo, MBChB, FICMS DV, Consultant Dermatologist and Venereologist, Al-Kindy Teaching Hospital, Baghdad, Iraq.
| Email: |  |
Copyright © 2012 Scientific & Academic Publishing. All Rights Reserved.
Abstract
Miliaria is a common disease in hot humid climate. It caused by blockage of the sweat ducts, which results in the leakage of eccrine sweat into the epidermis or dermis. According to the level of sweat duct obstruction, miliaria is subdivided into three main types: miliaria crystallina, miliaria rubra and miliaria profunda. The aim was to study the clinical types of miliaria in patients attending Al-Kindy Teaching Hospital in Baghdad. This study was done in the Department of Dermatology and Venereology in Al- Kindy Teaching Hospital during the period from April 2010 to November 2011. A total of 113 patients exposed to extreme heat including eighty nine males and twenty four females. Their ages ranged between one year and fifty two years with a median of thirty one years. All of them complaining of itchy rash at different sites of the body. The patients were examined fully and diagnosed as miliaria depending on a clinical aspect, and all were photographed using a digital camera SONY DSC-T700 10.1 Megapixel. Through studying (113) patients with heat rash, eight patients (7.7%) shows classical miliaria rubra and 105 cases(92.9%) show a peculiar type of sweat rash that differ from the classical miliaria ; these type of lesions appear as dry red to red brown toasted-like patches or erythematous sun–burn like lesion. Neither miliaria crystalina nor miliaria profunda was reported. In conclusion, the commonest type of miliaria that has been observed in patients included in this study was a peculiar type of sweat rash. The lesions appear as brown toasted-like or erythematous sun –burn like patches associated with mild to moderate itching seen mainly on the trunk or the site of friction. This type is regarded as atypical type of miliaria that differs from the known classical forms of miliaria.
Keywords:
Miliaria Crystallina, Miliaria Rubra, Miliaria Profunda, Sweat Rash
Cite this paper:
Maytham M. Al-Hilo, Shakir J. Al-Saedy, Ahlam I. Alwan, "Atypical Presentation of Miliaria in Iraqi Patients Attending Al -Kindy Teaching Hospital in Baghdad: A Clinical Descriptive Study", American Journal of Dermatology and Venereology, Vol. 1 No. 3, 2012, pp. 41-46. doi: 10.5923/j.ajdv.20120103.02.
1. Introduction
Miliaria also called (sweat rash or prickly heat) is a common skin disorder of eccrine sweat duct integrity1.it is a common problem in hot and humid conditions, such as in the tropics and during the summer season. Although it affects people of all ages, it is especially common in children and infants due to their underdeveloped sweat glands. Miliaria is thought to be caused by blockage of the sweat ducts, which results in the leakage of eccrine sweat into the epidermis or dermis.2,3Based on the level of sweat duct obstruction, miliaria is subdivided into three main types: miliaria crystallina, miliaria rubra and miliaria profunda.The primary stimuli for the development of miliaria are conditions of high heat and humidity that lead to excessive sweating. Occlusion of the skin due to clothing, bandages, transdermal medication patches4 or plastic sheets (in an experimental setting) can further contribute to pooling of sweat on the skin surface and over hydration of the stratum corneum.Resident skin bacteria, such as Staphylococcus epidermidis and Staphylococcus aureus, are thought to play a role in the pathogenesis of miliaria.5,6Prickly heat can be prevented by avoiding activities that induce sweating using air conditioning to cool the environment,7 wearing light clothing and in general avoiding hot and humid weather. Anhydrous lanolin resolves the occlusion of pores and restores normal sweat secretions. Soothing, cooling baths containing colloidal oatmeal or corn starch are beneficial. Mild cases respond to dusting powders, such as corn starch or baby talcum powder.8
2. Patient and Methods
2.1. Patients Assessment
This clinical descriptive study was carried on in the department of dermatology in Al- Kindy Teaching Hospital in Baghdad during the period from April 2010 to the end of October 2011.A total of 113 patients were included in this study. All of them gave a history of exposure to extreme heat associated with excessive sweating followed by evidence of itchy rash at different sites of the body. The patients administered questionnaire elicited information on their age, sex, occupation, site of the rash, duration of rash, frequency of attacks before (whether it was the first attack, second attacks or recurrent if recurred more than three times before), history of associated symptoms (pruritus which subjectively prescribed as mild, moderate and severe), history of associated disease and history of any medication taken by the patient. The patients were examined fully and categorized clinically to either typical miliaria or atypical miliaria. Typical cases of miliaria were classified depending on the following criteria: 1). Miliaria crystalina with superficial tiny, fragile, clear vesicles that rupture easily.2). Miliaria rubra with an extremely pruritic erythematous papules or papulo-vesicular rash and on the other hand miliaria pustulosa when pustules develop in lesions of miliaria rubra and finally miliaria profunda that produces asymptomatic flesh-coloured papules2,3. The lesions were photographed using a digital camera SONY DSC-T700 10.1 Megapixel.
2.2. Statistical Analysis
Descriptive statistics were undertaken using Microsoft Excel.
3. Results
3.1. Age and Gender Distribution
A total of 113 patients with heat rash, their age varied between one year and fifty two with a median of 30 years.Miliaria was seen in eighty-nine male patients (78.76%). Their ages varied from 1 year to 52 years with median of thirty years.Female patients were twenty-four (21.23%). Their ages varied between 5 years and 44 years with a median of twenty nine years.Patients were classified according to age groups and gender distribution.| Table 1. Miliaria distribution according to age and gender |
| | Age group | Male | Female | Total number | Percentage | | ≤ 10 years | 3 | 2 | 5 | 4.41% | | 11-20years | 8 | 2 | 10 | 8.84% | | 21-30 years | 34 | 2 | 36 | 31.85% | | 31-40 years | 30 | 11 | 41 | 36.28% | | 41-50 years | 11 | 7 | 18 | 15.92% | | 51-60 years | 3 | - | 3 | 2.65% | | Total | 89 | 24 | 113 | 100% |
|
|
The least figure was seen in those with age group less than 10 years only five (4.41%) patients., Patients who were 5 years or less, were only 2 patients (1.76%) while Patients between 5-10 years were three patients (2.65%).Patients between 31- 40 years age group show the highest figure. They were forty-one patients (36.28%): (Thirty males and eleven females). Table 1
3.2. Occupation of Patients
Heat rash was reported with highest figure, 34 patients (30.08%), in people who drive or long distance travellers during the day; followed by housewives and military personnel, 16 patients for each (14.15%). The least reported cases were in children less than five years of age with two patients (1.76%).table 2| Table 2. Occupation of miliaria patients |
| | Occupation | Male | Female | Total number | percentage | | Children ≤5 | 2 | - | 2 | 1.76% | | Students | 9 | 4 | 13 | 11.50% | | Employee | 14 | 4 | 18 | 15.92% | | Driver | 31 | - | 31 | 27.43% | | Housewife | - | 16 | 16 | 14.15% | | Military | 16 | - | 16 | 14.15% | | Free job | 14 | - | 14 | 12.38% | | Retired | 3 | - | 3 | 2.65% | | Total | 89 | 24 | 113 | 100% |
|
|
3.3. Duration of the Rash
All patients gave a history of rapid onset rash that varies between three days and ten days with a mean of 5.24 days ± 2.007 SD.
3.4. Time of Occurrence of the Rash
Most of the reported cases in this study were seen during hot summer months of the year with peaks in August 36.28%, followed by July 33.62% and the least was seen in October 0.88%, no reported cases were seen during the remaining months of the year table 3. | Table 3. Time of occurrence of miliaria rash |
| | Month | Number .of patients | Percentage | | June | 29 | 25.66% | | July | 38 | 33.62% | | August | 41 | 36.28% | | September | 4 | 3.53% | | October | 1 | 0.88% | | Total | 113 | 100% |
|
|
3.5. The Frequency of the Attacks
Seventy-five patients (66.37%) out of 113developed the rash for the first time, while eighteen patients (15.92%) have a previous similar attack once before. On the other hand, the remaining 20 (17.69%) patients gave a history of recurrent similar attacks (three or more than 3 times before).
3.6. Site of Body Affected
The most common affected site was the upper back in seventy-nine patients (69.91%) followed by the lower back in seventy-four patients (65.48%). The least site reported was on the lower legs in twenty patients (17.69%), Table 4.| Table 4. The site of the body affected by miliaria |
| | Body site | Body area | N0.of patients | Percentage | | Chest | Upper Anterior chest | 57 | 50.44% | | Lower Anterior Chest | 59 | 52.21% | | Back | Upper Back | 79 | 69.91% | | Lower Back | 74 | 65.48% | | Extremity | Upper Arms | 21 | 18.58% | | Lower Legs | 20 | 17.69% | | Head and neck | Neck | 24 | 21.23% | | Head | 0 | 0% |
|
|
3.7. Associated Symptoms
One hundred of the affected patients (88.49%) have associated moderate pruritus; thirteen patients (11.50%)was complaining severe pruritus and five patients (4.42%) gave a complaint of tingling, prickling and burning sensation. Eight patients (7.07%) with rash involving chest or back or both areas, gave a history of disturbance and interference with daily activity, sleeping or sitting.
3.8. Associated Diseases
Only 8 patients (7.07%) gave a history of diabetes mellitus and three patients (2.65%) with history of hypertension.No associated dermatological disorders were detected during the time of the study.
3.9. History of Medications
Those patients with diabetes mellitus were on oral hypoglycemic drugs (Glibenclamide or metformin).Patients with history of hypertension were on antihypertensive drugs (methyl-dopa or captopril) medication.
3.10. The Clinical Types
Eight patients (7.07%) show classical miliaria rubra. Those patients show lesions of confluent small erythematous papule on erythematous background. The lesions distributed on upper and lower back and anterior chest , in addition to the lower arm, side of neck and axillae as shown in Figure (1).The other clinical form of miliaria seen in this study was different from the known classic form.One hundred five Patients (92.92%) showed a similar peculiar rash which started as erythematous or red brown patches that appear as dry red to red brown toasted-like patches or erythematous sun–burn like lesion that coalesce to form a larger one; the lesion was dry and with fine scales and covers most of the affected chest, back or extremities. The rash lacks the uniform non-follicular erythematous papule or papulo-vesicles that developed on erythematous base; this is typically seen in classical miliaria rubra. Similarly, these lesions lack the clear superficial easily ruptured vesicle seen in miliaria crystalina .It neither shows the firm flesh coloured non-follicular papule seen in miliaria profunda.This unusual presentation of miliaria was commonly seen in areas of friction like the back and chest. Figure (2),Figure(3) and Figure(4).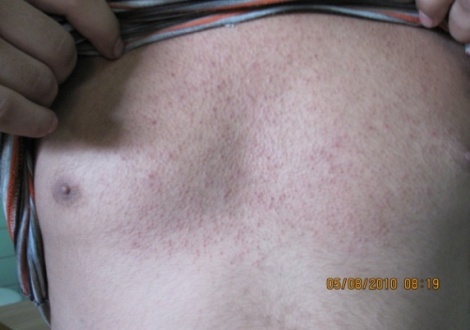 | Figure 1. Classical miliaria rubra on chest of male patient with tiny red non follicular papules |
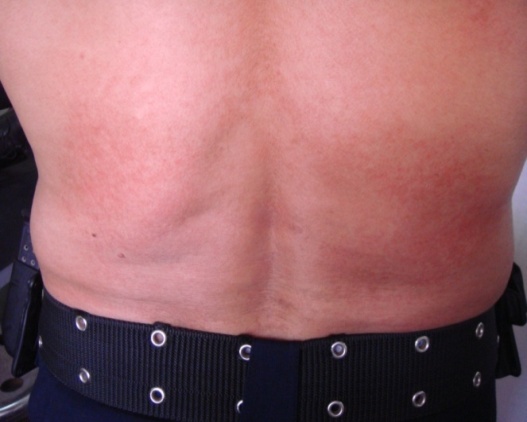 | Figure 2. Atypical miliaria on the back of military patient show dry erythematous sun burn like rash |
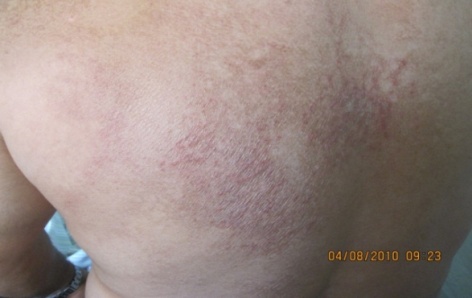 | Figure 3. Atypical miliaria on the back of male patient that show dry toasted like skin rash |
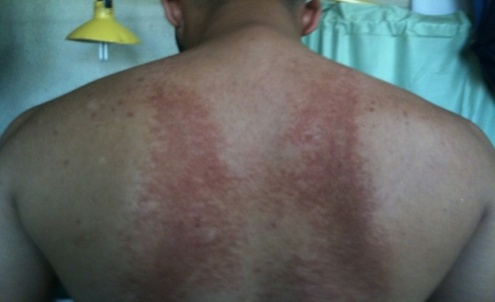 | Figure 4. Atypical miliaria on the back of male patient seen over the site of cotton under wear dressing |
Neither miliaria crystalina nor miliaria profunda was reported in this study.
4. Discussion
Miliaria is a common disorder of the eccrine sweat glands that often occurs in conditions of increased heat and humidity. Miliaria is thought to be caused by blockage of the sweat ducts, which results in the leakage of eccrine sweat into the epidermis or dermis.9,10Miliaria occurs in 3 forms namely as miliaria crystallina, rubra, or profunda, based on a transient occlusion of the eccrine sweat duct at different levels of the skin.11In Iraq, the climate is hot and dry in summer while it’s cold in winters. The average temperatures in Iraq range from higher than 48 degree centigrade (120 Fahrenheit) in July and August to below freezing in January.The reported types of miliaria in this study, shows the occurrence was markedly seasonal; all cases were seen during summer months especially during June, July, and August when the temperature reaches its highest level during the day time, sometimes reaching 48 or 49 degree centigrade in midday.The peak of reported cases was in August forty one (36.28%) followed by July thirty eight (33.62%) and least was in October only one (0.88%); this result agrees with I.H. Coulson &Wenzel FG that the disease is seasonal and seen mainly in hot humid tropical area.12,13The disease affects both sexes equally. 14,15Our study found that male patients were reported more than female(89 males) (78.76 %) versus 24 female (21.23 %).This is probably because male patients spend longer time outdoor and exposed to heat and sun than do female patients causing them to be more susceptible to develop heat rash.Regarding age groups, miliaria can affect any age group but the most age preponderance for both miliaria rubra and crystalina was in adult and paediatric age group.14,15,16This study revealed that the least reported age group was in paediatrics and childhood age group with age group (>5) years which was only two patients (1.76%). On the other hand, those with age group of (5-10) years were three patients (2.65%). These findings were probably because most of paediatrics age group referred to paediatric hospital rather than to general hospital.The highest figure of miliaria reported in this study was in adults (31-40) years and it was forty one patients (36.28%), followed by (21-30) years age group which was thirty six patients (31.85%). These results agrees with the previously reported studies worldwide regarding age groups affected by miliaria.14,15,16All patients in this study gave a history of rapid onset of the disease which varied between two days and ten days from the appearance of the rash, this time of onset of disease is compatible with what has been reported that lesions may occur within days of exposure to hot conditions and resolve within days after the patient is removed from the hot, humid environment13.The most affected site of the body was the trunk. The upper back was involved in seventy nine patients (69.91%), the lower back was involved in seventy four patients (65.48%) and the chest (mainly the lower anterior chest) was involved in fifty nine patients (52.21%). These sites represent the most common site of heat rash as these are covered areas and contain large amount of sweat glands. The least reported site was in upper arm 18.58%, probably because these are mostly uncovered area of the body during summer time.Regarding the frequency of attacks, this study showed that most of the patients (seventy five patients 66.37 %) developed the rash for the first time. Patients with previous attack were a minority; eighteen Patients (15.92%) have a previous similar attack once before. The remaining 20 (17.69%) patients gave a history of recurrent similar attacks (more than 3 times).The infrequent second or even third and more attacks can be attributed to the possibility that patients(who have the rash once before) were educated well about their disease so they managed to avoid high temperature and protect themselves from sun or extreme hot environments.From all the reported cases of miliaria in this work, no cases of miliaria crystalina were registered. This may be attributed to the fact that miliaria crystalina is mostly seen in infants and children, so such cases are mostly seen in paediatric clinics or in intensive care units rather than in dermatology units were this study was carried on or they may attend out ward private clinics . In a retrospective study from Japan, including 5387 infants in a newborn ward, miliaria crystalina was seen in 4.5%, with a peak around the 6th and 7th postnatal day. In this large series, the occurrence was reported to be extremely rare before day 4.17Similarly, a study survey from Iran in 2006 found an incidence of miliaria of 1.3% in newborns.18A similar figure of incidence of paediatric patients in North-eastern India showed an incidence of miliaria of 1.6%.19Worldwide, miliaria rubra is most common in tropical environments. It occurs in as many as 30% of people who move to tropical climates especially among people who recently moved to such environments from more temperate zones. Miliaria has been a significant problem for American and European military personnel who serve in Southeast Asia and the Pacific20. Only eight patients (7.07%) of miliaria rubra were registered in our study (six males and two females). No miliaria profunda was reported in this work. Miliaria profunda occurs in individuals who usually live in a tropical climate and have repeated episodes of miliaria rubra. In our study, there were only eight patients (7.07%) of classical miliaria rubra and none of these had previous attack(s). Although there were other patients with previous attack(s); eighteen Patients (15.92%) have a previous similar attack once before and twenty patients (17.69%) gave a history of recurrent similar attacks (more than 3 times). Due to the lack of a proper medical registration for the previous attacks, we were unable to determine the clinical pattern of these attacks. However, the absence of miliaria profunda in this study may be explained by the low number of both patients with rubra and patients with recurrent attack(s); on the other hand miliaria profunda occur in short time and disappear quickly within hours so this will not give enough time to see and report such cases. The majority of reported cases105 patients (92.92%) of miliaria rubra in this study does’t fulfill the criteria of the classical miliaria rubra. Although it shares appearance of erythematous patches,it lacks the erythematous papule or papulovesicular lesion seen in classical miliaria rubra. This dry rash is probably related to the hot dry weather in Iraq, which quickly causes the sweat to evaporate, especially when there is some sort of friction with the clothes.This rash was mostly recorded among males 89 patients (78.76%) than among females (only 24 patients 21.23%). This is probably because male individuals spend long time outdoor and exposed more to higher temperature and sun. In addition, most of Iraqi males use to wear cotton underwear beneath the shirt. As cotton is an absorbing material, so it get soaked with sweats during hot days; this will allow the sweat with all its constituent of salts and minerals to cause an irritative effect to the skin in close contact with. Also, this may act as an occlusive dressing which may exacerbate the hypohidrosis or even the anhidrosis that follows miliaria. Eventually, after days the skin will become dry and erythematous associated with itching and tingling sensation. This possible effect of occlusion is similar to what has been published by Tommy et al.21Tommy et al described the outcome of experimentally induced miliaria which was induced by occlusion and the resultant hypohidrosis or anhidrosis.21We also found the rash to be more severe in drivers, or long distance travellers, and in military personnel who wear shields for many hours which prevent the rapid evaporation of sweat and provoke its direct irritative effect on the skin.We also found the rash to look more severe in housewives who spend long time in hot environment, especially, during the extended time of poor electric power supply. Those, particularly, wear long sleeve clothes made of impermeable type of fabrics.For the best of our knowledge this form of peculiar rash has never been described before and we can describe such rash as atypical form of miliaria superadded with irritative effect of sweat or is another descriptive form of miliaria which required to be studied in more details and to perform histological study for it.
5. Conclusions
The most common clinical presentation of miliaria in patients of Al- Kindy Teaching Hospital is atypical form of miliaria consists of dry erythematous or brown red erythematous patch with or without dry fine scales usually seen on the trunk and other site of friction and associated with mild to moderate itching.
References
| [1] | Shuster S: Duct disruption, a new explanation of miliaria. Acta DermVenereol 77:1, 1997 |
| [2] | Champion RH. Disorders of sweat glands. In: Champion RH, Burton JL, Burns DA, Breathnach SM, eds. Textbook of Dermatology. 6th ed. Malden, Mass: Blackwell Scientific Publications; 1998:1997-9. |
| [3] | Wenzel FG, Horn TD. Nonneoplastic disorders of the eccrine glands. J Am Acad Dermatol. Jan 1998;38(1):1-17, |
| [4] | Ale I, Lachapelle JM, Maibach HI. Skin tolerability associated with transdermal drug delivery systems: an overview. Adv Ther. Oct 2009;26(10):920-35. |
| [5] | Holzle E, Kligman AM. The pathogenesis of miliaria rubra. Role of the resident microflora. Br J Dermatol. Aug 1978; 99(2):117-37. |
| [6] | Mowad CM, McGinley KJ, Foglia A, Leyden JJ. The role of extracellular polysaccharide substance produced by Staphylococcus epidermidis in miliaria. J Am Acad Dermatol. Nov 1995;33(5 Pt 1):729-33. |
| [7] | Niparko, John Kim; Klag, Michael J.; Lawrence, Robert M.; Romaine-Davis, Ada (1999). Johns Hopkins family health book. London: HarperCollins. p. 1308. |
| [8] | James, William D.; Berger, Timothy G.; et al. (2011). Andrews' Diseases of the Skin: clinical Dermatology. Eleventh edition. |
| [9] | Szabo G: The number of eccrine sweat glands in human skin, in Advances in Biology of Skin, edited by Montagna W, Ellis R, Silver A. New York, Pergamon, 1962, p 1 |
| [10] | Sato K, Dobson RL: Regional and individual variations in the function of the human eccrine sweat gland. J Invest Dermatol 54:443, 1970 |
| [11] | Hashimoto K, Gross BG, Lever WF: The ultrastructure of the skin of human embryos. I. The intra epidermal eccrine sweat duct. J Invest Dermatol 45:139, 1965 |
| [12] | I.H.Coulson. Disorders of sweat gland. B.Tony,B. Stephen Breathnach S., Cox. N,G.Christopher. Rook’s Textbook of Dermatology. 8th edition UK Blackwell 2010. |
| [13] | Wenzel FG, Horn TD. Non neoplastic disorders of the eccrine glands. J Am Acad Dermatol. Jan 1998; 38(1):1-17; quiz 18-20. |
| [14] | Hidano A, Purwoko R, Jitsukawa K. Statistical survey of skin changes in Japanese neonates. Pediatr Dermatol 1986; 3:140-4. |
| [15] | Moosavi Z, Hosseini T. One-year survey of cutaneous lesions in 1000 consecutive Iranian newborns. Pediatr Dermatol. Jan-Feb 2006; 23(1):61-3. |
| [16] | Huda M, Saha P. Pattern of dermatosis among pediatric patients attending a medical college hospital in northeastern region of India.Indian J Dermatol. 2009; 49:189. |
| [17] | Kirk JF, Wilson BB, Chun W, Cooper PH. Miliaria profunda. J Am Acad Dermatol. Nov 1996;35(5 Pt 2):854-6. |
| [18] | Arpey CJ, Nagashima-Whalen LS, Chren MM, Zaim MT. Congenital miliaria crystallina: case report and literature review. Pediatr Dermatol. Sep 1992; 9(3):283-7. |
| [19] | Straka BF, Cooper PH, Greer KE. Congenital miliaria crystallina. Cutis. Feb 1991; 47(2):103-6. |
| [20] | Sanderson Ph, Sloper Jc. Skin disease in the British army in S.E.Asia.I.Influence of the environment on skin disease.Br J Dermatol. 1953 Jul-Aug;65(7-8):252-64 |
| [21] | Tommy B.et al Miliaria and anhidrosis,journal of investigative dermatology vol.49,No.4 1997. |





 Abstract
Abstract Reference
Reference Full-Text PDF
Full-Text PDF Full-Text HTML
Full-Text HTML